Archive for March, 2023
AI, is not risk free in medical science !
Posted in Uncategorized on March 25, 2023|
A hemodynamics quiz: What is the effect of AF on mean LA pressure?
Posted in Uncategorized on March 25, 2023|
ERS pattern in ECG : “Iatrogenic panic” is unwarranted !
Posted in Uncategorized, tagged ers pattern in ecg, ERS syndrome on March 23, 2023|
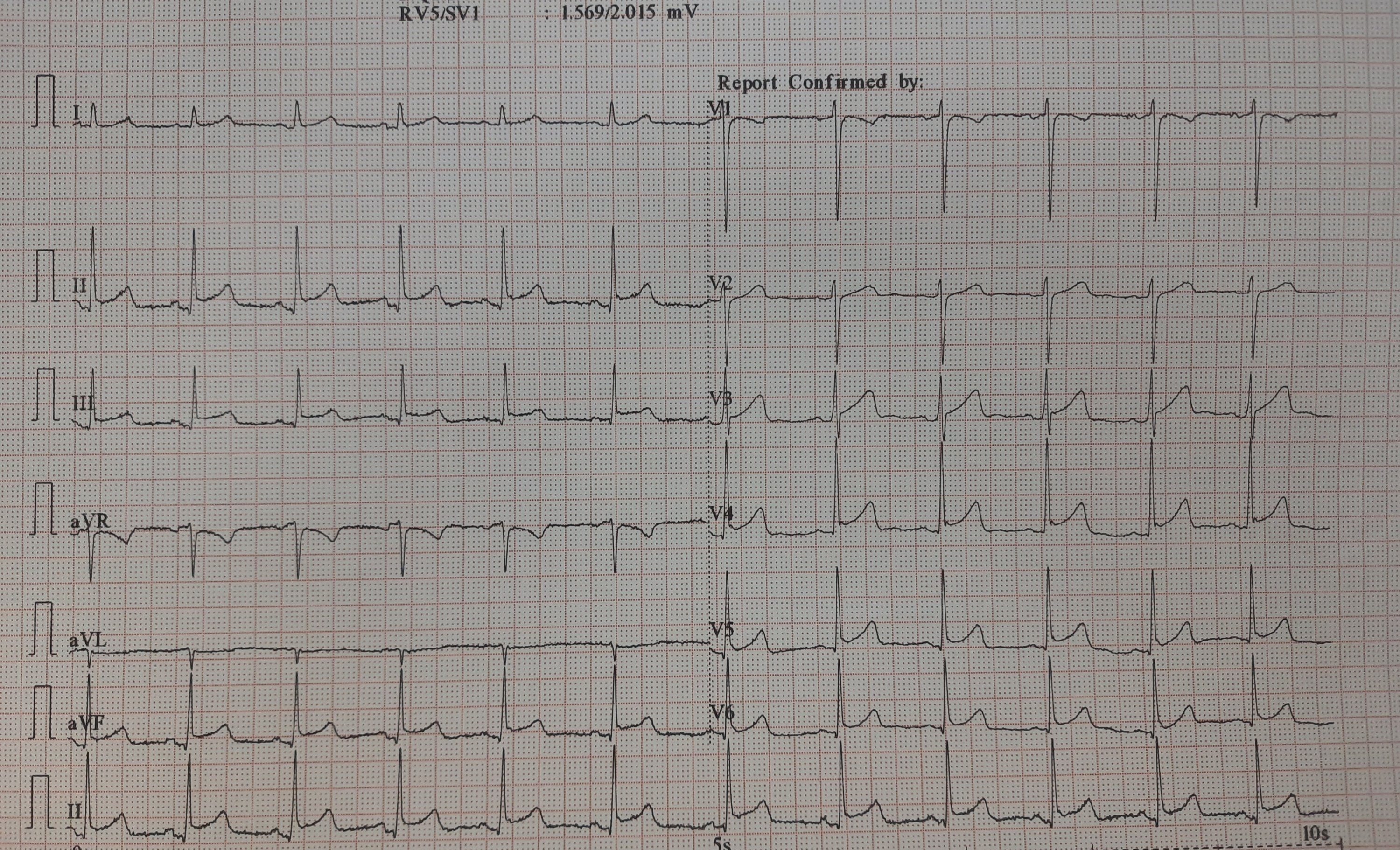
This is an ECG of a 25-year-old, recorded in master health check-up.
It would be mind-boggling to know the prevalence of such ERS patterns in the general population. One estimate suggests it could be anywhere between 3 to 13 % depending upon the criteria used. Let us assume the mean as 5 %. Then, it would be 30 crores of human beings in our habitat show this ECG pattern. If applied, in my city Chennai alone 5 lakh people could carry this tag.
While it is true, some forms of ERS and J wave syndrome can be markers of serious ventricular arrhythmias, either spontaneous or at times of Ischemia. Currently, It has become a fad, in cardiology academic circles*, to propagate the idea that ERS is no longer a benign condition. This is not acceptable at any degree of cognition. This happened mainly after few studies in powerful journals created some alarmist views. (*Maybe there is a bit of truth there. I still have doubts about whether we interpreted the Michel Haïssaguerre study properly)
Final message
ERS is a widely prevalent normal ECG variation with a minuscule risk. High-risk subsets need to be screened only if the J waves encroach and spill dangerously into the ST segment as well. Of course, this pattern is of serious concern if there is a family history of young SCDs has occurred.
Reference
Here is a good review of this topic by
Learning targeted IAS puncture in 20 minutes
Posted in Anatomy of heart, Uncategorized, tagged anatomy of heart, ias puncture, right vs left atrial anatomy on March 10, 2023|
The main reason for all those jitters, we cardiologists, get every time we puncture the IAS is not due to a lack of expertise and experience perse. There are two more reasons. First and foremost, it is still largely a blind* procedure. (Even in this era, where drones with HD vision shoot one-meter targets from a 1000 KM range ) *TEE and ICE are there, but they rarely give enough confidence.
The second reason is more important and is rectifiable. It is the perception error in our anatomical cognition, that is fed to us from first-year medical school. We are made to believe (at least to people like me ) The right atrium is aligned like a perfect box on the right side, sharing a wall called IAS, and the left atrium is obediently placed left of the right atrium. Please realize the heart is such a complex twisted single tubular organ, the venous end, in a stunning backward loop brings the LA most superior and posterior to the right atrium overriding the left-right relationship.)
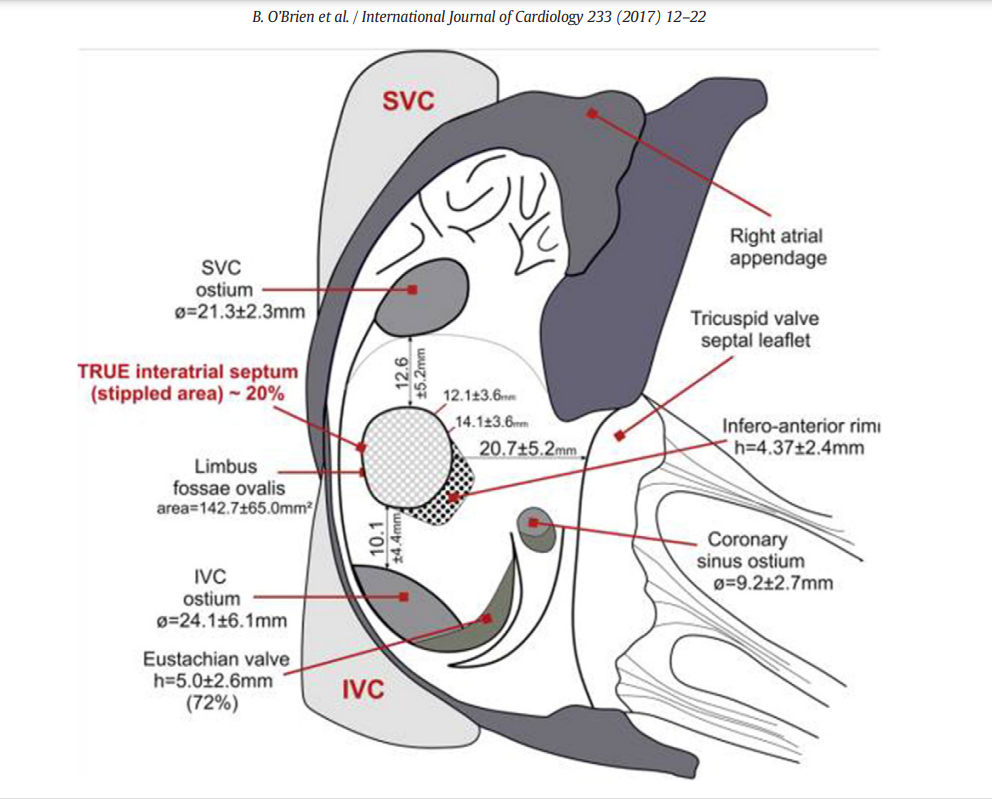
The right atrial terrain and IAS with multiple bumps and holes. Note the true IAS constitutes only 20% . This is where our punctures need to be.
Development of IAS
IAS development and the number of layers it sandwiches, the tortuous tracts of PFOs, the fossas, and its variable limbus is a big topic. Further, It is worth recalling, the true IAS hardly forms 20 % of the area of the interatrial contact surface.
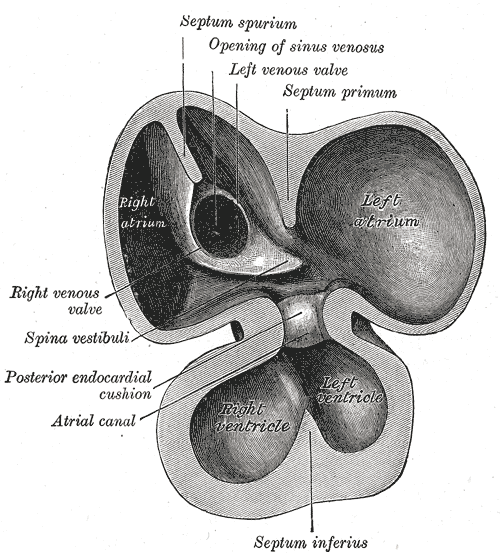
(the differential regression of sinus venous, along with infolding of the roof and along with curious septum spurium , the ubiquitous septum secundum make the texture, area & shape of IAS, a fascinating creation, though troublesome for the cardiologists ! ) Whoever named that part of vanishing IAS as spurious, (I think it is Henrry Grey ) has much fore-vision.
Forget about all this. Tell me how to cross this difficult terrain
Coming to the real world of interventions, we need to do targeted punctures in different spots of IAS in various interventions.(Mitra clips, LAA device, PTMC, PV abaltions, Mitral paravalvular leaks , TMVR etc) This has made this task even more tricky. Experts are always there to help us out. Like swimming, it can never be learned in books.
This 19-minute clip from. Seoul, South Korea is an excellent resource. Thanks to Dr. Sang Weon Park
Along with sound anatomical knowledge, improved hardware, and imaging like deflectable sheaths, TEEs, and ICE (intracardiac echo ), let us hope, it will soon become an easier task for everyone.
Final message
Understanding “attitudinal cardiac anatomy” with fluoroscopic overlay is the key. Again, it needs to be stressed, “Right is not right, and left is not left” when it comes to true atrial geo position. LA is equally posterior, superior, and of course to the left of RA. Some of my colleagues are blessed with a special 3-dimensional skillset (Inherited ?) I failed miserably to understand this, till very late. I am sure, Dr. Park’s video will help all our youngsters to cross the difficult gateway to the left side of the heart.
Reference
One more good read
B. O’Brien et al. / International Journal of Cardiology 233 (2017) 12–22
P wave spotting in AF is not forbidden
Posted in Uncategorized, tagged cardiology research topics for fellows, causes of absent p wabes, p vs f waves in af, p waves in atrial fibrillation, research topics in atrial fibrillation on March 8, 2023|
Fibrillation is a continuous, chaotic muscular activity. In AF, atrial muscle is expected to lose all coordinated contractions with fibrillatory waves replacing P waves. Have you ever spotted a suspicious P wave in a strip of otherwise explicit AF? If not, this write-up is not for you.
An evolving rare theme in Atrial fibrillation
Have a look at this ECG
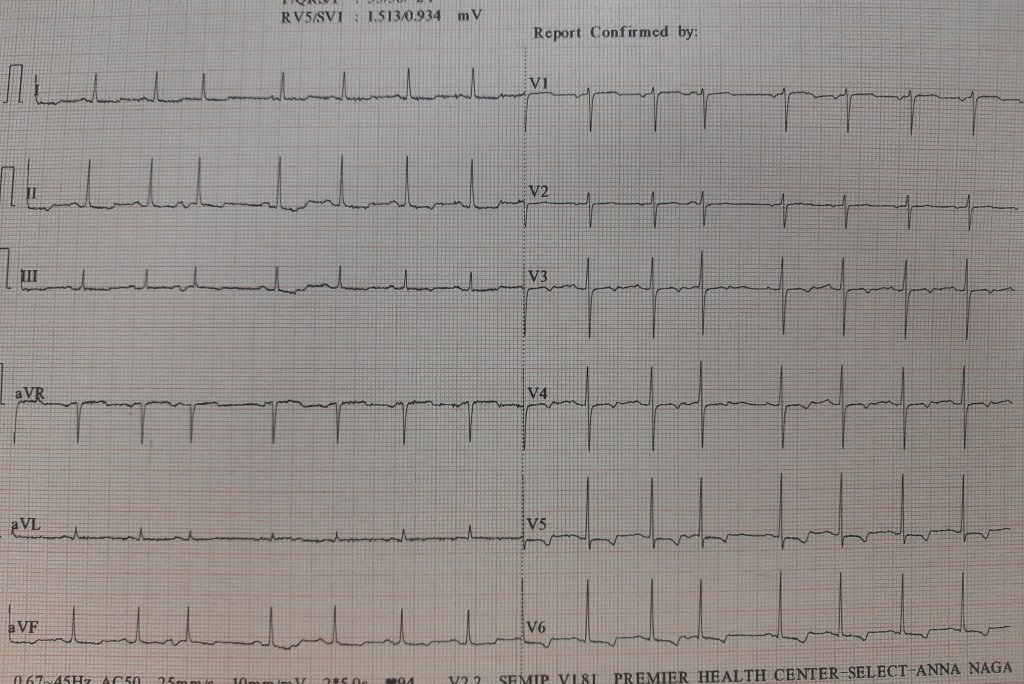
Here is an ECG, that was reported as AF, multiple APDs, or Possible AF, Pre AF. I suggested the term AF in transition. While few agreed, many said it is a straightforward SR with APDs, making it appear irregular RR.
But, the fact of the matter is, ECGs are insensitive to pick all fibrillatory wavelets. It can selectively pick a few coarse F waves and make them appear as P. I think, in this era, we should not diagnose AF by proxy, ie absent P waves. Rather, we need to look actively for fibrillatory wavelets. (Imagine all sinus arrests will qualify for f fine AF with a slow ventricular rate is it not ?)
The semantics of AF nomenclature is long. Intermittent AF, and paroxysmal AF, are well-known entities. It is now clear, AF can occur for a few seconds and vanish too. It seems we need to play some more linguistics with the most common cardiac arrhythmia. (Non-sustained AF, evanescent AF, etc )
Some thoughts on this hide & seek P waves
- Apart from the conventional list of absent P waves, one more example is repetitive APD can stun the atrial muscle for a few moments or minutes.
- Then, we always have the issue( eluded to earlier) of sinus node paralysis, with irregular junctional escape mimicking AF.
- Amiodarone can reduce fibrillatory rate, and (AF cycle length ?) Coarse F waves slow and stabilize it to mimic an organized P wave
- P on Ta waves (Like R on T ) can trigger a nonsustained AF for a few moments in a functional manner without real pathology in atria.
A funny memory brings back an EP truth
During our student days, my Professor used to trap us with this question, Which atria would fibrillate in mitral stenosis? Many of us blinked, and few had no hesitation to say, it is the LA that fibrillates. Now, after 50 years we realize, how fascinating the secrets AF has unfolded. Some organized activities are often in the right atrium, even as LA begins the process of AF. It is possible it may take variable time for the left atrial chaos to spill over to RA*. During these electrical uncertain times, some of the right atrial P wave activity refuses to die down. Even more dramatic one Atrium alone can permanently fibrillate and others completely insulated by blocking the signal in the Interatrial pathways. (Ref 1 ) Ndrepepa’s paper in the JCE 2000)
Final message.
True scientists rarely bother about questioning a dictum. The concept of non-uniform AF was first thought of by (Schrmp et al Ref 2) 100 years ago in 1920, and Zipes(Ref 3) hypothesized this in 1973. now, in the Year 2000, Ndrepepa confirmed it with EP studies. The spotting of occasional P waves is not forbidden in AF if the contralateral atria decide to block the incoming AF signals and keep generating their own P waves
Young EP guys, now that you are equipped with the sophisticated intracardiac GPS, please pursue this provocation in AF. One more piece of evidence we observed in the echo lab. Try to look at Tricuspid doppler A velocity waves in full-blown AF patients. You can see the surprise for yourself. This is very good research work to do. This is one of the ideas I gave to my fellows at MMC. Now, it is free for all to pursue whoever wants to do this. The clinical implication* will follow.
* A lingering query, how common is RAA clot in mitral stenosis with AF and the possible threat of pulmonary embolism?
Reference
2.Zipes DP. DeJoseph RL: Dissimilar atrial rhythms in man and dog. AmJCardioi I973;32:6l8-628.
3.Schrumpf P: De 1’interference de deux rythmes sinusaux. Preuve du dualisme du nodule de Keilh. Arch Mai Qwur 1920;l3:168-173
Postamble
The snapshot from Ref 1 . The term Isolated AF confined to one atrium could be a rare event, but, no one can deny we have plenty to learn from them