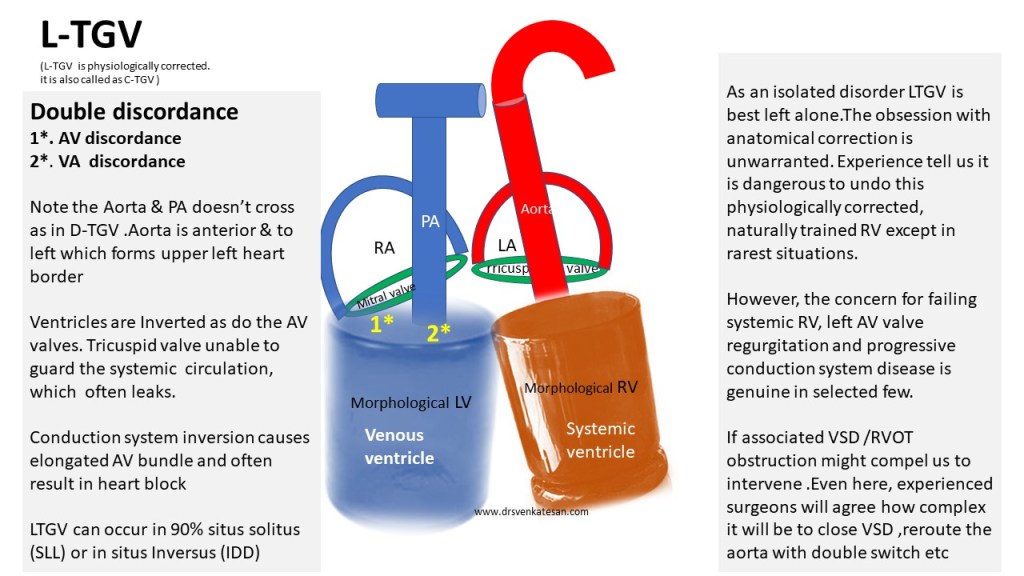
The relationship between Aorta & PA is the key to diagnose many complex congenital heart diseases. Here is a simplified illustration for gross understanding. Please refer to other sources for complete review.

Further reading
Posted in congenital heart disease, Embryology : Heart valve development, embryology of heart, Uncategorized, tagged accessorry av node, Aorta pulmonary artery relationship, atrial septostomy, double switch surgery, dtgv ltgv ctgv, embryology of heart, left av valve regurgitation, ltgv ctgv in situs inversus LDD, rv lv function in ctgv ltgv, senning surgery, spiral septum, three letter code for chd, ventricular inversion on June 12, 2021|
Posted in congenital heart disease, history of cardiology, tagged history of cardiology, Jane somerville, pulmonary atresia jane somerville on February 7, 2016| Leave a Comment »
The field of cardiology has seen great men over the centuries. Few women have permanently stamped their presence in that history .Jane Somerville can be termed mother of pediatric cardiology along with Maude Abbott She has a fascinating life history , having worked in Royal Brompton , Imperial and Guys London.She was mentored by pioneers like Paul wood , Blalock and others .She is primarily interested in the pediatric cardiology especially congenital heart surgeries .The classification of pulmonary atresia with VSD goes with her name.
She carries the credit of starting the Pediatric cardiology world congress in 1990 ,is the founder of GUCH (Grown up children with congenital heart disease.) .
Here is a rare interview from he to Dr Robert Califf for Heart.org. For those,who like to have a glimpse of cardiology in its vintage times , don’t miss it.Dr Jane addresses the past treasures , explores specific issues of facing pediatric cardiology and frank expression about the issues of women being a cardiologist in a man’s world.
She has a foundation in her name that helps the children and adults with congenital heart disease.
Reference
The landmark paper in BHJ 1970
Posted in congenital heart disease, tagged effective pulmonary blood flow in tgv, mixing in dtgv with intact ivs, pfo vsa asd pda in tgv dtgv, role of pda in dtgv on August 5, 2015| Leave a Comment »
TGV is the most common cyanotic heart disease to present at birth.The outcome is dismal unless it is intervened at the earliest .It becomes a real emergency if the dTGA is associated with intact IVS and IAS. (Though foramen ovale /ductus may help for a while prolonging the survival . Often times , it is restrictive and demands immediate septostomy if primary arterial switch correction is not attempted )
Presence of VSD provides vital time interval to plan surgery in a less emergent fashion. Otherwise , arterial switch if contemplated one has to do it before 2-3 weeks (Rarely up to a month ) .The principle is to reverse the circulation before the systemic left ventricle regress its myocyte function as it is exposed to low pressure pulmonary circuit .
Hemodynamics
We know , dTGA has two parallel circuits in a bizzare hemodynamic disconnect .The right sided pulmonary circuit sustains the systemic blood flow with deoxygenated blood.The left sided systemic circuit recirculates oxygenated blood into pulmonary circulation again and again.
Survival depends upon , the anatomical communication between two circuits and the effective quantum (Deoxygenated) of blood flow to the lungs .
Which communication is best for survival d TGA ?
The key is to understand what we mean by “mixing vs shunting” and the effective pulmonary blood flow (ie quantum of truly deoxygenated blood reaching lungs vs oxygenated blood recirculating the lungs in a hemodyamically wasted loop
It appears both atrial ventricular level mixing is good for maintaining adequate O2 saturation than PDA .
What does PDA do ?
Ductus is expected to persist in dTGA when IVS and IAS are intact . It is not clear what determines the persistence of duct in dTGA with intact IVS. Principles of natural hemodynamic adoption would argue , all patients with dTGA should never close their ductus and foramen ovale. While , In reality it may be true for PFO to persist, ductus often gets closed on schedule* , aggravating the hypoxia .(Both flow mediated myogenic resposne, O2 content of ductal blood and size are the determinants of ductal closure)
The ductal circulation in dTGA can be complex . It initially acts as a channel to mix both arterial and venous blood flow .It can become a liablity if its large , as the pulmonary vascular resistance falls, blood is shunted from aorta to pulmonary circulation and potentially precipitate failure .Please note, this shunting also can improve the saturation as it diverts aortic blood into lungs ,still the ultimate usefulness will depend upon intermixing at some other level other than ducuts , ie either atria or ventricle .One should realise ductus can never bring good admixture as it happens outside the heart .It is obvious intra cardiac mixing with ASD and VSD is always better and devoid of providing differentially saturated blood to the extremities , which is an inherent feature PDA mediated mixing .If ductus is the only means of mixing and shunting the lower half of the body has an advantage as it is perfused continuously by oxygenated blood .This may manifest as reversed differential cyanosis in few combinations of TGA physiology. (Relatively pink lower limbs and cyanosed upper extremity )
Summary
Ductus can be a double edged friend or single edged foe in dTGV . It depends upon the size , quantum of shunt and associated channels of mixing like ASD and VSD . If it occurs with intact IAS and IVS it plays a role of life sustainer.
Presence of ductus is definitely useful initially.It can either help by mixing, intermittent bi-drectional shunting or committed left to right shunting .This is why we attempt to preserve its patency or even recannalise it by stenting in such situations .The later can be used to buy time and train the regressing LV .However ,large ductus can be counter productive if additional shunts are also present where one should even contemplate closing it .
Reference
1.
 2.Transposition of the great arteries with intact ventricular septum and patent ductus arteriosus. Waldman JD, Paul MH, Newfeld EA, Muster AJ, Idriss FS.Am J Cardiol. 1977 Feb;39(2):232-8.
2.Transposition of the great arteries with intact ventricular septum and patent ductus arteriosus. Waldman JD, Paul MH, Newfeld EA, Muster AJ, Idriss FS.Am J Cardiol. 1977 Feb;39(2):232-8.