Time window for intervention with thrombolysis in STEMI starts from onset of chest pain, but when it comes to primary PCI, a different time window takes the center stage, pushing the former to the background. In primary PCI, the distorted time window starts right from the patient arrival at the door of (either the ER ) or cath lab, and many times, endlessly extend beyond the prescribed time.

Why this dichotomy ?
No guideline bothers to reiterate , that if the S2D time is prolonged, D2B need to be correspondingly short or ultrashort. How can we have uniform standard of 90-120 minutes D2B in all STEMI cases ? Why the cardiology community is silent on this crucial time mis-management error ?
Answer
I think the answer should be one of the following .
1.It is intentional .
2.Ignorance
3.To favor the perceived superiority pPCI .
Only time will answer.
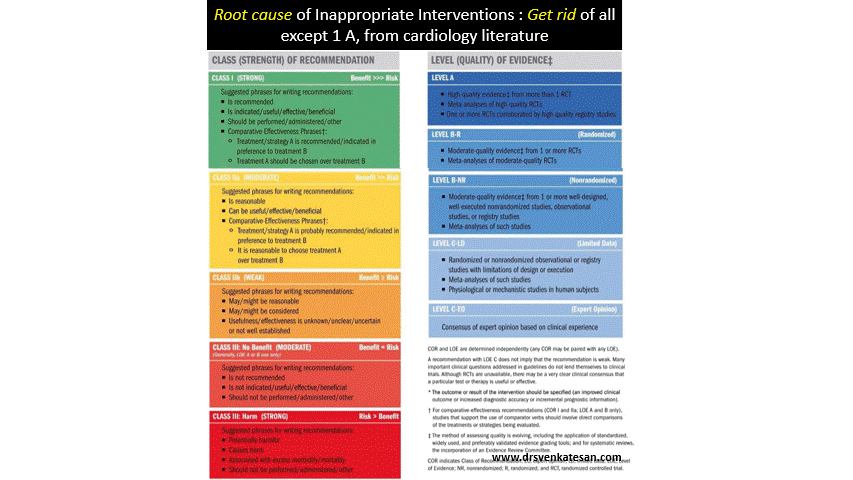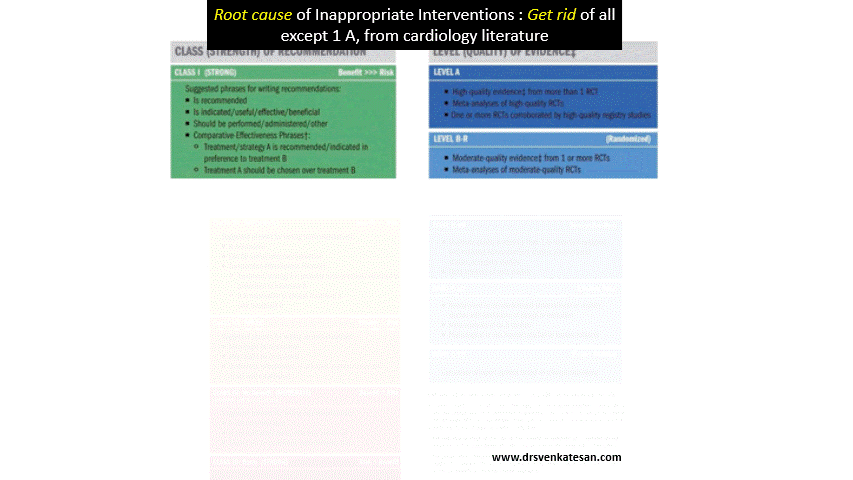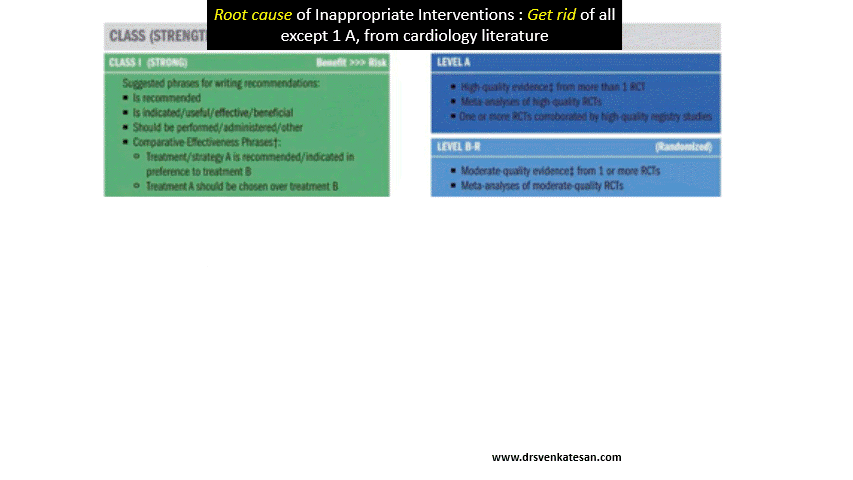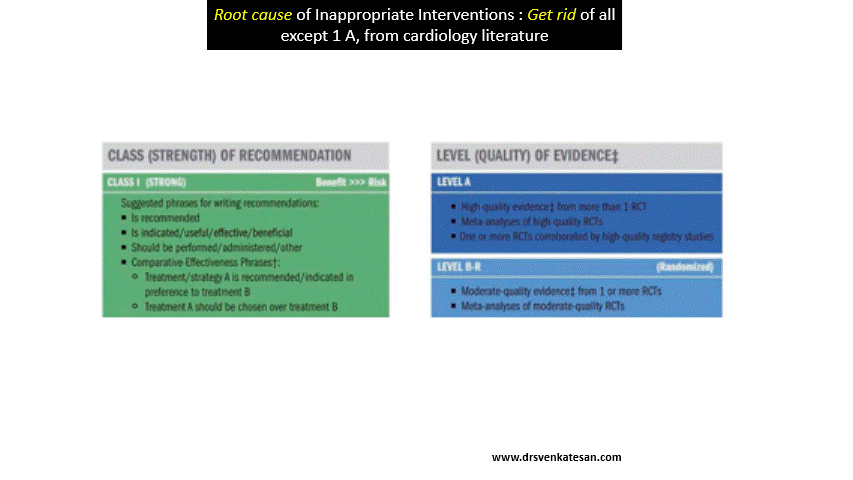
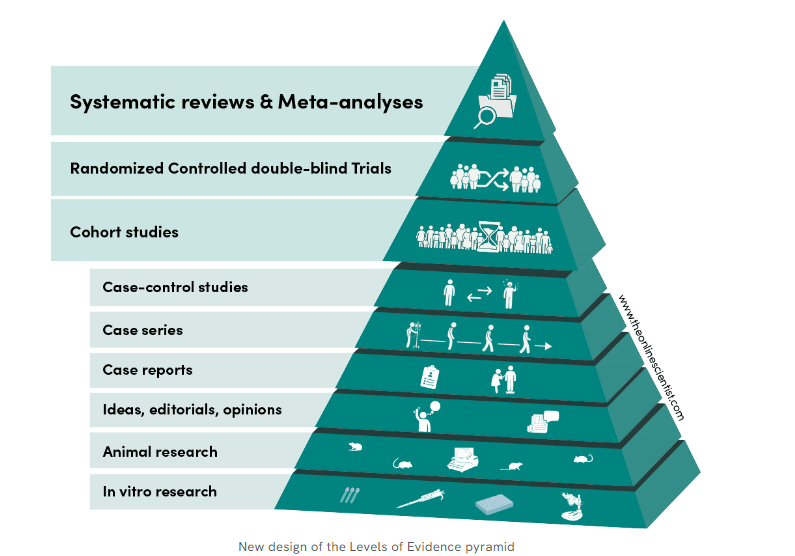
Curiously, none of the globally accepted standard guidelines seem to realize that, they have not given sufficient weightage to this aspect of coronary time window , while gathering the evidence.(Most papers on pPCI never mention about S2B times vis a vis with IRA TIMI flows)
Final message.
No amount of guidelines will lead us to proper pathway of coronary care ,unless we are ready to course- correct and eliminate basic errors. Of course, If we are knowingly straying from the right path, there is no escape for our patients from science.
Post- amble
How is this possible in this cutting edge scientific era.?
*The problem with hyper Intelligence is, that any amount of scientific evidence can be created to show, what we are doing is right.
What could be a lesson we can learn here ?
If symptom to lysis time is less than 50% of Symptom to balloon time , probably,every such patient should enter “pharmaco- Invasive or pharmaco only” strategy according to the prevailing CAG anatomy.
Counterpoint
D2B is under you control. S2B is not in your control*, so simply don’t bother about the former. The other possible argument for ignoring symptom to balloon time ,is late lysis doesn’t work that effectively, hence the only option is PCI however delayed it is. But, in the process, we forget , most times we are the ones who created this deadly delay and master the art of loosing the golden hour in STEMI , that is backed up with flawless RCTs.
*Is S2B is really not in out control ? Yes , it is true, until we replace S2B to S2R (R-Revascularisation) time. This is unlikely to happen as long as we strongly believe balloons have the exclusive capacity to revascularize the IRA.
Reference
S2D -Symptom to door time
S2B-Symptom to balloon time
D2B– Door to balloon time
S2R*-Newly proposed . Symptom to revascularisation time (any modality)