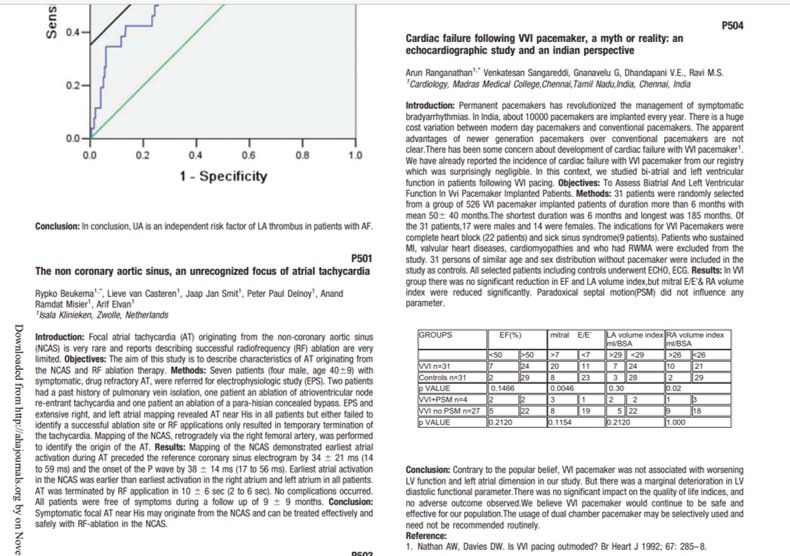
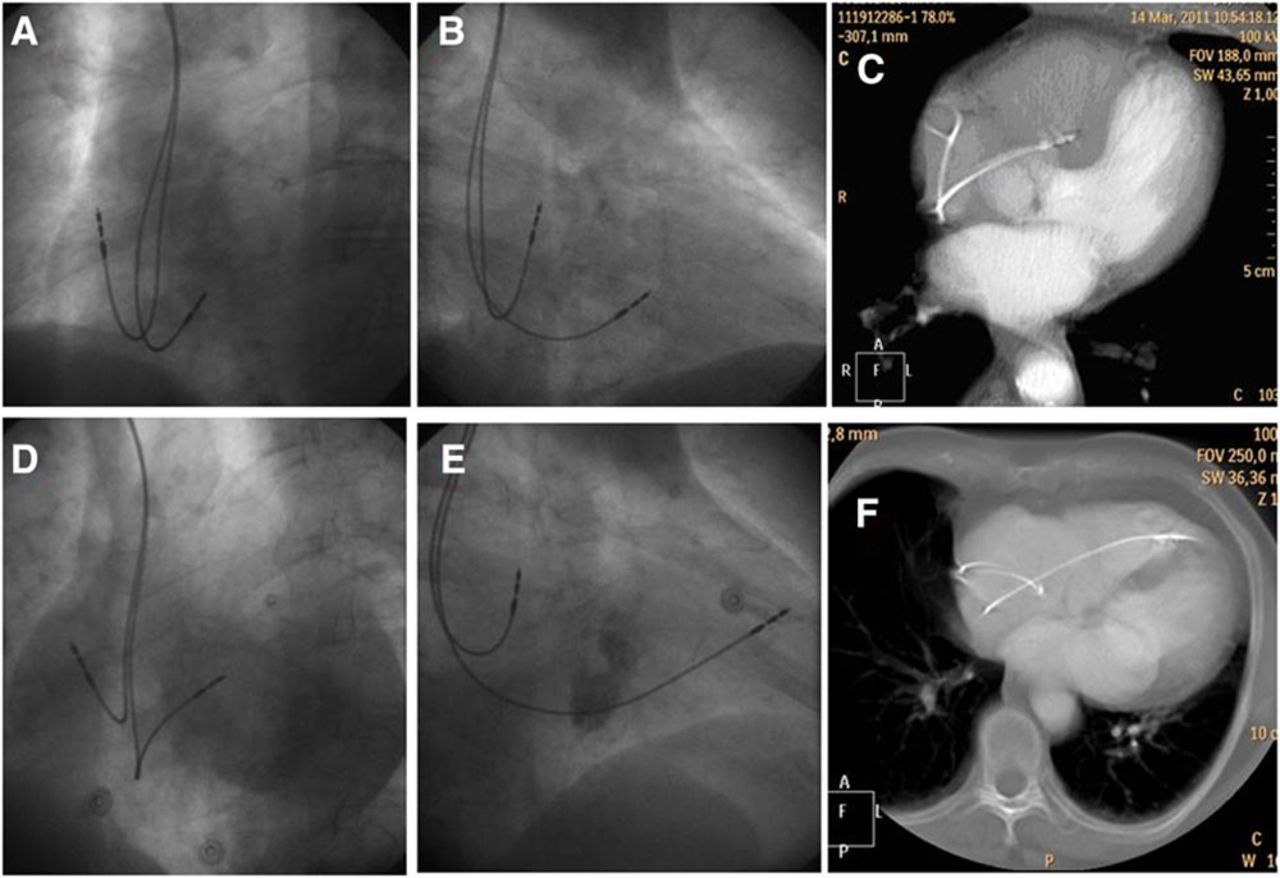
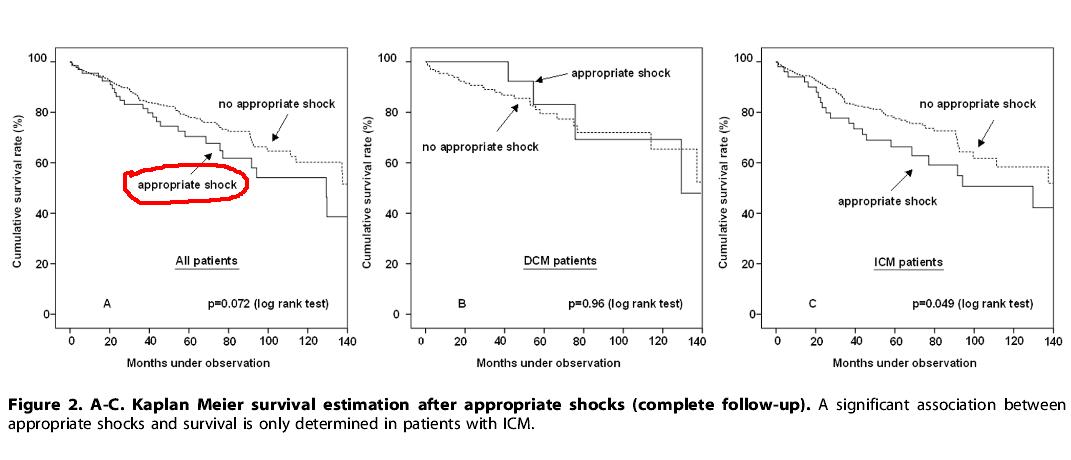
We have been taught right from first year cardiology residency how to trouble shoot a pacemaker .It has been a real complex thing for us. Now looking back ,all the troubles we took to understand seems to be redundant.Here is a summary of my thought process on the issue. It can be approached with reference to time, symptoms and ECG features. With due respects to all those brainy hardworking EP experts , I have taken few academic liberties!
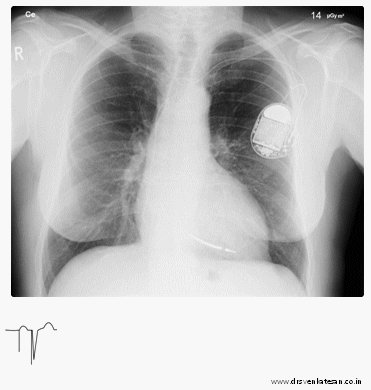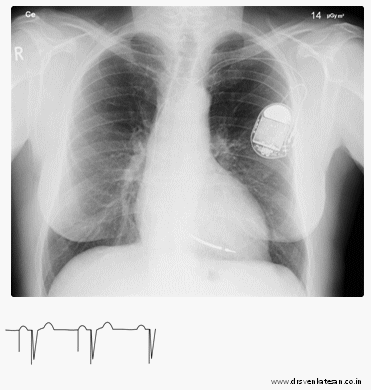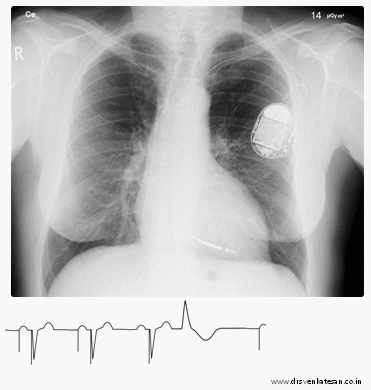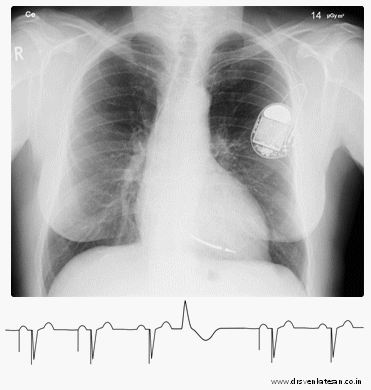
Timing
- Within 24 hours -100% technical or procedural Issues , like lead dislodgement/Screws and nuts.
- Within 1-2 week – Again technical , Pocket issues , Infections.
- Within 6 months – Benign pacemaker syndrome ,Threshold settings, Scars
- After first year – Generally Issues are rare , Lead issues , Associate disease progression.
- Beyond 8-10 years /Near end of life – 95% Energy depletion leads issues .( Please note , pacemakers do not stop all of a sudden it has a intrinsic end of life indicators .We have to look for it. May be ,we can expect a warning siren in the future ? )
Symptoms
- Vague dizziness – Pacemaker syndrome ? Anxiety ?
- Near syncope – Show some concern (For many , Impending true syncope is a non existent entity )
- True syncope – Real emergency*
* Syncope can be unrelated to pacemaker but always consider them electrical unless proved otherwise . Few patients may continue to have significant symptoms in-spite of normal pacemaker parameters. This would mean , the original symptom for which pacemaker was put is not related to the Brady-arrhythmia .It could suggest alternative hemodynamic explanation like vaso-depressive component of vagal syncope ,autonomic dysfunction , orthostatic intolerance or a coexisting neurological /systemic condition.
**Never forget syncope is not an exclusive symptom of bradycardia .A new onset tachycardia , which is either a part of brady- tachy syndrome or separate arrhythmia can continue to provoke the symptom.
Gross ECG findings
Bradycardia /Often implies back to original rhythm – Indicates real trouble . Since ,in a paced patient HR cannot be less than programmed rate of 70.
Tachycardia -No spike.( Not to worry ?) A common situation if the original indication was sinus node dysfunction . Many of them are in own sinus rhythm or AF . Just ensure spikes reappear when the rate falls below 70 . If the rate never goes down , what to do ? Try a carotid massage or observe a nocturnal ECG or call analyst and increase the rate to document pacing . (In DDD mode we have a rare PM mediated re-entrant tachycardia , which is mainly used to grill cardiology fellows in their board exams with all those PVARP stuff !)
Simple pauses – Any pause more than the pacing interval is a definite concern .
Spikes more than QRS – Indicate capture failure.
No spikes (Can be so benign to ultimate danger )
- No spikes , but excellent own rhythm – Good functional SA node
- Regular spikes ,but intermittent own rhythm or only random spikes with good own rhythm – Needs bedside hairsplitting and EP assistance !
- “No spikes -No Own rhythm” -Most dangerous .Sudden lead issues or hyper sensing .(Emergency switch off by magnet application before inserting temporary pacing advised )
* Anatomical issues like lead dislodgement , fracture , compression , perforation are to be ruled out in every pateitn with intermittent capture or failure .This is done by combinations of imaging as well physiological assessment.Dislodgement must be visualized .The term micro dislodgement may not exist.
Other Investigations
- X ray
- Echo for any new structural lesion (RA,RV dilatation , TR RV clots or vegetation )
- Holter
- Event monitors ,Loop recorders.
Pacemaker analysis
- Battery life ( Very important parameter .Usually around 10 -12 years.Unexpected early drain can occur.)
- Threshold (Most failure to capture associated with high threshold Note :Threshold will be normal in battery depletion Acute threshold can increase marginally .Should be reasonable other wise battery will drain.New protocols like auto capture and managed pacing will help optimal threshold
- Impedance – Normal in battery depletion , dislodgement and exit block, Increased in lead fracture and loose screws.Decreased or lost in insulation failure.
Management
The principle of management are simple. Few logical questions ,
- Is the pacemaker generator is alive and has has enough energy ?
- Are the leads okay ?
- The problem is in the settings ? can it be rectifies by the programmer
- Or should we replace the pacemaker ?
Technical jargon like under sensing , over sensing or no sensing , fusion beats , micro dis-lodgement etc are important for academic reasons . We may talk any thing , realistically , what the ventricle want is a non stop heart beat every second or so !
Emergency
Bradycardia – Insert a temporary pacemaker /Call the analyst /Inform the electrophysiologist /Senior cardiologists /(Please realise , some fellows can be better than the personnel mentioned above in tackling emergencies !)
Tachycardia : Native or machine induced ?
Native – Mostly safe , Ignore or treat with drugs.
Machine induced :(very rare) Switch of the pacemaker . No off switch available as in a mobile phone ? *What to do ? if unclear about the whereabouts tachycardia origin . If hemodynamically unstable no harm in shocking .Nothing will happen .Call the EP guys on hot line and decide.
Elective symptom guided.
- Asymptomatic -Normal ECG : Reassure and send home.
- Vague symptoms -Do Holter and Observe
- Syncope -Normal ECG needs extensive all system investigation.
- Syncope -With pauses /Bradycardia /Asystole – Ironically ,decision making is easier. Temporary pacing is the ultimate savior. Later , check the lead, generator .One may need to change either one or both of of them.
** While the above principles apply for both single and dual chamber pacemakers , the later doubles our thinking burden . While atrial tracking is a great technological advancement , what to do with those sensed event can be really tricky .The response of ventricles and the AV intervals can be tentative at times. Cross talks from unexpected atrial and ventricular arrhythmia can occur. Further , mechanical atrial lead issues are far more common . When confronted with recurrent atrial lead related problems , one simple solution is silently convert the mode to single chamber VVI mode.
Final message
Pacemaker trouble shooting appears complex at the first look .It’s all common sense.Thinking with simple state of mind and being clear about the intended goal is vital. Electrical intricacies are tough to understand but most situations do not require them. However ,If the initial indication was for complete heart block one has to be very alert.
Principles of medicine argue us to make an exact diagnosis before treating . But,realise this is rarely possible or even desirable in emergency .Curiously , most pacemaker troubles can be solved successfully without making a proper trouble shoot !
If we can summarize in one line , a prompt emergency back up temporary pacemaker insertion is key to management most of the serious pacemaker related problems.It ,not only tackles the emergency , buys time till we decode the real problem . . . if we wish to !
Related article.
Role of magnet application in pacemaker trouble shoot
Read Full Post »