Coronary arterial spasm is a commonly discussed entity in clinical cardiology. Originally described by prinzmetal decades ago .It was reported to occur only in coronary care units as variant angina .There is nothing called stable spasm every episode of spasm is considered as unstable angina.
How common is coronary artery spasm ?
This condition thought to be very common during ACS , but notoriously difficult to confirm.In fact many of episodes are clinically suspected and never confirmed. There has been lot of provocative tests for confirming coronary spasm like ergonavine etc.None of these tests were neither useful nor practical.
What are the clinical situations where coronary spasm occur ?
Old concepts die hard.Most of us believe , the most common cause for coronary spasm is prinzmetal’s angina ie , angina in normal coronary arteries or with minimal lesions .Clinical experience , has taught us coronary spasm can occur in all spectrum of acute coronary syndrome or even chronic coronary syndromes.
Some believe every episode of STEMI will have a component of coronary spasm.
In NSTEMI/Unstable angina spontaneous coronary spasm is an important pathogenetic mechanism
Now, we witness transient coronary artery spasm in the cath lab due to catheter and other hard ware.The spasm here , is secondary to mechanical stress and this in no way related to the coronary spasm described by prinzmetal in the pre cath era.
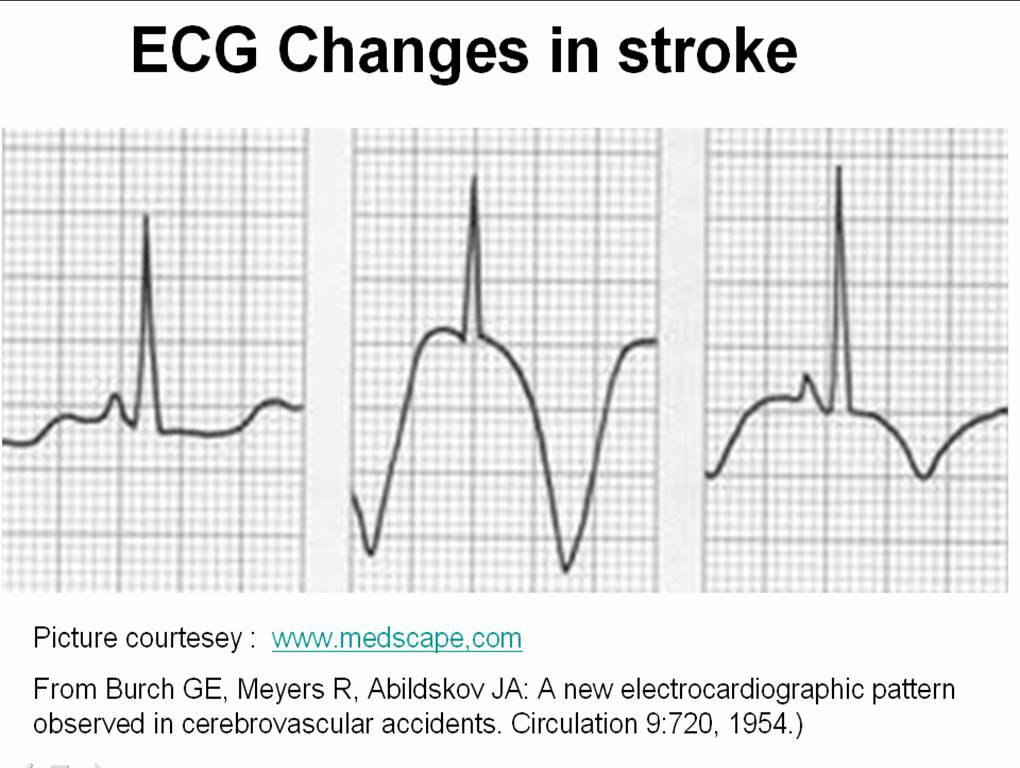
What is the link between coronary spasm and electrocardiogram ?
The most common fallacy among coronary care physician is , if it is spasm there must be ST elevation
The classical cardiology teaching all over the world , has been so powerful this myth continues to prevail over . The fact of the matter is , the coronary arterial spasm , can never have any direct impact on the ECG. (Unless , coronary smooth muscle generate ST currents !) . So , whatever be the effect of spasm it is through it’s effect on the myocardial blood flow.
Hence , it is not the coronary artery spasm that will dictate the movement of ST segment . It is the impact of myocardial blood flow to the layers of the myocadium namely , endocardium, epicardium , epicardium ( or a combination of the above ) that will dictate ST segment dynamics.
What are the the ECG features of coronary artery spasm ?
It can be
- ST depression
- ST elevation
- Only with T wave changes (Tall or Deep T invrsions)
- Flattish ST segment or rarely , entirely normal ECG indicating balanced ST forces
Among this , the most common manifestation of coronary spasm is thought to be , subendocardial ischemia and resultant ST depression .This classically occur in many cases of NSTEMI/UA .
This makes ST depression the dominant manifestation of spasm ,
How coronary spasm can elevate the ST segment ?
If it can induce a transmural ischemia it can elevate a ST segment . Does all episodes coronary spasm result in transmural ischemia ? No,not at all .in fact it happens very rare as we have already seen .
To result in transmural ischemia , the spasm should be total & sustained , at least for few minutes to completely occlude the blood flow .
Milder forms of spasm can elicit only a sub endocardial ischemia that depress the ST segment.
*There is a rare variety of spasm where subepicardium is more affected than endocardium and hence ST elevation may occur.
What is the effect of Nitroglycerine on coronary spasm ?
This is a very powerful coronary spasmolytic agent.We can witness it’s action more vividly in cath lab .
It brings back the ST segment to neutral position , from either a elevated or depressed state .Many believe , ( may it’s a fact ) much of the early benefit of angina relief in UA/NSTEMI is amelioration of coronary spasm
Is coronary spasm a neural event or a biochemical event ?
The exact answer is not known .It should be chemicals as neural signals are also mediated by chemicals.
What are the biochemical mediators of coronary spasm ?
- Smooth muscle calcium : Calcium flux is the immediate cause for spasm
- Mediators .Neural :Catecholamine ,
- Thrombus secretes Thromoxane A2 which is a powerful vasoconstrictor
Smooth muscle calcium
Is coronary vasoconstriction and coronary spasm are synonymous ?
Both terms are synonymous . Vasoconstriction is often used to refer constriction of microvasculature
while spasm often describes the event in large epicardial vessel. Some times the term coronary vasomotion is used to describe fluctuating coronary arterial tone.
What are the determinants of coronary artery spasm ?
- Location (RCA>LCA)
- Lesion characteristics -Eccentric overhanging lesion can trigger a spasm by the plaque ‘s weight.
- Thrombus content
- Acuteness of the event
- Adrenergic tone and nerve activity
- Concomitant betablockade . Theoretical risk ?
What are the types of coronary spasm ?
- Discrete ring or band like spasm
- Segmental
- Diffuse long segment spasm
- Multilevel spasm in same coronary artery
- Pan coronary spasm entire vessel (rare)
- Remote spasm away from catheter tip
Unanswered questions in coronary spasm
Can a totally normal coronary artery go for spasm all of a sudden ?
It is thought to be rare. Even in prinxmetal series some amount of atherosclerosis was documented in most patients.
What is the relationship between spasm and adjacent lesion ?
Spasm following PCI :Can spasm crush a stent ?
Can a coronary collaterals go for spasm ?
Logically Spasm can occur coronary collaterals .But it is difficult to document .coronary collaterals eventhough has three layes as that of artery (Intima, media, adventia) th medial smooth muscles are less sparse. Advential lack vasa nervorum and hence neural input is less.So spasm is a rare event in coronary collaterals
Read Full Post »