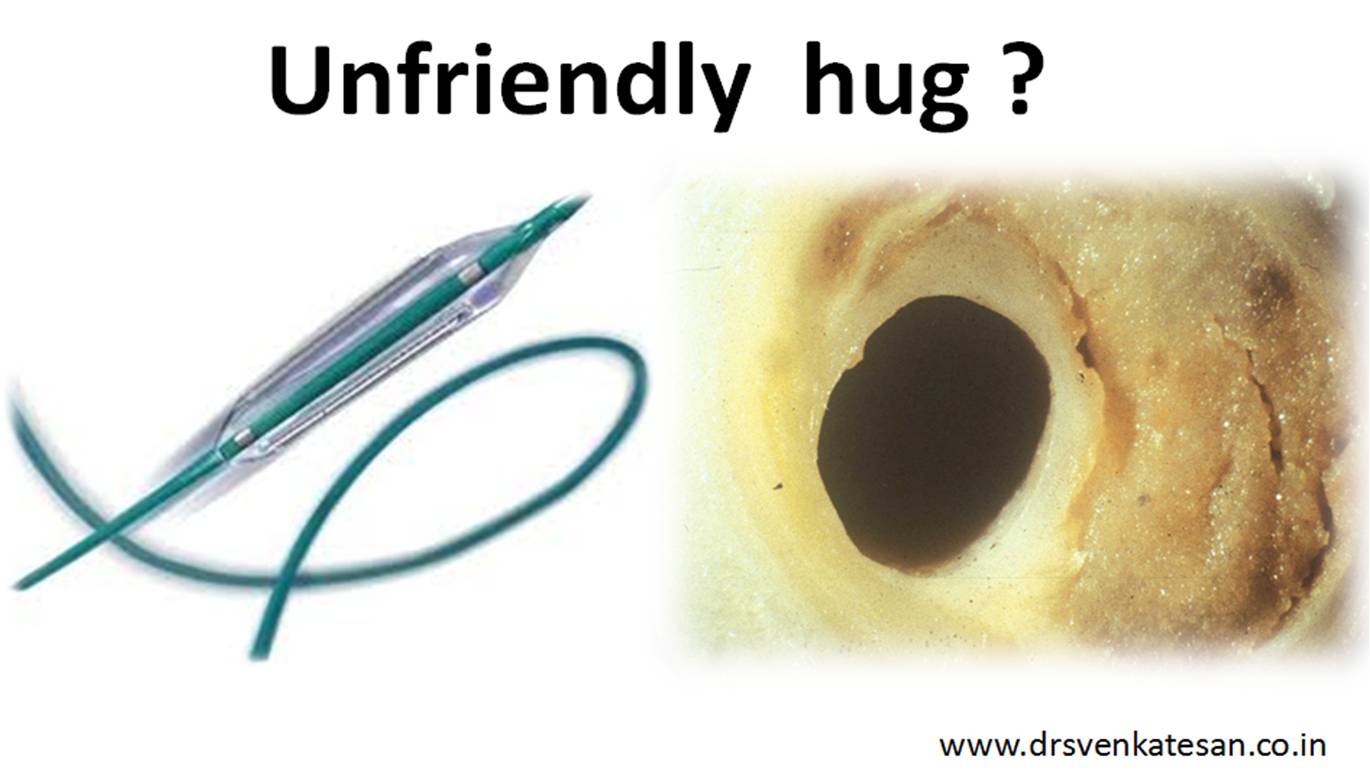
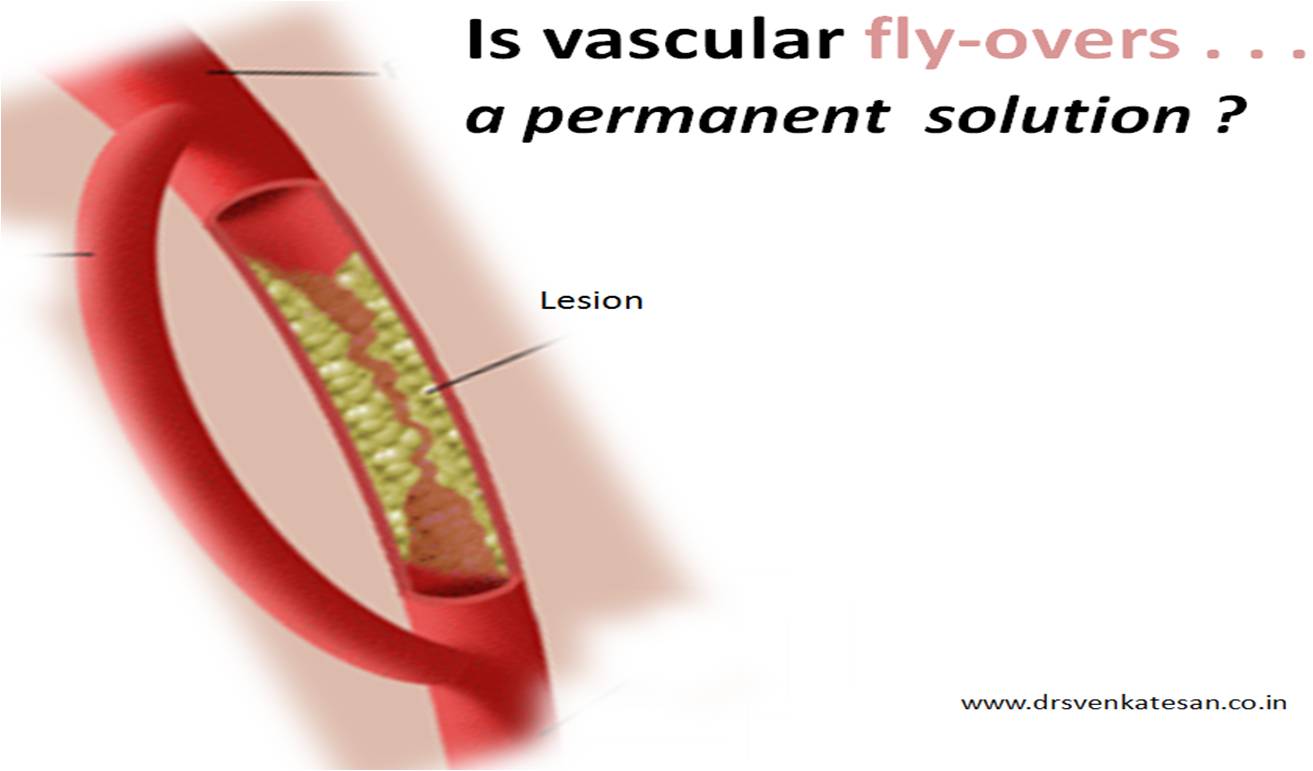
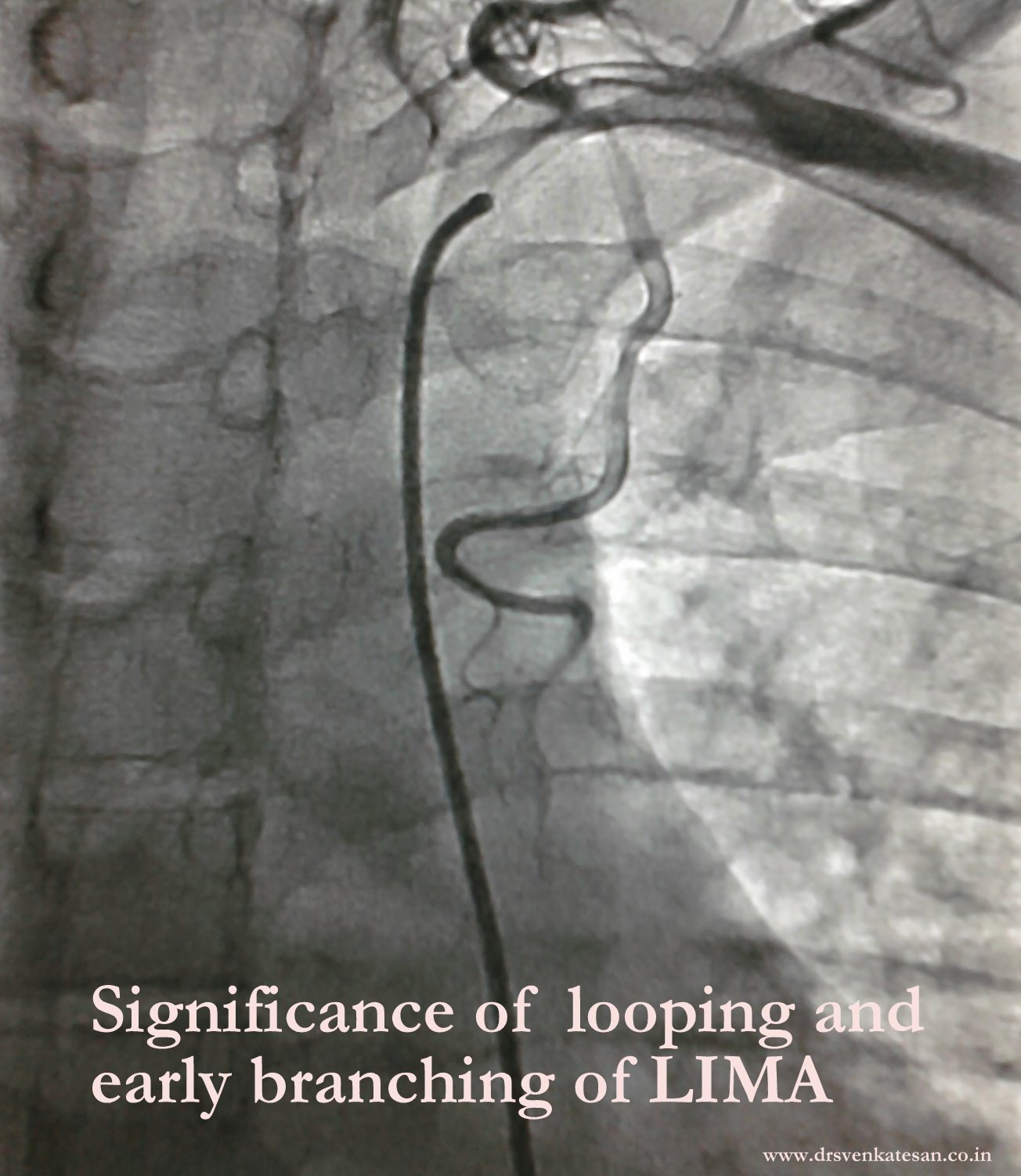
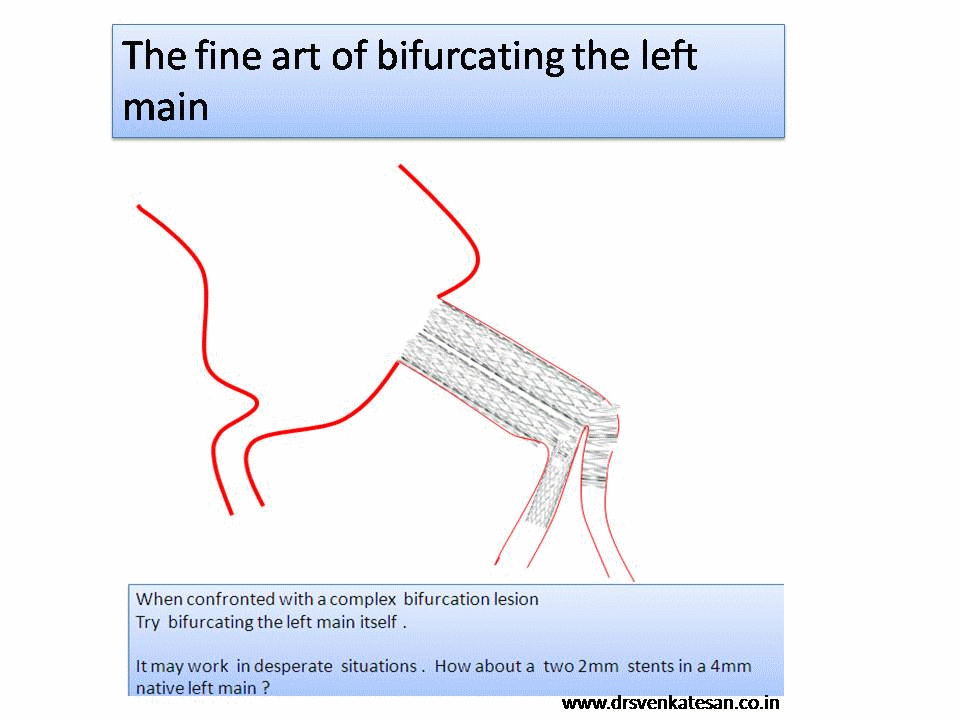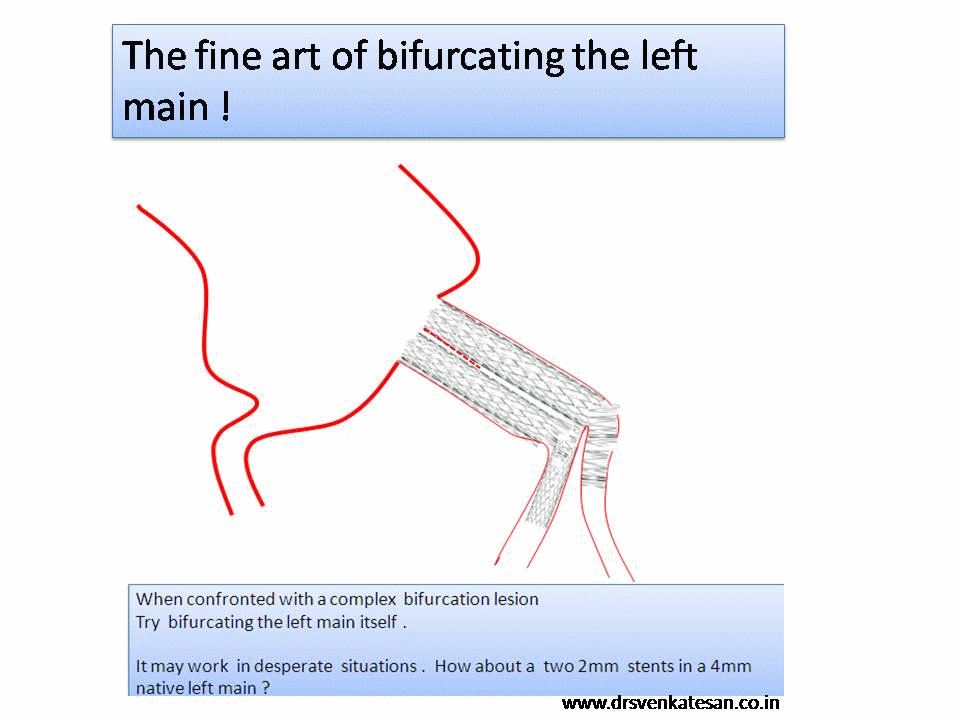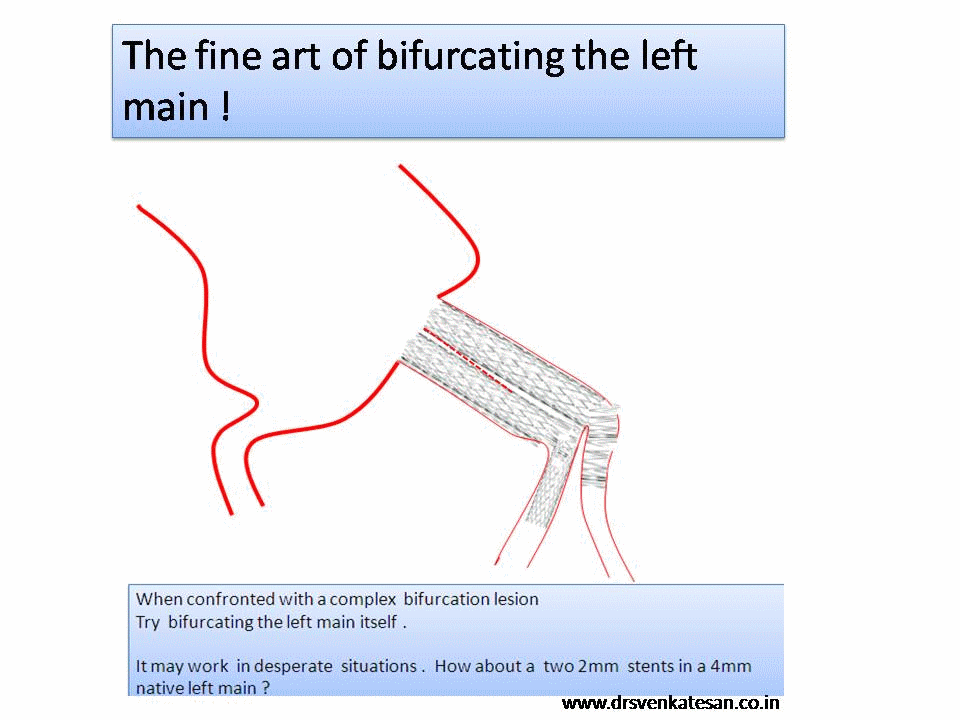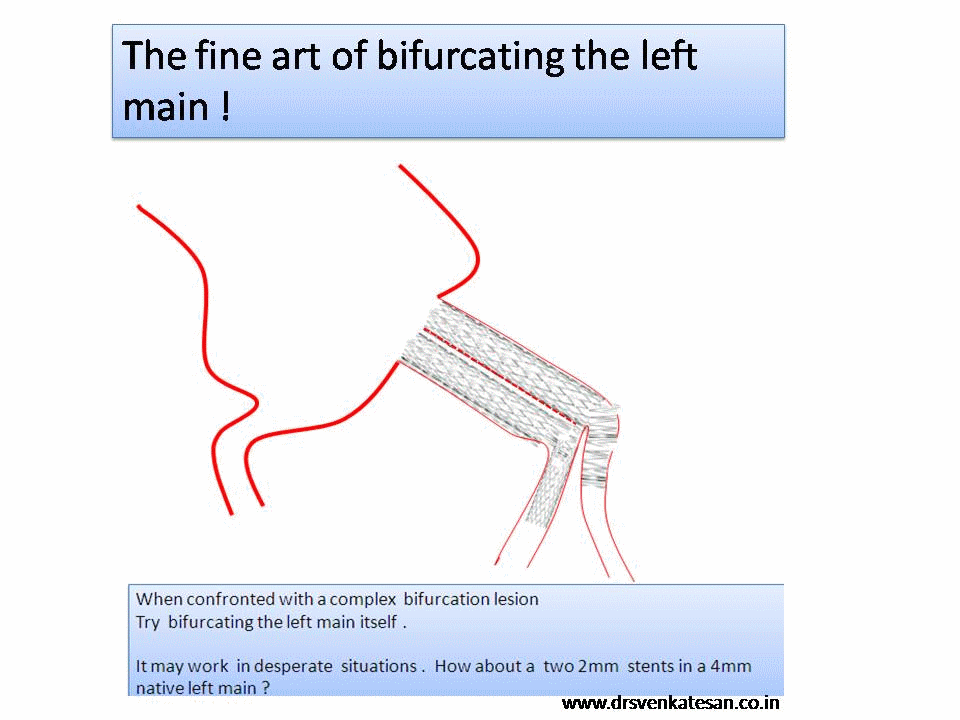
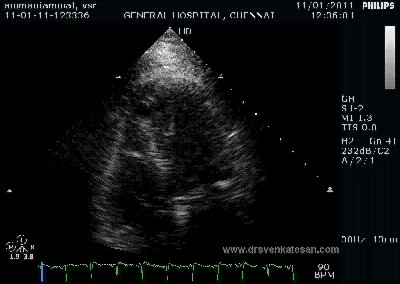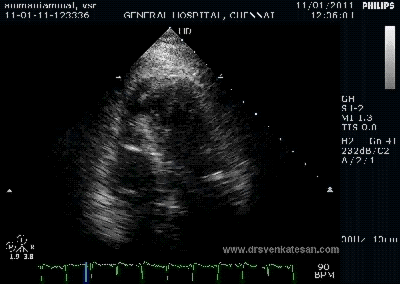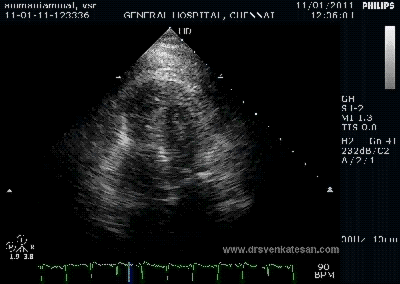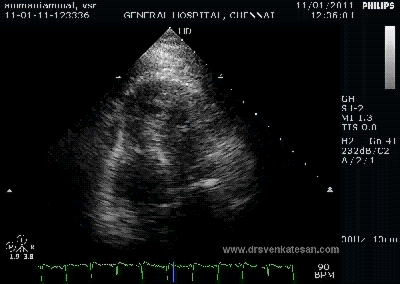
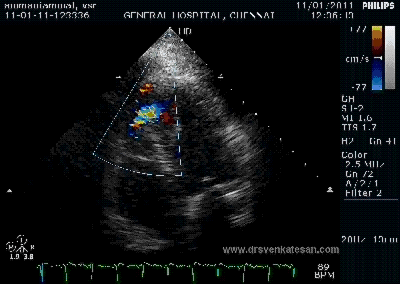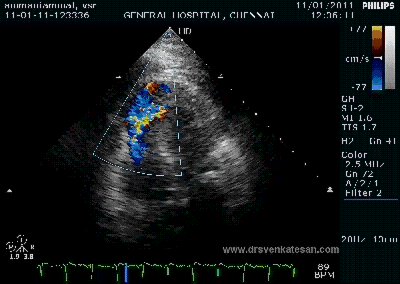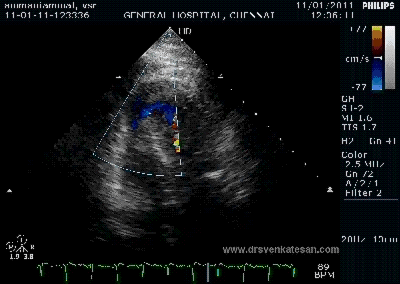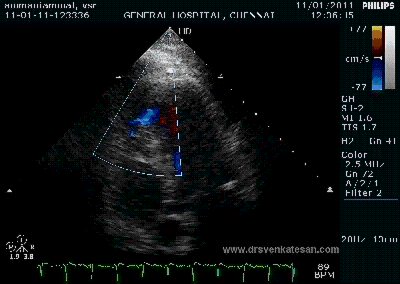
It is a well known fact , CABG and PCI provides immediate relief for patients with angina , which is refractory to medical therapy. Of course , this happens only if a critical occlusion of at least one epicardial coronary artery is opened . It need to be realised , angina due to microvascular disease can not be cured by maintaining epicardial patency .
While angina relief is prompt , dyspnea is not ! . If we believe, opening up a coronary artery in a patient with LV dysfunction will restore the LV function , it is grossly mistaken !
Why is it so ?
Angina relief requires simple restoration of oxygen supply and correction of local ischemia . This happens without any issue as the blood seeps in to the ischemic cells and soothes the ischemic nerve fibres that trigger the pain signals . While , for LV function to improve , the blood flow has to be converted to mechanical activity in the form of myocyte actin/myosin interaction. For this, there need to be an intact cellular contractile mechanism . The myocyte architecture should be appropriate .In post MI ventricles we know there is zig zag orientation of myofibrils due to myocyte slippage that interfere with mechanical recruitment . Further , integrity of extracellular matrix namely the collagen frame work is also vital . Note , angina relief is not concerned with any of the above .
And now , we also realise dyspnea in failing ventricles is vitally dependent on diastolic function , which is also very much impaired in ischemic DCM .There is little proof for PCI/CABG to correct the molecular mysteries in diastolic dysfunction !
Dysfunctional LV means what ? (read the link )
It is a collection of variety of myocardial tissues . Viz : Fully necrosed , partially necrosed , ischemic viable, non ischemic viable, ischemic non viable, non ischemic non viable , Apart from this patchy necrosis, patchy ischemic, areas are common. Finally , necrosed segments may also be perfused normally by spontaneous reopening of an IRA.
One can imagine the complexity of events in these segments once we do the PCI /CABG . The response is highly variable and unpredictable. The major concept we , the physicians believe or ( to be precise made to believe !) is the sanctity devoted to the viable myocardium .For many us , it is considered a holy exercise to identify viable myocardium in patients following MI and then revascularise them if found to have significant viable myocardium (Atleast 20% of infarcted area )
A full 2 decades were lost or (shall we say wasted on this futile exercise !) as we have since realised most of the cardiologists do not follow this rule .
Now , even a scarred myocardium is revascularised in the hope of recovery .As such , we have reached a stage where there is no contradiction for not doing a PCI /CABG with reference to LV dysfunction.
Now every patient with post MI LV dysfunction is considered to have some amount of viable myocardium that is fit enough for revascularization
Are we justified in doing this ?
Many clinical trials have revealed , the recovery of LV function in these segments has not been consistent at all .
The most surprising discovery is a viable myocardium need not be ischemic .It might get adequate blood supply either from invisible collaterals or trickle of antegrade flow . Hence an adequately perfused myocardial segment can still be non contractile . This shatters the myth that revascularisation must have a dramatic effect on the recovery of contractility in all viable segments.
The other major finding is , even ischemic viable myocardium ( documented by metabolic activities PET etc) need not regain it’s original contractility after the ischemia is fully corrected .
*reference for both the above statements are available from variety of sources including real life experiences .(Type C evidence )
Final message
- Do a PCI/CABG promptly for patients with refractory angina.
- Never advocate PCI/CABG for a primary relief of dyspnea . (Never is a harsh word, let it be “use it with caution ” ! and the patient should be revealed the whole facts about what we know and what we do not know regarding the complex hemodyanmic events in revascularisation )
Counter point
If the above statements are really true , How does PCI/CABG help relieving dyspnea and functional class what is your answer for thousands of patients with CAD and ischemic DCM who have greatly benefited from CABG ?
The answer could be simple , The revascularization piggybacks over the medical management (which , these patients pursue vigorously) like ACEI, statins, salt restriction, betablockers , optimal diuretics and tend to hijack the credits from the poor drugs !
Read a related blog
Revascularisation for ischemic DCM
Read Full Post »