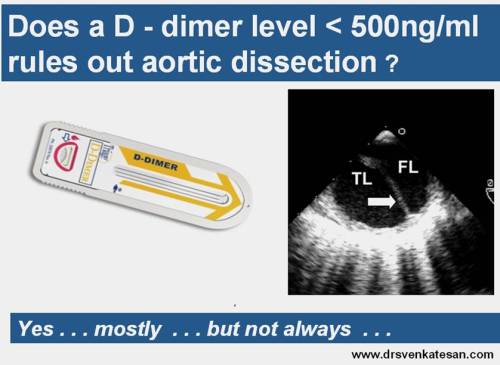
Role of d dimer in acute aortic syndromes
D -Dimer is a marker of intravascular fibrinolysis .It is a degradation product of fibrinogen. A level more than 500ng/ml is significant.In acute aortic dissection this level is reported to be more than 2000ng/ml.
The beauty of this molecule is it is elevated in three important chest pain emergencies.
- Acute myocardial infarction
- Pulmonary embolism
- And now aortic dissection.
The issue is not simple , as we know any intravascular coagulation and lysis can elevate this molecule.In patients with chronic CAD as like a chronic thrombotic lesions within the coronary arteries can also elevate d dimer.
Similarly , in portal, cortical, deep venous thrombosis all result in elevated D dimer.
So , such a non specific test , how can be useful in the diagnosis of aortic dissection ?
Yes, you are right ,
D Dimer helps us not in diagnosing aortic dissection but helps us in ruling out a possible dissection
D-Dimer levels <500 has a negative predictive value of 98% .
What is the bio- chemical dynamics of D dimer in dissection ?
D dimer in aortic dissection is mainly secreted within the false lumen. For d dimer to secrete into systemic circulation the clotted area should be exposed to a adequately flushed systemic blood at a good perfusion pressure.The contact area between the clot and fresh blood is of critical importance.
So , even though it has been reported d dimer has near 100% negative predictive value . . . is there a chance a dissections might occur with normal d dimer levels ?
Yes, very well possible with due credits to published data
- A dissection without thrombus(Rare . . . but still possible !)
- A clot confined to false lumen with entry or exit points sealed.
- A dissection without a exit point.
- Intramural hematoma with no communication with aorta
Infrequently asked questions
- Time window ? Dimers are mainly useful in patients who report before 24h after the onset of chestpain.
- How long it takes for the dimers to get excreted ?
- Can coronary dissections in STEMI elevate dimer ?
Final message
D dimer is mainly useful in “not making a diagnosing” aortic dissection.
If dimer levels are strongly positive and clinically the patient has has no evidence for acute MI or acute pulmonary embolism and continues to have chest/back/atypically located pain suspect aortic dissection , and order for further imaging like TEE,MRI, MDCT etc.
* Do not forget the role of routine , simple bedside transthoracic and suprasternal echocardiogram.It can diagnose dissection correctly in good number of patients.
** Never oder for costly thoracic imaging whenever d dimer is elevated.
*** When you send the sample for dimer make sure to mention the clinical likelyhood of dissection .If it is very high the lab has every reason to reject the sample and suggest you to go ahead with thoracic images.
This is because , it could be costly miss . . . if you depend on dimer to diagnose a dissection
Imagine this scenerio , while your patient has a absent left radial pulse due to dissection and you are waiting for the lab report to arrive !
Never use it for diagnosing aortic dissection.