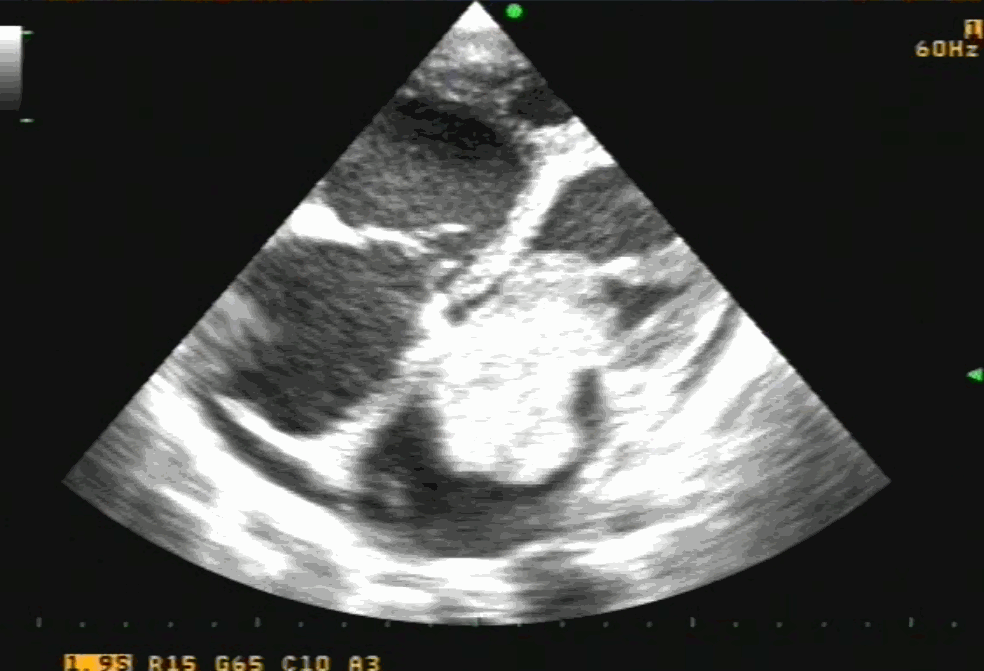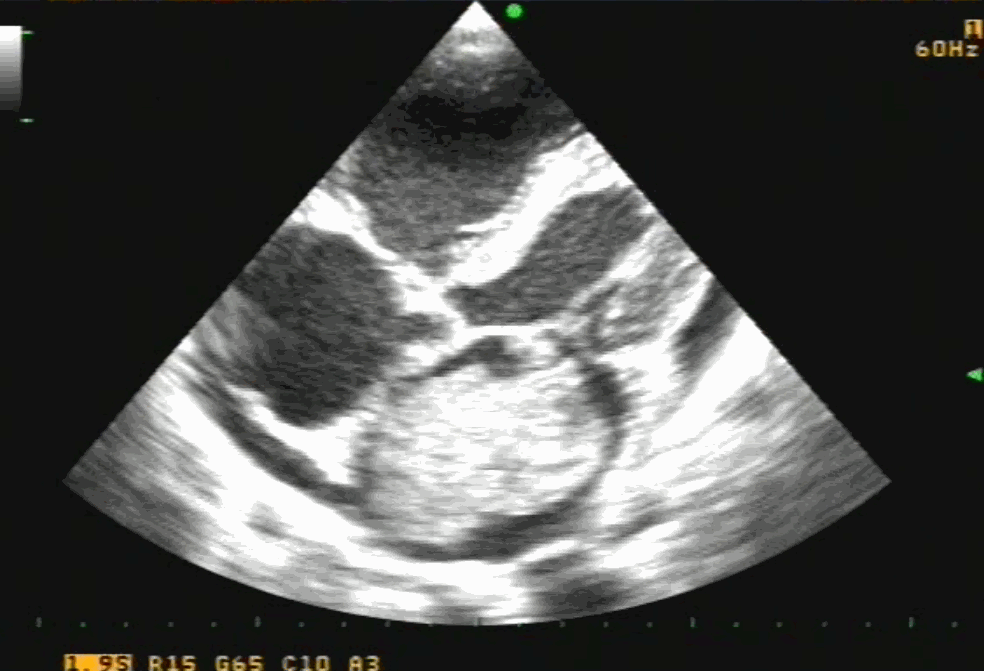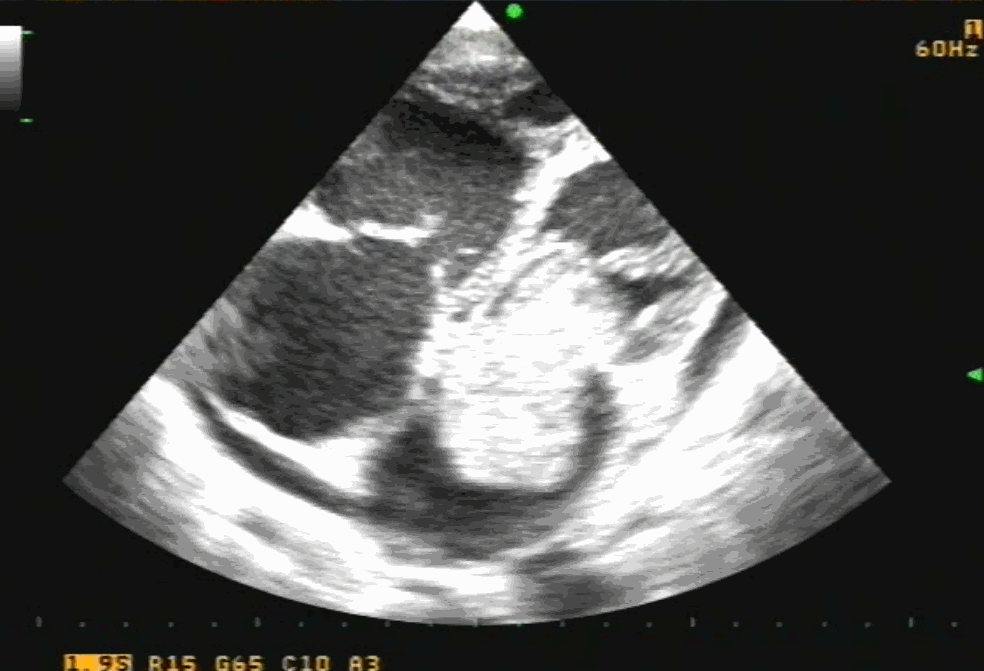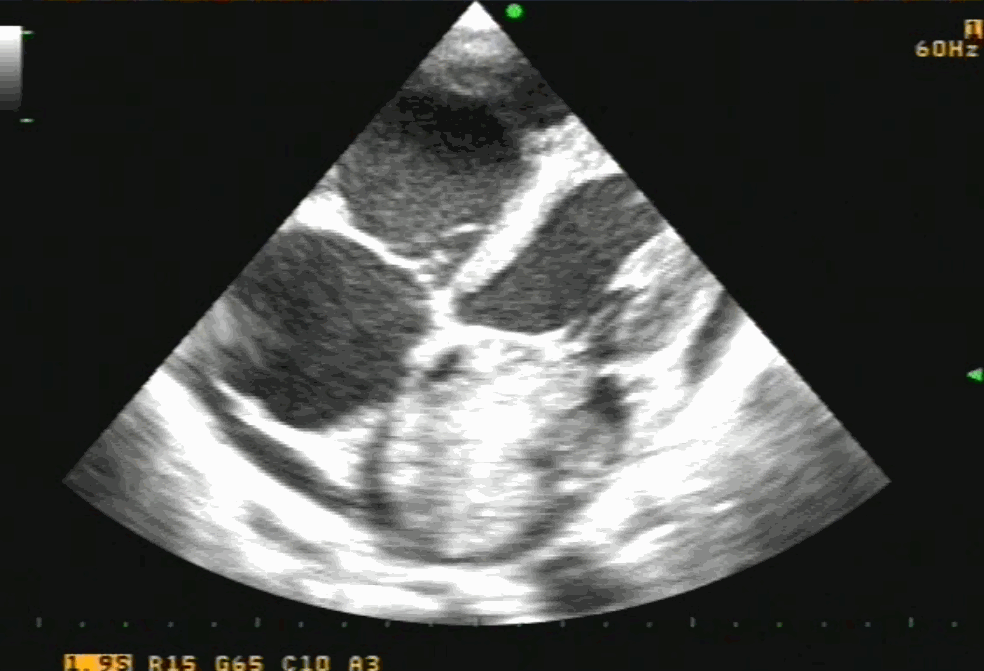
Cardiac myxoma is the most common primary tumor of the heart that presents as mitral inflow obstruction/ regurgitation often with a systemic presentation. It can be either familial, syndromic, or sporadic. Excellent imaging is possible and diagnosis has become straightforward. Surgery is the specific treatment,
What information do the Surgeons need?
Size, attachment to surrounding structures is the key. The myxoma origins most often in IAS and defining its attachment is crucial. Mitral leaflet distortion, Injury ( and even attachment) is possible. It is helpful for the surgeons if we let them know the mechanism of mitral regurgitation prior to surgery. Echocardiogram including TEE is sufficient in most. MRI may add some more info. The aim of surgery is to remove the tumor mass completely.
Is myxoma a completely benign tumor?
Another issue is our poor understanding of the recurrence of myxoma. Why should a benign tumor be recurrent? If recurrence is a feature to be counted as a sign of malignancy, myxoma can be definitely a suspect. There seems to be a catch. It is invasive, locally recurrent, still not malignant. (Whether sarcomatoid degeneration happens is not known. Most pathologists deny this) The problem is, still we are not clear about the cell of origin of this tumor. All that we know is its origin mesenchymal stem cell.
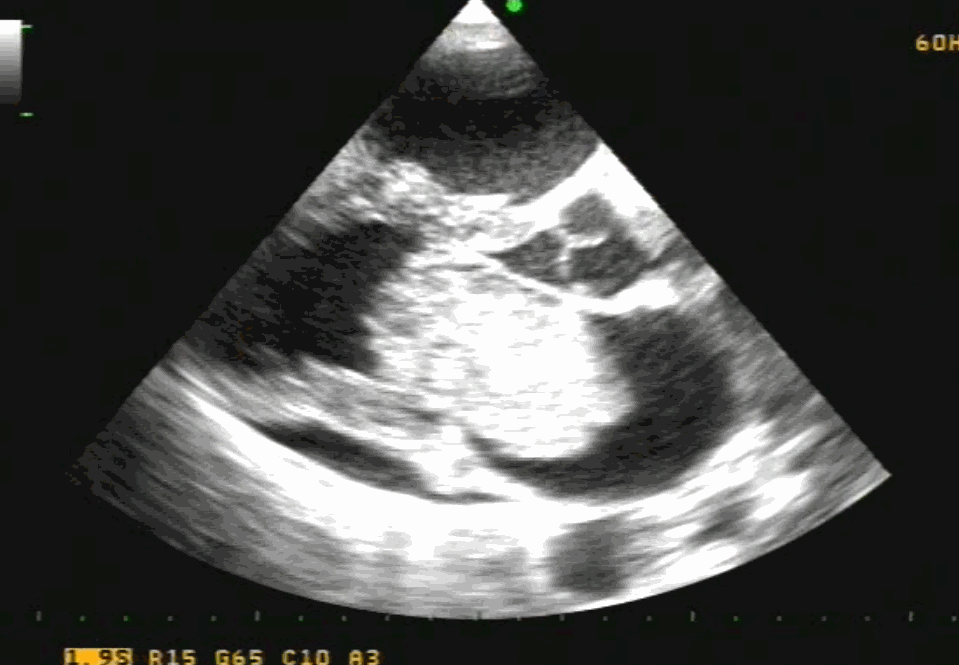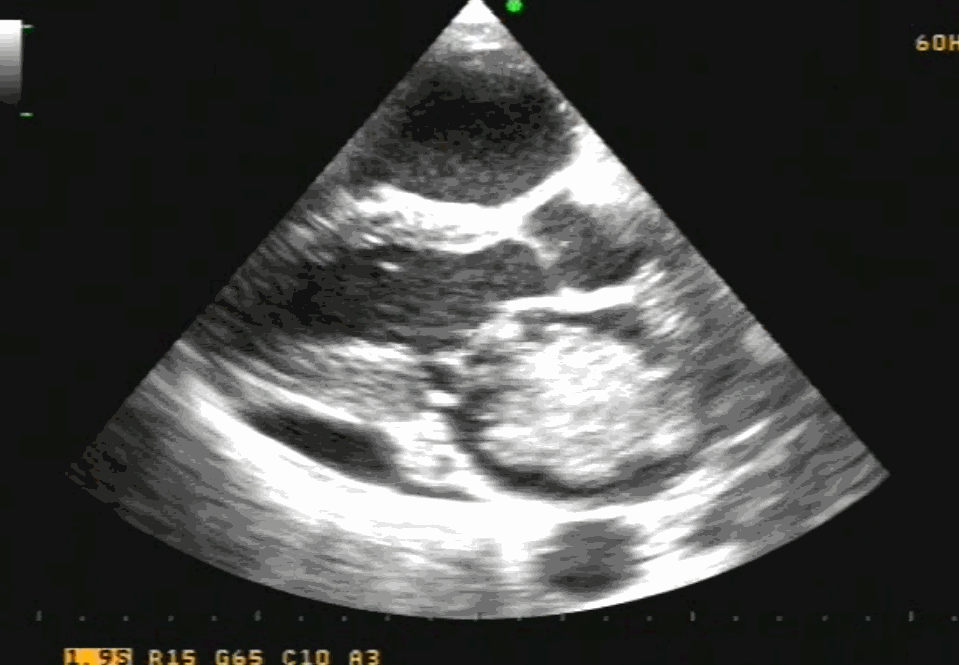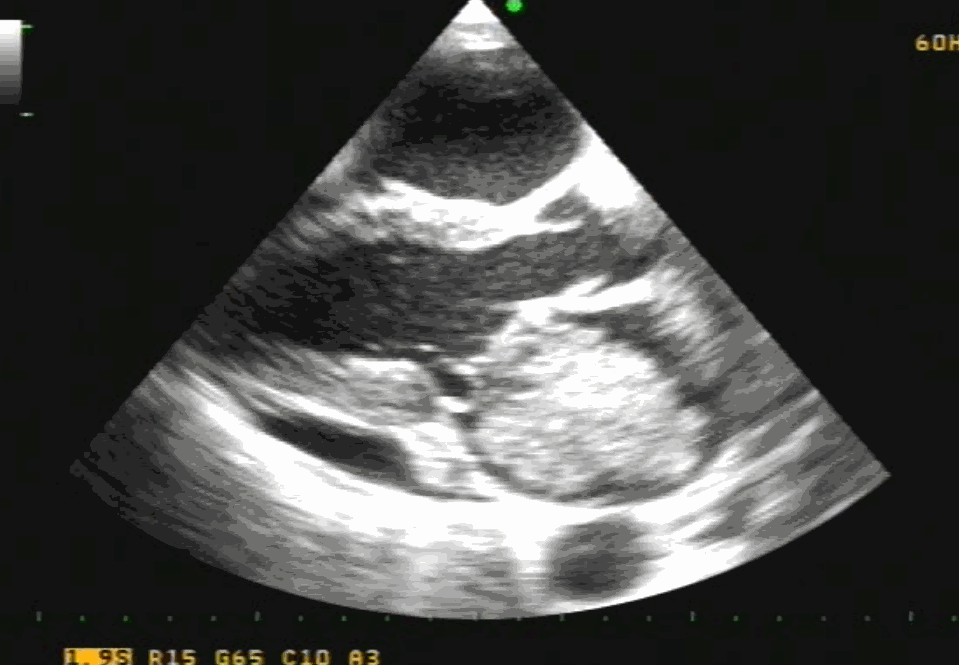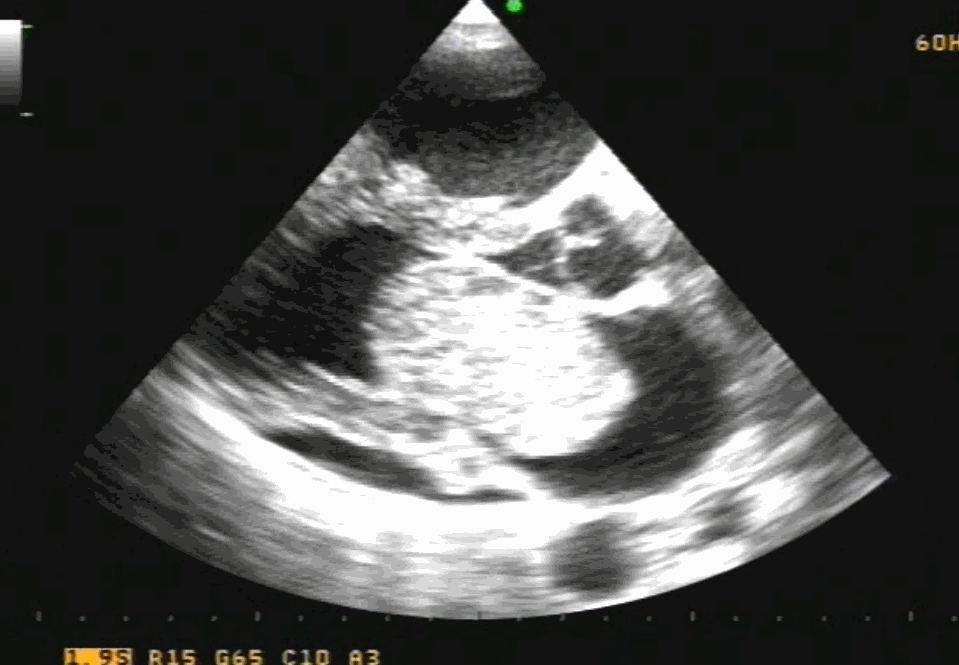
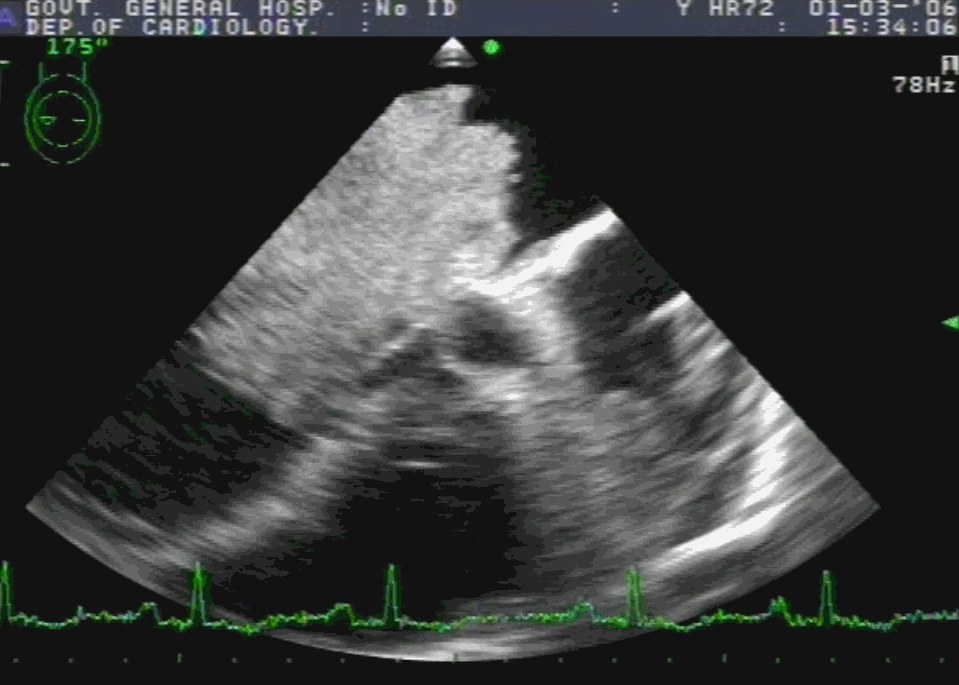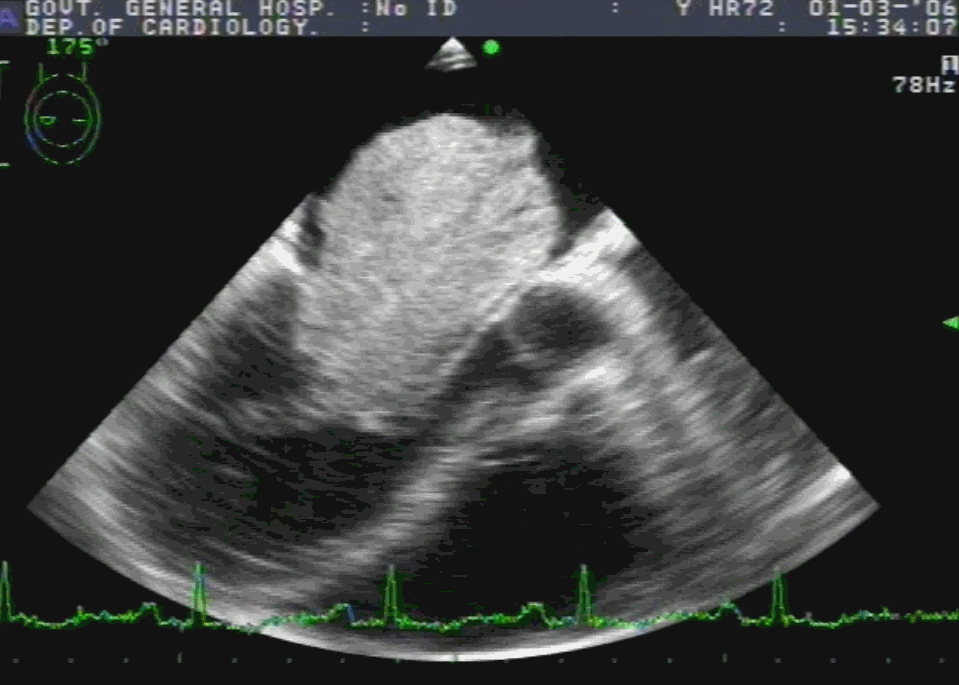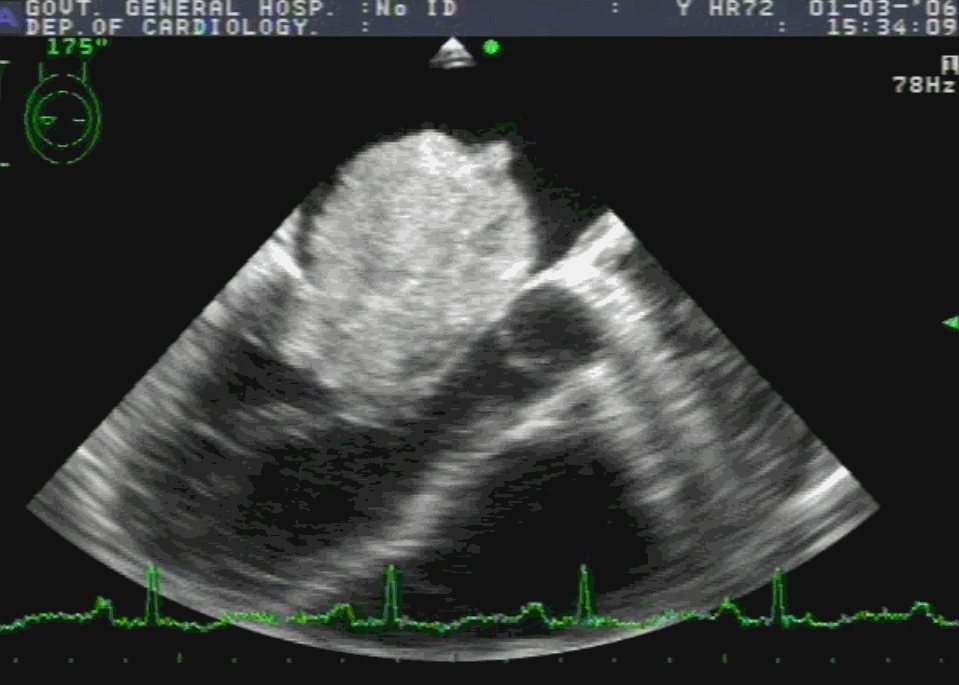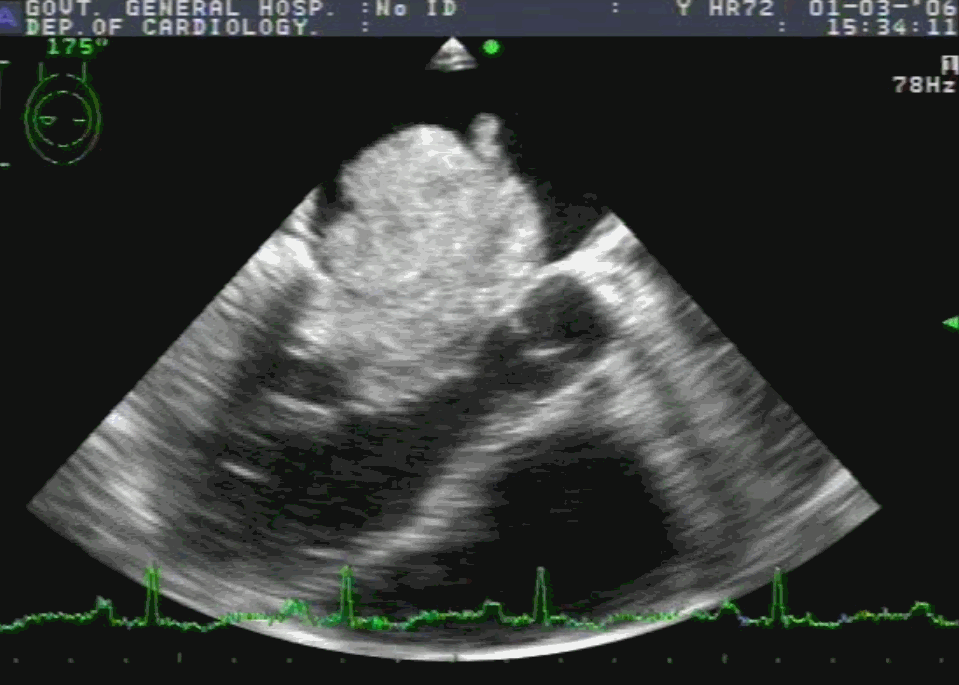
Note 50 % tumor mass enters the left ventricle with diastole. No wonder, as the tumor plops with diastolic cardiac cycle a high-pitched sound simulating opening snap followed by an MDM perfectly mimics rheumatic mitral stenosis. An MR murmur is equally common.
Common sites of recurrence
- Interatrial septum
- The atrial surface of anterior mitral leaflet
- From contra-lateral atrium rarely
The mechanism of recurrence is either due to incomplete resection or due to its multifocal origin.
What the surgeon needs to do?
The aim of surgery is to remove the tumor completely. It’s painful to diagnose recurrence and subject the patient to another surgery. (We encountered a sorry situation recently) So, when we remove the tumor we should ensure sufficient clearance with normal tissue.Biatrial approach is preferred by some surgeons.( Ahmet Yüksel Braz. J. Cardiovasc. Surg. vol.31 no.4 July/Sept. 2016)
If the tumor is not well delineated, it is better to remove a significant area of IAS along with tumor mass and subsequent patch closure. Recurrences in AML and contralateral atria is unfortunate and can’t be predicted.
Further, the mitral valve is to be inspected and functionally tested. Minimal repair work or even rarely replacement might be necessary.
Final message
Referring a patient to a cardiac surgeon is not a bland ritual. (Have seen many single line referrals such as triple vessel disease referred for CABG) A well-informed interaction by the cardiologist with the surgical team and a possible per-operative echo consult, especially in rare surgeries will bring the best for the patient.
Reference