There were days when acute pulmonary embolism(APE) was almost always diagnosed post-mortem. We are in the era , where we can recognise most of the pulmonary embolism without any difficulty.
Experience has taught us , when to suspect this dreaded syndrome . Any unexplained, dyspnea, hypoxia, tachycardia , syncope* with vague chest discomfort and a predisposing condition (DVT , post operative state ,etc) will make acute PE highly likely .
*Postural dyspnea and syncope is a classical finding in many.
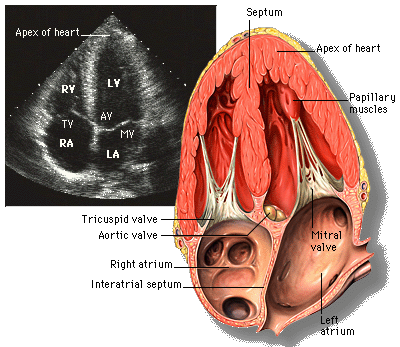
Pulmonary Echogram
We have advanced multi detector CT scans and MR angiogram , V/P scans and pulmonary angiograms to diagnose and confirm Acute PE .What we fail to realise is we also have a simple bed side tool called echocardiography to rapidly detect, assess the pulmonary anatomy and its hemodynamic status. In fact , we can visualize the entire MPA, and its bifurcation and to certain extent RPA,LPA. It is strange physicians always ask for pulmonary angiogram to diagnose APE , when we have a totally non invasive pulmonary echogram available at the bedside .It can rule out almost all cases of massive pulmonary embolism with a good festivity and specificity .

How often Echo miss a Acute PE ?
Echo may fail to image a thrombus if it is distal but it is very rare to miss a thrombus in MPA, and its bifurcation. Most of the patients with massive pulmonary embolism , are likely have a thrombus in the bifurcation.
Even if echo fails to image a thrombus , the effects of acute pulmonary arterial hypertension on the tender walled right ventricle is conspicuous. In fact, the effect of Acute PE on the RV morphology and function is the single most important feature to suspect APE . This is also considered as an indication for thrombolysis.
The following Echo features suggest Acute Massive Pulmonary embolism.Imaging these patients may be difficult especially if they are acutely dyspneic .Luckily , pulmonary artery short axis view can be obtained even in supine position in most of the patients.
- RV dilatation ( One popular criteria is End diastolic RV dimension > LV end diastolic dimension .It should be remembered , strict criterias can not be followed in this high risk medical emergency . Visual estimation of RV size is equally important.If in the para sternal long axis , RV is > 3cm it is significant . The only issue is, in patients with preexisting COPD RV size will not be useful to diagnose APE.
- RA dilatation (this is also a usual accompaniment )
- RV wall motion defect(Considered , as RV SOS calls !)
- Paradoxical septal motion
- D shaped septum is an absolute sign of distressed RV.
- Tricuspid regurgitation(This depends upon the leaflet length and orientation, some may not develop in spite severe PAH )
Less common features
- Pulmonary regurgitation
- RA , RA appendage , IVC , RV clots
Diagnosing RV hypertension
TR jet
MPA acceleration time (Not useful in an emergency situation )
Other thinks to look in Echo
- LV function (Hypoxic dysfunction or associated CAD )
- IVC for thrombus source .
- IAS anatomy : PFO may increase the chance for stroke as these patients carry the risk of further embolus. When the RVEDP, RA mean pressure raise to APE, the PFO becomes hemodynamcially patent and may develop propensity to shunt the incoming thrombus to left atrium rather than right ventricle as LA pressure is considerably less than RV
Unanswered questions
At what pressure RV begins to dilate ?
This is not clear.The response of RV , to pressure overload is not constant. In acute raise of RV pressure ,RV tend to dilate , while in chronic PAH RV hypertrophies and dilates .It is believed , the first signs of dilation begin , even with a 30mmhg of PA pressure . So , even minor dilatation could become important in acute PE.
Can RV dilatation alone , be taken as evidence for hemodynamic instability ?
Yes , but realise , clinical , hemodynamic instability is much more important than degree of RV dilatation (Hypotension /hypoxia )
The curious behavior of RV and TR jet in APE ?
Normal peak RV pressure is 25-30mmhg .In acute pulmonary hypertension RV pressure is supposed to raise . But it does not always happen.It all depends upon how the RV respond to the sudden raise in its afterload.
Some RVs fight vigorously and take on the challenge imposed by pulmonary embolus.These are the patients who show strong TR jets which may reach 60 mmhg. More often , the RV is stunned and overwhelmed by the unexpected sequence of events and lose the battle from the beginning .They become flabby and dilated.These patients do not show any significant TR jet , in spite of raising PA pressure. This implies, a good TR jet > 3.5 could virtually rule out severe RV dysfunction.
(One popular thought gaining ground is , the primary determinant of pulmonary artery systolic pressure in Acute PE is the RV contractile force , rather than pulmonary impedance .)
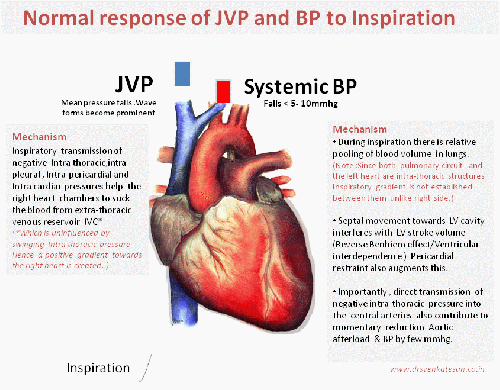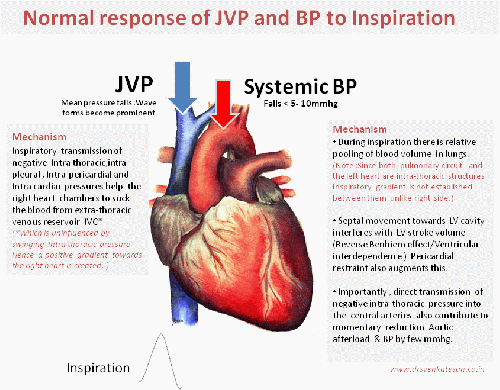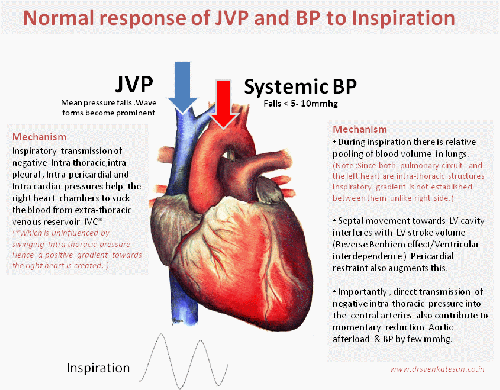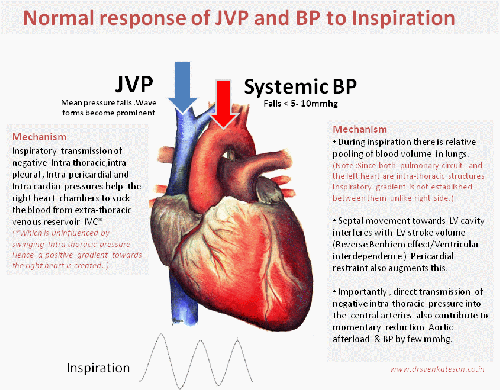
Hypotension is common in APE .What is the relationship between PAH and systemic blood pressure ?
- Inverse relationship is expected . This often result in syncope in these patients.
- Bernhiem effect
- Hypoxic LV dysfunction
Final message
RV faces the brunt of the hemodynamic attack of acute PE. .Differentiating simple RV involvement from RV dysfunction is a difficult and subjective exercise. But , it need to be done accurately as RV dysfunction becomes an indication for thrombolysis . RV dilatation , wall motion defect, mild PAH, all indicate RV dysfunction . Diagnosing RV dysfunction is better done by the treating physician who has the overall clinical data.
Read Full Post »