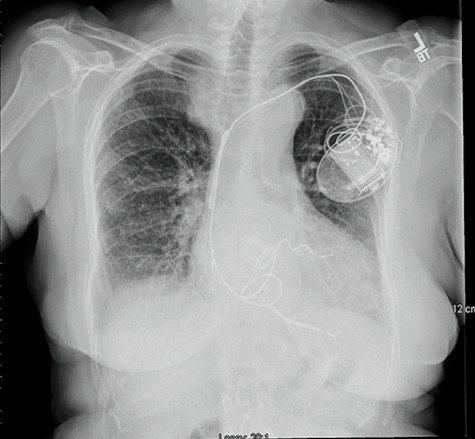
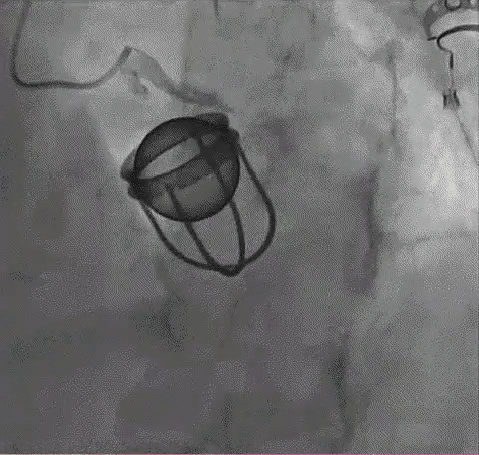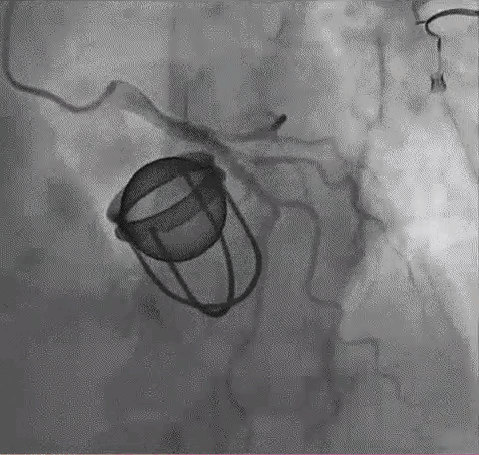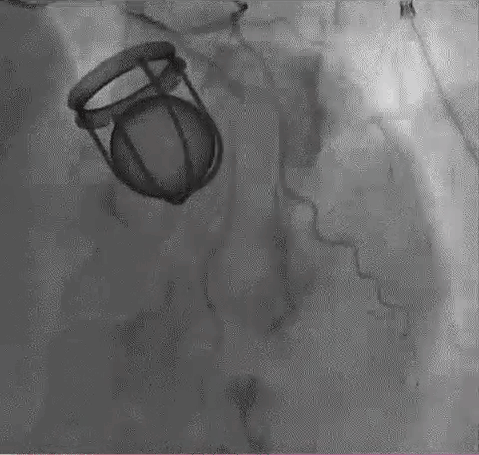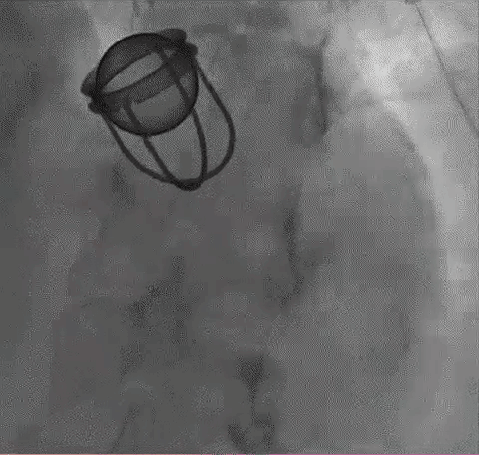Coronary Imaging : OCT works only in OCTOBER ! What to do in other months !
— Dr.S.Venkatesan (@VenkatThoughts) August 29, 2023
ESC 2023, throws silently two spanners( ILUMIEN 4, & OCTOBER) into the confused cath lab corridor ! https://t.co/GLwdz6tOV5 via @VenkatThoughts
Archive for August, 2023
ESC 2023 : Coronary Imaging update
Posted in Uncategorized on August 29, 2023|
New ESC 2023 Cardiomyopathy guidelines: Truths trail by 17 years!
Posted in cardiomyopathy, Dilated cardiomyopathy, hypertrophic cardiomyopathy, ischemic cardiomyopathy, Uncategorized, tagged drsvenkatesan, ESC 2023 new cardiomyopathy guideline, ndlvc, non dilated cardiomyopathy on August 27, 2023|
It was 2006
Allow me to recount an unassuming piece of a PowerPoint presentation from my institute, Madras Medical College, at the annual Cardiological Society meeting in New Delhi. The paper was categorized under miscellaneous sessions. I vividly remember the day. I have to admit, It was a nearly empty hall E, located in the basement of Hotel Ashoka. After the talk, I looked up to find that neither the chairman nor the handful of kind academic souls had any questions or comments to make. Pausing for a few moments, I quietly walked down the podium with an inexplicable silent pain.
The title of the presentation was “Non-dilated cardiomyopathy”
Welcome to ESC Congress Amsterdam August 2023
ESC, has come out with this new update on cardiomyopathy. It is a pleasant surprise to find the term “Non dilated cardiomyopathy” entered the cardiology academia, authenticated by the ESC.
I must confess, it is difficult to conceal the joy and a little bit of self-pride.


Some observations from this document
1. Despite our tremendous knowledge base, we are yet to hang up our boots, in pursuit of an Ideal cardiomyopathy definition. Genotypic or phenotypic ? Phenotype is closer to reality, while genotype is largely imaginary. It looks like, The newer guidelines are moving towards a phenotype-based approach in all aspects except in risk prediction. Fair enough.
2. All cardiomyopathies, whatever way we segregate, ultimately end up in the common clinical syndrome of heart failure. So. it is better to spend some quality time here and concentrate on HF therapeutics.
3. Cardiologists are expected to critically fine-tune their general medical knowledge, which will help recognize and treat systemic disorders like Amyloidosis, and other metabolic infiltrates.
4..Almost all RCMs have non-dilated ventricles, so why a new term NDLVC? Anyone wants to ask this question ?. Further, there can be significant overlap between RCM & NDLVC as well. Definitely, there is a lot to understand beyond this 2023 document.
5. Why do some ventricles refuse to dilate even in the face of adverse hemodynamic and pathological conditions. Is it an advantage or disadvantage? If ventricles are adamantly stiff and decide not to dilate, there is no other option, the atria will proxy dilate, creating more problems in the lung circuits. This also raises a fundamental question Is NDCM a better stress buster (think Laplace law ) than DCM? or vive versa , the accomodative nature of LV passify & blunt the slope of LVEDP at times of exertion.
6. One more reality is, NDLVC is also an Important subset in the now fashionable HF entity HFpEF
Final message
The message to youngsters is this. Discuss, debate, and document your thoughts in whatever forum, that is available. Don’t wait for all those big brother journals and their recognition. If there is truth in your writing, someday it will be revealed to the world.
Reference
Best excercise for optimal BP control : A meta-analysis & a surprise conclusion !
Posted in Uncategorized on August 26, 2023|
Lifestyle modifications and non-pharmacological modalities should be started in every hypertensive individual before starting them on long-term drugs. This is one of the foundational lessons in the therapy of hypertension. (Please mind, in no way, it conveys a meaning that we can give less importance to them after starting drugs.)
Exercise prescription has become a big-ticket event in hypertension clinics in recent times. Though any physical activity in adequate quantity is good, we have classified exercise into complex subtypes and found fancy ways of its administration.
Traditional belief gets a kick-back
We (At least me!) have been taught, isometric exercise is not BP-friendly. In fact, it can cause intermittent spikes that may persist for a variable duration depending upon the basal as well as dynamic adrenergic vascular tone. This is what I had taught to my students. This presumption is nearly shattered by this meta-analysis. It concludes that among all, Isometric exercise reduced the BP more than others. (especially wall squats and planks). More surprising is, that the usefulness of aerobics is lesser than dynamic resistance training as well.

Final message
Contrary to popular belief, Isometric exercise is not really hard on blood vessels and is likely to have a more favorable effect on blood pressure than aerobics.
Still, hesitating to fully accept the conclusion of this study. Exercise prescription is highly individualized & includes multiple cross-over strategies and self-learning. Caution is required when doing strong isometric exercises, especially after a vascular event.
Reference
A simple tip for peace of mind … for the modern patient
Posted in patient education, tagged ai in medicine, faith trust in doctors, patient behaviour, patient empowerment, technology in mediine on August 20, 2023|
Preamble
A patient who had a PCI some time back , asked me in one of his recent visit.
Doctor what is microvascular endothelial dysfunction and erosison ? Am I at risk of developing it ?
What am I supposed to answer ? Yes, I some how managed .” Don’t worry , it is a complex biological phenomenon. you need not go deeper into that. Take medicines regularly” He wasn’t happy with my answer is a different story.
A simple tip for peace of mind … for the modern patient
If the current generations of patients , equipped with hyper-knowledge engines, insist to understand 100% about their illness, imagine the consequences to the global healing system ,that has so many ground level issues to bother about.
One unofficial estimate from an elite , professional academic chatterbox of medicine suggests that the knowledge base with which doctors diagnose, treat, and understand the diseases they tackle, is at best 15%. Pateints need not be thankful , but atleast understand we are for working around with 85% ignorance, and still tries to bring out the best. I am sure this is a fact, no one can disagree ,regardless of the presence or absence of evidence to support it.
Final message
It might appear fair if someone argues blind faith in a trusted physician or hospital could end up as unscientific or unethical. But,what they fail to realize is, sciences’ blindness can be much darker, especially when it comes to the outcome of treatment and prognosis.
What does statin do to Cholesterol absorbtion from Intestine ?
Posted in Uncategorized on August 19, 2023|
Does this sound a difficult question ? Many felt so. Hence, I decided to chat with the popular AI machine.It is a brief little chat that surprised me .Please click the link , you can learn somee academic manners from the machine.
https://chat.openai.com/share/6b96c54e-ad52-472a-9ebd-b7b1e1c762be
Statin: Some untold story.
Last century’s rockstar drug, statin do stimulate cholesterol/sterol abosorbtion as well as possible neo-hepatic synthesis.This is basic bio-feed back mechansim , when one molecule is blocked in a living organsim. We must be aware, It is a less popularised truth (Intentionally ? ) among the cardiology community,
Ofcourse LDL comes down, at the cost of residual pre -choleterol particles that spill over to circulation resulting in hepatic and skeltal muslce injury.
There is an important corollary and a pharmacological cross invention and a new big market for a otherwise orphan drug called Ezetimibe.
It is not an optional accessory in statin therapy as many would like to think. There is good scientiifc logic, with and and without evidence though , that Ezetimibe, is an essential add on adjuct for optimal statin action.This is understandable, since statin consumption systematically depletes intracellular cholesterol, make the entire small intestine hungry for cholesterol by a bio – feed back mechansim once its synthesis is blocked.
There is also some concern liver might also synthesise some abnormal new unnamed lipids ,? as its normal cholesterol pathway is blocked. These info were never released to clinical domain.
Final message.
Statin tiggers increased lipid absorbtion at the intestines. Stand-alone statin therapy, still turns out to be a suspect value in atleaset one third of users as the bio -feed back surge could not be countered effectively. However, for statin to be optimally effective,add on Ezetimibe helps.
Also, It is clear one of the important duties, of medical professional is to teach the AI engine and help correct potential and real mistakes in its data base.
Reference
This is evidene less cardiology , ie class C evidence.Experts may add, dispute and contibute to this thread.In the process Chat GPT might learn as well.
Found one evidence
I am 49 … not out, how about you TAVI ?
Posted in Uncategorized, tagged prosthetic aortic valve, starr edwards valve, tavi valve on August 1, 2023|
This post was written after coming across a case report Oxford medical case report.
What is the life of a prosthetic Aortic valve?
The standard answer needs to be, mechanical valves can last up to 25 years or more. But, we are in a techno-conflict era. Instead of working on the longevity of the valve, ( with concerns for long-term OAC ) we fell for the biological valves. Curiously, this has made the durability of the valve, a less relevant discussion in many centers. We get excited when some company brings out a long-lasting bio-prosthetic valve that can live up to a maximum of 15 years.
Now, the biological valve comes in a new avatar ie TAVI, in a big way. Soon, we may celebrate an event free 10 years after TAVI. Going percutaneous is transformative. But at what cost? Fusion of metallurgy, chemistry, and pharmacology should make it possible for in-vivo metal valves to be safe for 75 years of human life span. The irony is we almost had one, One valve’s longevity was consistently exceeding the patient’s life span,(at least as far as we observed in the Rheumatic heart disease) This has been the star of all valves. We know what happened to that valve.
Final message
Most SE valves are implanted in the mitral position. Starr-Edward in an Aortic position working for 50 years is a big proof of reality. Of course, we can’t extrapolate with a single case report. We have stopped the production of these valves. So, there is no way to test it either. Anyway, cardiologists, cardiac surgeons, and finally the generation X, TAVI Innovators have something to learn from this case report. Forget Starr-Edwards, It looks like, there are some invisible forces that work against mechanical valves in recent times, which may not be good for our patients as of now. (There is something interesting related to this in Ref 2)
Future directions: Past need not be past
Nothing is impossible for our hyper-talented scientists, except probably in the “faculty of looking back” the past-Innovations (falsely labeled as obsolete) and bringing them again to optimal usage. If cardiologists feel surgical AVR injures their interventional pride, how about a percutaneous cage delivered at the root of the aorta, after ablating native leaflets, followed by an inflatable silicone ball?
Reference
A current 2023, opinion from the renowned Dr. Catherine Otto on this Mechanical vs biological valve , Indications, current usage pattern, the cut-off age, etc