Archive for October, 2017
Interventional closure of potholes outside cath lab with simple concrete device !
Posted in Uncategorized on October 29, 2017| Leave a Comment »
Early thrombolysis knocks out pPCI yet again . . . this time from Shanghai !
Posted in Cardiology -guidelines, cardiology -Therapeutics, cardiology journals, tagged EARLY MYO trial circulation, ppci vs thrombolysis, primary PCI vs thrombolysis, stream trial on October 18, 2017| 3 Comments »
Hemodynamics of sudden “Toilet deaths” following STEMI !
Posted in acute coroanry syndrome, Cardiology -Interventional -PCI, cardiology -Preventive, Cardiology -unresolved questions, tagged acs, hemodynamics in LAD following valsalva, predischarge stress test, primary pci, stemi, Sudden cardaic deaths in bath room toilet, valsalva vs squatting on October 1, 2017| 1 Comment »
The age old statistics , 30 % of deaths following STEMI happen even before patients reach the hospital may still be true. But ,there is an untold story that happen regularly in the rehabilitation phase .Its ironical many apparently stabilised STEMI patients still lose their life just before they get discharged or within 30 days .More often than not this happens in the toilet when they strain for defecation. At least a dozen deaths I have witnessed in the last few years. Of course we have resuscitated many near deaths as well.
What exactly happens to these ill-fated patients inside the toilet ?
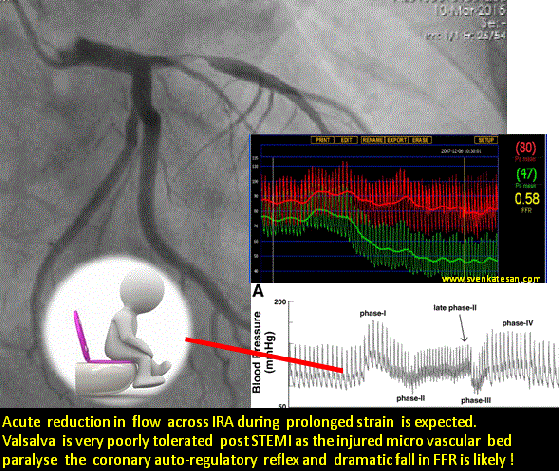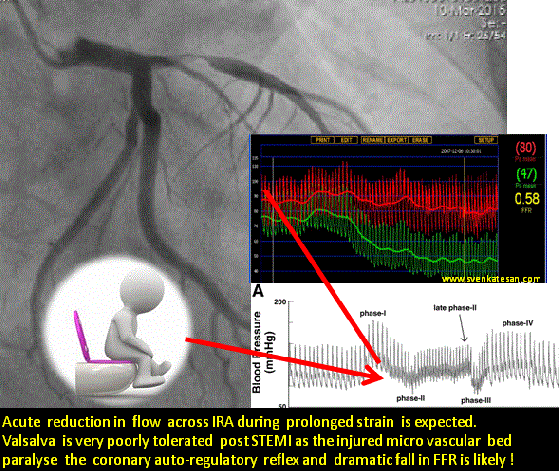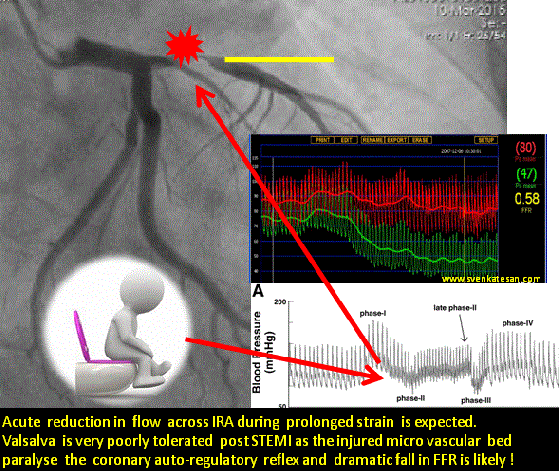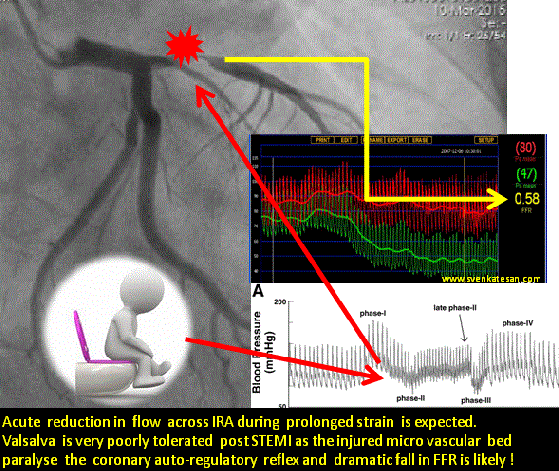
Straining is often an isometric exercise and prolonged strain ends up in valsalva maneuver , a prolonged valsalva strain realistically shuts both vena cava due to raised intrathoracic pressure .Vena caval shutdown is equivalent to asystole and imagine the chaos in the delicately recannalised LAD when the coronary perfusion pressure nose dives (Even the stented segment in IRA is vulnerable as distal flow restoration may take time !)
The sudden systemic hypotension leads to fall in coronary arterial pressure proximal to the lesion. The normal physiological response to proximal fall would be corresponding distal fall maintaining the flow gradient . If the microvascular bed is damaged( loss of capacity to vasodilate ) this distal fall may not happen promptly .So its acute standstill of flow across IRA ( or even Non IRA if it has a lesion ) triggering events that rapidly destabilise unless intervened.
.
Other modes of sudden toilet deaths
*The opposite process , ie sudden spikes of blood pressure (In contrast to hypotension of Valsalva strain ) can occur as straining is equivalent to Isometric exercise which increase afterload .This can either cause LV failure, another episode of ACS, myocardial stretching, even tear it and result in mechanical complication.
- Acute LVF triggered by spikes of BP /new onset ischemic MR.
- Free wall rupture and tamponade.
- Emboli getting dislodged from LV during strain
How to anticipate and prevent these deaths ?
- All complicated STEMI patients should have special rehabilitation program.
- A simple rule could be patients with persistent ST elevation with are prone for further events.They should be flagged. (Stented / TIMI flows matters very little !)
- Restrict all vigorous activity for minimum of one to two weeks ( I am not a believer of pre-discharge stress test even in uncomplicated MI )
- Use laxatives adequately.
- Western toilets may have an hemodynamic advantage. Indian closets that require squatting which increase the venous return , ultimately it compromises coronary hemodynamics more. We don’t understand as yet ,what will happen if one perfoms a valsalva and squatting simultaneously.(Which will prevail over the other ?)
- Finally toilet shouldn’t be locked during rehabilitation for safety purposes.
- All post STEMI pateints should have registered with emergency contact and alert service ready.
Has primary PCI has reduced the sudden deaths in Post MI period in current era ?
I’m afraid , I can’t say a dogmatic yes . May be ,to a certain extent , However, it has created a new subset of perfectly stented still prone for ACS.A physiologically or pharmacologically recannlised IRA generally heals by themself. A Stented IRA hands over the responsiblity of healing the injured IRA to us .Ofcourse ,we try to do it with lot of difficulty .(Different versions of confused DAPT regimens !)
Final message
Please note , “discharge to 30 day mortality” following STEMI which is upto 2 % .It is the most neglected and mismanaged phase in coronary care .Toilets are definitely not a benign place for them and all the good work done by you in cath lab and CCU can be nullified in few Innocuous looking seconds !
Postamble
Is Toilet room death amounts to negligence / mis-management inside hospital ?
May be there is a reason for this argument. When to ambulate in complicated STEMI is a big question. ? Though we have guidelines some of the patients are reluctant to use assisted service.
I think its a calculated risk , and there is trade off between the benefits of early ambulation and potential exertion related risk.
One such argument by a cardiologist in a medicolegal situation goes like this. “I thought my patient’s heart is stable enough to use toilet , it misfired , hence it is just an error of judgment. I can’t be faulted. Though this argument appear logical , many times it can’t hold water in court of law !”
Further reading
Cardiac rehabilitation NICE guidelines : Myocardial infarction: cardiac rehabilitation and prevention of further cardiovascular disease 2013




