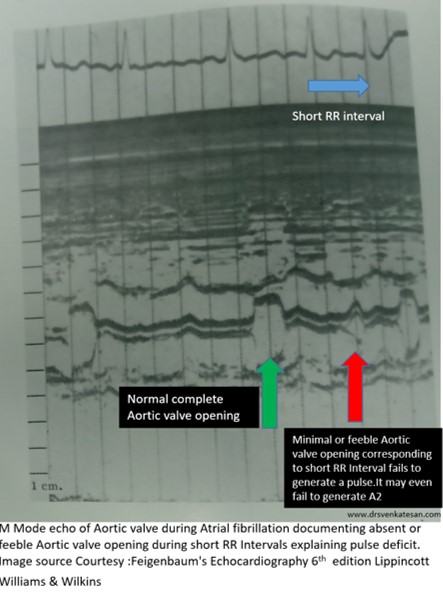
Atrial fibrillation has a direct effect on systemic blood pressure as stroke volume swings from beat to beat because of changing RR Interval ( preload ). The variation in systolic pressure actually reflects not only the changing stroke volume but also the enhanced contractility of the ventricle to the preload( Frank-Starling principle ). The net effect is reflected in the pulse as an irregularly irregular pulse (Both rate and volume /Amplitude).* However, In dysfunctional ventricles or in acute AF* this variation in systolic BP can be significant. Also realize, If the preload is changing every beat, there is a considerable dynamism in the afterload as well because of ventricular arterial coupling.
(*Acute effects on BP with the onset of AF : There can be transient hypotension with loss of atrial booster pump.This is not significant in otherwise healthy hearts. Inpatient with baseline LV or RV dysfunction, the onset of AF can be detrimental. The ventricular rate is also a determinant of blood pressure. At fast rates, there can be a fall in BP)
How to record BP during AF ?
As you record the BP by cuff, the Phase 1 Korotkoff sound floats up and down with each beat. If the variation in RR interval is huge one may get a beat-to-beat variation even up to 40 mmHg.We also know, AF can cause pulse drop /deficit intermittently.
What happens to Korotkoff sound during pulse deficit?
Obviously, there will be a loss of these phase 1 sounds, though the other phases of sound may be heard, which are generated by the previous cardiac cycle. So, measuring blood pressure in AF is not a clinically pleasant task. That’s why we are asked to record 3 times and take an average.
Now, coming to diastolic BP in AF. It’s a real hemodynamic riddle. Traditional teaching is, systolic BP is determined by cardiac output and diastolic BP by peripheral vascular resistance. This is at best a gross understanding of circulatory physiology. Both systole and diastole are coupled together as blood flow across the system of varying resistance. In fact. The preceding systolic pressure head stores the elastic energy in large vessels that are thrown back as diastolic BP.
So what happens to BP during AF? What does the literature say? It doesn’t say much. So we decided to look for ourselves. Here is a tracing of femoral arterial pressure curves during atrial fibrillation. Note: the systolic BP shows considerable variations with changing RR interval with little change in diastolic blood pressure.
Final message
In Atrial fibrillation, the systolic blood pressure changes from beat to beat and it impacts the timing of the Korotkoff sounds. The diastolic blood pressure behaves the same, but it’s less in magnitude and difficult to detect by conventional sphygmo-manometry.
Further reading
Clinical Implication for irregular BP of Atrial fibrillation :https://drsvenkatesan.com/2021/05/04/cerebral-hemodynamics-in-af-irregularly-irregular-brain-perfusion-and-risk-of-dementia-cordis/
The effect of AF on pulmonary arterial pressure is an unexplored topic .Cardiology fellows please note.