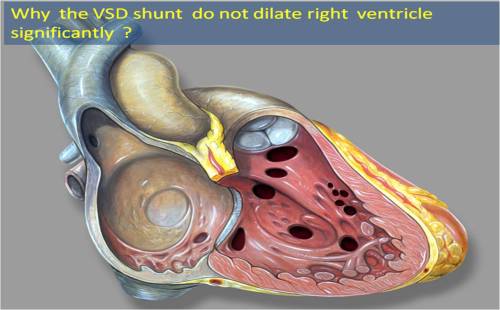
The following questions are asked frequently in clinical cardiology classes on congenital heart disease.
What are the chambers that dilate in ASD ?
Right atrium and right ventricle .
What are the chambers that dilate in VSD ?
LA, LV , ± RV,
* Image courtesy Wikipedia
While there is no controversy about ASD, The chambers that enlarge in VSD , is by and large poorly (or rather wrongly ) understood . Whenever we diagnose VSD , our brain is tuned to think this way : Blood will be shunted form LV to RV. RV would handle more blood and it should enlarge . In reality it does not happen.
The VSD shunts the blood from LV to RV outflow* or even directly into pulmonary artery . Hence , VSD even if it is large , does not dilate the RV until the onset of pulmonary hypertension and RV dysfunction sets in . It is surprising to note , even the RVOT ( The entry point of most VSD jets) does not significantly enlarge
Importance of diastolic shunting in determining RV size in VSD
It is also important to recognise, the VSD shunt predominately occur in systole .(90% ?) In systole , the RV is also contracting along with LV , so it’s size is diminutive and hence RV can not be volume overloaded in most of the VSDs however large it may be. Instead in ASD , there is diastolic overloading involving all regions(Inflow, Body, Outflow) of RV .This enlarges the RV in a classical fashion.
Significance of anatomical location of VSD and RV enlargement
When VSD shunts blo0d into RA as in Gerbode defect it is bound to enlarge RV (like ASD) as there is diastolic volume over load of RV.
In some large muscular VSD , RV body can be volume overloaded. This is because the VSD and RVOT are well separated geographically .The blood that is coming in from LV can enter the pulmonary artery , only in the next cardiac cycle . So , RV needs to accommodate the shunted blood till the next beat. Hence RV enlarges.
What are the situations RV can enlarge significantly in VSD ?
- Rare VSDs of inflow or large muscular VSDs.
- Eisenmenger syndrome.
- Tricuspid regurgitation
- Pulmonary regurgitation
- Associated RSOV.
Final message
Right ventricle does not enlarge significantly in uncomplicated VSD .This is in contrary to the traditional teaching and understanding for many years. It enlarges only in specific sub types of VSD or after the onset of PAH and cardiac failure .
Coming soon
Katz-Wachtel phenomenon is not due to bi -ventricular hypertrophy !