“Every Interventional Cardiologist, realistically, need to be a preventive neurologist too!”
The concept a permanent ascending aortic porous membrane filter (PAA-PMF) is an extrapolation of the idea of mechanical thrombus capture, as proven by IVC filters for venous embolism prevention . Also we do have and temporary intra-aortic filters like Sentinel , Embol-X for arterial particulate capture.
Device Concept
The PAA-PMF would feature a self-expanding nitinol frame, with a fully porous head end. The device can be heparin-coated polyester or polyurethane mesh membrane, deployable via 12-14 Fr femoral sheath, similar to IVC filter designs but should be optimized for aortic pressures. Suggested pore size of 100-125 μm targets >100 μm emboli, akin to Embol-X filtration efficacy in capturing 95% of particulates (atheroma, fibrin) during aortic declamping. The essential requirement is that the porous membrane should not create an impedance gradient. How feasible it is, to be tested. Conical shape, the radial force will ensure good ascending aortic wall apposition.
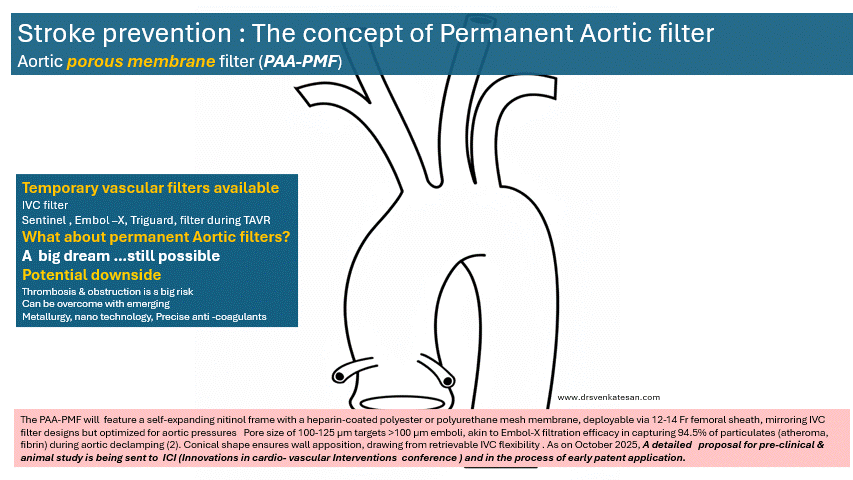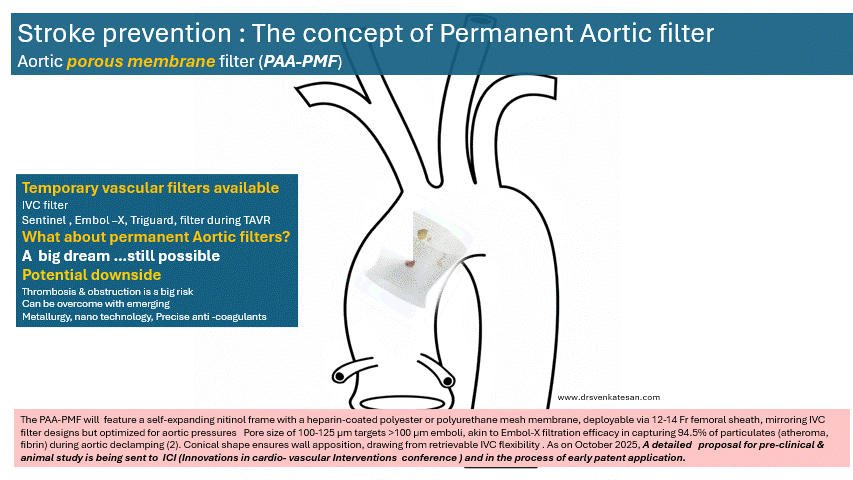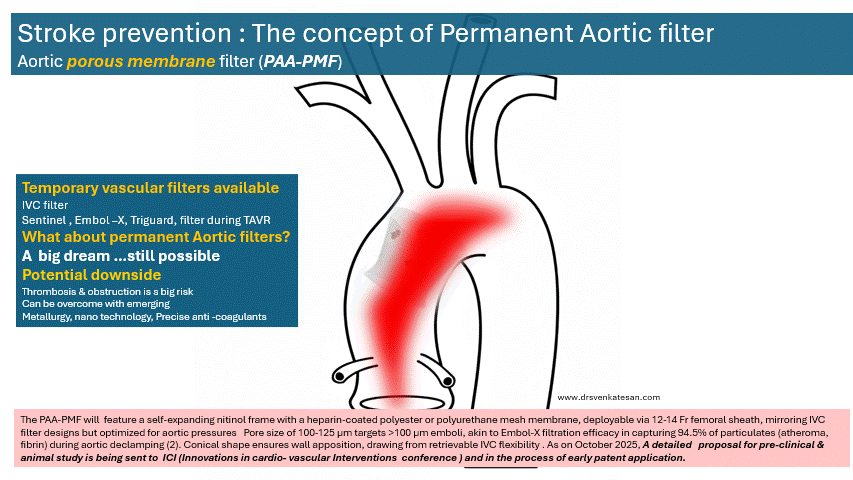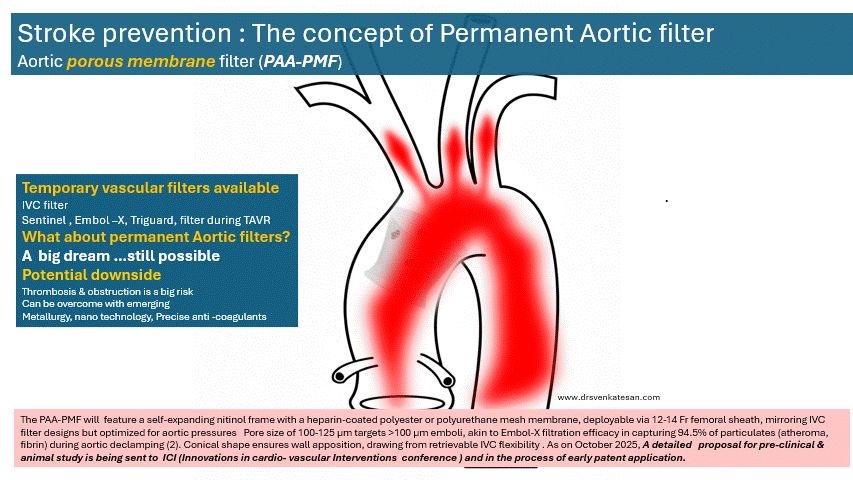
Device location site
Site of placement is critical. Proximal ascending aorta, 2-3 cm distal to sinotubular junction/proximal to brachiocephalic trunk, as in Embol-X for maximal cardiac/aortic debris interception without coronary/arch compromis
Potential indications
(Only in patients with very high risk of cardioembolic stroke)
1.Chronic stroke reduction in patients with MVR/AVR/TAVR/MAVR
2.High-risk mobile LV mural thrombus
3.Chronic AF with visible and invisible clots in LA
4..High-risk procoagulant conditions with recurrent embolism
Definite Risks
*Occlusion and hemodynamic compromise is the most crucial issue. However, when compared to the incidence IVC filter clogging, the high pressure aortic flow is likely to self-wash the device (as happens in a prosthetic aortic valve)
Trapped emboli may enter into coronary circulation is a possibility. Putting a filter at ascending aorta precludes left heart catheterization.
*Migration , Hemolysis are other expected complications.
Intense anticoagulation would be required to prevent occlusion of the filte . (Still, stopping it temporarily doe not not increase the risk of stroke)
Final message : Is it Worth for a Preclinical trial ?
We do have temporary aortic filters. The concept of permanent or semi-permanent filters is largely theoretical, with potential risks being more than benefits. The device can take care of only cardio-aortic embolic stroke.
However, considering so many complex, risky intracardiac and intravascular devices being tested on a daily basis, it is not a big deal for the current generation of interventional cardiologists to try this.
More than our interventional appetite, we really need a device that prevents stroke in a permanent fashion. It is definitely worthy to do initial studies in a porcine model. Would be glad , if Edwards, Abbot or Medtronic and other new Innovators respond to this.
References
- Shammas NW, et al. Intra-Aortic Filtration: Capturing Particulate Emboli during Cardiopulmonary Bypass. NIH. 2004. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC1351822/
- Shammas NW, et al. Embol-X Intra-Aortic Filtration System: Capturing Particulate Emboli in the Cardiac Surgery Patient. NIH. 2004. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC4682540/
- PCI Mag. Revolutionary Anti-Thrombogenic Coating for Stents Promises Safer, Faster Healing. 2024. Available from: https://www.pcimag.com/articles/112641-revolutionary-anti-thrombogenic-coating-for-stents-promises-safer-faster-healing
- Kaufman JA, et al. Radiologists’ Field Guide to Retrievable and Convertible Inferior Vena Cava Filters. AJR. 2019. Available from: https://ajronline.org/doi/10.2214/AJR.19.21722
- Cleveland Clinic. Vena Cava Filters: Purpose & Placement. 2025. Available from: https://my.clevelandclinic.org/health/treatments/17609-vena-cava-filters
- Bilal H, et al. Complications of Inferior Vena Caval Filters. NIH. 1997. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC3036364/
- Alpaslan M, et al. Embolic Protection Devices in Transcatheter Aortic Valve Implantation. NIH. 2025. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC12194329/
- Almanza DC, et al. Comparative Review of Large Animal Models for Suitability of Cardiovascular Devices. IJMS. 2024. Available from: https://ijms.info/IJMS/article/view/763/1645
- Mohammadi H, et al. Simulation of blood flow in the abdominal aorta considering hyperelasticity of the wall. J Carme. 2021. Available from: https://jcarme.sru.ac.ir/article_1223.html
- Ketha S, et al. Comparative Review of Large Animal Models for Suitability of Cardiovascular Devices. IJMS. 2019. Available from: https://ijms.info/IJMS/article/download/763/1644?inline=1