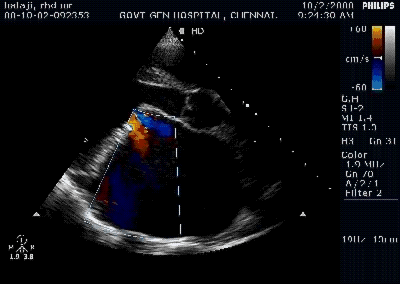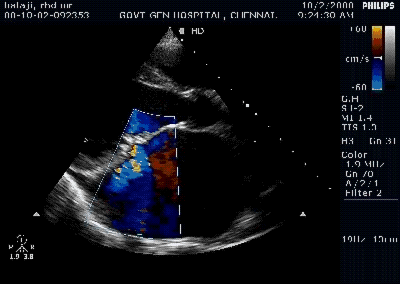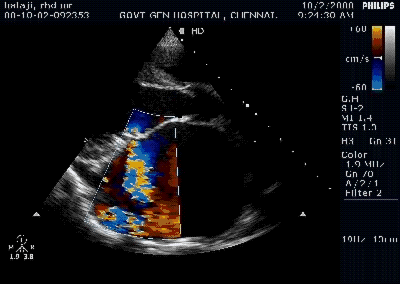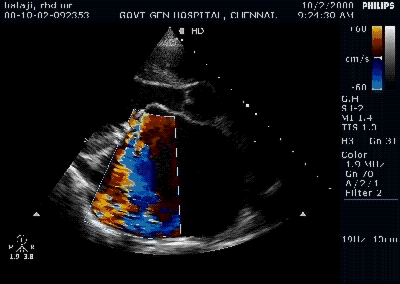
Pericardial effusion is often detected in patients with Infective endocarditis. Incidence can be as high as 25% . Most often it is mild, can be moderate in few.
Mechanism
- Sympathetic effusion in response to endocardial infection. It’s never more than minimal. (Evidence ? it’s only an assumption)
- IE related cardiac failure (Raised systemic venous pressure to which pericardial veins drain)
- Local sepsis, Abcess formation tracks to pericardial space through transmural lymphatics
- Fungal , granulomatous , Tuberculous IE (Rare) Here IE and PE share the same pathology
- Part of systemic sepsis activated Immune mechanism (Polyseroists)
- Renal Involvement of IE-Renal failure
- Postoperative pericardial effusion in Prosthetic valve IE (Common, often loculated)
Clinical Implication
- If the pericardial effusion is more than mild, it often denotes worse outcome. This implies more extensive infection or a marker of extracardiac causes of effusion like renal dysfunction.
- Effusion may predispose to local dissemination of infection and ends up as peri-annular abscess is whether it is a cause or effect of effusion remains to be understood.It is often exudate as one would expect, but transudative effusions also occur and would indicate more benign course.
- The sterility of pericardial fluid has not been proven. Culture studies are rarely done from effusions associated with IE.
- Pericardial effusions appear more often seen in IE of right heart valves. They turn out to be IV drug abusers.
- Contained rupture of an abscess needs to be differentiated from effusion
Can we give steroids for PE associated with IE?
Steroids can rapidly plug the inflammatory pores in the from the pericardial surface.It may also prevent future constriction. Currently, routine steroid therapy is not advised in infective pathology . If the infection is confirmed and is being taken care of by antimicrobial therapy there could be a role for steroids with user discretion.
Final message
During the echocardiographic evaluation of IE, the presence of pericardial effusion should be specifically looked for. These patients should be flagged and will require monitoring as the prognosis of PE complicating IE is a concern unless proved benign.
Reference
Two studies one from Spain and other from Egypt looked into this issue specifically.