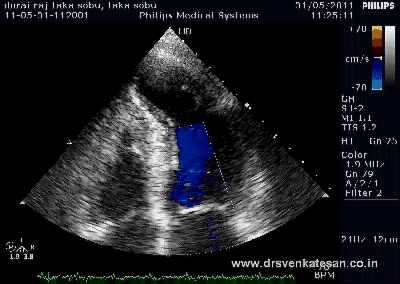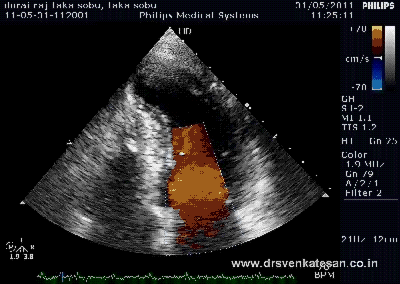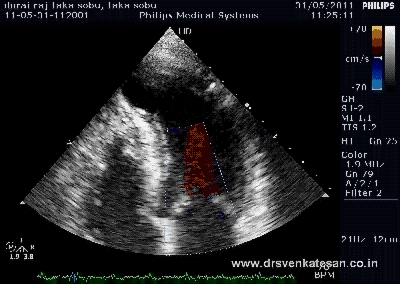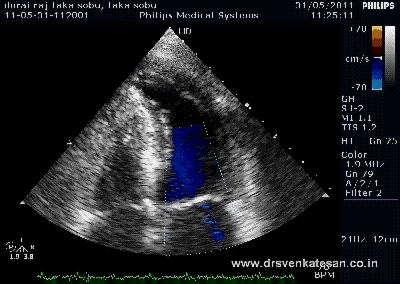
Interventions in Eisenmenger syndrome or severe PAH in left to right shunt continues to be a major diagnostic issue.The challenge lies not only in assessing whether the progression of PAH can be prevented by blocking the left to right shunt , but also to assess it’s impact on survival.
The factors involved are
- Pulmonary artery pressures
- Pulmonary blood flow
- Pulmonary vascular resistance
- RV function
- Co-morbid /general condition of the patient
While cardiologists worry more about LV , surgeons have different issue . In left to right shunts with PAH RV function bothers them more , as the high pulmonary artery pressure may never allow the surgeons to come off the pump , once the decompression provided by ASD/ VSD is removed
How relevant is Ohm’s Law in complex shunt with leaky valves and bidirectional shunting ?
The fundamental hemodynamic equation is derived from Ohm’s law .How relevant is Ohm’s law in Eisenmenger is not clear. For decades we have been using complicated calculations with many presumed and assumed parameters. The calculation of effective pulmonary blood flow in bidirectional shunt may be most complex equation in clinical cardiology. One can only imagine how one error could amplifies the other.

The hemodynamic equivalent of Ohm’s law states
R = Pressure / Flow .The current thinking is If the PVR is between 6-8 it is operable .
Is it really that simple ?
We know pressures can be measured with a fair degree of accuracy . Flow and resistance are subjected to change in a moment to moment basis .They are determined by a gamut of neural and humoral factors.
Ironically , we are not yet clear , whether flow determines the pressure or pressure determine the flow .
The right heart blood flow can get complicated by not only bi-directional shunt but also by pulmonary and tricuspid regurgitation ,
There is a huge perception problem here . We are tuned to think , reversibilty of PAH is same as operability of shunt lesion . Definitively not ! This is the reason why there is a vast difference in ultimate outcome with little correlation with PVR !
In Eisenmenger physiology , critical decisions regarding surgery are made outside the cath lab
- Good clinical acumen,
- A meticulous echocardiography
- Hard parameters like pulmonary artery diastolic pressure and pulse pressure
- Above all a harmonious Cardiologist – Cardiac surgeon team is vital to plan this complex surgery
So, now it would seem cath studies are primarily done for academic pursuit , and it rarely helps in genuine decision-making process.
The following table synthesized in our hospital (Mainly with clinical data ) can be a useful tool.

Reference: Learnt in the bedside from poor children of India
We had a situation like this . A patient was in class 3 or 4 and calculated PVR was less than 6 Wood units what will you do ?
Never give importance to numbers . These patients will 99% of times won’t survive a shunt closure surgery.
Future development
With the availability of modern drugs like Nitric oxide, prostocyclins, Sildenafil analogues medical management has a potential to improve upon surgical results. Unfortunately large studies are not possible in these population . In the surgical front, fenestrated VSD closures peri-operative intensive nitric oxide show some promise.
Final message
I think we are about to say a final good-bye* to oxymetry ( or even cath study ) in the work up of PAH due to shunts.
*Still, pressures of right heart chambers and pulmonary artery is vital .Echo can not be expected to provide accurate measure of PA pressure .(Even though there some echo studies available to calculate qp/qs and PVR non invasive)
Reference
Pulmonary artery pulse pressure : A simple parameter to assess reversibility of PAH
Read Full Post »