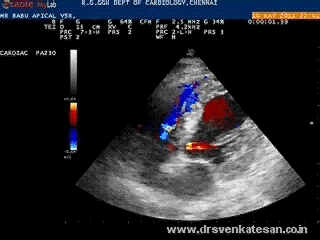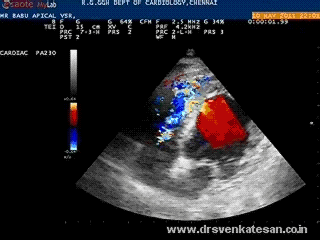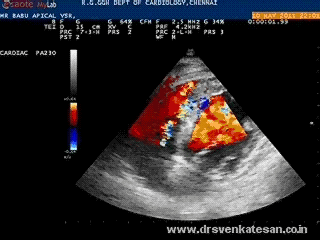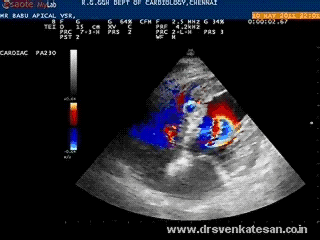
Angina and dyspnea are the two cardinal ( classic ) symptoms of cardiac disease . While dyspnea is a manifestation of raised LV filling pressure , angina implies reduction in blood supply to heart .
In other words dyspnea is related to excess blood in the lungs and angina is due to less blood in the coronaries !
So , it is obvious even though these two symptoms are closely knit entities , patho- physiologically they are distinctly different in real time , when an actual cardiac event unfolds in the bed side .
This also partially explains , why simultaneous presentation of angina and dyspnea is relatively uncommon in CCUs , than one would expect .(In a given patient , one of them will be dominant)
Why and how our patients (and also physicians !) get confused with dyspnea and angina ?
When William Heberden described angina over a century ago , he was so meticulous in his description and observation. In fact , it was, as if he felt the angina himself and wrote it .One can rarely expect such a description from any of our patients . So , it is not at all a surprise for mistaking any mid sternal discomfort as dyspnea instead of angina . (This error in describing angina is the commonest cause for dyspnea playing this dubious dual role !)
When to suspect dyspnea as an Anginal equivalent ?
Here are some real situations ( and clues ) where dyspnea may be considered as anginal equivalent.
- Diabetics
- In elderly with autonomic dysfunction
- Patients with chronic beta blocker and other anti anginal drugs.
- Post PCI/CABG patients (Normal LV function but dyspnea : Denerved heart blocks pain ?)
- Exertional dyspnea that stops immediately could be anginal equivalent.
- Dyspnea with palpitation is rarely be anginal equivalent as palpitation indicate good LV /mitral valve function.
- Dyspnea on isometric exercise rather than isotonic exercise .
Mechanism of anginal equivalence
While the trigger for dyspnea is elevated LVEDP which stimulates the stretch receptors in lung .For angina , it is the free nerve ending in myocytes that gets irritated and generate pain signals.
When ischemia presents as dyspnea two mechanisms are considered. One is myocardial , other is purely neurogenic.
- It is believed critical ischemia of myocardium ( Defective Ca ++ uptake into sarcoplasmic reticulum) induce “a wide area diastolic dysfunction” of LV that raises PCWP to generate dyspnea. Further , ischemia induced regional LV dysfunction that subtends the pap muscle could result in ischemic MR and severe dyspnea. (Exertional Mitral regurgitation is getting major attention now )
- In many patients with diabetes or autonomic dysfunction the velocity of pain signals become sluggish or blocked en-route to brain stem . Often they change track to travel in the nerves meant for carrying somatic siganls , J receptors , intercostal spindle etc . This spill over and cross talk creates a false sense of dyspnea , whenever ischemia occurs. This is attributed to the wide and complex neural network of thoracic sympathetic ganglions.
Some of the known associations with Angina equivalent .
- Diastolic dysfunction
- Ischemic MR
- Small rigid left atrium
- Atrial fibrillation
How to investigate a patient who is suspected to have angina equivalent dyspnea ?
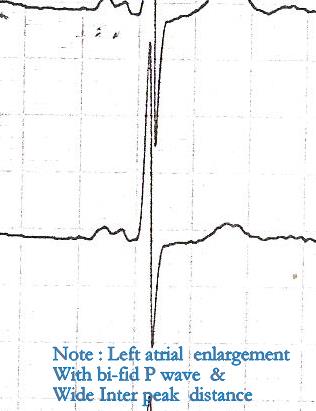
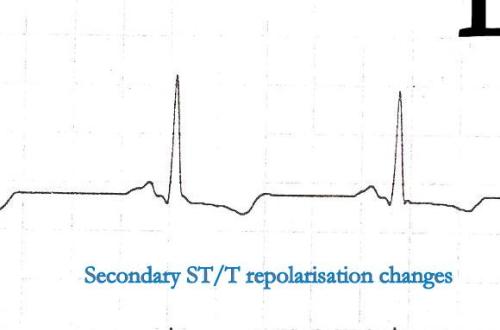
- ECG
- X ray chest
- Echocardiogram will settle the issue most times.
Nuclear scan and angiogram in deserving patients
When can angina and dyspnea occur together ?
Angina and dyspnea if truely occur together causes grave concern for the physician.
This indicates two things .
- The myocardium is ischemic and generates pain (And possibly ongoing necrosis) .
- Simultaneously its pumping or receiving function is also compromised resulting in entry block from the lung resulting in acute dyspnea.
Both are ominous signals . This situation occurs most often in STEMI with LV failure .
If dyspnea occur in NSTEMI/UA , it is a worst possible complication . GRACE registry quotes maximum mortality for unstable angina with cardiac failure .The reason being the cardiac failure in UA is due to non necrotic global ischemic stunning of LV myocardium with or with out acute mitral valve failure.(Flash pulmonary edema)
Why angina is rare in chronic congestive cardiac failure ?
The main reason being , a severely dysfunctional heart contracts poorly .In reality , it is never thirsty for blood . Even if it is perfused well , there is no good muscle mass to burn the ATPs from it .A failed myocardium is more or less a sleeping myocardium .It does not even have the energy to cry with pain at times of ischemia ! .However significant the ischemia is , it can often evoke only a gasping sensation .
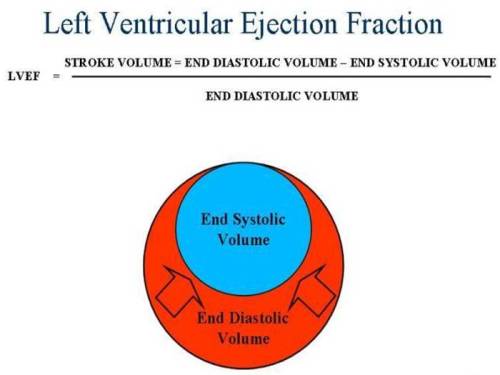
The other explanation is more imaginative . In cardiac failure heart dilates .The end diastolic and end systolic volume is high. The cardiac chamber is always filled with excess residual blood .This , some how tend to perfuse the myocardium directly and provide a good reserve .This may be more important in RV perfusion .( Trans myocardial laser revascularization is based on this concept – direct myocardial perfusion from the chambers)
While angina is rare in chronic cardiac failure, it should also be realised ,dyspnea is rare in uncomplicated acute coronary syndromes. We know ACS primarily present with angina. Exceptions are always there.
In elderly, diabetic , with co morbid patients , ACS may present without angina . Instead they present with vague dyspnea and shortness of breath . It is here , physicians face a tough task to identify dyspnea behaving like angina equivalent. Of course , the good old ECG bails us out most of the time.
Therapeutic importance of recognising anginal equivalents ?
The revascularisation procedures (CABG/PCI) are too good in relieving angina , but least effective in providing relief from dyspnea.So real anginal equivalents if recognised properly can be subjected to early revascularisation .
Can we consider exertional dyspnea as evidence for ongoing ischemia in a post MI patient ?
This is tricky question . We do not have answers to it. Readers can try to answer . The commonest cause of dyspnea following MI is due to physical deconditioning and associated LV dysfunction.
Final message
Coming back to the basic question , Is this dyspnea . . . an angina equivalent doctor ? No simple answer is available .
The first and foremost investigation to do is ECG .This will settle the issue many times. Next is the reassessment of history clinical presentation and past history. Every patient with unexplained dyspnea must undergo a minimum of three investigations (ECG, X ray chest and Echocardiogram ) If any of these suggest a cardiac compromise further evaluation is indicated.
So, the message here is , clinical findings are insufficient to rule out ischemic etiology for dyspnea.
References
Nil . Every thing is my random thoughts !
Read Full Post »