Mitra clip is a small metal device that is delivered percutaneously, to clip the incompletely coapting (closing) mitral valve. It was first introduced to treat degenerative mitral regurgitation. It is an interventional imitation of the famous edge to edge Alfieri stitch repair.This procedure in fact converts the single mitral valve orifice into two. In the process, curtails the regurgitation jet orifice significantly. Though the technique looks nice and simple to hear, lots of per and post-procedure issues need refinement. Conceptually it is ideal in primary disorders of the mitral valve. (Read EVEREST 2 criteria for optimal patient selection) There have been more than 60000 Mitra clips implanted worldwide wide. Thanks to Abbot.
In secondary MR (due to LV dysfunction) Mitra clip has shown mixed results( MITRA-FR not much benefit, COAPT -Did show benefits)
Now, what about Mitra clip as a remedy for rheumatic mitral regurgitation?
This is the question everyone likes to ask. Now we have some interesting breakthroughs. Dr. Ningyan Wong from the National University of Singapore reports probably the first case (Ref 1) . The videos are reproduced with the creative commons license.
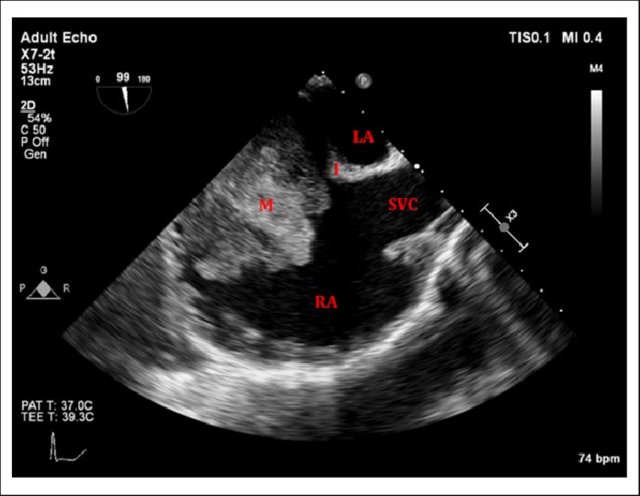
Note the classical thickened AML in rheumatic mitral regurgitation.
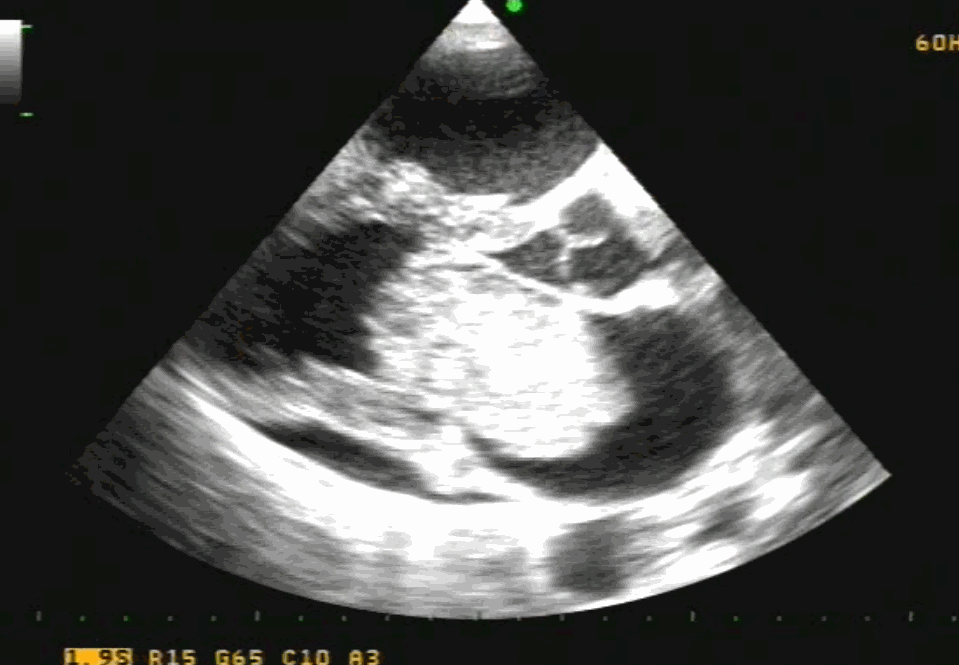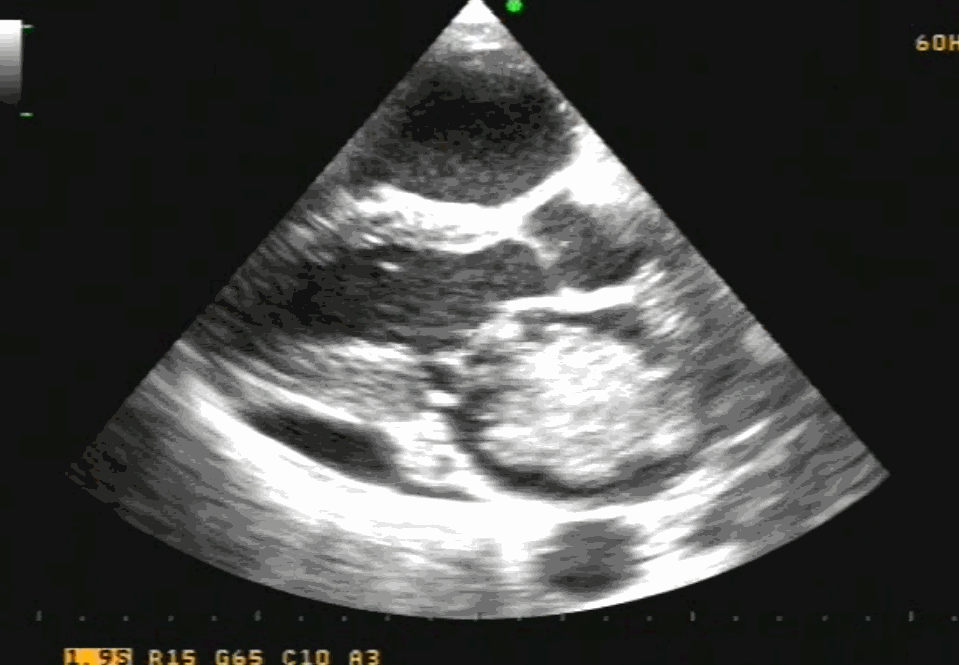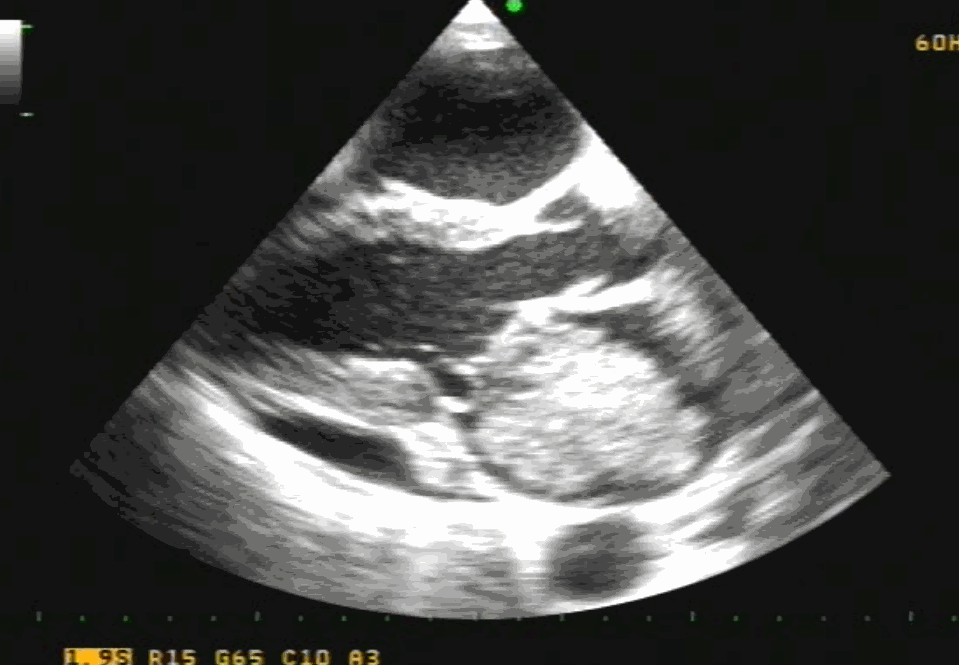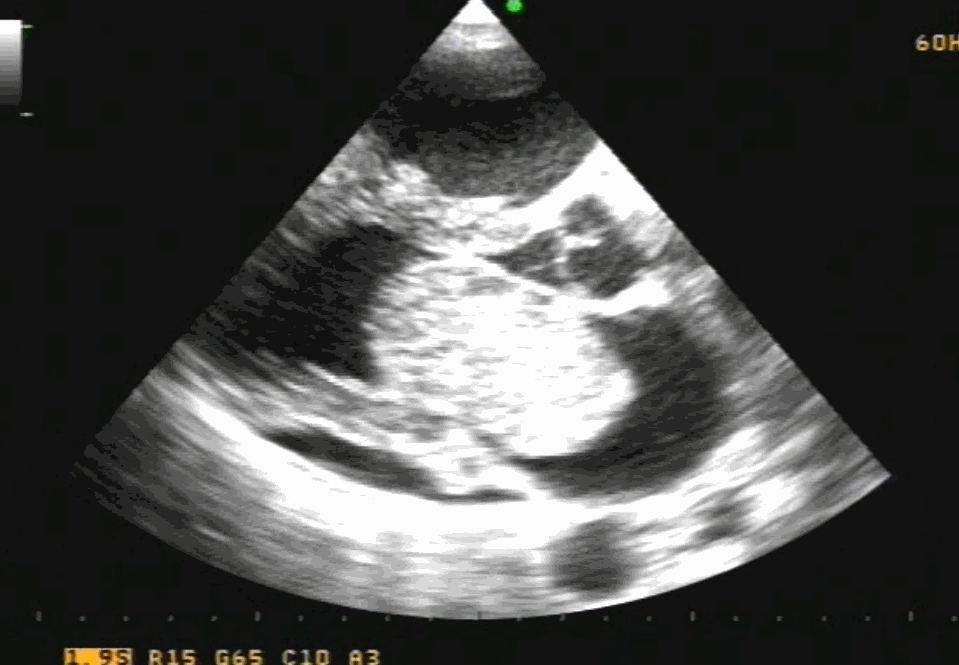
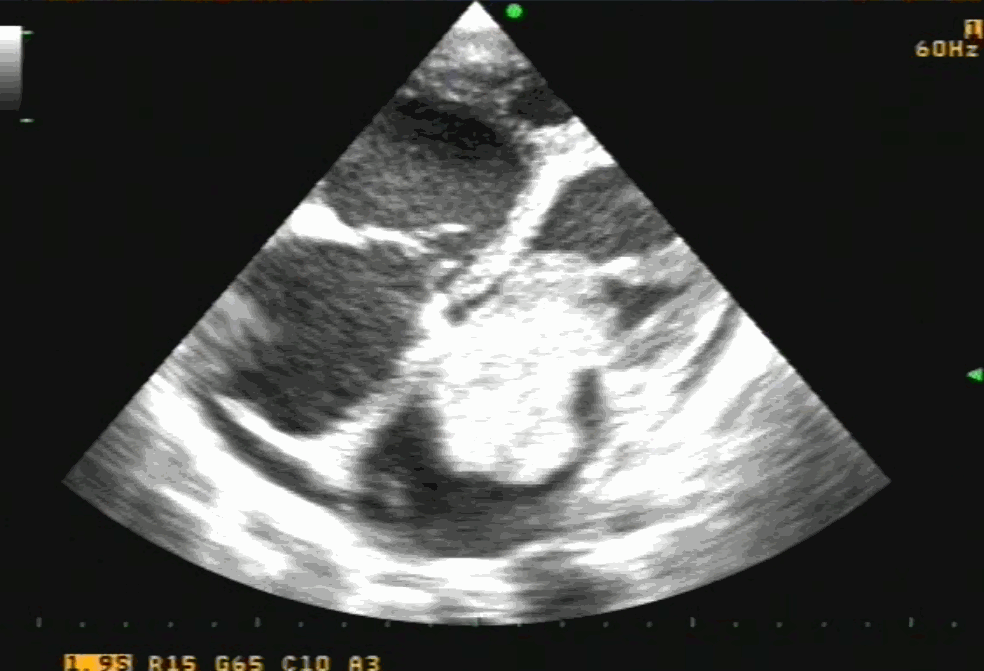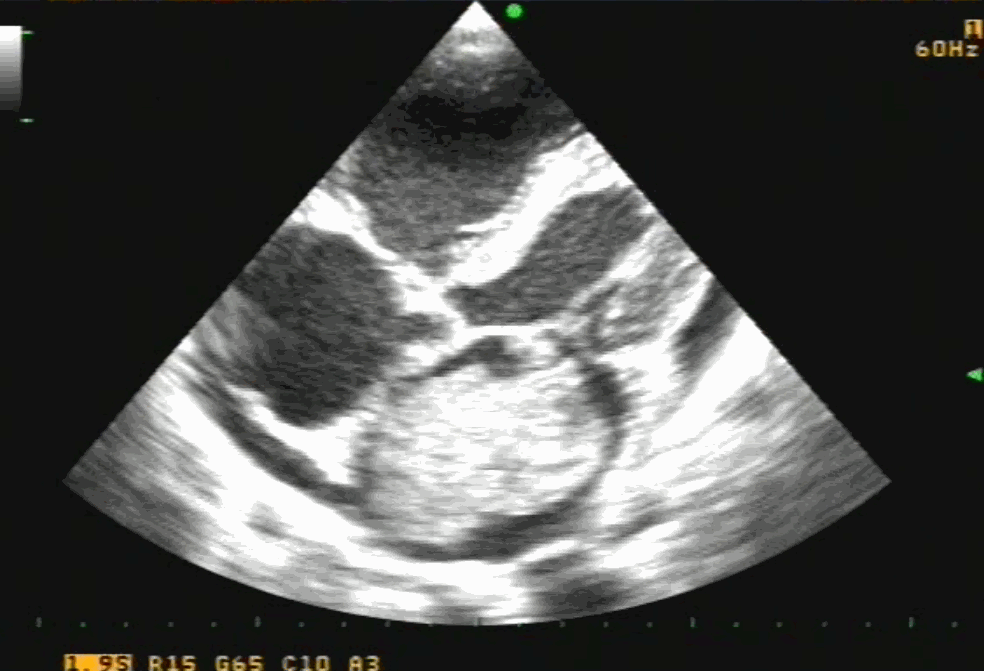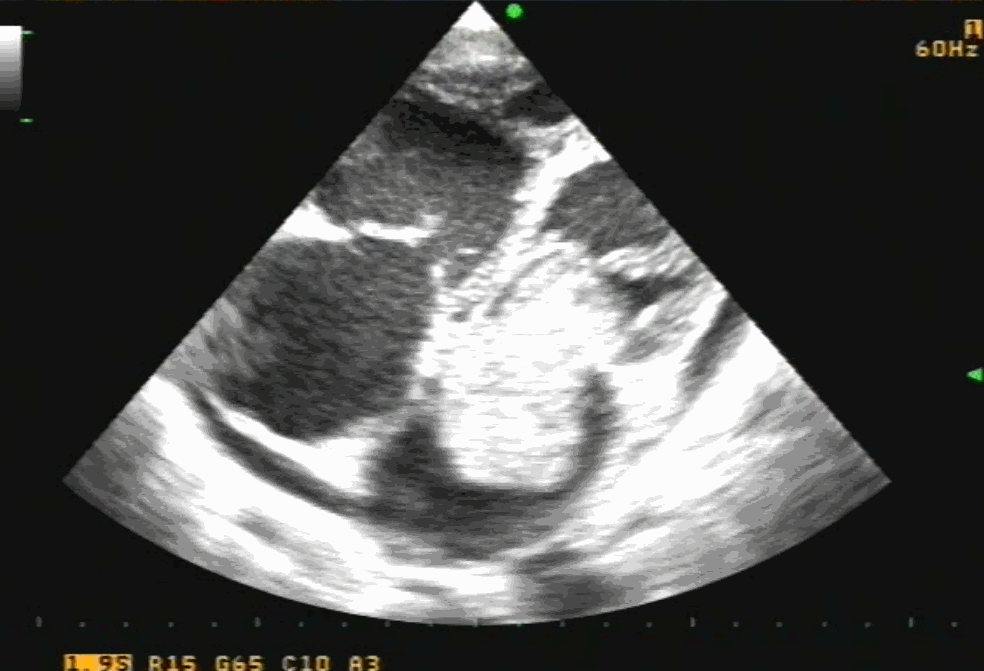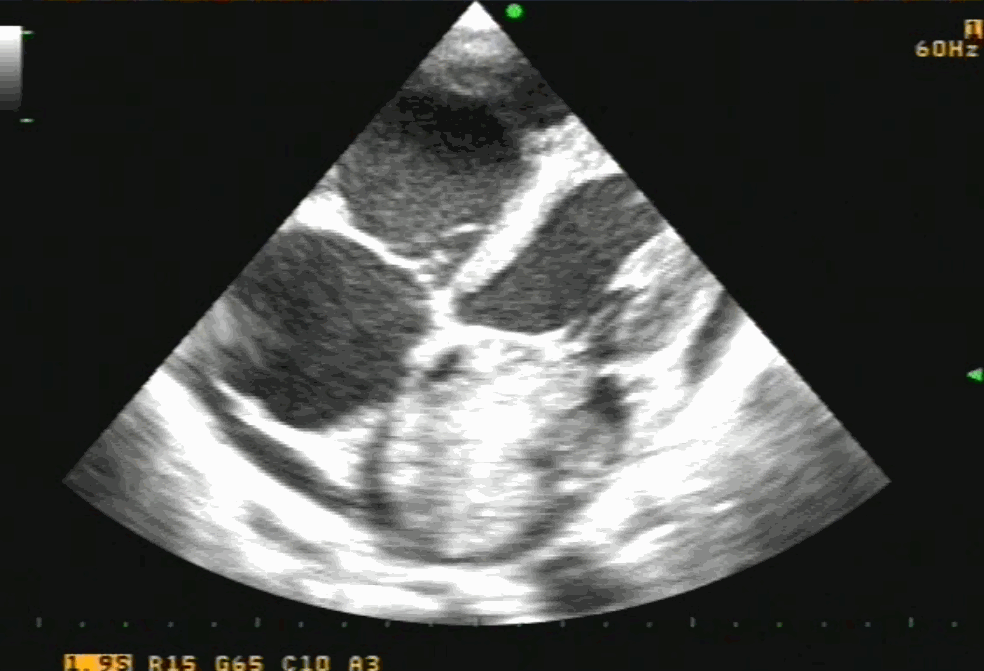
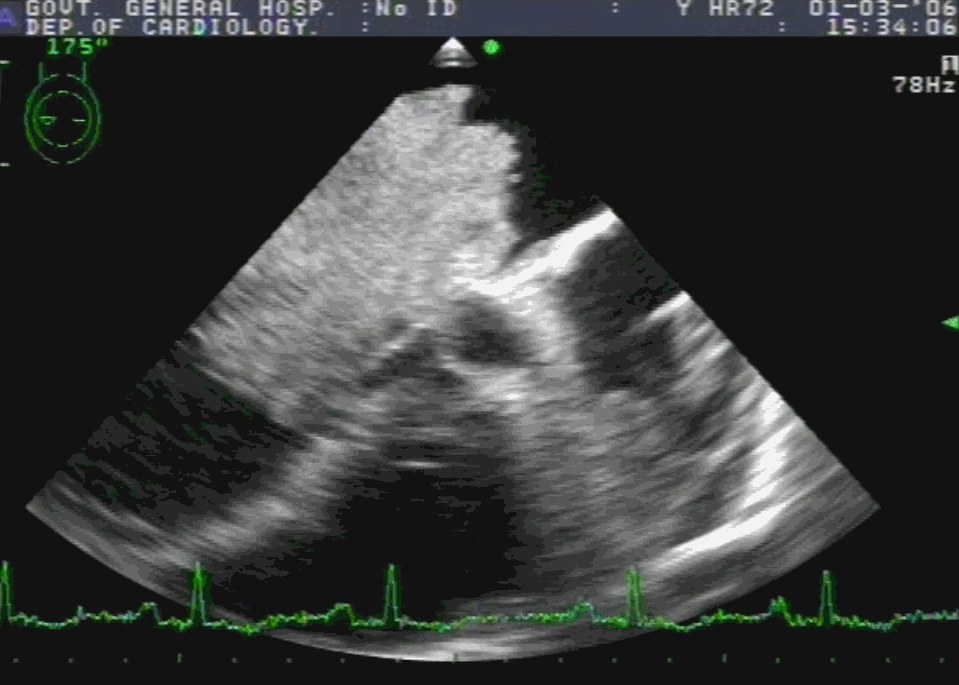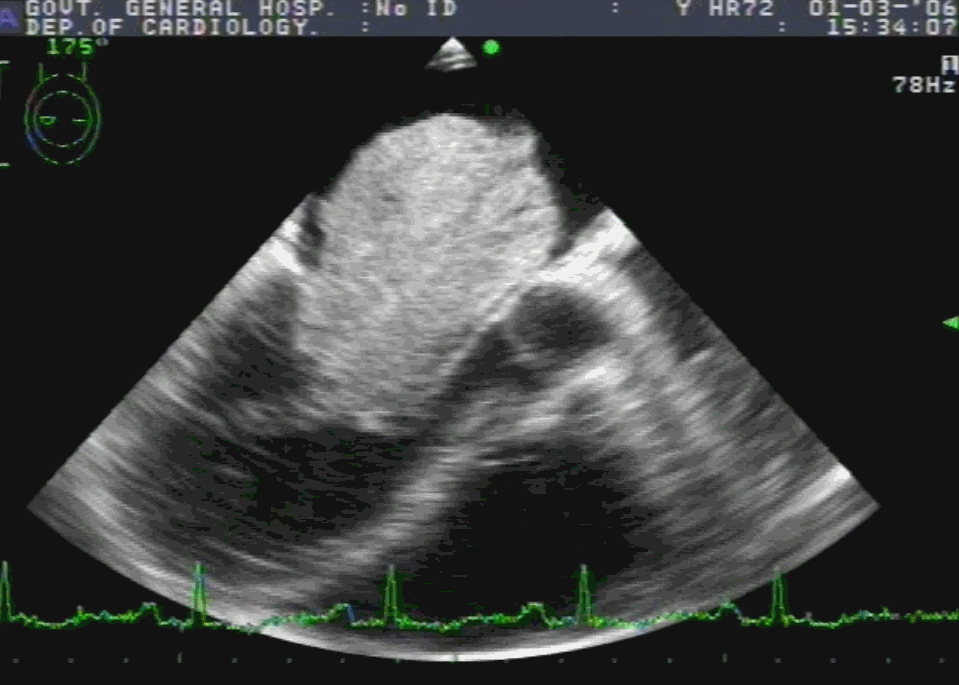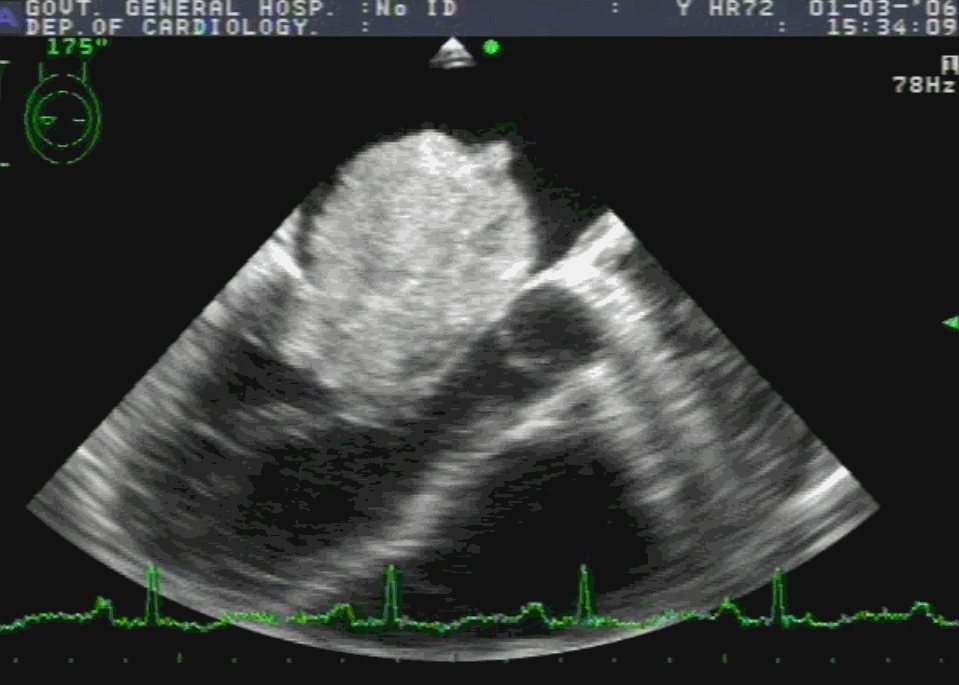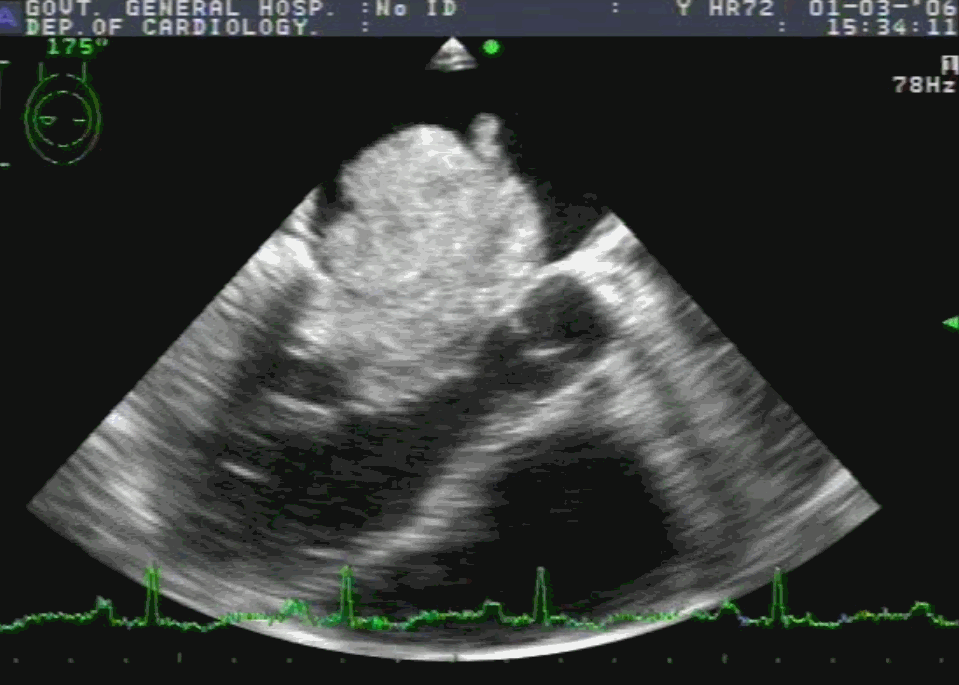
TEE showing severe MR
Post Mitra clip : A real surprise to note near-total abolition of regurgitation. (This really is good news for the rheumatic mitral valves )
Technical issues
- Should be isolated MR
- P2/A2 scallop clipping is the key to success.
- The thickness of the leaflet limits the success (Grasping the leaflet will be difficult)
- Clip Induced mitral stenosis is a distinct risk.
Potential role and future
RHD forms 90 % of valvular heart disease in a country like India. The incidence of Isolated MR in both acute rheumatic fever and chronic RHD are substantial. If only we refine the hardware and technique to suit these thickened rheumatic valves, Mitra clip is expected to make an impact in this unique group of patients where surgery can be avoided or at least postponed.
Though we would very much like to do such a trial in our place, logistics has effectively precluded it. I wish some large centers like AIIMS New Delhi or PGIMER Chandigarh and others can take this concept to the next level.
Reference