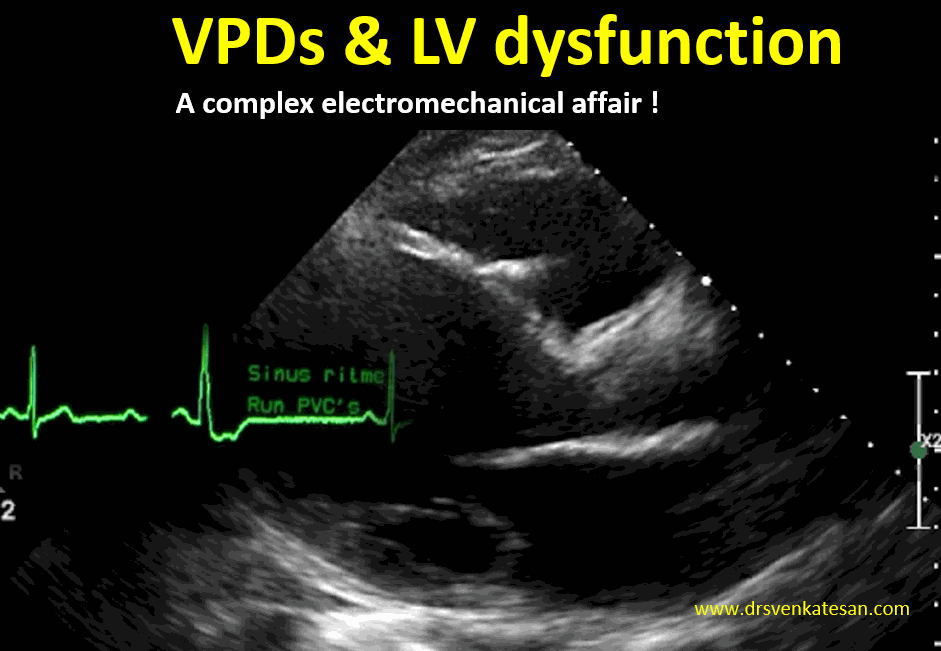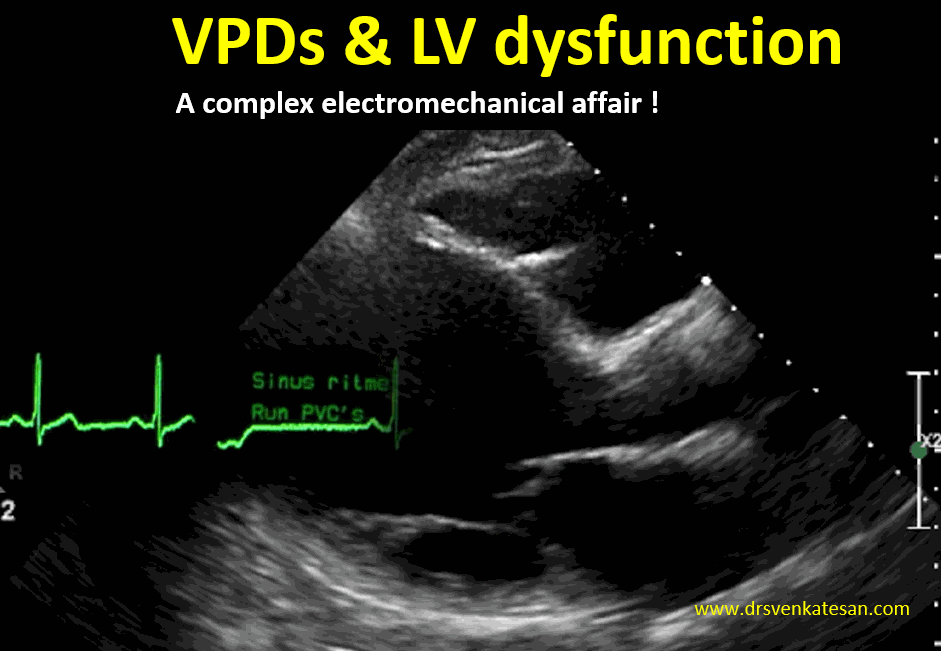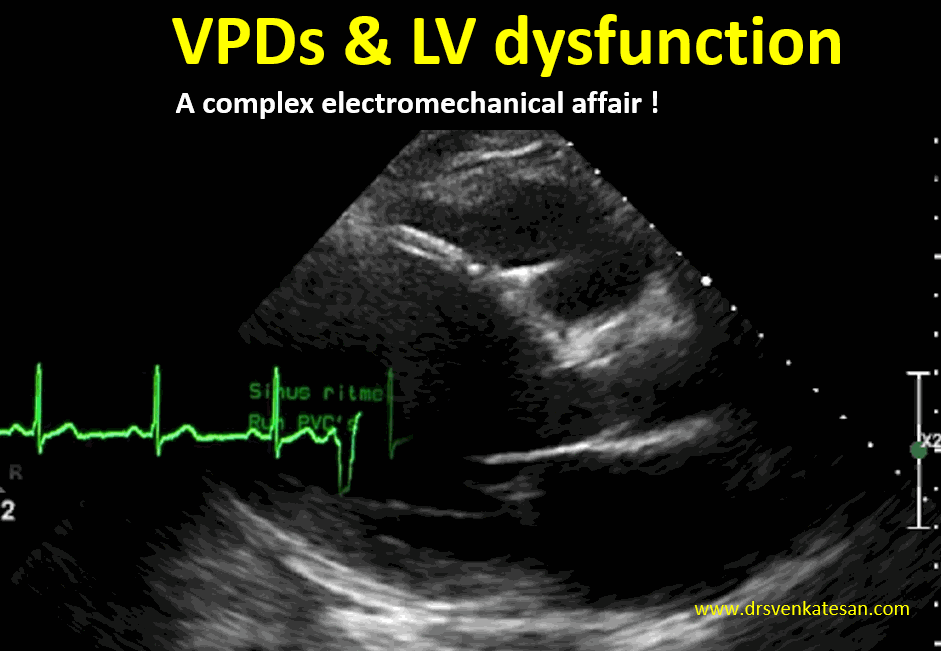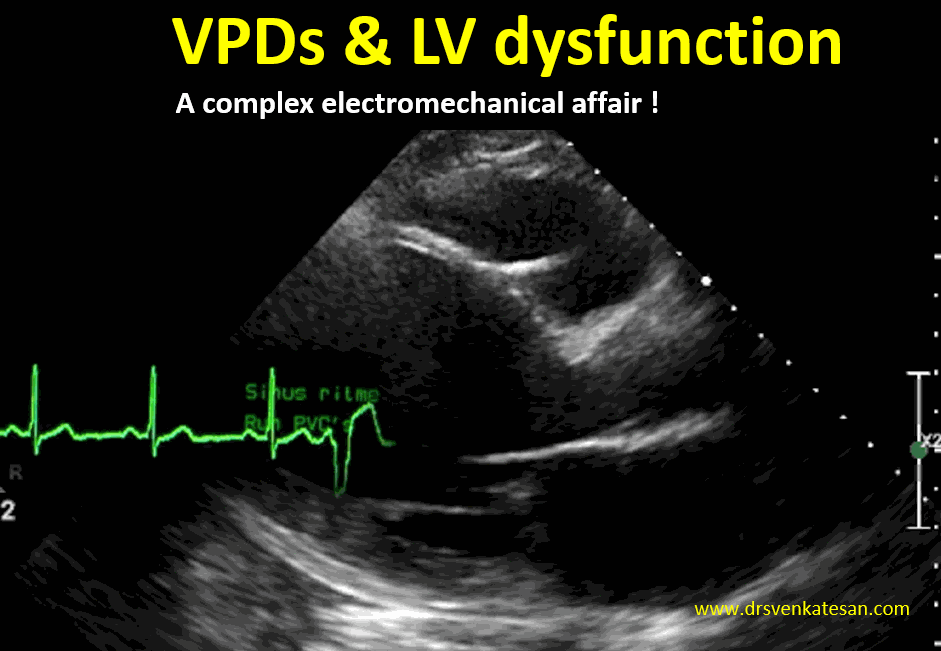
We know, LV dysfunction of any etiology can cause VPDs.This must be differentiated from VPD induced LV dysfunction. Mind you, this is not an easy job at all.
When do you suspect excess VPDs are the cause (or might cause) of LV dysfunction?
- In young, otherwise healthy persons with “VPDs and LV dysfunction” would suggest chronic abnormal electrical activity is the cause for subsequent LV dysfunction. (An expression of electromechanical remodeling)
- Monomorphic VPDs more often suggest primary electrical pathology(Like OTVT, Fascicular VT)
- VPD count more than >10000 in 24 hrs in Holter will probably Indicate an electrical defect that requires Intervention.
- VPD burden (>10% and usually >20%),
- Frequent NSVT,
- Retrograde P-wave after the PVCs,(Chronic AV desynchrony)
- Lastly one may argue its myth as well. VVI (& mode switched DDD) is a perfect example of how our heart tackles undesired VPDS. (We see hearts living comfortably with only with VPDs from the right ventricle (Pacemaker rhythm) without any troubling LVD.
Ref
1.Baman TS, Lange DC, Ilg KJ, et al. Relationship between burden of premature ventricular complexes and left ventricular function. Heart
Rhythm. 2010;7:865–9.
2.Ban JE, Park HC, Park JS, et al. Electrocardiographic and electrophysiological characteristics of premature ventricular complexes associated with left ventricular dysfunction in patients without structural heart disease. Europace. 2013;15:735–41
When do you suspect VPDs are because of LV dysfunction?
- History , clinical examination is the key. If there is a known cause for myocardial pathology.
- Here, the VPDs are more often multifocal (Rarely monomorphic)
- QRS complex other than VPDs may show slurring or fractured abnormality
- More severe forms of LV dysfunction
- Severely scarred ventricle obviously would Indicate primary structural disease that causes VPDs
Clinical implication
- If VPDs are the cause of LV dysfunction we may try to suppress or abolish it.
- No point in ablating otherwise asymptomatic VPDs in cardiomyopathy. Here we have to identify the cause for LV dysfunction(CAD, Myopathy etc)
- Beta-blockers can be useful in both subsets.
- The over-enthusiasm of ablating all forms of VPDs in any structurally abnormal heart is to be restricted. (Of course, Indication for RF ablation/ ICD may be appropriate in malignant forms )
- The beenifits of CRT therapy can be negated with frequent VPDs
- The relationship between the risk of SCD with the number of VPDs, is never found to be linear. (We have learnt in a hard way, that It is the degree of LV dysfunction that writes the script for SCD in a given patient)
What is the mechanism of VPD induced LV dysfunction?
VPDs alter the way ventricle contracts by inducing wall motion defect. In fact, it is intermittent cardiac desynchrony. Generally, LV tolerates this well. When the number exceeds a critical level LV size, shape and contractility is affected.
We need to differentiate chronic tachycardia mediated LV dysfunction (Tachycardic cardiomyopathy) with VPDs per se. This differentiation we can only guess.
* Some how cardiologists have not, implicated RV dysfunction induced VPDS. My guess is, it is equally important. Logically,at least 30% of VPD in end-stage DCM must be attributable( and arise from) RV dysfunction.
How to confirm is it a cause or bcoz ?
The only way is to prove LV function improves to normal or near-normal with ablation of VPDs .This can happen only with primary electrical disorders.
Final message
The link between VPDs and LV dysfunction is stuck in a complex two-way affair. Though a cause and effect component might be quantified to a certain extent, both can be coupled sequentially . “VPD promoting LVD” & “LVD begetting VPD” is always a possibility. This is the reason, we are tempted to take on any VPDs, which of course, is definitely not warranted.
Two resources
The HRS guidelines must-read for all fellows
This is a real state of the art lecture on VPDs straight from a world-renowned Dr Gacia Courtesy : Methodist, Houston