Bicuspid aortic valve (BCAV) is one of the common congenital abnormality of heart . Incidence can be 1-2% of population . It can result in premature aortic degeneration with Aortic stenosis/Aortic regurgitation or both .
The normal development and arrangement of three cusps is altered ( rather interrupted ) during fetal life.
There can be two ways BCAV can occur. One is due to the fusion* of two leaflets to covert a tricuspid valve into bicuspid , and the other is two cusps develop de novo .The former has a raphe , while the later has no raphe.
The fusion* occurs between either
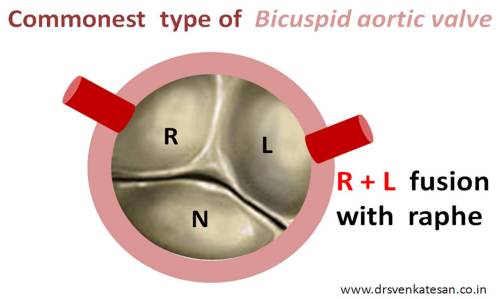
- Right and left (R +L)
- Right and non coronary cusp (R +N )
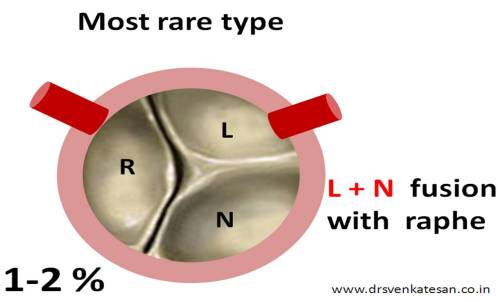
- or Left and Non coronary cusp (L +N)
(* The fusion is embryological , not acquired )
Most often the fusion is due to lack of division in the valve analgen .Hence a raphe (A conjoint remnant) is noticed .
90% of BCAV has raphe ,only 10 % lack raphe . Aortic root is also structurally abnormal in many .(Little clinical sequale though !)
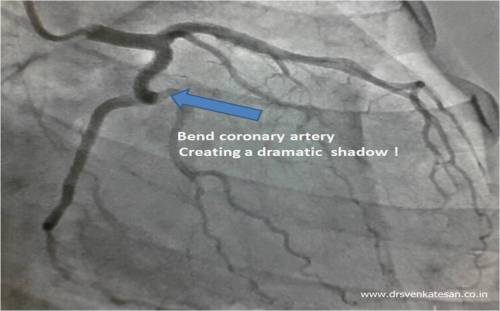
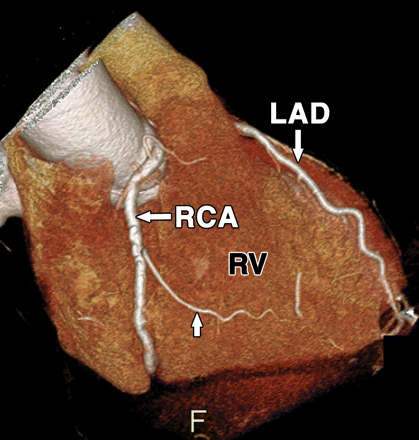
Coronary artery origin anomalies are more common with BCAV. We also know co-arctation of aorta has a embryological link with BCAV.
The commonest type of BCAV is
The most hemodyanmic stressed BCAV is R +N type fortunately it is rare
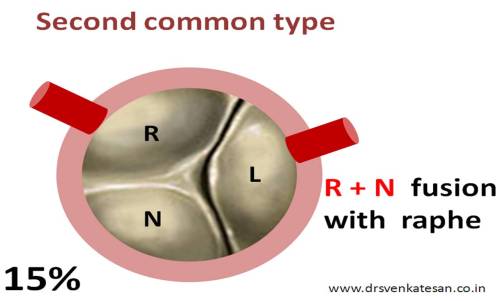
R + N fusion is a high risk BCAV as degeneration occur fast
The least common type is
The coronary artery origin anomalies are common
BCAV in the absence of raphe is classified separately (This constitutes 10 % of all BCAV)
The nomenclature is
- Antero posterior (Common type ) AP
- Lateral (L )
What is the pathological significance of raphe ?
Many believe presence of raphe accelerates degeneration as leaflets have rough surfaces . Still , BCAV with raphe has less coronary anomalies and aortic root pathology .
Presence of raphe indicate relatively a minor embryological defect , as the fault is in the failure to divide after the formation of analgen , while BCAV without raphe imply lack of development of analgen itself . This is expressed in the coronary sinus anatomy and aortic root dimension and orientation .
So currently it is welcome to spot a raphe in the patient point of view .Echo cardiogram is notoriously unreliable to diagnose raphe. Once degeneration process sets in , it is almost impossible to recognize the presence or absence of raphe .
* Please note ,tricsupid aortic valve with eccentric leaflet closure shares a close pathological relationship with BCAV. Premature degeneration , (AR more common than AS here ) .This entity will be discussed separately later.
Image courtesey
Part of the Image (The valve) is adopted from Yale university Image Bank .
Read Full Post »