As the medical literature expands exponentially, the quality and intent of the research questions sound awry. There are only a handful of journals like JAMA that are bold enough to ask some tough and pragmatic questions in this glitzy world of medical extravaganza.
The current issue wants to set the pace for an important debate, on a topic that is rarely discussed.
The question is

Check whether your answers concur with this crucial query from Harvard Medical School and Massachusetts General Hospital. Three questions this article wishes to address.
1.What is the reason it is happening?
2. What are the implications?
3. What can be done for it?
My thoughts
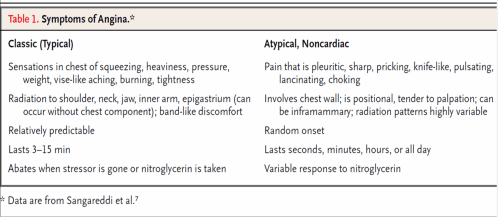
“It is indeed over diagnosed. Once labeled, a chain reaction is set in. The cost, and resource consumption that follow a misdiagnosis are nearly identical to that of a true MI. More than that, the adversities of the tense investigative protocol can convert a misdiagnosis into a real one because that sadly includes even an overzealous poking right at the mouth of the coronary artery just o exclude a non existing MI . and ICU-related anxiety stand apart in this scientific comical game of ruling out a cardiac emergency.
The paper seems to blame mostly on the powerful screening test high sensitivity Troponin, Everyone will agree it has a major role in this. But, the more important reason is the cardiology community’s vigorous adoption of a universal definition of MI criteria (which is never intended to apply at the bedside) .Next factor is probably more important. The fear of missing a potential MI and legal consequences thereafter. I wish, the experts who sit on medical juries need to learn few extra lessons in the art of medical uncertainties.
Medical jurists, need to take some Intellectual cues from their criminal courts. How is it that, even well-planned criminal murders are successfully allowed to be argued and won in courts,…while inadvertent events such as missing an inconsequential MI by doctors are rarely pardoned?
How to avoid over diagnosis of MI ?
In this scenario, It is sad, that only very few cardiologists have the guts to ignore this omnipotent molecular sub-fraction of cardiac muscle Troponin, with their clinical skills. What we can do, at our level is to incorporate a new term “benign or micro myocardial Infarction” – akin to lacunar infarcts or TIA equivalents of the brain in the heart. We need to de-list the vast majority of chronic ischemic,non-ischemic, or systemic causes of Troponin leaks from the myocardial infarction chart. Physicians must realize, that protocol violation should not be deemed a crime always, rather it has a sure potential to benefit your patient if it is done properly and intelligently.
Final message
Recently one cardiologist in a sub-urban center was thrashed both physically and in social media ,for missing an ACS , which was subsequently recognised and treated well and good.
“Doctors should be legally allowed,* (rather forgiven) to make permissible levels of errors in the medical decision-making process ” like any other profession .However, we must ensure our constant pursuit towards zero error, which may not be possible always. This should include overlooking apparently positive lab results if they have reasonably applied their clinical acumen. *Until this happens, the unquantifiable suffering of our patients* due to over-diagnosis and inappropriate interventions can not be reigned in.
*Maybe, this sounds more controversial statement in my 15 years of writing. Beloved patients shall note, it is a rare for me to make what probably, look like an anti-patient statement. Till now, I have been blamed my many of our colleagues, as self slandering my own profession for too many errors in many of the posts. Nothing can be done for this. When you search for truths , you need to tolerate all these.
Reference