Truely a great demonstration of life saving Mitra clip procedure.
Found this from
Truely a great demonstration of life saving Mitra clip procedure.
Found this from
Posted in Uncategorized | Tagged acute mitral regurgitation, left atrium, mitra clip, v waves in mr |
Can a bedside echocardiogram help rule out STEMI in patients with suspicious ECG?
No, it can’t (Though, it may be tempting to use a rapid echo to look for wall motion defect to rule out ACS )
If your answer is No, probably you don’t need to read any further in this post.
Diagnosis of STEMI* is based on
*Please note, two of the most popular investigations namely Echo and Coronary angiogram are missing in the list.
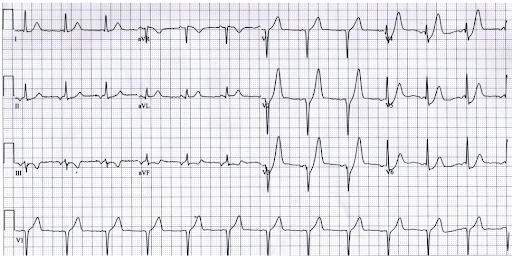
A middle-aged man with chest pain. Can an echocardiogram help you confirm STEMI here? Most likely not. It may still be an evolving STEMI. But, observation, serial ECGs, and Troponin is the answer. (ECG -Source http://www.emdocs.net/hyperacute-t-waves/ )
Though, echocardiography, a great noninvasive imaging tool at the point of care, it stands almost helpless in the diagnosis of the commonest cardiac emergency ie ACS. It can be called as mother of all paradox even visualizing the myocardium directly with high-quality imaging will not tell you, whether there is ongoing ACS or not.
Relying on wall motion defects without diagnostic ECG changes to diagnose STEMI can be misleading for the simple reason, both unstable angina and old MI can be a 100 % confounding effect. Similarly, absence of WMA doesn’t rule out an evolving STEM(Apart from the bizarre behavior of Ischemic cascade, In the early hours only subendocardial wall stress is noted, that is not good enough to cause visible WMA)
Role of CAG in the diagnosis of STEMI
Urgent CAG is an easy way out in confusing coronary conundrums. But, unless you know the background info even a CTO can be mistaken for ATO/ STEMI . So it is essentially new ST/T shifts (corroborated with CAG) will be the guiding force.
Final message
The humble Clinical examination and ECG will prevail over all other modalities in the diagnosis of ACS. Mind you, ECG findings are built within the diagnosis of myocardial infarction ie STEMI (ST-segment) so can’t diagnose it with Echo. Further, an indication of thrombolysis or PCI goes with ECG finding only.
Counterpoint
*Having said that, there is a key role for echocardiography in the ER to diagnose alternate cardiac emergencies like Aortic dissection, Acute pulmonary embolism or ACS mimickers like HOCM, etc. Further, echocardiography is used in a big way, in the risk stratification or identifying complication during the ACS management.
Exceptions
In patients with atypical presentations, pacemaker rhythms, LBBB, especially elderly, comorbid, ECG can be quiet normal or non-diagnostic. Here, echo and angiogram may have some adjunct diagnostic roles.
What about newer echo Imaging modalities?
** There has been a suggestion, that regression of Global longitudinal strain(GLS) or new-onset regional loss of myocardial strain, detected by speckle tracked echo is a powerful and the earliest sign of myocardial ischemia.
A potential tool to rule out ACS by Echo -Global /Regional longitudinal strain (GLS) still trailing behind ECG.
GLS is proposed to be used in coronary units to rule out ACS. In spite of its Initial promise, we understand it has not been accurate enough to be included as criteria to diagnose ACS . So, as of now, it appears unlikely for echo criteria to be included in the diagnose of STEMI.
Posted in Uncategorized | Tagged diagnostic criteria for stemi, gls in stemi, role of echocardiography in diagnosis of acs stemi nstemi, wall motion defect in stemi by echo |
Who is a doctor? Where are they made?
I haven’t clearly understood the true meaning of customary Dr tag, my name carries for more than 3 decades, till I saw this. Wish, this video is played to all young medical students on their graduation day.
I am realizing with guilt, it requires a Holywood movie buff to remind us the true meaning of the famous WHO – definition of Health, done in the most holistic fashion in the year 1948.
Health is a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity.
So, technically, whoever serves to improve these three components and alleviate human suffering becomes a doctor.
Happy to share this on July 1st, the official Doctor’s day in India in memory of the Bharat Ratna Dr.B.C.Roy of Bengal.
Reference
The clip is from the movie Patch Adams, Directed by Tom Shadyac. A Hollywood celebrity movie maker, Virginian professor of communication turned philanthropist, now retired to a minimalist life. He is also known for his famous documentary I am that talks about the problems faced by the world. Though his works are much appreciated, I must say, they are underrated. Deserves more than an Oscar for communicating his thoughts on the medical profession perfectly and for social equality.
Posted in Uncategorized | Tagged ethics in medicine, hippocrates otth on medical education, Iam documentry Tom Shadyac, medical education, Patch adams, Tom Shadyac |
It’s halfway way through 2020 , still miles to go.
Welcome to a non academic break.This 3 minutes video definitley helped, amidst the paronia.
Wish, we can retire peacefully and join this family.
Posted in Uncategorized |
That’s how the title sounded to me, when I happened to read this paper from the reputed Circulation journal.

Even in the serene non-covid days, primary PCI rate in most countries is at best 10 % and thrombolysis* is the only savior in STEMI.(*with or without Pharmaco Invasvive )
It’s Covid times you know, can’t take science for a ride. Let us all take a pledge, in this deadly pandemic to increase pPCI rate to atleast 50% and ditch that dedicated, trustworthy , uncomplicated all weather friend !
Reference
https://www.ahajournals.org/doi/10.1161/CIRCOUTCOMES.120.006885
Posted in Uncategorized |
FFR is based on the hemodynamic principle of pressure drop when fluid or blood flows across a narrowed segment (similar to Bernoulli principle). If there is more than 25 % pressure drop across the lesion under maximum hyperemic condition (or steady-state) it is counted as significant.(FFR is .75)
Now, if the distal vessel is supported by collaterals, what happens?
When a vessel in question, is supplied by well-formed distal collaterals, it will prevent this pressure drop and hence lesion is underestimated. Similarly, if the donor artery has a suspicious intermediatory lesion, the FFR across it is falsely low, and overestimates the lesion.The distal pressure drop here is not because of the lesion but due to rapid collateral flow into the recipient artery.
Let us take a hypothetical case. In a post anterior MI 90 % LAD lesion receiving well-formed collateral from RCA which also has a 70 % proximal lesion.
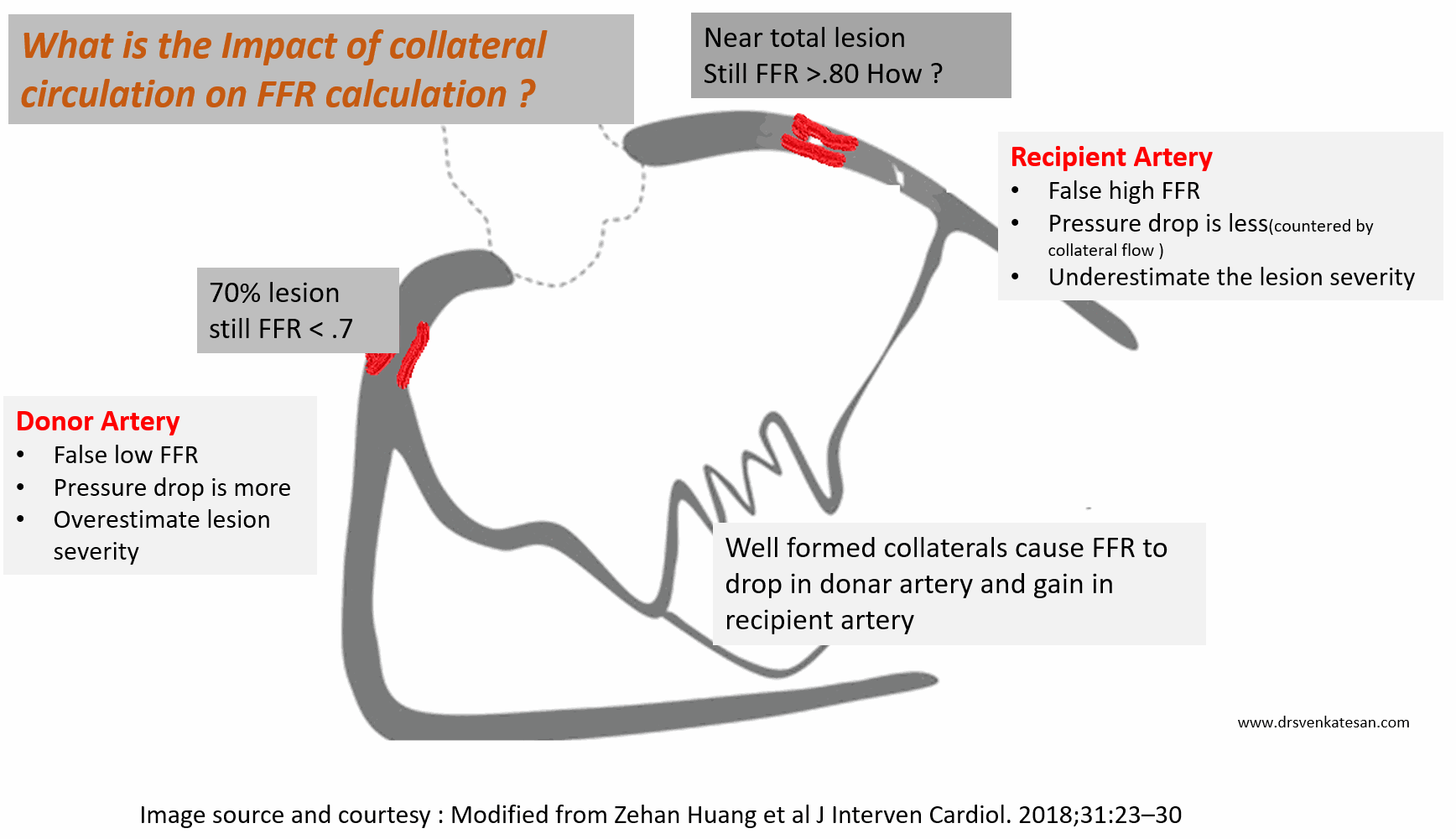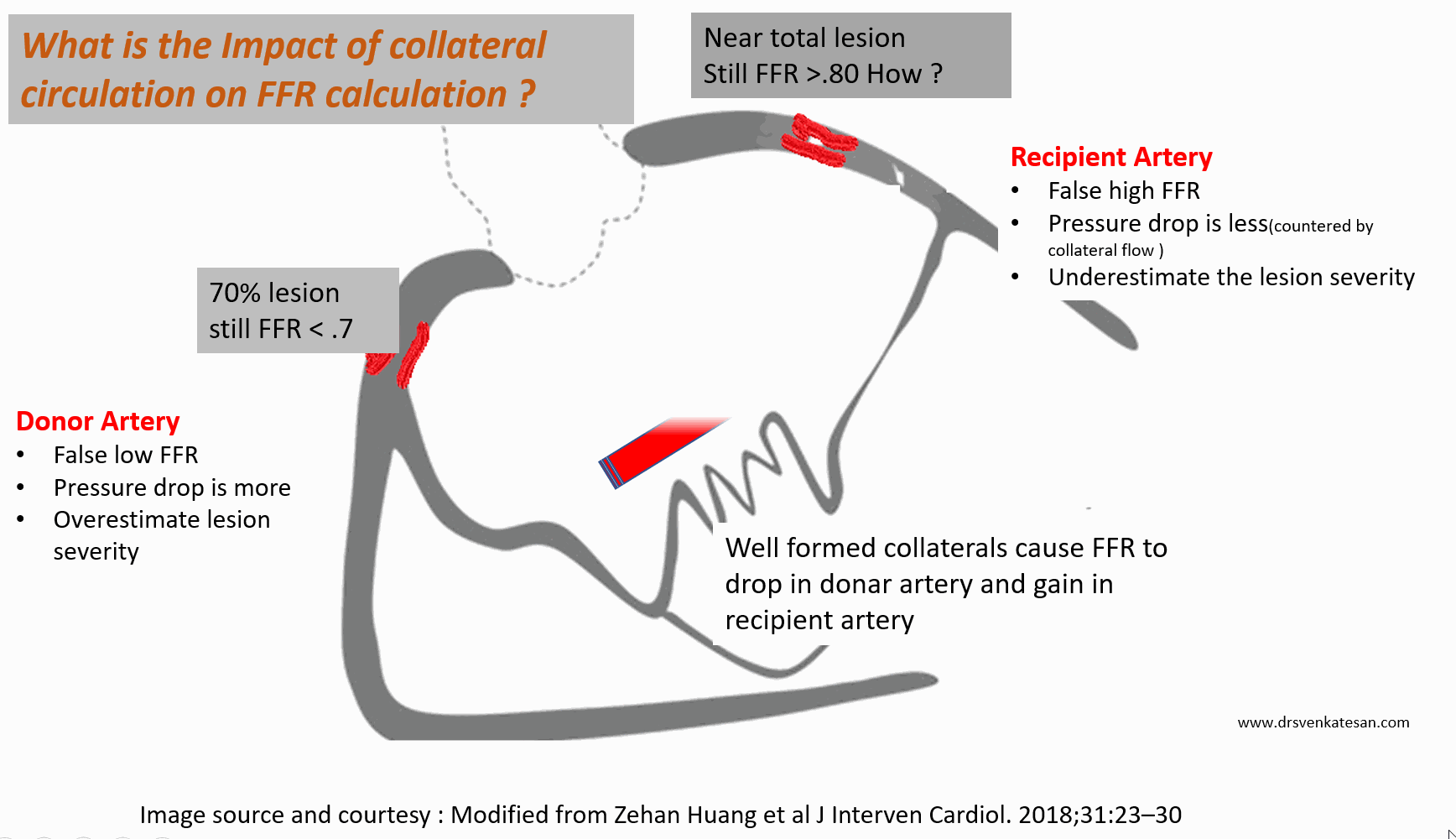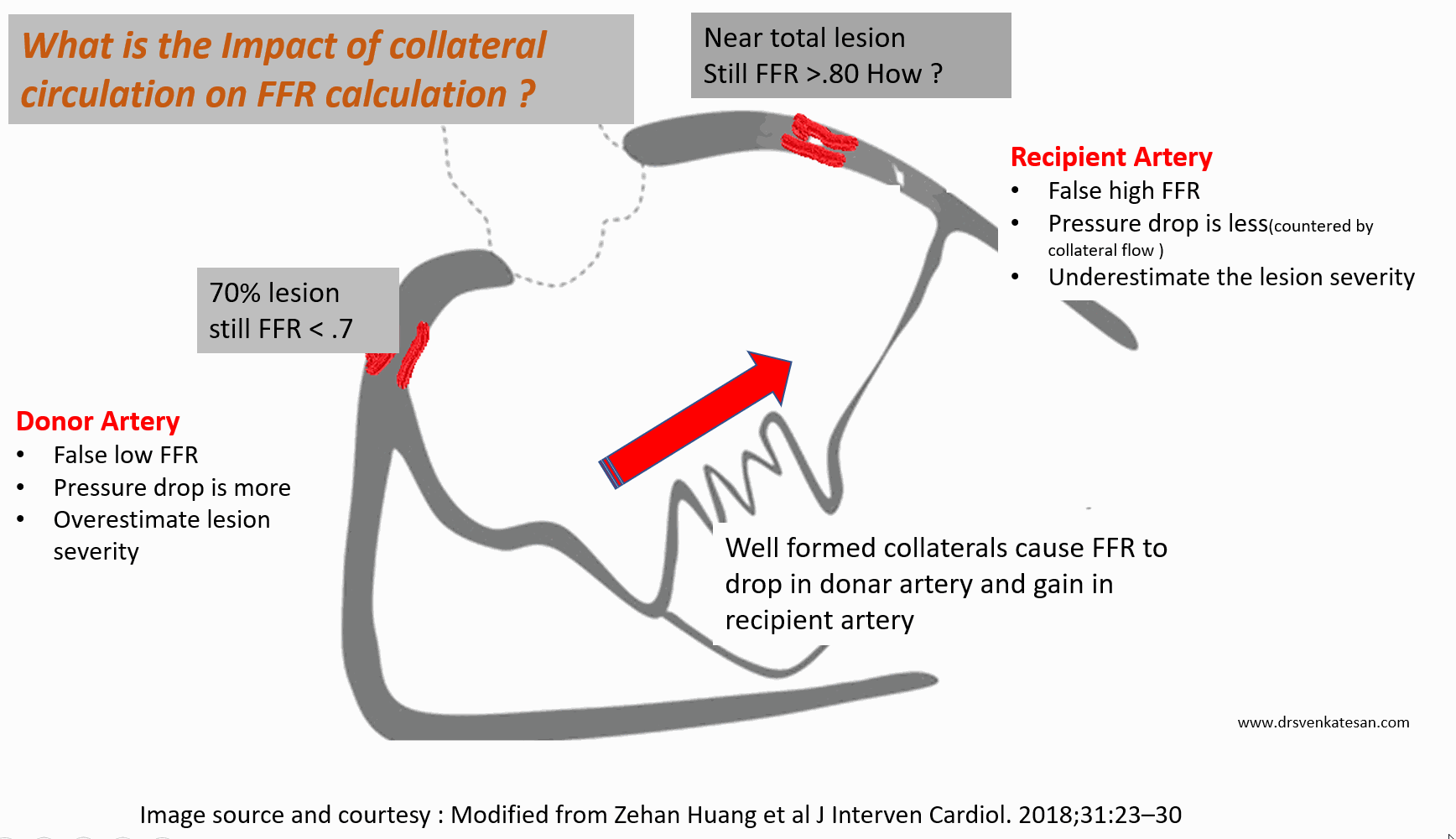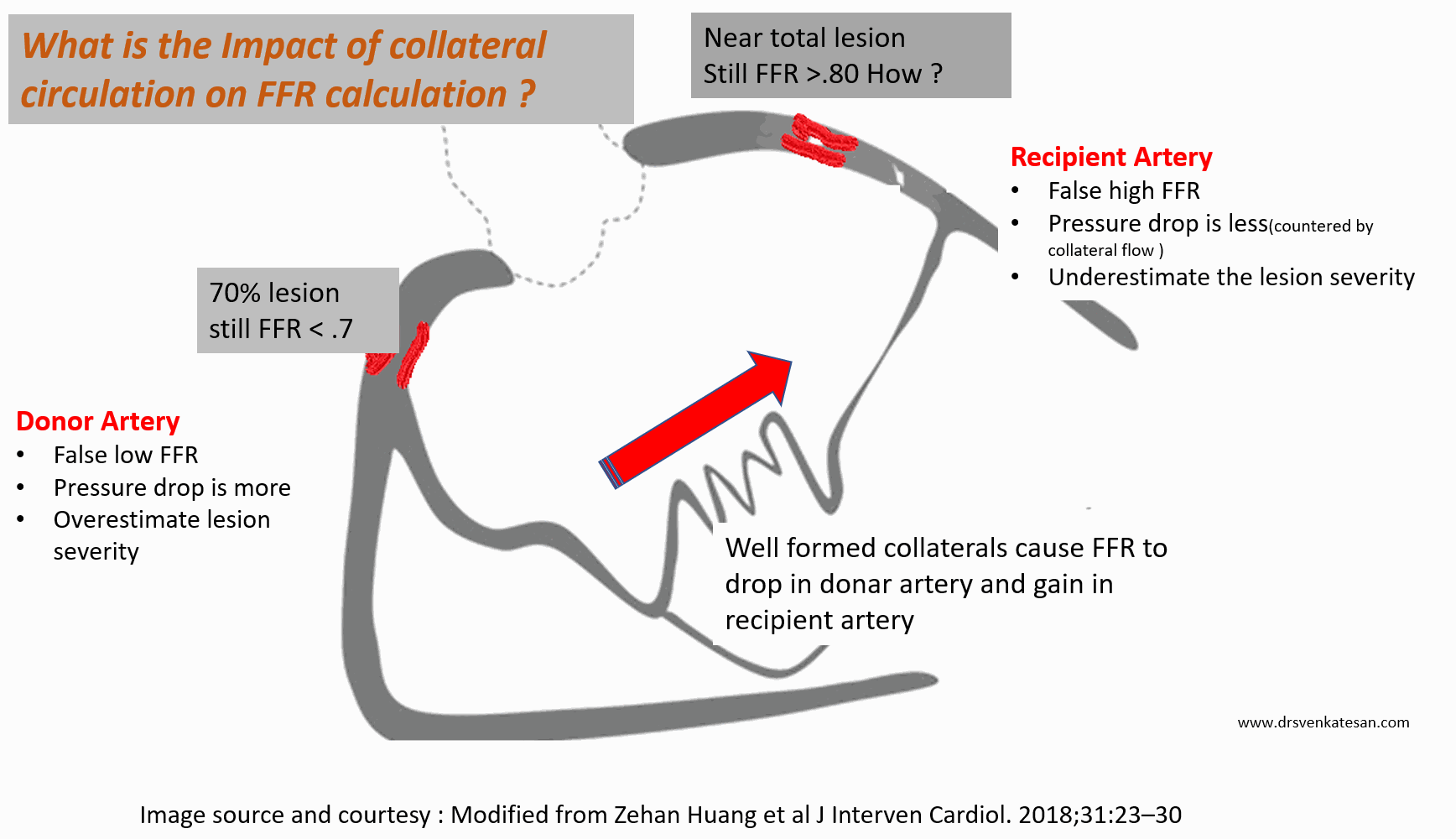
FFR is artificially low in donar RCA (<.75) and makes an insignificant lesion as significant ( ie false positive) . Meanwhile, in the recipient artery LAD FFR is artificially high, and give a false negative result, underestimating the severity
Clinical significance
Summary
FFR overestimates lesion in the donor artery. Under-estimates lesion severity in the recipient artery.
Reference

Reality check
FFR as a concept has suffered a conceptual as well as situational issues (Left main, bifurcation blues, ACS confounders, Adenosine antics! etc) . Hence,we have moved to IFR, CT-FFR, QFR, IMR, etc.(Sorry to say this, even these modalities are struggling to become a practical tool for the true physiological assessment of a lesion)
I used to tell my students, do a stress test if we encounter 70 to 90 % single-vessel lesion (or even multivessel ). If it comes negative or if the patient has good exercise capacity, it is a non-invasive marker of adequate FFR and avoids an Intervention.
I wish , we can call the humble stress test as poor(smart) man’s FFR.
Posted in Uncategorized | Tagged FFR IFR wave free qfr imr ct ffr, ffr in left main bifurcation lesion tandem lesion, ffr vs tmt stress test, impact of collateral on ffr, oor man's ffr, stres test equivalent |
Two stents Onyx (Medtronic) and Biofreedom(Biosensors) appear promising with rapid endothelisation and hence short DAPT. There are three more options, available for this situation.
Option 1
Avoid the endothelium unfriendly DES and use BMS* with MAPT (Mono or minimal duration antiplatelet therapy). For the sake of young generation cardiologists, let me expand BMS,ie Bare metal stents.
BMS in 2020 , what nonsense are you talking about ? (For those who ask this question, please go through the following study with a conscience)
(NORSTENT 2016 -One of the most underrated, deliberately concealed landmark paper in cardiology. We understand, even papers from NEJM don’t get noticed, if it confronts commerce. As expected, none of the cardiology bodies considered it worthy to use this study data in CAD management guidelines)
Want more evidence?
One more study, BASKET -PROVE explicitly showed in large-caliber vessel (Stent >3mm) BMS vs DES doesn’t make any difference.(Christoph Kaiser 2010 NEJM)
What is the 2nd and 3rd option?
Did you guess it ? Yes, correct, avoid the stent altogether. Do a POBA* if feasible, or just continue with the self humiliating medical management and be happy to prevent a potential stroke.
Mind you, in our hind sight, we always realise, most lesions are amenable for medical management, unless it is critical, proximal and symptomatic.
*If you think doing POBA downgrades your Interventional worthiness, we may add a DEB top up, to pacify our restless scientistic sense.
BVS(Bioreabsorbable vascular scaffold)
It is not yet ready as on option, since it appears risky even with 60 micron struts as stent digestion is patchy and incomplete and paradoxically create a more thrombotic milieu.
Final message
In high bleed risk patients, though special stents are avialable, BMS is always an option.
Postamble
After seeing this , one of my colleagues told me, two weeks of vigorous search all through India, he failed to get a single BMS supplier. When enquired, I also found the same. Yes, India is a poor country, they can’t afford to stock cheap BMS, try asking rich western countries. I am sure Germany has it.
( Scientifically, the option of BMS need not be confined to high bleeding risk ,it can very well extend to any CAD profile)
What Dr Antanio Colombo has to say on this

https://www.sciencedirect.com/science/article/pii/S0735109717376064
Posted in Uncategorized | Tagged biofreedom vs onyxone, bms for high bleeding risk, BMS VS DES IN 2020 NORSTENT BASKET PROVE NEJM, POBA DEB to reduce bleeding risk |
Anti-platelet drugs find a place virtually in every prescription written by a cardiologist for CAD.No doubt, it sits right on top among the highest prescribed medication in the world. They are used in all forms of CAD/ ACS. It becomes mandatory in post PCI as a stent maintenance protocol.
Cardiologists (at least me) are exhausted with so many studies with these drugs. When we thought we are relaxing for a while, the current issue of circulation release a big meta-analysis with 50,000 patient data.It tries to draw fresh battle lines between the three friendly P2Y12 inhibitors.
What should you believe in?
This meta-analysis or the ISAR React 5? Don’t believe either, Then what shall I do? Maybe, go with your Intuition. (Considering the fact, P2Y12 receptors are more attracted to unidentified wall street ligands, than Adenosine diphosphates)
Final message
Let us hope true breakthroughs happen in antiplatelet drugs so that we no longer need to see these boring fights between the same old drugs.
Posted in acute coronary syndrome, anti platelet drug | Tagged bms vs des, isar react 5 themis, stents for high bleeding risk biofreedom onyxone, ticagrelor vs prasugrel vs clopidogrel |
I stumbled upon this unique historical info about my college. *According to Prof. Emeritus M.G. Sahadevan., F.R.C.P. (London), the first medical college of Kerala was started at Calicut, in 1942-43, during the Second World War. Due to a shortage of doctors to serve the military, the British Government decided to open a branch of Madras Medical College in Malabar, which was under Madras Presidency then. The Medical School was started close to the then district hospital at Kottaparamba ( now Women and Children’s Hospital).
The war was over before the medical students completed their course. After the war, the medical school at Calicut was closed and the students continued their studies at Madras Medical College. Captain A.B. Das,(late) a veteran doctor who practiced in Calicut belonged to that batch. Nothing much is known about other students who might have served in the British military. Until recently the building which housed the medical school was the R.D.O office. The building next to that is the public health laboratory even now and the buildings beyond those are the doctor’s quarters of W & C Hospital even now.
Those of you, who have any further information on this historical fact are welcome to share it here.
http://calmedcollege.freeservers.com/cmchistory.html
Posted in Uncategorized | Tagged histroy of madras medical college, madras medical college calicut branch |