We are at the mercy of the three major coronary arteries (LAD,LCX,RCA) that sustain our life . Their job is clear cut .It has to perfuse about 300 Grams of live bundle of energy for an average of 6-7 decades.
What are the hurdles it faces , how it overcomes these obstacles forms the fascinating story of “survival of human heart”
When coronary blood supply is confronted with a sudden compromise as in ACS , often the heart has little time to respond . Hence the damage and risk of death is more. Even here there are lots of safety mechanisms and natural lytic process that limit the loss of life to less than 30 % of all STEMIs. This implies nature protects against the death in 70 % of individuals and help them to reach hospital.*
*Among those who reach hospital , we the cardiologists try to reduce the mortality to about 6-7 % (20% without treatment ) with all those hi-tech gadgets .It is a different story and will be addressed elsewhere .
When it comes to chronic insults , the heart has a unique potential to stage long haul battles. It has many tricks under its sleeves when challenged in a slow fashion.
The main weapons are two
1. Coronary collateral circulation.
2. Ischemic preconditioning.
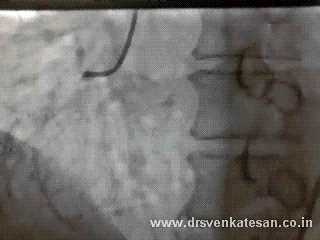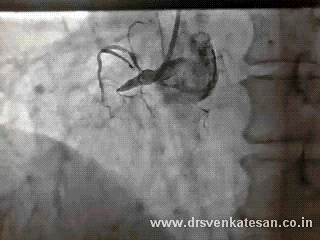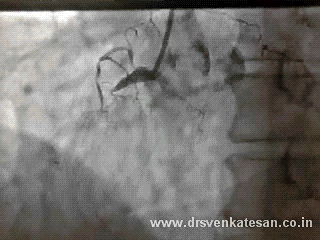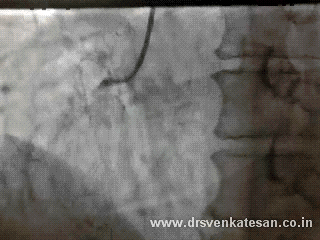
Here is a patient who fights his life even after all his three coronary arteries totally blocked and surviving with one of the branches of left main -Ramus intermedius .
If you have thought his RCA was the savior you are mistaken .
To every one’s surprise his RCA was awful as well !
He had angina which was troublesome but manageable .Was able to live a life with acceptable standards (Indian standard ) After the angiogram he received CABG. A turbulent post operative course ensued due to various reasons . He struggled but fully recovered . . . and ultimately reached the previous standard of life !
Final message
Modern cardiology is all about not trusting powers of nature .
But youngsters should realise the enormous potential of those invisible powers.It may sound philosophical , but please remember . . .after all . . . philosophy is nothing but search for truths. Atleast believe in them once in a while !