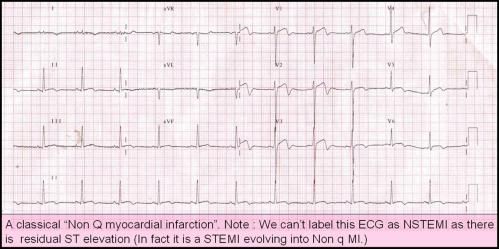
Now , some one wanted to know, Can we diagnose unstable angina without Chest pain ?
Crazy question isn’t , Angina by definition should have chest pain .There is nothing called silent angina , only silent Ischemia .
- We know Ischemia can occur silently .
- We also know STEMI can occur silently (About 10 % of MI do occur without any symptoms )
- If STEMI occurs silently why not UA/ NSTEMI combo ? (Collectively called as NSTE-ACS)
The debate goes like this .If stable angina can present with equivalents ? what prevents “Unstable angina” to present with Anginal equivalents without chest pain ?
If a diabetic patient who had a silent MI in the past . . . subsequently experience severe episodes of resting ischemia , will he feel the pain , that is supposed to occur with his “unstable angina” or not ?
Hmm , difficult to guess right, So it seems highly plausible UA/NSTEMI do occur silently ! Literature hasn’t looked into this specifically. Chest pain is built integral into definition of UA , infact it is a symptom complex rather than an disease entity by itself, while NSTEMI is ECG and enzyme combo ! Making the term NSTE-ACS look perfect.
Any other technical explanation ?
The concept of Ischemic cascade says angina occurs last, well after biochemistry , wall motion defect and ECG , hence its distinctly possible for UA/NSTEMI present to be painless !
Final message
Anginal pain perception is related to intactness of neurogenic circuits and also probably the severity of Ischemia.If full thickness myocardial necrosis can be painless in few, nothing prevents from an episode of UA/NSTEMI be truely painless .
Clinical implication of this conundrum
Can we admit a patient as UA/NSTEMI with out chest pain ?
Yes, it would seem so .
No, we can’t .
Indeed we can , if ECG changes are there .
No, we can admit even with normal ECG if its real unstable angina.
This is the crux of the problem in ERs all over the globe. Our knowledge base is simply not good enough. Every one of us has seen Troponin positive silent NSTEMIs ! but . . . to me still something is missing in the link .
Modern day approach
Pain or no pain,any fresh ECG changes ( Both T and ST shifts*) should be rushed to cath lab.Whenever you are not sure .Always better to err on the side of over investigation.That’s the mantra ! So ,you do an Angiogram , find an Incidental intermediatroy lesion which may not be responsible for the ECG changes but you are compelled to go after it FFR//iFR , OCT, IVUS and so on !
*There is huge list of non Ischemic ST/T shifts in ECG that can be read elsewhere .
Counterpoint
Can’t agree with this article. Foolish to diagnose UA without chest pain. Never treat ECG in isolation unless its a convincing ST elevation or depression with clinical input and thorough scrutiny of past record . Realise , how important is the basics principles of medicine taught by Oslers and Cushings a century ago.