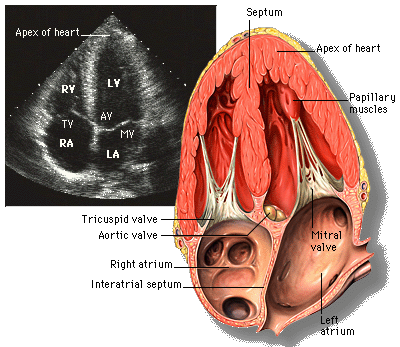
VSD is the leading cause of congential heart disease .
- The natural history is hugely variable spectrum , from totally asymptomatic , incidentally detected in childhood to a fulminant cardiac failure and death in early infancy .
- Many small VSDs get closed by year 10. None of the large VSDs close spontaneously.Few of the moderate sized VSD may get closed.
- The site of the VSD is a major determinant of spontaneous closure. Muscular VSDs are more likely to get closed .Of course many of the membranous VSD have at least a rim formed by a adjoining muscular septum
- Associated defects, RVOT obstruction and late onset AR also has a influence on the natural history.
- Progressive PHT leading onto Eisenmenger syndrome occurs has become a diagnostic curiosity in many countries .
It is natural to expect the VSDs to share a close relationship with the conduction system which fights for “equal rights” to occupy the inter ventricular septum , (In spite of a defective septum ! )
How often we see conduction defect in VSDs ?
It is rather surprising to note conduction defects are not common in VSDs .In fact it can be termed rare . How this is posssible ? VSDs , however large it maybe , usually spares the conduction system . This is simply due to the fact , developmentally the two systems , ventricular septum and the electrical system of the heart comes from different embryological focus and and are simply anchored together.
If the IVS is not formed properly ,the bundle of His and it ‘ s major right and left branches are simply displaced and not are destroyed , they tend to occupy one of the rims of VSD
*Further, a VSD located peripherally and distally towards the apex has little impact on the conduction tissue as it has already fanned out and small little twigs are affected ,while central , proximal, and basal VSDs can have more significance .
Classically , it has major significance for the surgeons than cardiologists , as post operative blocks are more common than the preoperative blocks !
What are the changes to the conduction system in various VSDs ?
Membranous VSD
- Migration of A-V node posteriorly toward crux of heart *
- His bundle courses along the posteroinferior rim of defect
* This makes sure the compact AV node never comes into picture of VSD . It also it explains the rairty of complete heart block due to mechanical damage to the AV node by the VSD jet

How to avoid injury during surgery ?
Sutures are made a few millimeters from postero-inferior rim, Do not penetrate the septum. Suture along RV side of the septum as the His bundle is often located on the LV side of muscular septum.
RV approach to close VSDs, make postoperative RBBB a common issue but generally it has no great clinical significance
Location of conduction defect in various VSDs
- Membranous VSD – Conduction tissue runs along posteroinferior border of defect
Muscular VSD
- (Especailly with Inlet extension) – conduction tissue is anterosuperior to defect
- AV canal defects . This is the only type of VSD where serious defects of conduction occur .Interruptions can also occur in the AV node.
Coming soon . . .
Where will the conduction system run in single ventricle where there is no IVS ?
Read Full Post »