It is just past midnight: This is a gloomy conversation between a patient’s son and a cardiologist in the silent waiting room, just outside the dim-lit ICU of a popular 4-star hospital in Chennai.
“I am sorry to say, Mr. B., your father didn’t make it. Has succumbed to the heart attack. We have been trying to resuscitate him for the past one hour. We have done everything. We have managed to open up IRA, and 2 more critical blocks still it couldn’t help. It was a massive one. Sorry again.
“Doctor, I feel very bad. What went wrong, I want to know. Doc, did you try ECMO ?,” the elder son queried
“No, we didn’t”
Do you have it in your hospital doctor?
“No,we don’t have it”
The son in distress couldn’t take it lightly. “How can you say that doctor? such a big hospital doesn’t have ECMO, “What a mistake we have done, we should have gone elsewhere” he quipped
The visibly exhausted cardiologist was taken aback and struggled to retain his composure. He took some time and tried to explain the bereaved family with a semi-scientific explanation.

“Please understand the reality. Do you know, how likely an emergency ECMO will resuscitate a patient with cardiogenic shock and arrest”
- ECMO is not a magic machine that will bring back your heart to life
- It is a temporary circulatory support device ideally used prophylactically in high-risk situations
- It takes a minimum of 20 to 30 mts (If it’s in ready mode) to insert the AV ECMO , Further, there must be some cardiac activity till the ECMO takes over.
- It is almost impossible to resuscitate with ECMO after cardiac arrest and circulatory standstill.
- In fact, prolonged CPR with an absent pulse is a contraindication for ECMO.
-
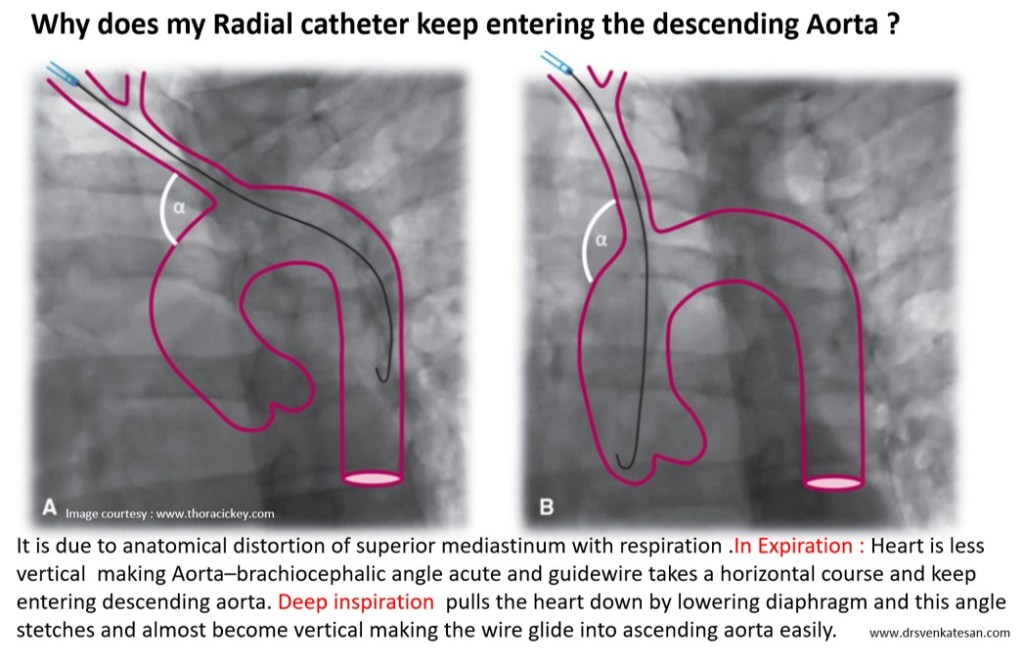
“Let me go little deeper into the hemodynamics of ECMO, even if it is inserted on time, ECMO doesn’t support coronary circulation much, (the one that matters most in the failing heart) ECMO circuit that brings oxygenated blood from below upwards in descending aorta. This stream may not reach the aortic root as it has to competes with ventricular contractions however feeble it may be” (Ref 1)
“Don’t mistake me, In my opinion, all these macines like ECMO Is more like a fancy customary add on machine in a high profile patients”.
“So, you are saying, my dad is destined to die, that’s not at all fair doctor”.
“I can’t say that openly, it could be the fact. A series of miracles could have saved your dad’s life. A tandem heart as a bridge to an emergency heart transplant is a dream thought. Of course, for a heart transplant to happen someone else should have lost their lives in time, just to save your father’s life. That’s in God’s domain”.
The son gradually got back to his quieter sense. “Sorry doctor, I misunderstood ECMO I was told it was like a lifeboat that will bring back life from a dying heart. Thanks for all your efforts doctor. “No worries, even, many of us haven’t come to real terms with this ECMO stuff. Thanks to misplaced mainstream media coverage concerning celebrity lives”
The much-relieved cardiologist left for home in peace of mind.
Reference
1.Junji Kato, Takahiko Seo ,Hisami Ando et al Coronary arterial perfusion during venoarterial extracorporeal membrane oxygenation, The Journal of Thoracic and Cardiovascular Surgery, Volume 111, Issue 3, 1996, Pages 630-636,
Postamble
Final message
We must realize ECMO is not a new breakthrough technology. It’s a 50-year old concept, that was used primarily in infants with respiratory failure. (VV ECMO) In the complex high-risk interventional cardiology field, it has a different purpose. It gives the aggressive players a little more time to try their luck of reperusing a failing heart.
All these circulatory assist devices Like ECMO, Impella, IABP help to support the heart before a cardiac standstill. Ideally, we may use them prophylactically ( in situ and ready to fire) It has helped save lives especially in pre and post-transplant hearts However, it’s too complex a procedure to be relied upon after unanticipated Ischemic cardiac arrest. We can expect, It might get miniaturized and user friendly soon.