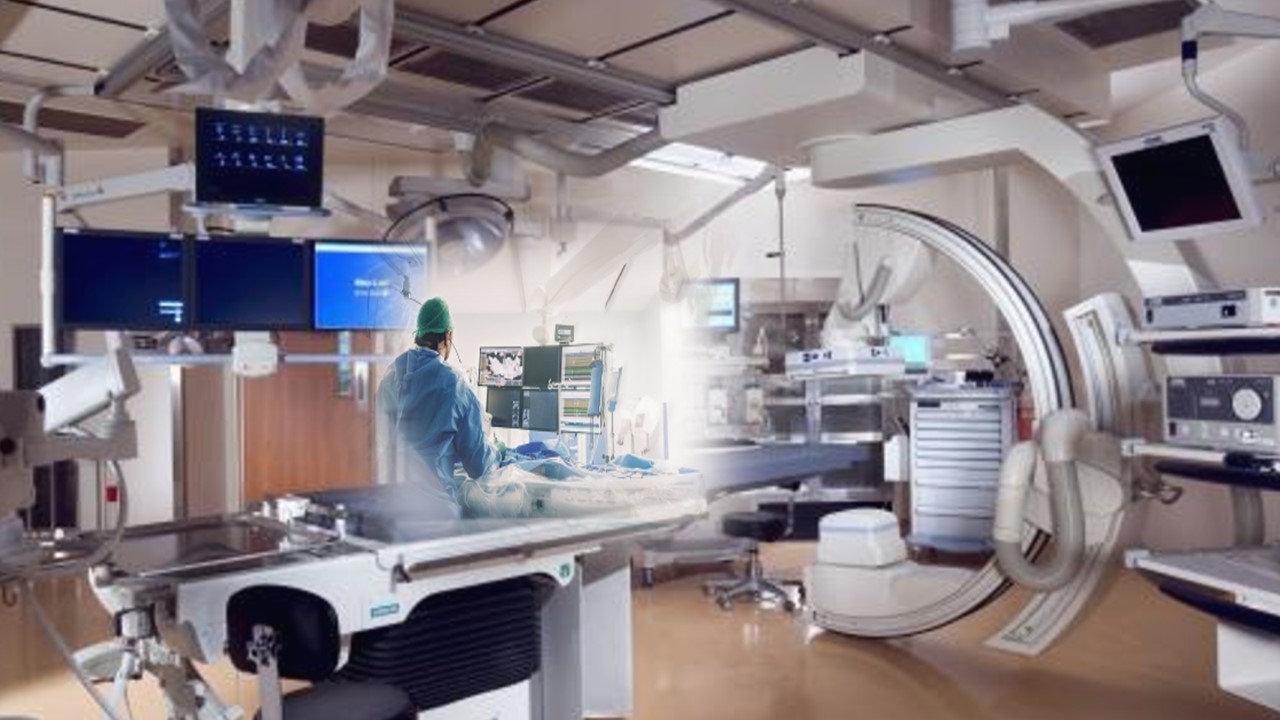
Recently, I visited a seven-star cardiology center. It had a fascinating lab with a near-360-degree roaming arm and floor (even the roof, I think!). The lab also had provision for optional thoracotomy support by surgeons and a CT scan. What’s more, I was told that an adorable robot will soon be added to the cath lab workforce to assist in delivering and maneuvering catheters. It’s truly amazing to see the advancements in science!
I asked the chief staff nurse how many procedures are being performed per day. She pulled out an Excel chart from a gesture-controlled touch panel. It was clocking about 20 to 25 cases per day. The lab performed the best of all procedures in our country. Great, well done, and congratulations, even as my lips uttered, my mind was thinking the opposite. Do we require such labs when the majority of the population struggle to get even basic medical care in emergencies?
Quantity vs quality of procedures
The said lab went on to achieve 2000 cases recently. It was crowned with glory in a stunning anniversary bash. We all take pride in numerical accomplishments. Quantity is easily measured. It’s simple mathematics. Assessing quality is a tricky one. Even professionally well-accomplished interventions may be of low quality.

Low quality and low impact may not be synonymous; still, it conveys the same meaning if we look at it from the patient’s perspective. The quality of the procedure shall be assessed with reference to the cost involved, clinical outcome, procedural as well as a perpetual chain of risk, finally, and most importantly the test of time.
Overall, the quality check of a cath lab is not only for the machines, it is also about the operators & what they do.
Postamble
Whover wants join this cath lab award session. Welcome .
“Top 10 low-quality (Impact) cardiac Interventions”
There were 10 nominees
- Distal bifurcation lesion
- LAA closure
- Delayed PCI in STEMI
- Valve in valve
- VSR closure post-STEMI
- Septal ablation in HOCM
- His bundle pacings & CRTs
- Poorly planned TAVRs
- Clumsy Paravalvular leak blockage
- Complex EVARS
* The winner was selected without any difficulty: No 3 : Its delayed PCI beyond 24 hours after STEMI (This accounted for 30 % of all procedures put together)
Meanwhile following competes for “high-quality” intervention
- PTMC
- Left the main/ proximal LAD stenting in UA/NSTEACS
- Permanent pacemakers in CHB (Not all in SND)
- ICD implantation for the truly deserving
- RF ablation for AVNRT/ Some VT
- Selected cases of Primary PCI
- Some life-saving palliation in the newborn(Ductal stenting/IAS septostomy)
- Diagnostic coronary angiogram in a strongly suspected ACS.
Choosing the winner was really tough, just leave it to the readers.
Final message
It’s worthwhile to go for such an analysis periodically to improve procedural quality & Impact. It’s wiser to allow our brains to prevail over hands. Global health is all about technology optimization, outcome analysis, comparative efficacy. The future sounds exciting though, with deep machine learning, data mining, skill transfer. However, there seems to be a definite risk. In the name of artificial intelligence, we might contaminate machines as well with humanness.
Let us restrict funding and stop Insurance coverage for low impact procedures. Instead, may use the resources for a truly life-sustaining & healing process.
Reference & Further reading
Posted in Uncategorized | Tagged comparative efficacy trials, cost effectiveness in medicine, ethics in medicine, EVO;LUTE PRO SAPIENS XT, health economics, HYBRID CATH LAB, TAVR TAVI VALVE IN VALVE, top 10 best and worst interventions in cath lab |