A young man aged around 40 years, had a STEMI was promptly thrombolysed in a small hospital located about 40 KM away in the suburbs of my city Chennai. They did an awesome job of saving the patient life and salvaging the myocardium.
Now begins the story . . . one of the non-medical person who is the owner of the hospital has an unfortunate working business relationship with a frighteningly big nearby hospital which had signed a memorandum of irresponsible understanding . It demanded any patient who arrives in the small hospital with MI should be transferred at earliest opportunity to them.
So, an ambulance was arranged and the patient (with a fairly well reperfused heart ) was shifted in an emergency fashion . It reached desired destination after nicely chugging along the choked chaotic Chennai evening traffic for 45 minutes.
The guy was taken directly to cath lab through the side doors to perform a second salvage procedure on a successfully opened IRA. Young cardiology consultants in designer cath suite welcomed the smiling ACS patient to their posh new lab .Did few rapid radial shots, mumbled among themselves for few minutes, decided to stent a minimal LAD lesion for a patient who was in zero distress with well-preserved LV function.
*The relatives of the patients were curious when they were asked sign a fresh set of consent which elaborately mentioned about possible life risk during the procedure.
The patient’s wife was clearly amused and she pointed out to the superior cardiologists about the earlier briefing by the Inferior freelance cardiologist who treated him in the previous hospital. She recalled , “I was told in confident terms that Initial thrombolysis has been spectacularly successful and bulk of the treatment is over and risk of complication has dramatically reduced”.

Then why is this distressing risk taking story again , she asked ?
The doctors hurriedly explained ,”this procedure is different. We are sorry to say we have no other option but to add further risk to you” ! but , its all for your good !
Why should I ? If the initial lysis is very successful why do you want to meddle with it again ?
No Madam , you are ill-informed , you can’t talk like that .This is what modern science is all about. Leave the professional decision to us. We need to check immediately whether the lysis is really successful .We can’t rely on the ECG.Further, true success lies in stenting the lesion as we fear the ill-fated site may close again.We are taught to practice protocols based on standard scientific guidelines. This hospital has highest rating in-terms of quality care. That’s why we got updated ISO 2000 NABH accreditation
The women who is a soft ware engineer was smartly and scientifically silenced in 5 minutes flat !
Post-amble :
What happened to the patient then ? (When you fear something it happens is in’t the Murphy’s law ?)
The apparently asymptotic and comfortable patient had uneventful PCI. A long drug eluting stent was implanted in recanalized lesion in LAD with around 30 % narrowing that ended with an innocuous looking diagonal pinch. The procedure was uneventful , however next day he developed some fresh ECG changes and chest pain . The worried team took him for another angio found stent was patent But , ultimately after a stressful 3 days of stay , some thing went wrong he ended up with new LV dysfunction.He got discharged fine with a caution that , his stent needs to intensively monitored for the next 1 year since technically he had recurrent ACS !
Lessons we don’t learn from such cases.
When two procedures are done to accomplish the same aim (Reperfusion) , but with differing success rates, expertise, time ,and unpredictable hazards , the benefits from them may not add together. There is clear knowledge deficit here. Scientific data can never provide fair answers to these questions as all real life cofounders can never be recreated in study population.
While we expect 1+1 to become two in pharmaco-Invasvie strategy ,one should realise it may end up with either zero or even – 2 .
1 -1 = 0
-1 + (-1)= -2 ?
Learning cardiology from lay persons
The patient’s shrewd wife threw this question ,
After two modes of re-perfusion done sequentially in my husband’s heart , at a total cost of Rs4.5Lakhs Why he is still left with significant LV dysfunction (Which was around 40% EF.)
The query raised by the lady appeared much more crucial and logical than the ones discussed in many top-notch live interventional workshops we attend every few months!
As usual , I started mulling over the issue. There is something wrong with the way , we understand the pharmaco invasive approach-PIA .You go with it only if initial pharmacological approach has failed.
Of Course ,there is one more modality possible ie Pharmaco -Angio strategy where in, you look at the coronary anatomy and take a call ! This sounds good , the only issue is taking a right call ! My experience suggests wrong calls are the rule and exceptions are rare. Then a whole new issue erupts about all those non IRA lesions
Final message
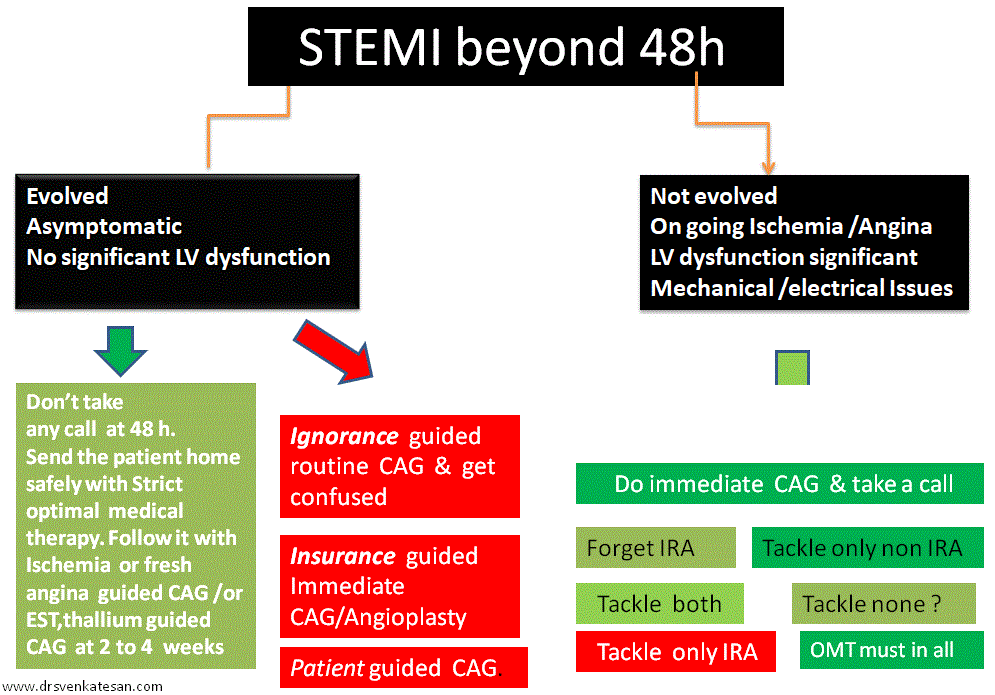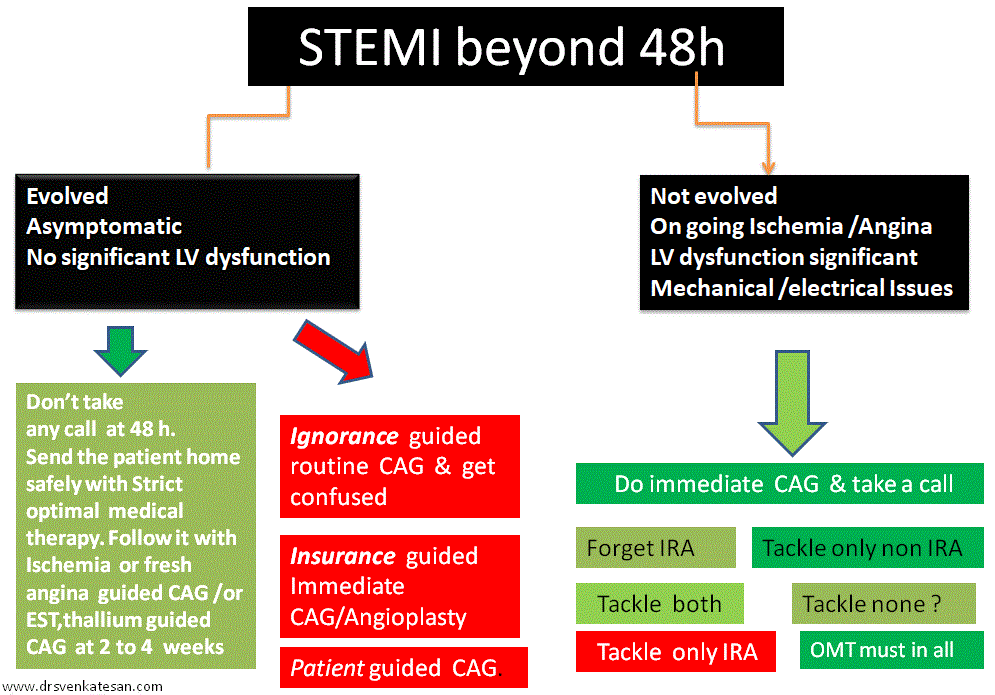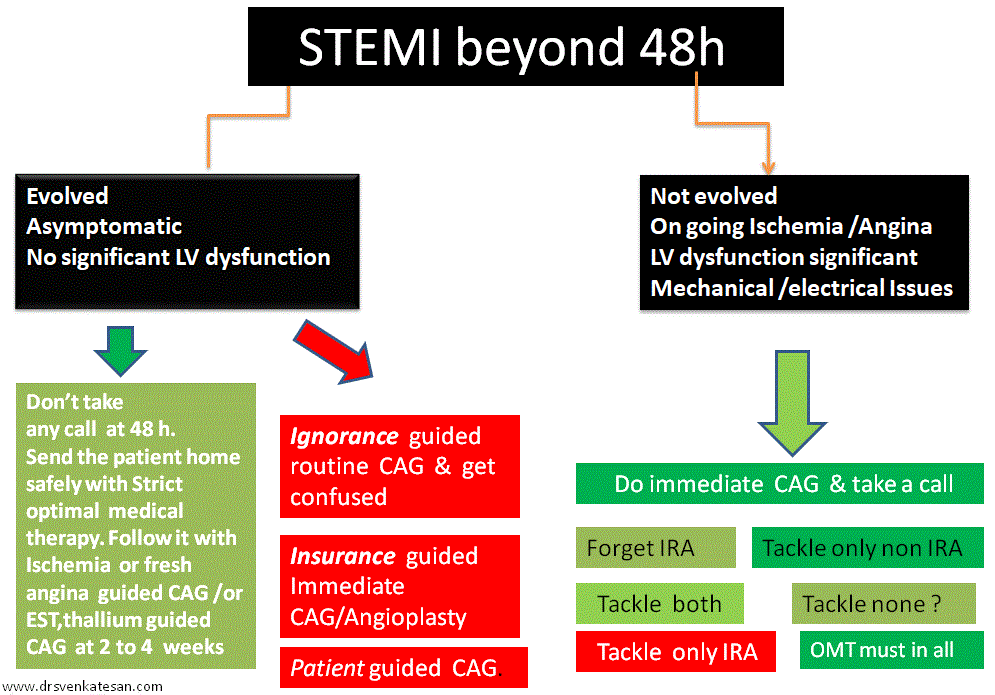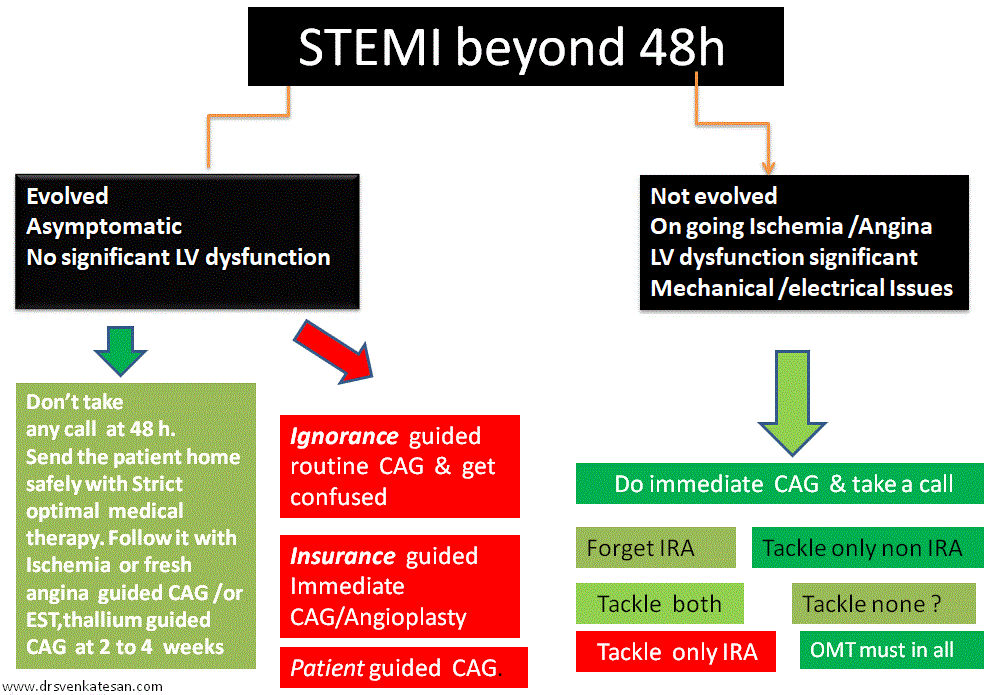
So, til we have gain complete self-control over our evolved ignorance and evolving knowledge , it is better to follow this proposed funny new ACS algorithm called “Pharmaco -non invasive” approach (PNIA) in asymptomatic ACS patients who have had apparently successful lysis.
*Please note, Incidentally PNIA actually refers to simple good old traditional stand alone thrombolysis.
Counter point
No one can deny Interventional cardiology carries a risk of untoward effects.Don’t blow this out of proportion. Do you know, how many lives have been saved by routine Pharmaco -Invasive approach ?
I am not sure , my experience may be limited.Let me ask the readers. Is routine PIA is warranted in all asymptomatic , successfully lysed STEMIs ?
Read Full Post »













ORBITA trial : First let us do some harm . . . second , we shall . . !?
Posted in Cardiology -Interventional -PCI, Cardiology -Technology, Cardiology -Therapeutic dilemma, cardiology -Therapeutics, Cardiology -unresolved questions, cardiology journal club, cardiology wisdom, Medical education, Medical ethics, Uncategorized, tagged ABUSE OF STENTS, ACC AHA ESC ORBITA GUIDELIES, CHRONIC STABLE ANGINA GUIDELINES, drsvenkatesan, HOW ORBITA TRIAL WILL CHANGE MY PRACTICE, INAPPROPRIATE USE CRITERIA AUC STENTS, LANCET ORBITA STUDY, ORBITA COURAGE BARI2D FAME 2, ORBITA IMPERIAL COLLEGE, ORBITA study, ORBITA TRIAL LANCET, ORBITA trial review and comments, ORBITA VS COURAGE, reviewing ORBITA trial study critically, TCTMD 2017 ORBITA, WAHT WE LEARN FROM ORBITA STUDY on November 6, 2017| 2 Comments »
Cardiologists at confused cross roads !
Perils of limited Intellect & Infinite greed
When not so appropriately trained cardiologists do Inappropriate things “use becomes misuse” . . . then, it won’t take much time for science to become total abuse. That’s what happened with the murky world of coronary stents .No surprise, it’s time to firefight the healers instead of the disease !
Now ,Comes the ORBITA study . Yes , it looks like a God sent path breaking trial that spits some harsh truths not only in cardiology, but also in behavioral ethics .Let us not work over time and hunt for any non-existing loop holes in ORBITA. Even if it has few, it can be condoned for sure as we have essentially lived out of flawed science for too long Injuring many Innocent hearts !
Yes , its enforced premature funeral times for a wonderful technology !
GIF Image courtesy http://www.tenor.com
Meanwhile, let us pray for a selective resurrection of stenting in chronic coronary syndromes and stop behaving like lesser professionals !
Postamble
Extremely sorry . . . to all those discerning academic folks , who are looking for a true scientific review of ORBITA , please look elsewhere !
Rate this:
Read Full Post »