Hi all ,
I get frequent comments about my blog. I do try to answer many of them . This is a very unique one , and it is making me think further.Since he has specifically wished his clinical data could be eye opener for others , I am jut posting it here . The comment was in response to my article Who said coronary collateral circulation will not support exercise ? here is the extract
Dr. Venkatesan,
I read your blog with great interest and I think I may have something useful to contribute from my own personal experience. I am a 68 year old male with a long history of smoking (for fifty years), and a history of uncorrected hypertension over the years (it has been corrected to normal with medication for many years now). I am a non-smoker now for the past 18 months. I have PAD and a moderate aortic aneurysm of about 3.5CM (ascending and descending) which is being watched with regular vascular scans.
The common femoral arteries in both of my legs are nearly 100% occluded between my thighs and my knees, and yet my ankle and toe blood pressures (and my circulation in my ankles and feet) is almost normal. The reason for that is that according to the vascular scan, my deep femoral arteries are much larger caliber than normal with extensive vascular collateralization by passing the common femoral occlusions.
About twenty years ago before the PAD diagnosis, I realized that I had claudication in both of my calves when I walked a short distance. I expected this was being caused by an arterial blockage in my legs, so I went to the gym every day for about three years, and walked through the pain every day. I believe this contributed to the formation of the collaterals that have perhaps saved my legs and feet.
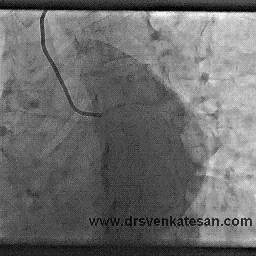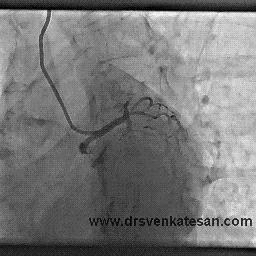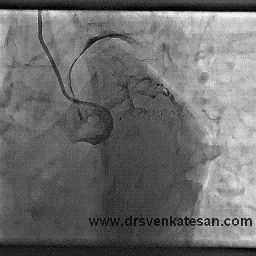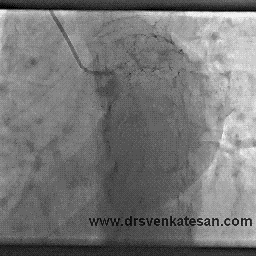
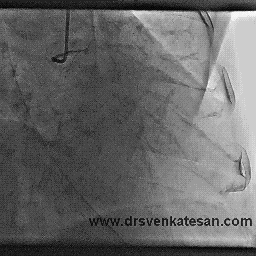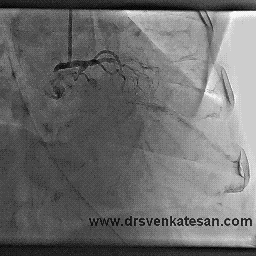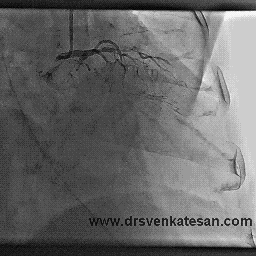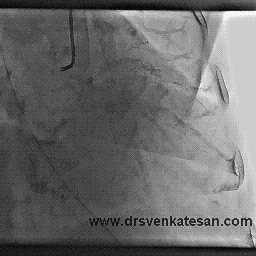
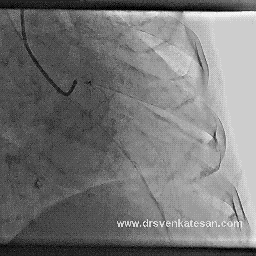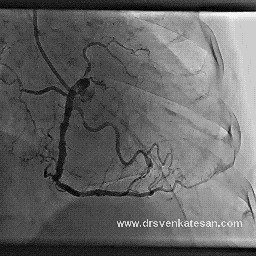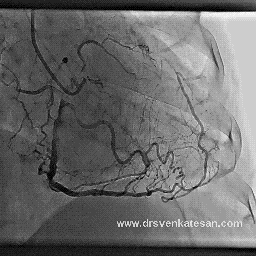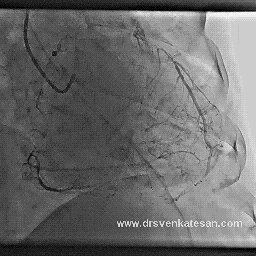
I also have heart disease, and had a fairly minor heart attack in 1999. No stents were placed nor angioplasty performed at that time. I recently had an arteriogram and cardiac stress MRI which showed that two of the three coronary arteries are now 100% occluded (apparently I had another cardiac event and did not know it). The cardiologist says that the LAD is in extremely good condition and has numerous collaterals branching from it. I have no symptoms whatever from all of this, except that my LVEF is low (about 35%). I walk at a very brisk pace six miles per day, five days per week, and I monitor my pulse rate with a pulse monitor when I walk. I keep my pulse between 115 and 120 which I calculate to be 80% of maximum for my age. I believe this cardio exercise / walking has also helped with the collateral formation, and I am hoping to bring the LVEF back up to a reasonable number with this exercise regimen.
My cardiologist has recommended an ICD, but I have decided against that since I have never had VT or VF or any other type of cardiac arrythmia (except for non-symptomatic PVC’s which I was born with).
I believe that I am the lucky recipient of good genetics to begin with, but also I am highly motivated now to take better care of myself, and know as much as I can about the conditions that I have. I plan to have an echocardiogram in six months to see if the LVEF numbers have improved, and I fully expect that they will have. I give credit to the smoking history for the vascular problems that I have including the cardiac problems. I am a lucky person I think, and suspect that not everyone has the fortunate ability to heal themselves the way I have.
I have asked for copies of my arteriogram and stress MRI records. If you are interested in looking at these I would be happy to share them with you.
The letter ends .
Dear Mr Weigel
Yours is an extremely interesting story told in a most scientific manner.Thank you .
It gives me great insight , how a human vascular system can transform when confronted with natural disasters like multiple blocks on its way .A flowing river will definitely reach its destination however bizarre the path it takes . Human biology is vested with vast reserves of genetic building blocks put on sleep mode. While billions of dollars are being pumped into do research in human angiogenesis we have tuned a blind eye to the vast net work of natural collaterals.
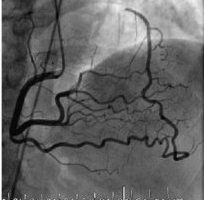
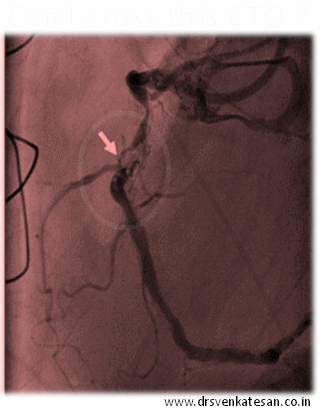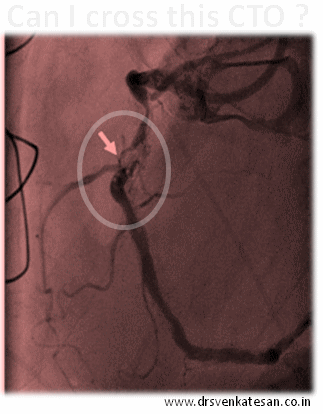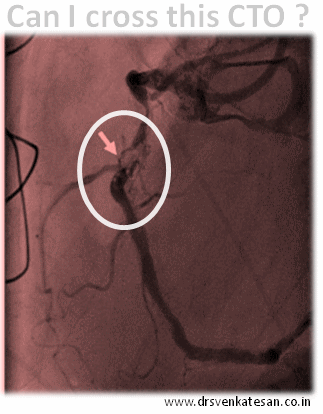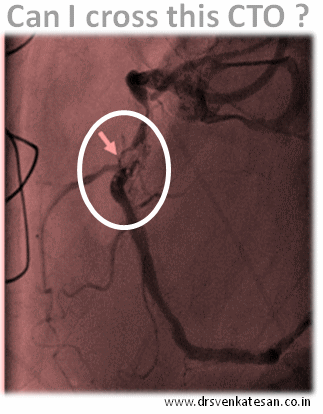
Our clinical experiences also tell the same thing . In chronic total occlusion majority of patients would develop good collaterals if only we do not tamper the main vessel .None of scientific studied available has proven opening CTOs (Chronic total occlusions) has improved the clinical outcome .
Regarding the guidelines for revascualrisation , I am yet to come across a standard scientific guidelines that includes the extent of collateral circulation as one of the determinant for need for revascularisation !
I will definitely use your case study for the benefit of so many patients ! I always feel , a properly interpreted experience , even from a single patient can make a tremendous impact in the growth of science .
Thanks again for sharing your personal health issues !
Dr Venkatesan
Chennai .India .
Read Full Post »