One of my patients with atrial fibrillation recently developed a fairly moderate sized right MCA stroke that resulted in dense left sided hemiplegia .He was on warfarin , but the stroke was confirmed to be ischemic,the etiology was fixed as cardio embolic .After a smart recovery he asked this question.
Why did the clot from my heart preferred to enter the brain doctor ? Is there no other place for it to go ?
I told him in simple terms , “It is your destiny and the clot’s wish”. In fact , you are some what blessed as the clot did not enter the left side of the brain .If it had gone, your speech would have severely affected and you may not be asking this question to me ! It is true the clot do have other options to embolise , however they are still trouble some !

What is the diameter of internal carotid artery , and cerebral artery ? The common size of LA appendage clot almost match with this !
It can go straight down to your leg , kidney , intestines or upper limbs .All are equally dangerous and present dramatically . Very rarely it can enter coronary arteries bringing a heart attack rather than a brain attack .If it is going to the legs you are at risk of acute monoplegia instead of chronic hemiplegia .Peripheral embolism are very painful .Intestinal ischemia evokes a most excruciating pain one can ever encounter ! Luckily stroke is not painful.God is kind enough ,he foresaw cerebral ischemia to be more common and hence made it pain-free ! (There is no cerebral angina equivalent !)
Having said that , I felt we should get a scientific answer to my patients query .
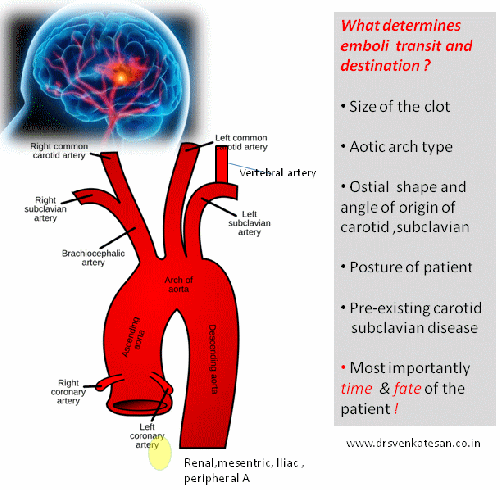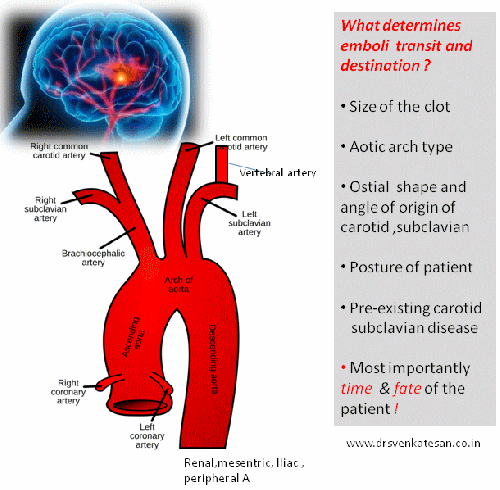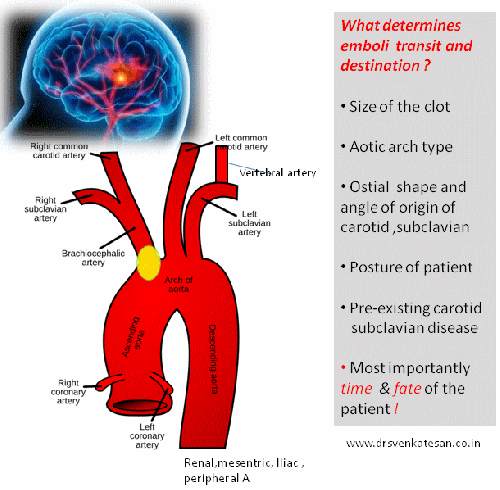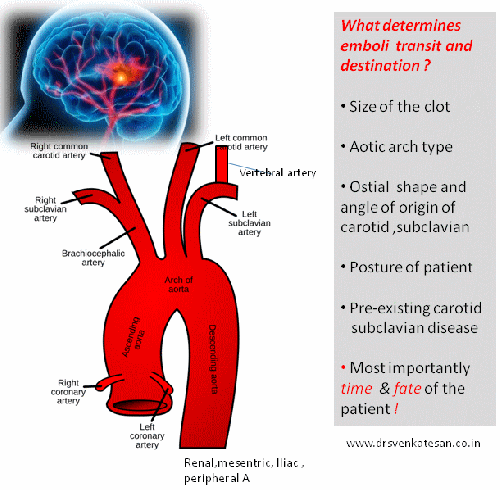
What determines the destination of these emboli in transit from heart ?
The dynamics of a cardiac emboli hitting the cerebral arteries can never be known in live human vascular tree. The following factors might play a role.
- Clot size and morphology
- Anatomy of aortic arch -Right MCA is in immediate capture zone .
- Arch type and curvature radius
- Arch branch ostial size , shape
- Vertebral arterial embolism is rare because it is a second order branch.
- Dessication and disintegration of clot in transit is possible leading to multiple destination.
- Most shaggy looking large clots fail to enter carotid instead reach the peripheral circulation.
- Vegetations, tumor debri behaves differently as the density and mass of emboli has a some effect on the transit velocity and momentum.
Variations in Aortic arch anatomy

Image courtesy : Anatomy Atlases by Michael P. D’Alessandro, and Ronald A. Bergman, from university of Iowa. http://www.anatomyatlases.com
It is surprising, human beings can have as many types of Aortic arch as English alphabets . Then,there are innumerable ways for cardiac clots to embolise too !