
Archive for the ‘Uncategorized’ Category
A forbidden quote about science
Posted in Uncategorized, tagged forbidden quotes, medical education, medical ethics, medical quotes, science quotes, venkat quotes, venkatesan sangareddi on December 20, 2023|
Rules of myocardial revascularisation REVIVEed : Quantify”non-viable tissue” first.
Posted in Uncategorized, tagged accc aha esc guid;ines on myocardial revascularisation, cabg, cabg patch study, ischemic dcm, myocardail viablity, pet scan for myocardial viablity, REVIVED BCIS2, viablity study myocardial on December 20, 2023|
”It looks like, science oftentimes struggles at the hands of scientists“
The weakest link in medical research is framing the right research question. How will you explain the drama of research on myocardial viability studies that have been going on full steam for more than 3 decades,? Which has become junk now.
This truth came out from a secondary analysis of the famous REVIVED-BCIS2 trial. For the busy guys, the conclusion is given in the box below.
JAMA Cardiol. 2023;8(12):1154-1161.


Final message
We realize, in the game of myocardial revascularisation the quantum of dead tissue determines the outcome of revascularization, not the amount of living tissues. This same question was asked & answered more than a decade ago (2009) on this site, of course without that damning evidence.
Common myths in cardiology: The presence of viable myocardium does not mean one must do a revascularisation procedure following myocardial infarction!
March 15, 2009 by dr s venkatesan
Many times, we don’t require large-scale RCTs, years of toil, and efforts wasting resources to prove an apparent sense of thinking.
What is conservative management ?
Posted in Uncategorized, tagged accc aha guidlines, ethics in medicine, GDMT, OPTIMAL MEDICAL THERAPY, principles of practice of medicine, WHAT IS CONSERVATIVE MEDICAL MANAGEMENT on December 16, 2023|
Conservative management conveys two tangentially opposite meaning.
For the superior “physicians & Interventional cardiologists” it would mean

For the “Inferior genre of physicians” it will sound like this

Reference
This is a partial repost from a 2008 article . https://drsvenkatesan.com/2008/11/30/what-do-we-mean-by-conservative-management-why-it-is-often-considered-as-an-inferior-form-of-treatment-in-medicine/
A basic query in LV function measurement
Posted in Uncategorized, tagged ase criteria for lv function measurement, ecg gating in ct scan, ecg gating volume correlation, ecg vs echo gating, end diastole in ecg, end systole in eco vs ecg, end systolic point in ecg, lv function measurement, peak r and peak t systole and diastole, t wave relation with diastole on December 16, 2023|
Which point in ECG is taken as reference for End systolic dimension for LV function assessment?
Marking the end diastolic point in ECG is quiet straight forward. Peak of R wave.(or Q)*
But, what about the reference point for end systole.
- Descending slope of T wave
- Peak of T wave
- End of T wave
- If T is absent or not clear , I will be confused
- To be realistic, ECG has no reliable reference point for end systole.
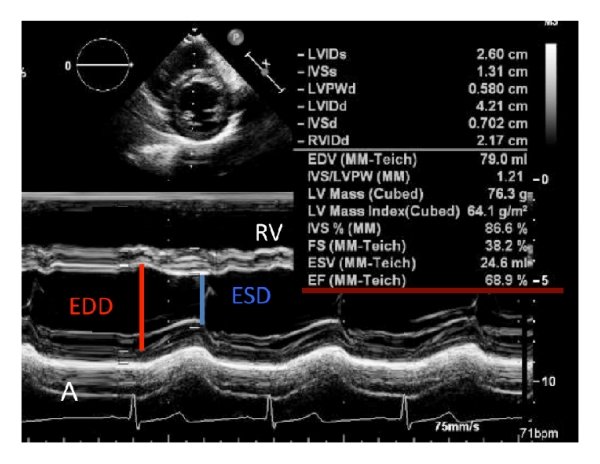
Answer: If I say the answer is 5, no one is going to agree. Please note, the relationship between the T wave and the peak systolic phase in echocardiography is weak. Is there any relation at all ? Then, how to measure LV function in echocardiography? There is a electro-mechanical delay in every segment and sequence of cardiac contraction and relaxation, with former piping the later (electricity beats).
Surprisingly (illogically as well), we take the point of maximum thickness in M-mode as end-systolic, which, in fact, corresponds to peak mechanical systole. This point has no consistent relationship with any part of the T wave. We must realize, the clinical cardiac cycle is defined based on sounds, i.e. S1 and S2, while the biomechanical cardiac cycle is different. Similarly, echocardiographic systole is not the same as clinical systole. 2D echo eliminates this uncertainty to a large extent. This is one of the reasons , we are advised and encouraged, not to measure LV dimensions in M mode.(A very tough advice to follow though)
Final message
We are not completely clear yet, in the “ECG vs Echo” time correlation of hemodynamic events. The errors may be in only milli-seconds, still, when planning for Interventions like re-synchronisations, and in the follow up of DCM patients this could matter much.
Reference
An extract of “Illustrative echocardiography” in Twenty pages.
Posted in Uncategorized, tagged ase-posters, best-echocardiography-book, echo-manual, echocardiography, illustrative-echocardiography on December 15, 2023|
Learning resources in the web, has made the traditional methods of learning & teaching almost redundant.
American society of Echocardiography (ASE) has produced this 20 page PDF document, which covers the entire field of echocardiography , in an Illustrative format.

Take a print out, of this and stick in your lab (If you have space) for an Immersive experience. Hope, sharing this document here doesn’t violate any copyright issues.
Can you try these two questions on Amyloid ?
Posted in Uncategorized, tagged Alzheimer disease, amyloidosis, ttr amyloid, what is amyloid on December 1, 2023|
Is it a physiological molecule ?
1.Yes, It is a physiological molecule.
2.No, Amyloid is always pathological.
Where does it gets deposited ?
A .Extracellular*
B. Intracellular
C. Both
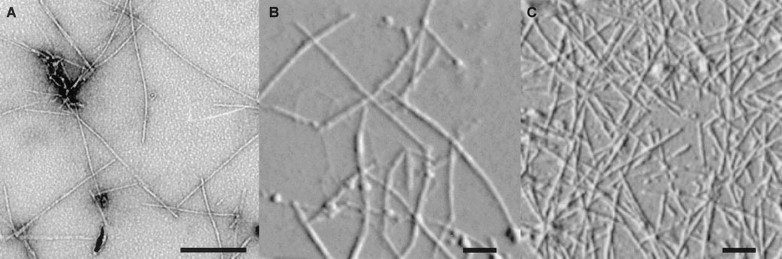
Answer : Q 1: A / Q 2: C. It is indeed a physiological molecule in small amounts that help carry hormones across the blood. In pathology, it accumulates in huge amounts. It is a disorder of protein folding, making them thick, stiff , sheets of peptide, hence mis-behaving with adjacent cells, injuring them in the process. This is responsible for the systemic nature of disorder right from the brain to peripheral nerves, Heart, kidneys, liver, spleen, etc. (Ref 1)
(*It should be stressed , majority of deposition occurs in extracellular space.They clog the interstitial space, also can invade the cell, especially in neurons in Alzheimer’s disease . Now we have evidence that Aβ (A beta) get into the myocytes as well. (Troncone L, J Am Coll Cardiol. 2016) Fellows, better say amyloid is primarily extracellular, but, by pressure effect and injury of cell membrane it results in cell death.)
Can we dissolve it or get rid of it ?
Till now, these disorders has been termed as a degenerative disease with no viable options. Now, we have made a breakthrough. A group of drugs genetically created work by unfolding the proteins by interfering with RNA (SiRNA) that home in on the host liver and help clear these systemic proteostasis, the key pathology in Amyloidosis (TTR).
Patisiran is approved by FDA for peripheral neuropathy and used in cardiac amyloidosis. Patisiran is a siRNA encapsulated within a lipid nanoparticle delivery system for targeted delivery to the liver, the primary source of serum TTR . Once in the liver, siRNA binds to the untranslated region of TTR mRNA and degrades it, inhibiting TTR synthesis. ( Adams D et al NEJM 2018)
Tafamidis is another similar drug. (N Engl J Med 2018; 379:1007-1016)
Final message
We are moving in the right direction in tackling the cell aging, degeneration and cell fibrosis that is behind majority of chronic systemic disorders.(Anti-fibrotic drugs is the next big target Ref: Front. Pharmacol., 31 May 2017 )
Reference
What happens to blood pressure when we stand up ?
Posted in Uncategorized, tagged bp response on standing, hemodynamics of standing, hypertesnion, orthostatic hypertension, orthostatic hypotension, pots syndreome on November 29, 2023|
Many times , an Innocuous question poses a real challenge, to our life time understanding of circulatory physiology.
This question is very important , if we want to understand the true mechanism of postural hypotension, a commonest autonomic disorder in elderly (& also the newly recognised entity orthostatic hypertension)
Mechanism

Orthostatic hypotension is defined as a sustained drop of at least 20 mm Hg in systolic blood pressure (SBP) or 10 mm Hg in diastolic blood pressure (DBP) within 3-5 minutes of going from a supine to a standing position. In patients with associated supine hypertension, the criteria for orthostatic hypotension allows for a drop of at least 30 mm Hg in SBP or 15 mm Hg in DBP.
Can you discuss the answer to the question please ?
The correct answer is likely to be this. In normal adult, the systolic BP falls and diastolic BP is either static or raises by few mm . DBP is never expected to fall on standing, as the fall in systolic BP is invariable, that trigger a vasoconstriction which will increase the PVR and make sure the DBP doesn’t fall. In the process mean BP is kept near normal and regulated.
However, hemodynamic response to standing has no fixed rules. That’s why we keep definitions, like acceptable fall in systolic and diastolic BP . It depends on , age , central and peripheral neurological nervous system, preconditioning of vascular tone.(Not only arteriolar, even the much neglected venous tone).
For the seekers of evidence, there is one study which was specifically done to find orthostatic BP response .(Smith et al Ref 3) .It highlights the point, the immediate vascular response ie (<30sec) is totally different from prolonged standing, Implying, the response time of even an intact autonomic nervous system can be quiet variable.
Orthostatic hypertension :
It is relatively new entity, and claimed to be equally a problem A proposed consensus definition of “an exaggerated orthostatic pressor response” in subjects in whom systolic blood pressure increases ≥20 mmHg when going from the supine to standing posture. (Jordan J, Consensus statement on the definition of orthostatic hypertension endorsed by the American Autonomic Society and the Japanese Society of Hypertension. Clin Auton Res. 2023 Feb;33(1):69-73. ) Surprisingly, diastolic BP is not included in the defining criteria. There must be valid reason for that I guess.
Secret link between both these entities
Obviously it will add on to the complexity, if we say there are common roots in pathogenesis between the two entities. It is indeed true. Both comes under the basket of dysregulated autonomic nervous system. Please recall , we have a condition called supine hypertension and standing hypotension , POTS syndrome etc that should stimulate us to search for those hidden secrets.
As the name itself suggest, autonomic nervous system has its own control(or no control ) with a complex and poorly understood brainstem and cortical network. This operates through physical wiring directly as cranial nerves or piggy packing along the spinal cord tracts , vascular tree, and somatic nerves. The biochemical orchestra of this system is played by a delicate balance of adrenergic vs cholinergic forces.
Next question
What happens to BP during exercise ?
This again has more dynamic and interesting changes especially in the diastolic BP .Read Guyton’s physiology or the good old Rushmer’s hemodynamics monograph, linked in this site elsewhere.
Reference
STEMI Breakthrough: Looking beyond Primary PCI with “Intra-coronary liquid oxygen”
Posted in Uncategorized on November 25, 2023|
“Yes, it is true. It is tough to consider oxygen as a “powerful and magical drug”, because it is freely available everywhere.”
Routine nasal Oxygen has little use in the management of STEMI. In fact, it can be harmful as it causes vasoconstriction. Hence current guidelines, has very strict advice about not giving oxygen unless systemic tissue hypoxia is documented.
Now, how about infusing Liquid oxygen right inside the LAD , the target zone , that is hit by hypoxia.?
This is not a new concept. G.W. Stone et al. tried this in 2009 itself.(Ref 1) For some reason, this was not followed up. How did we ignore basic fact myocyte hypoxia require Oxygen at that level. We were concentrating to reperfusing with blood, but what the cell need is not blood b but oxygen. Now,14 years later, some young researchers reaching out to this concept ,via liquid myocardial oxygen . Hope to be a possible breakthrough success .it was presented at the 2023 SCAI meeting in Phoenix. In this study, a 60-minute intracoronary infusion of liquid oxygen after pPCI reduced the infarct size and arrhymic risk .This study was sponsored by ZOLL® TherOx® .
A possible deterrent is the problematic and complex concept of reperfusion Injury. The term Oxygen radicals always sounds sinister .Really I can’t understand how a cell which get injured by the lack of a a particuar gas, get damaged by the same gas .(Oxygen in liquid from might behave differently as in this study ?) I think,its all in timing of delivery of oxygen, and if we start thinking like Einstein, then ,there is nothing called time.
Final message
Innovation and experimentation is must be allowed as liberally as possible. Breakthroughs happen accidentally at any time. Systemic oxygen may be harmful, but localised delivery of O2, might exactly be the thing, the dying tissues are waiting for. Sometimes we Ignore a good concept for no reason. Bias against drug companies also can be counterproductive.
Reference
Live view of yourself in the globe : Which dot are you ?
Posted in Uncategorized on November 24, 2023|
Now, you can view who all are reading this site live on a revolving globe. It makes all the more happier to note that all these grateful and honourable dots (i.e., you) are literally drawing the world map . Six million reads from 190 countries, right from the Solomon Islands in Micronesian Pacific, abutting the International date line, to the extreme west, reaching Chile and Hawaii has happened so far.
Please click here, to see your live location , zoom on the dot and check, it is indeed true.
https://www.revolvermaps.com/livestats/globe/53mvtnd7p2d/

ICMR study on sudden unexplained deaths in Covid times : An atypical observation
Posted in Uncategorized, tagged covid and sudden cardaic deaths, scd in covid on November 22, 2023|
News: A rare large scale study from ICMR is making news even in the mainstream media. (https://indianexpress.com/article/health-wellness/covid-19-vaccines-sudden-deaths-risk-icmr-study-9036761/)
A casual read of the original paper threw up some thoughts.
India’s apex medical body, ICMR, initiated a study primarily on sudden deaths among young people in covid times . The primary intention of this study was to find what causes sudden unexplained deaths . and also test the hypothesis that the deaths were not probably related to covid vaccination. The study did prove that. (I am not an expert to assess the statistical validity and scrutiny of the study. It is too complex a model. Still, I do have a primitive query as shown in the title )
But, we expected a minimum revelation. What caused these 729 deaths (filtered out of 29000 deaths) I understand physical autopsy could not be done in majority of deaths (Even in witnessed , in hospital deaths). So, the question remains . Is it sudden cardiac death ? Is it sudden “non cardiac ” death ? or can it be a “non sudden” masquerading as sudden in any way.
.A preformed hypothesis
Though this is not a hypothesis-proving study, it is apparent that the intention of the study primarily revolves around removing the stigma and fear associated with vaccination. (The fact that only a fraction of patients, (less than 2%,) were hospitalized for COVID indicates that this study primarily intended to test the risk of COVID vaccination, which was around 85% in both groups.) It makes sense, for the study group , they created a good methodology accordingly and indirectly proved the hypothesis right. As physicians and cardiologists, we wished also look into the data of what caused these deaths by performing autopsies in all possible cases. The results of these autopsies need to be known.
Conclusion is fair
It is traditional (and acceptable ) to blame the heart for all unexplained sudden deaths. The study suggests that heavy drinking, along with with intense physical activity in the background of positive family history, is behind many of the deaths. It is a fair assumption that they are all cardiac. Sudden neurological and pulmonary deaths are under reported. In fact many of the SCD is an arrhythmic event originating from CNS or electro-ionic triggers in blood with the healthy heart
Is this not a major limitation*
When you want to know whether COVID vaccination is related to sudden death in any way ,is not ideal, we need to have a control /cohort arm who have had no vaccination? In this study, both groups had nearly 82-88 % vaccination. In fact, the control group had few percent extra vaccination, and this helped the study, to claim that vaccination prevented some of the sudden deaths. This seems far-fetched with any statistical methodology. This, I feel is a serious limitation. It can even nullify the study conclusion to a large extent. (Experts please clarify , It may be an entirely wrong perception and lack basic knowledge in statistics.)
One more possiblity , can we combine a case-control study with add on accessory cohort and follow up as a dual mode study ?
Final message
It is a landmark attempt to study the mysterious deaths among young Indians in covid & post covid times. Two things .This study can talk about only vaccinated population. Does this study prove, people who have not vaccinated had more or less sudden deaths ? No. this study has no scientific grounds to talk about either positive or negative status of unvaccinated population , because there is no, unvaccinated cohort and follow-up.
At the end of the day, an unexplained death remains unexplained because we couldn’t do autopsy (Of course we have found the same known risk factors responsible , except probably new one vigorous physical activity , )

