*This post may not be meant for cardiology fellows but for young students of medicine
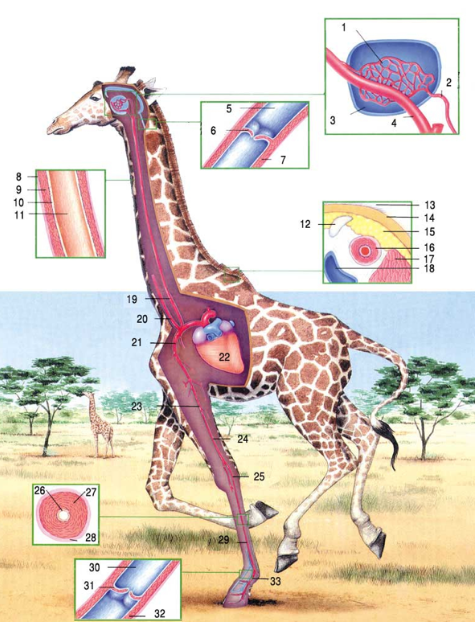
Have you ever thought about how a Giraffe’s heart can pump blood to the summit of a lengthy neck and perfuse the brain?
Unlike a blue whale which has a huge heart, a Giraffe’s heart is not as big as one would Imagine, A Giraffe’s heart weighs .5 to . 6 % of total body mass. If the average weight of a Giraffe is 650kg, the heart would be around 3 kg.It is almost in similar proportion to the human heart.( In a 70 kg man heart weighs about 350 grams). However, it generates more power and pressure, up to 300mmhg BP.
Lessons from Giraffe heart
1. Although the heart is not big, the walls are thicker many times times. In simple terms it mimics a heart of Hypertrophic cardiomyopathy, which we know has brisk ejection. The combination of thick wall and a small cavity attenuates the wall stress significantly .This enables the heart to pump a good stroke volume, high into the brain located more than 5 to 8 feet above the heart. What a remarkable phenomenon.(Laplace law executed in the best manner in biology) *Laplace law states , the wall stress is directly proportional to the cavity diameter, indirectly related to the thickness of the wall
2.We can also understand the principles of the management of cardiomyopathy from a Giraffe’s heart. If the ventricles assume a tubular morphology, optimal energy and cardiac power can be accrued. This forms the basis behind the ventricular reduction and reconstruction surgery for Ischemic dilated cardiomyopathy.(Batisda procedure etc)
3.The innovators and engineers of new-age mechanical assist systems could learn a few crucial insights from these unique and humble animal beings. (Shall we think about,axial pumps in ascending Aorta in series with LV. An Aortic Impella device, that is distal to the aortic valve and devoid of LV-related issues. )
With each systole, blood has to travel a maximum of up to 8 feet up, with enough power at the same time not to injure the vessel wall
When bending the opposite happens, and the valves in both arterial and venous systems come to protect by dampening the flow and avoiding congestion.
An alternate hypothesis: Siphon effect in cranial circulation
Some believe the heart is assisted by an alternate mechanism in the Giraffes. The carotid artery could act like a siphon from the heart. Siphons can defy gravity. Is it a reality in living beings? How is this possible? I am not clear. If so, that can be tried in human experiments on cerebral insufficiency.
Final message
Every living and (even non-living things) surrounding us, keep sending some silent scientific messages. The hemodynamic of the Giraffe’s vascular system is a good physiologic model of circulation, that defy gravity. It reinforces a basic, but important learning point* that a tubular & cylindrical heart can generate more power than a large globular one.
Reference