LBBB is a common ECG abnormality .The ECG is so classical , no one ever misses the diagnosis. But , what we miss often is the significance of it .
What is the cause of LBBB in a given patient is much more important than the LBBB itself !
Though the commonest cause of LBBB is a benign one (Pure electrical defect without any valvular , myocardial or ischemic heart disease ) , it is prudent to rule out organic LBBB . The term organic here refers to structural or ischemic etiology .
LBBB & STEMI
To diagnose STEMI in LBBB we have the much famed Sgarbosa criteria .It is a too popular to forget in spite of it’s limited utility . Applying it in an emergency is not easy exercise . Clinical prediction , cardiac enzymes are safe and could be more accurate. Thanks to ACC guidelines , it has simplified our task .You are encouraged to thrombolyse all cases of new onset LBBB* if clinical picture is strongly suggestive of ACS.(*The term “presumably new” onset LBBB was included , implying it is better to err on the safe side )
LBBB & NSTEMI
No one knows how to recognise NSTEMI in LBBB. Logic would say, primary ST depression might occur. How sensitive it is , and which lead to look for is not known.
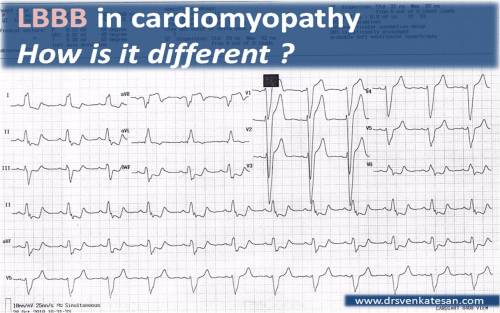
LBBB in DCM
Here is an ECG of a patient who came to our OPD absolutely asymptomatic for a routine review . He is been diagnosed as a case of dilated cardiomyopathy with 30% EF and no evidence of ongoing ischemia.If the history is not known he would have been diagnosed as a ACS.
To diagnose cardiomyopathy in LBBB we have no specific criteria. But we have found the following useful
- Extreme left axis deviation > Minus 45-60 degrees/AVR positivity
- Low voltage QRS , especially in limb leads
- ST depression is more flatish than the typical secondary ST/T changes of LBBB
- QRS notching or slurring either in the r wave or s wave.
- Atrial abnormalites as evidence by wide P waves.
- Associated VPDs
Further inputs are welcome to differentiate organic from benign LBBB
Counter point : When we have facility to do bedside echo , why should we scratch our heads ?
Do not waste time , do a spot echo . . .
Echo can be very useful in ruling out cardiomyopathies and old MI.But remember , echocardiography is unpredictable to detect acute septal MI in the presence of LBBB , as paradoxical motion of IVS tend to mask the ischemic wall motion defect .A simple clue is normal systolic wall thickening will be observed in benign LBBB , in spite of paradoxical motion .This thickening appears as post systolic beaking that face posteriorly . In STEMI and LBBB thinning or absence of thickening is expected.