Archive for the ‘Uncategorized’ Category
Forbidden quotes in medicine : Healing shall prevail over harming
Posted in Uncategorized, tagged bmj, british journal of medical ethics, dr s venkatesan, ethics in medicine, famous quotes on medical ethics, Hippocratic oath, indian journal of medical ethics, lancet, madras medical college, medical education, modern medicine, nejm, venkatesan sangareddi, world health organisation on April 9, 2026|
Why different cut-offs for diagnosing STEMI in men and women ?
Posted in Uncategorized, tagged stemi gender difference in defintion on April 6, 2026|
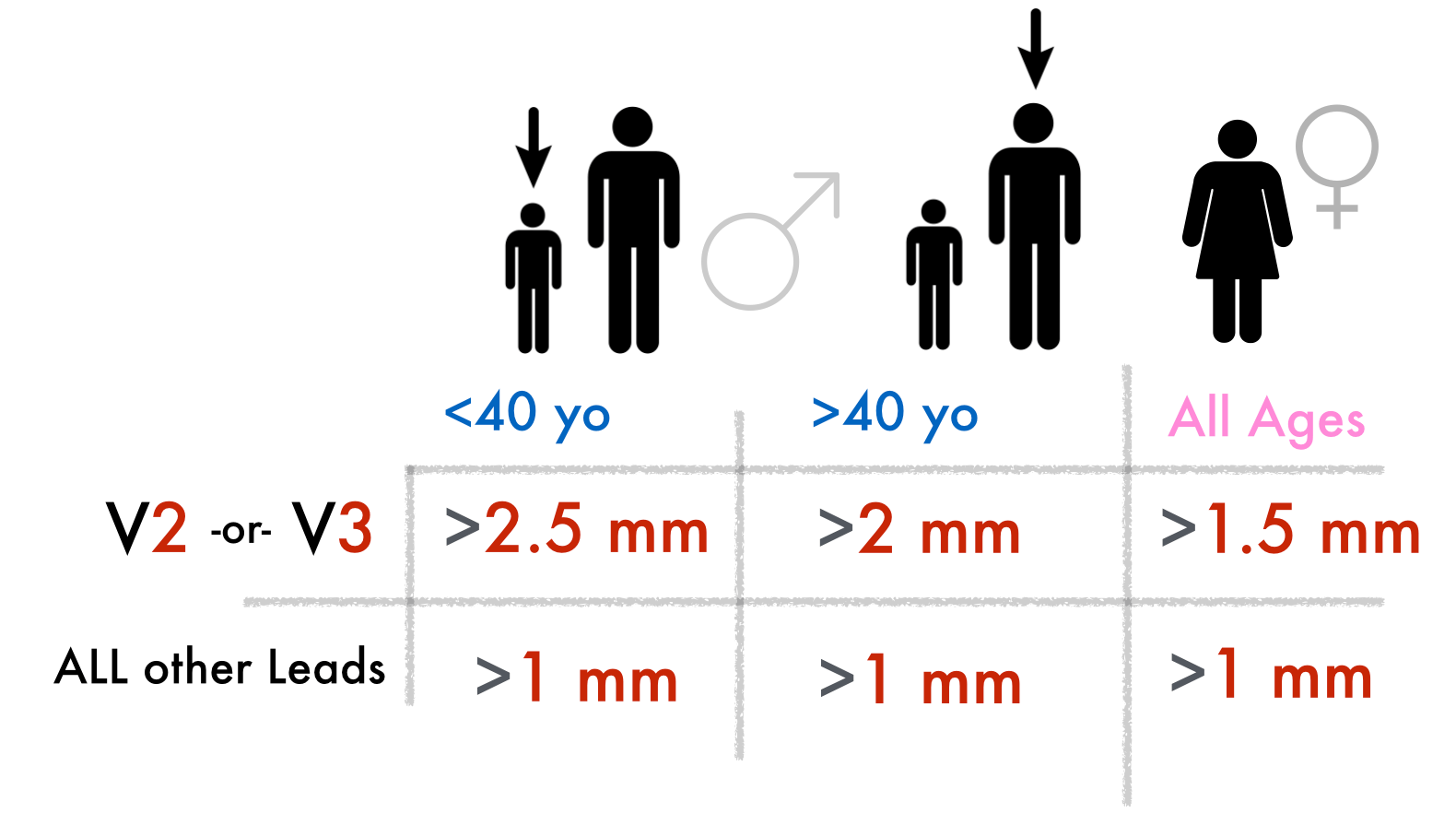
In healthy people, some J-point/ST elevation in V2–V3 is normal. This physiologic elevation is greater in men than in women Using the same cutoff for everyone would cause many false-positive STEMI calls in men (over-diagnosis) while missing true ischemia in women (under-diagnosis).
Molecular and Ionic basis
The difference is not because gender based difference in ischemia response . It is because ventricular repolarization differs between men and women due to sex hormones acting on cardiac ion channels. These differences appear at puberty and are belived to be driven by androgenic hormones.
Mechanism
Transient outward potassium current (Ito, carried by K+channels) is higher in male ventricular epicardium than in females. Testosterone up-regulates Ito density and function. In the action potential (AP) of epicardial myocytes higher Ito produces a deeper phase-1 notch This creates a larger transmural voltage gradient (epicardium vs. endocardium during phases 1–2 of the AP. This transaltes in the surface ECG as J-point elevation reflecting early-repolarization voltage gradients. Greater gradient steepr the J-point and higher ST takeoff .This is called the the classic “male-pattern early reppolarization.”Women have a shallow j point.
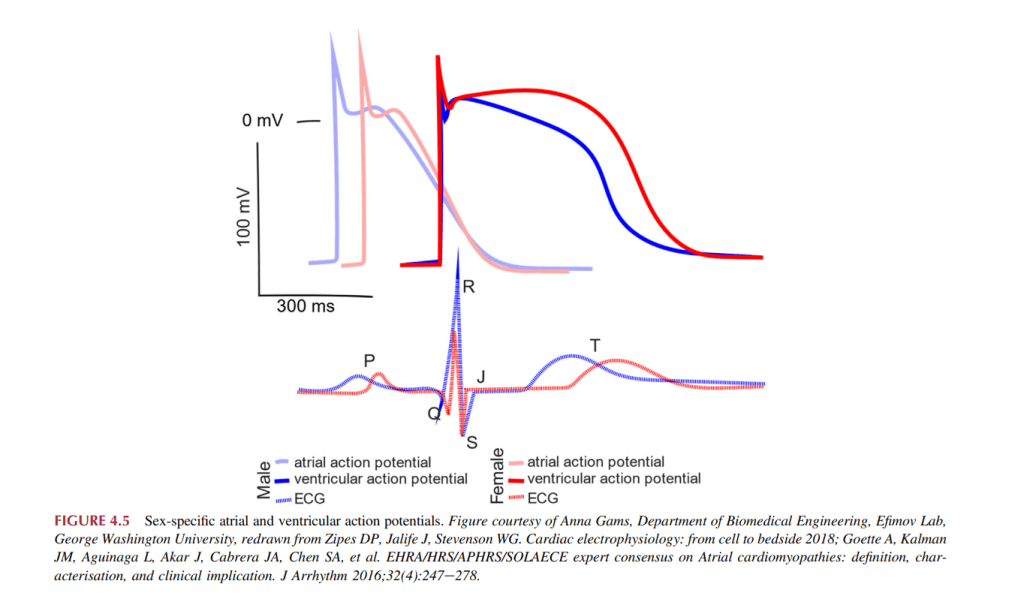
Image source : Blinova, Ksenia (2020). Sex and Cardiac Electrophysiology Atrial and ventricular tissue electrophysiology.
Why this difference is not seen in limb leads ?
Note : This J point difference is more prounuced in chest leads only because they are unipolar , and very close to epicardium and picks up the difference
Final message
Whenever we have trouble identifying the true mechanism in any gender-related difference, it is easy to blame it on either testosterone or estrogen. As in the atheletic filed , men are naturally a little faster to fly off from the start-boots in the early phase of repolarization. This also has some connection with why women have longer basal QT intervals than men. The whole repolarization process is slow but steady. We can alos realise, in spite of longer QT, women have less incidence of primary ventricular arrhythmias even during ACS, implying better reslience and stress handling. (Ref 2)
Reference
IVUS says good bye to complex PCI & left main : Cardiologists, are yet to blink !
Posted in Uncategorized, tagged ivus oct, ivus-chip study on April 6, 2026|
How many conferences, live workshops, where elite cardiologists, thought leaders (rather, academic influncers) , were projecting glittering power points about IVUS guided stent optimization, the sacred MLA’s , high precision POTS.They , sort of seduced us to believe , that these are going to rule the next generation PCIs .
In fact, some them warned us (with the company brand on the background) it’s a crime, to do any left main interventions without imaging.
Now, two back to back papers has come in NEJM* , exposing the futility of routine IVUS (after exhausting the market, and seeing no further scope for this deciet market ) . It simply unserscores the fact , that the good old luminogram is good enough for most PCIs including the complex ones *
Ironically , we should thank the same old companies, who for some reason , decided to stop this futility, by funding these studies.

Final message
The message from this study is , we should concentrate on the treatment of the whole burden of atherosclerosis. Let us not waste our resources to optimize the stent with exotic imaging , which can be done by conventional means.
Further, Cardiologists are obliged to apologize to their fellow physicians as well as the patient community for hyping up these unnecessary tools causing financial excess and promoting pseudo-science. They should also take an oath , they will not embrace the future technologies, prematurely and blindly.
Postamble
Waiting for OCT to go the same way as IVUS very soon. *By the way, I want to ask NEJM one question: Do you have any mechanism to identify these futilities earlier? Because you guys only publish and lift up the Iniital hypes.
Why Superior Scientists, will never rely on Non-Inferiority trials?
Posted in Uncategorized, tagged bmj, data torturing, fake science, fake stastistics, jama network, lancet, medical stastistics, nejm, non inferiority trials, stastistics, who is superior scientists, why rcts are riggged on April 4, 2026|
Statistics is the most advanced form of mathematics by which predictions about the future can be made with some degree of surety. It is a vital cog linking biology with maths. However, since the last few decades, an abnormal man made bio-mathematical mutation is being spotted in the field of medical statistics.
Why superior scientists avoid Non Inferiority (NI)trials?
They avoid relying NI -trials due to fundamental statistical, interpretive, and ethical weaknesses that undermine rigorous evidence and patient benefit.
Superiority trial models , reduce bias towards the null hypothesis and proactively protect against false claims. NI trials just do the opposite. The same issues dilute differences, biasing toward falsely concluding the new treatment is “not unacceptably worse” than the active control by a pre-specified margin . Without a placebo arm, sensitivity cannot be confirmed, and the assumption remains tentative.
Key vulnerabilities In NI trials include arbitrary, manipulable margins that may permit clinically meaningful inferiority. High success rates (>85–95%, especially industry-sponsored) suggesting bias, and risks ( Biocreep) where successive approvals erode standards. “Non-inferior” does not mean equivalent .It can mask statistically significant inferiority. Reporting often deviates from guidelines, with inconsistent margin justification and analyses (ITT vs. per-protocol).
Ethically, NI designs accept potential efficacy loss for unproven gains (convenience, cost, safety) without direct proof, exposing patients unjustifiably in high-stakes areas. They place disproportionate proof burdens on de-escalation or alternatives while entrenching suboptimal standards.
A Lancet Oncology piece highlights this as “the tyranny of non-inferiority trials”:. The authors propose abandoning superiority/NI distinctions for simple “comparative” trials.
Final message
Superior scientists prefer superiority or hybrid designs, or direct comparisons of net patient-centered outcomes .They never go for the NI shortcuts driven by regulatory or commercial pragmatism.
Reference
SMART- DECISION : When big science tries to disrupt our Intellect,what shall we do ?
Posted in Uncategorized, tagged abyss action trial, acc aha esc, beta blckers post mi, comet trial, drsvenkatesan, esc guidlines, euro pcr, GDMT, jama cardiology, jama network, lancet, nejm, non inferiority trial, omt, reboot trial, reduce ami, secondary prevention of cad by beta blockers, smart decision, tct md on April 1, 2026|
Caution: Harsh language & Unscientific truths
It is a pattern out there, rolled out periodically in cardiac- pharma literature . It happened for Digoxin. They have been trying to do this to beta blockers for quite some time. They successfully ditched beta blockers in systemic hypertension with synthesized evidence. Mind you, BBs are the only drug that received a Nobel Prize for its invention, and its role in post-MI protection is well established.
The script is well written. Trying to ring a death knell for cheap and established medical therapeutic norms, citing lack of evidence. It is done based on some non-sensical study designs called Non-Inferiority Trials. (Tannock I, Buyse M, De Backer M et al.The tyranny of non-inferiority trials The Lancet Oncology, 25, e520-e525 Now, powerful cartels want to get rid of BBs in post-MI ecosystem. REBOOT, REDUCE-AMI, ABYSS all were done with fixed ideas. Of course, ABYSS didn’t follow their agenda. Now, a the latest trial has come out with a magical name SMART – DECISION.

Read this paper https://www.nejm.org/doi/full/10.1056/NEJMoa2601005
One famous statistician said, non-inferiority study concept is foundationally flawed. Hence, it is generally not worth reviewing them, as most conclusions are deemed to be wrong and not scientifically consumable. Still, looking beyond the trial design, three important flaws are obvious in SMART-DECISION’ trial , which argues for beta-blocker discontinuation after MI.
The study population is highly selected (median 4.7 years 98% revascularized; median LVEF 59%). The study advocated discontinuation among long-term accrued beneficiaries of BBs rather than typical 6–36-month post-ACS patients. Physician-driven HF hospitalization amplifies open-label bias. A wide non-inferiority margin (HR upper CI <1.4) plus low events (132 total) leave it underpowered, unable to exclude modest 15–25% harm (7.2% vs 9.0%).
Final message
In science, we need to be right first … being polite is optional.
When big science tries to corrupt our minds, what should we do? Let us continue with our conscience and follow the instinct and work for the welfare of our patients. We know the healing power of BBs. Let us be cautious and alert. Never allow wayward science to intrude upon our minds to take STUPID DECISIONS and defame the OMT in CAD.
Postamble
A newchallenge to take on
Fact : There is no published RCT that proves diuretics improve mortality and survival in heart failure.
Action requested : Let all evidence-based cardiologists withhold injections of Furosemide or Torsemide when they encounter their next patient with acute heart failure and pulmonary edema.
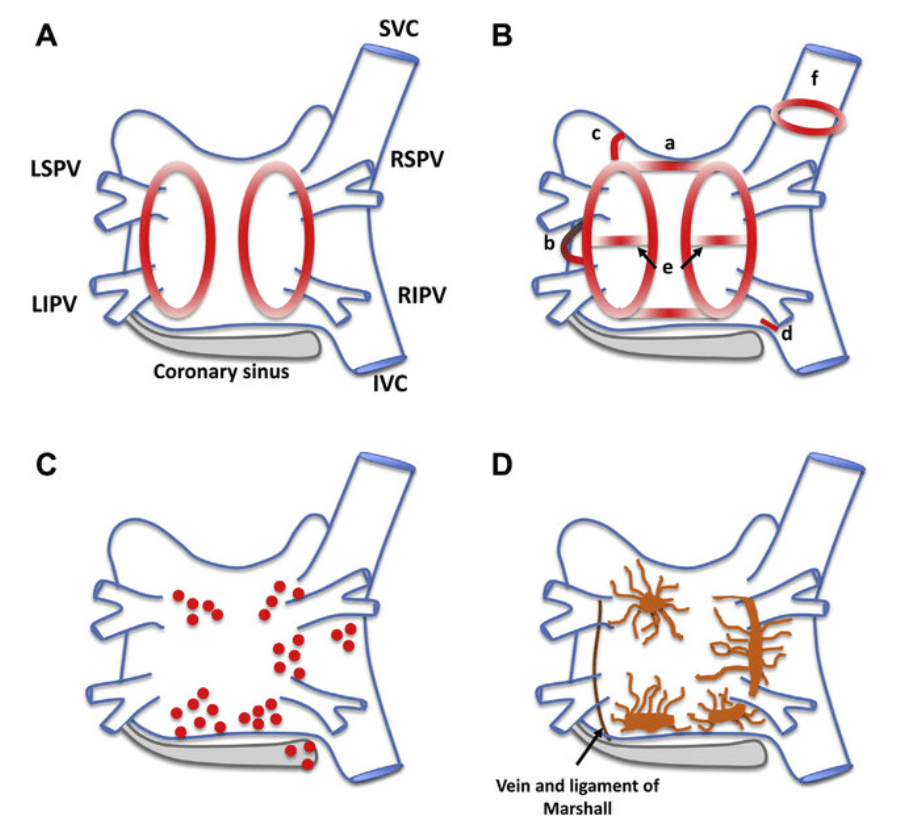
How often PV ablation converts AF to AT ?
Posted in Uncategorized, tagged atrial fibrillation, pulmonary vein ablation, pulse field abaltion pfa, rf vs cryo ablation on March 31, 2026|
PV isolation or ablation is considered as an ingenious modality in tackling chronic recurrent AF. Still, it is too invasive and complication-prone, with less than desired success rates. EPs are struggling to mitigate the adverse events. Hardware has vastly improved. We have since moved from RF , cryo , to pulse field ablations.
Whatever said, AF is a chaotic arrhythmia. When we try to take on the chaos head-on with more force, considerable damage, mostly invisible, is expected in the atrial battlefield. One such thing is post-ablation atrial tachycardia. The exact incidence is under-reported. Many times EPs don’t consider this as a complication at all. It is funny, some percieve it as a partial success as the chaos has become less intense. The fact of the matter is, an AT can be more unpredictable and carry electrical morbidity, whike the risk of further AF always remain.
Incidence of AT post AF ablation
Organized atrial tachycardias (ATs) occur in 5–40% of patients after catheter ablation for atrial fibrillation (AF), with the exact rate depending on the index procedure strategy, AF duration, LA size, and follow-up duration.
- With pulmonary vein isolation (PVI) alone: Incidence is lower (5% or less). When AT occurs, it is frequently focal, most often originating from reconnected PVs
- With additional substrate modification (linear lesions, complex fractionated atrial electrogram ablation, etc., common in persistent AF): Incidence rises to a prohibitive 20–50%.
- Macro-reentrant ATs also occurs due to gap-related peri-mitral or roof-dependent circuits.
Final metssage
Both focal and non focal ATs are much common after PV ablation, than we realise.Very often, they require another procedure or more intensive drugs . Realistically, the original purpose of treating the chronic AF is lost , if AF is likely to be transfomed to some other form of AT.There is nothing called 50% chaos reduction in AF treatment.
What is the purpose of “24-hour” upper limit cut off in the pharmaco invasive strategy ?
Posted in Uncategorized, tagged acc, dr s venkatesan, esc, extended pharmaco invasive strategy, fast mi trial, madras medical college, pharmaco Invasive strategy, primarypci, stemi, stemi nstemi guidelines, stream trial, why 3 to 24 hour time window in pharmaco invasive strategy on March 30, 2026|
Why 3-24h ?
The famous & popular 3-24 hr time window for pharmaco-invasive strategy (PIPCI) was adopted, blindly from STREAM (prehospital Tenecteplase + PCI <6-24h in <3h presenters) and FAST-MI trials assuming uniform IRA patency. It fails to stress the importance Initial time window to lysis, and its response . This makes the distinction between true rescue vs routine pharmaco invasive PCI a hazy excercise . Thus, both inappropriately delayed or a hastily-routine PCI has become all too common.
The 24-hour upper cutoff in pharmacoinvasive strategy serves to prevent reocclusion, or to address any residual mechanical stenosis . It is not meant for myocardial salvage, which is irrelevant if lysis was successful.
Mind you, IRA optimisation is not a time bound emergency in a well recannalised vesseel. In fact, PCI is not an absolute neccesity for long term IRA patency especially if it an coronary erosion. If there is TIMI 3 flow ,and there is little ischemic substrate , there is no need to chase the , supposedly sacred 24 hr time window. If the lysis achieves complete( or almost complete) IRA patency, PCI can safely be extended to 48-72 hours, or even permanent deferral (No-PCI , stand alone thrombolysis) in stable patients with optimal medical therapy.
An interesting study is published , from my institute in the current issue of AJC with a title ” Extended Pharmacoinvasive PCI Compared to Primary PCI: Insights From Madras Medical College STEMI Registry” . This study argues for extending the time window for pharmacoinvasive strategy to 48 hrs. (It could still be higher.) It suggests , this flexibility suits the LMIC, due to logistical realities. ( Glad to be listed as a co-athour)

Link to the PDF of the article
I am sure, this study, demands to reset the 24 hr upper limit of cut off for pharmaco invasive strategy.Looking beyond this study, there is an urgent need to clarify the specifc purpose of the generalised time window of “3 to 24” hr time window in pharmaco invasive strategy.
A call for new sub defintions in the time windows in PIPCI
1.Successful Lysis* (TIMI 2-3, in about 70%): Routine angiography/PCI 3-24h (prevent reocclusion/residual stenosis) .Extendable to 48-72h + is possibel. Permanent deferral if the pateint and myocardiumare , with a patent IRA . (Implying no need for further salvage at all , we should allow a green corridor for patients with successful standalone thromolysis to exit the hospital without a PCI ) Doing a PCI onlu t0 prevent fear of reocclusion in the first 30 days is not backed with good data.
2.Failed Lysis* (TIMI 0-1, 30%): Rescue PCI immediately (<3-6h post-lysi, like PPCI) Here the time window should be hastened and can never afford to extend it, at any stretch of imagination.
* Ironically, the 24hr cut of has no place in both the above subsets. (May be in failed lysis , 24 hr cut off might apply , again it is 12 hr longer than primary PCI )
Final message
“Time is no longer muscle , if the Intial lysis is successful“
What is the purpose of “24-hour” upper limit cut of time in pharmaco invasive strategy ? The 24 hr is not universally valid. Pharmaco Invasive strategy time windows need to be based on timing and efficacy of the Initial lysis.
Postamble
Commenting this paper as a third person :
One limitation in this study is to be admitted. I think, the generalised comparative efficacy of extended PIPCI with primary PCI can not be made, for the simple reason, the extension of time window is possible only in patients who had successful lysis. This study may ideally be concluded as “3-24h pharmacoinvasive PCI can be extended to 48h if the initial lysis successful” . Further, If initial lysis fails (30% TIMI 0-1), any extension is contraindicated and requires immediate rescue PCI akin to PPCI. Also, data regarding non-IRA intervention might help understand the importance of the extension of the time window better.
How GDMT, succumbs to the faulty coronary revacularisation credit equation ?
Posted in Uncategorized on March 26, 2026|
Ischemic Coronary artery disease is probably the most common medical ailment in humans.
It is managed by four strategies by modern day cardiologists.
A.Only life style modification.
B.Intensive medical management (Also called as GDMT or OMT)
C.PCI
D CABG
Which one of the above modality is considered superior (& popular) among physicians and patients ?
No doubt, PCI is the undisputed winner for all the wrong reasons.
PCI success lies literally at the mercy GDMT. CABG has the same story to tell. While, only GDMT, has the vigor to stand alone in style and triumph in most CAD patients. It needs no great wisdom, to acknowledge, GDMT never gets its due respect. The problem is ,we are all part of those guilty cardiology professionals, who silently watch the PCI, shine in false glory.
How often we can treat CAD , effectively without doing a coronary angiogram ?
Posted in Uncategorized on March 23, 2026|
A. Very Often. We don’t really require the anatomical Information. A well performed stress test will tell us the presence and significance of obstructive lesions .
B .Majority of CAD patients will require CAG , as we can’t rely on other non invasive tests.
C.Atleast all ACS need CAG, but many CCS don’t need it.
D . Forget about it .It is unethical or rather blasphemy to treat CAD without knowing coronary anatomy.
Pathways to an answer.
Even acute STEMI can be managed without initial ( or even permanent) knowledge of coronary angiogram in atleast 70% of pateints.
* It is sad truth, the modality of standalone thrombolysis has been brutally stigmatised and being portrayed as incomplete and Inferior form of treatment in STEMI. It is pity , such a perception is deep rooted in many cardiologsist’s mind inspite of the fact great studies exists to prove treating STEMI without knowing the anatomy( ie prehospital lysis) could beat PCI consistently )
**How often we need CAG in Chornic CAD? You know the answer . If moderen day cardiac Intervetions insist us take a decision based on Physiology, then why do we want to know anatomy?
A stress test, technically is , equivalent to simultaneous multivessel FFR or iFFR . If some one crosses 10 METs in a stress test , whatever the lesion subset, it can be considered net-equivalent for a normal FFR of near unity. (No one has tested this hypothesis, so as of now it is junk science.) Still every experienced cardiologsist would acknowledge the truth in this.
Can you find the type of pacemaker in this ECG ?
Posted in Uncategorized, tagged aai va ddd in aai mode, atrial paced pacemaker, ddd vs vvi, lbbb area pacing, lbbbp, lbbbp vs aai, mode switching, pacemaker choice in sinus node dysfunction, single lead physiological pacemaker, vdd pacing on March 16, 2026|
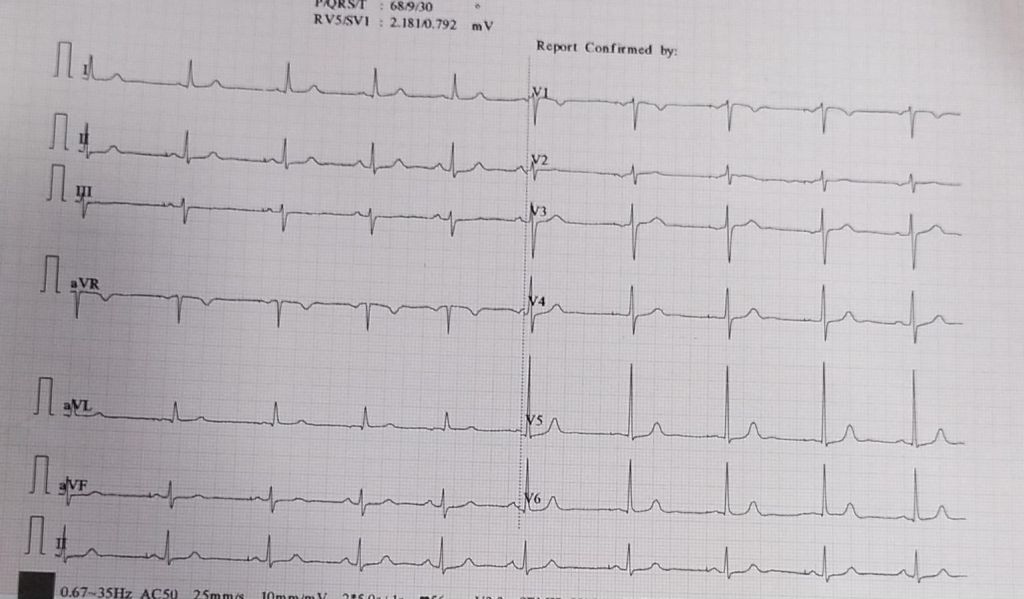
This pateint has
A. Single lead AAI pacemaker
B. DDD in AAI mode* (A pace V sense )
C.Single lead AAIR pacemaker
D. Can never answer this question without X ray or the implantation records.
Answer : I think, we can’t answer this question with this ECG strip. So we can only guess it is DDD, as single chamber AAI pacemaker is not in vogue , even though it is the most physiological pacemaker possible in ideal conditions.( If any one has any points to differentiate , please comment)
* A pace V sense in DDD, though equivalent to AAI mode , can not be compared to AAI pacemaker, for the simple reason, ventricles just don’t have a lead in the later.
Final message
This post might appear as a EP parody. The purpose was different. It is sad to note AAI pacemaker might be dead , but the AAI as a mode will always be a great concept.It can beat on any day , the much hyped LBBBp in bulk of the pateints with SND in terms of physiology and synchrony.Fellows should realise single lead AAI can be most physiological , while, the DDD can become a pathological pacing , if it frequently switches to VVI mode , inspite of good AV conduction.
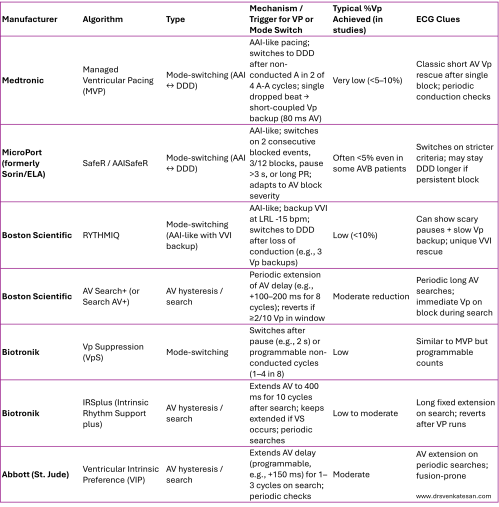
Part 2 : How do modern day DDD pacemakers reduce ventricle based pacing ?
Pacemaker vendors have unique proprietary algorithms designed to minimize unnecessary right ventricular pacing (%Vp) while maintaining atrial-based pacing (effectively mimicking AAI/R behavior) in patients with intact or intermittently preserved AV conduction (e.g., sinus node dysfunction without significant AV block). These algorithms promote intrinsic ventricular activation to avoid dyssynchrony, reduce atrial fibrillation risk, and potentially improve long-term outcomes.
There are two main categories:
- Mode-switching algorithms (AAI(R) ↔ DDD(R)): Operate primarily in atrial-based mode (AAI-like) with ventricular backup; switch to full DDD when AV block criteria are met.
- AV hysteresis / search algorithms: Stay in DDD(R) but dynamically extend the AV delay to search for and favor intrinsic conduction.
Annexure : Company brands and different modes and algorithms (Compiled by Grok)