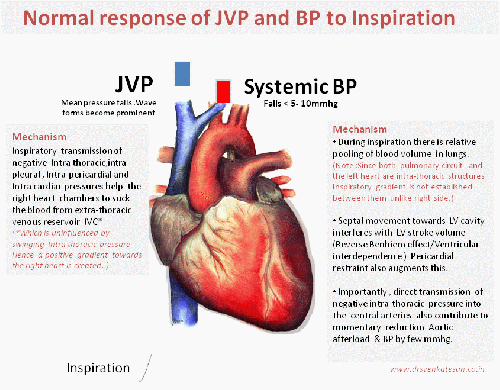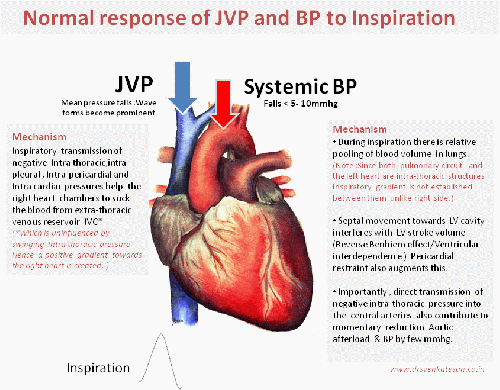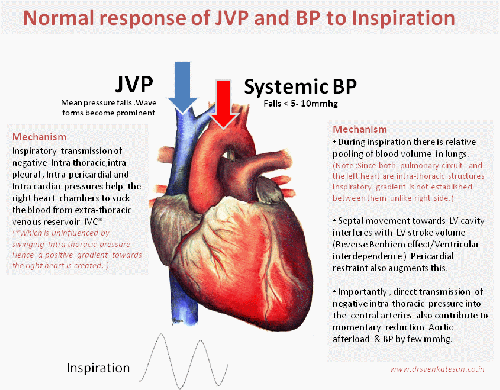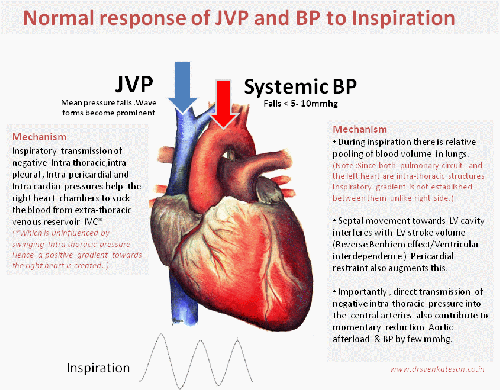
We can consider Jugular veins of the neck as a naturally present right heart catheter. It faithfully reflects the live pressure and waveform data from right atrium and ventricle .
Can JVP tell us anything about left heart pressures? Is there any relationship between JVP and PCWP or LVEDP ?
If you tell JVP reflects LV filling pressure in any graduate medical exams, you will be admonished. However in DM or post-doctoral exam, if you say there is no link between the two, you are likely to be chided.(It is unfortunate the answers vary depending upon the level of training , which I feel is not academically correct )
Though the JVP-PCWP link, apparently appears Illogical, it does have a scientific basis. It is true, there is a huge (& multiple) anatomical barriers between the left heart and Jugular vein in the form of pulmonary arterial & venous circuits, the right ventricle and right atrium.Still ,the hemodynamic principles demand, whenever left heart filling pressure increases, the right heart pressure should increase correspondingly to drive the blood from RV across the pulmonary circuit.This raise should be in the mean pressure. (or diastolic pressure,) it’s rarely related to systolic pressures as RV systole normally generate more than twice or thrice the LVEDP.
This driving pressure across the lungs is called the transpulmonary gradient. (PA mean minus LA mean) The normal being < 7mmHg. So if there is a sudden increase in LV filling pressure to 20mmhg, there has to be elevated right heart pressures.(20 +7) This will be reflected in JVP as well. So patients with acute diastolic heart failure as in HFpEF must show elevated JVP. This can be documented elegantly In patients with positive responses during diastolic stress testing. (JACC: Cardiovascular Imaging
There are important caveats in JVP-PCWP link
- If the PH is long-standing and precapillary (Reactive PAH) has set in the right heart pressure will no longer reflect the PCWP.
- If there is any organic Tricuspid valve disease (Both TR/TS) JVP can reflect PCWP.
- Finally, any cause of RV dysfunction will immediately elevate the JVP so biventricular dysfunction makes correlation of JVP with PCWP meaningless.(Acute pulmonary embolism, and RV infarction)
- Further confounding can occur if we contemplate RV diastolic dysfunction as seperate entity. (At what level of RV systolic dysfunction, does the RVEDP begin to raise ? I think we don’t have an answer for this . Researchers please note.)
Some more mechanisms of elevated JVP with left heart disease
- Bernheim’s effect and ventricular interdependence can make JVP elevated spuriously without elevating PCWP.
- Acute mitral regurgitation left atrial V waves can “tide-back” all the way to PA and the right heart to elevate the JVP
- In ASD and Lutembachers syndrome the RA pressure waveforms may reflect the LV filling pressure, though inconsistently.
- Finally, and importantly in Fontan circuit JVP may exactly reflect the left heart pressure for the obvious reason, as SVC is connected to the pulmonary artery directly.
Final message
JVP will always tell what is happening to the right heart chambers only . It can, no way be taken as a direct marker of PCWP/LVEDP. However, there can be a correlation between JVP and PCWP/LVEDP in a certain subset of cardiac failure. (As in exclusive isolated left heart failure (typically HFpEF) the elevated JVP might just reflect the elevated LEDP provided there is normal RV function )
Reference
1.This study elegantly shows a correlation (or lack of it) in different subsets of heart failure. It tells us very clearly If JVP(RAP) is not correlating or disproportionate to PCWP, it implies RV dysfunction.
2. This paper suggests a really useful scheme to classify heart failure as concordant and discordant with reference to right and left heart.
It throws some interesting facts. I guess it will help us guide diuretic management and prognosticate chronic heart failure.