The importance of venous system
Cardiovascular system consists not only of heart but also the blood delivery and retrieval system namely the arterial and venous circulation .As the heart pumps , 6 liters of blood every minute , it has to traverse the entire venous circulation promptly , to complete the hemodynamic circuit.

Source : From web. Thanks to whoever created this Image
While physicians are preoccupied with disease of heart there is an important groups of disorder of venous system .The deep vein thrombosis (Also called venous thrombo embolism . VTE ) is the most important entity .This disorder even though is a cardiovascular disease , it rarely presents to a cardiologist .
As we tended to ignore the veins for decades now, “sudden venous deaths ” other wise called massive pulmonary embolism is calling for our attention
What are the deep veins ?
Popleteal , femoral , iliac (External , Internal , common ) . Upper limb axillary and subclavian veins.
Clinical classification of DVT : Femoro popleteal , Pelvic ( Ilio femoral) , Mesentric DVT.
What are the high risk population for development DVT ?
- Genetic predisposition constitute the strongest risk(Factor V lieden mutation )
- Major orthopedic surgery
- Pregnancy /Oral contraception
- Disseminated malignancy
And now , the more fashionable risk factor “DVT after long distance flights”
What is key diagnostic issues in DVT ?
Key to diagnosis is clinical alertness .Local swelling , edema legs and inflammation should alert the physician.
- Homan’s sign(Pain on dorsiflextion of ankle) .
- Louvel’s sign (Leg pain on coughing ),
- Lowerberg’s sign (BP cuff induced pain on affected leg at low level inflation )
( Well’s score is based on pre test propabilityLancet 1997 )
Many times DVT is diagnosed only after it embolises into lung.So remember shortness of breath and acute dyspnea could be the first manifestation of DVT.
Once diagnosed DVT it should be risk stratified either as low risk or high risk .
Biochemical diagnosis of DVT : DVT is a form of intra vascular coagulation and it activates fibrinolysis.D Dimer estimation has strong negative predictive value .If D dimer is negative it excludes DVT by 99% .Positive D dimer does not confirm it .
Is it necessary t0 image the venous clots ?
No . It is rarely required. Instead we need to know the site of occlusion .Doppler and ultrasound scan can help locate the site of obstruction .
Other modalities * may help evaluate the thrombus
Venous angiography (Filling defect, collateral )
MR angiogram
Fibrinogen tagged nuclear scan
Management
- Acute management
- Long term management .
Acute management
Immediate Heparin , bolus followed by infusion ( 5000U, 1000U/h) followed by oral anticoagulation forms the corner stone of management of DVT .
Once a DVT is documented should we attempt to improve the venous circulation or try to slow down the venous circulation ?
There is a paradox here.The therapeutic strategy is to improve the venous circulation . A sluggish venous circulation predisposes fresh thrombus. So even though , it is logical to expect some migration of thrombus proximally with the standard therapeutic methods of DVT , it is the ultimate principle of management of DVT.
How heparin infusion achieves it’s therapeutic goal of clearing thrombus burden in the venous circulation is not clear .It is believed sub clinical PE occurs in every case with large DVT and these thrombi get microlysed either within focus of DVT or in transit circulation or within the pulmonary vascular bed.
What is effect of intensive anti coagulation on DVT ?
- Lyses the thrombus
- Dissolves the thrombus
- Dislodges thrombus
- It can prevent only fresh thrombus
Answer : All of the above can occur
Can we track the movement of deep vein thrombus ?
It is not an easy thing to track the movement. Doppler will give an idea. Invasive investigation to track the thrombus is neither practical nor necessary.
What is aggressive management * for DVT ?
* Aggression is rarely required in DVT management.
Interventional
- Thrombolysis : Systemic/local catheter based
- Venous angioplasty/Stenting
- IVC filters
Surgical
Indication for thrombolytic therapy
Surprisingly, thrombolytic therapy has limited role in the management of DVT. There is absolutely no role for routine thrombolysis in DVT (Heparin does the same job , more consistently with less risk )
It is used only when there is limb threatening or lung threatening situation .
Pulmonary embolism already occured
Massive iliofemoral thrombosis .
When will you call a vascular surgeon ?
Thromboembolectomy as a treatment for DVT is rarely advocated .
The 2004 American College of Chest Physicians consensus statement on the treatment of thromboembolic disease recommended against the routine use of venous thrombectomy in acute DVT except in cases of phlegmasia cerulea dolens . ( Severe necrotising venous edema )
The issues against surgery are
- Generally these patients are more sick and co morbid conditions
- Complex nature of surgery in deep iliac veins
- Blood loss from deep friable veins
- The surgery further traumatizes the vein, recurrence of DVT is very much possible
- Primary cause is not addressed by surgery
What are the indications for IVC filter ? What are the types of filter available ?
The indication for IVC filter in the acute management of DVT * has been ( Rather continues to be . . .) controversial .The major reason for the controversy is the risk ( The wasted effort too !) to benefit ratio and is not clear.
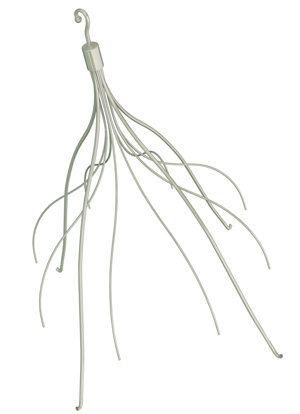
There are three types of IVC filter available
- Temporary venous filters
- Temporary retrieval IV filters ( Gunther tulip ) Nitinol recovery filter Bard
- Permanent IVC filters
*In long term prevention of PE the indications are fairly established.
Differential diagnosis
Is there an entity called superficial venous Thrombosis (SVT)
Superficial venous thrombosis and thrombophlebitis are more common than DVT and should not be confused with DVT. ( Easier said, some confusion is bound to occur !especially , when it occurs over thighs ) .This is common following IV line and varicose veins in lower limb Present with pain, tenderness, or an indurated cord along a palpable superficial vein with erythema. It is less likely to propagate into pulmonary circulation.
How often a superficial venous thrombosis convert into deep vein thrombosis ?
Patients with superficial phlebitis above the knee have an increased risk of deep venous thrombosis and should probably have ultrasonography.They may require warm compression , NSAIDS and local thrombectomy.
What is the post-thrombotic syndrome? How to differentiate it from recurrent DVT ?
Post-thrombotic syndrome is due to the damage to the valves in the veins that leads to chronic venous edema of extremities. It may mimic like an DVT . usually occur within 2 years of DVT.
Unanswered questions
1. What will happen to the thrombus following filter insertion ?
Large thrombus gets trapped in IVC .The problem gets shifted form the legs to the vena cava .This makes it mandatory for these IVC clots to be cleared either manually or pharmacologically. Small thrombus and embolic showers continue to cross the filter without difficulty.
2. IVC filters are recommended in DVT , if a patient has an absolute contraindication to heparin but , is it not a fact , filters also demand anticoagualtion ?
It is true , filters demand anticoagulation. So , oral anticoagualtion should be given whenever possible in all even after IVC filter. This is , not only to make sure filter does not get clogged but also prevent further clot formation in the legs and also distal to the filter in (Procoagualnt ) individuals .Further , anticoagulation forms the mainstay treatment in patients with chronic thromboembolic PAH , which the filter does not address to.
3. Is there safe venous clots that the pulmonary circulation can effectively tackle ?
Typically PE occurs as
- Massive acute PE
- Sub acute PE
- Chronic pulmonary thrombo embolism (Showers of microemboli lead to PAH )
Consider the following pulmonary vascular anatomy : MPA 2.5cm , RPA, LPA 1cm segmental pulmonary artery 5 mm , pulmonary arteriole 3 mm , pulmonary capillaries 200 microns . The deep venous thrombus typically has a diameter of up to 1-1.5 cm . It needs a at least 2. 5 cm diameter clot to occlude the main pulmonary artery.Micro thrombus may get cleared by pulmonary vascular bed.There can be safe venous clots.
Final message
- DVT and PE are the common venous emergencies.
- Prevention of PE is the major aim of acute managment.
- Identifying the underlying cause and prevention of DVT per se is the long term aim.
- Aggressive local approach is largely unnecessary except in leg / lung /life saving situations
Intensive Heparin protocol followed by long term oral anticoagualnats (1 year or more) is an excellent approach in most patients.
The most important point to remember is the treatment for high risk DVT and suspected or established PE is exactly same
*Only 10% of PE are candidates for thrombolytic or surgical therapy so at times of real dilemma , there is nothing wrong in administering heparin in all patients with suspected high risk DVT/PE even without confirmation.
All those hi fi stuff of V/Q scan , pulmonary angiography may be a misadventure .Remember empirical (Some call it as unscientiifc ! ) therapy too , can save many lifes
Further reading
Best Link for IVC filters http://www.tigc.org/eguidelines/VenaCava.htm
References
-
Decousus H, Leizorovicz A, Parent F, et al. A clinical trial of vena caval filters in the prevention of pulmonary embolism in patients with proximal deep-vein thrombosis. N Engl J Med 1998;338:409-415.
What is new in catheter thrombolysis in DVT ?

http://www.bacchus-vascular.com
A interventional catheter based clot lysis for DVT
For the comprehensive ACCP 2008 guidelines of managing DVT reach the following site
Read Full Post »