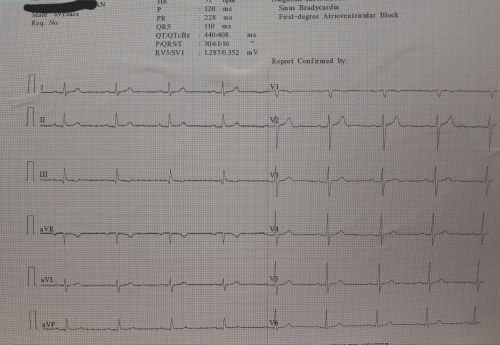
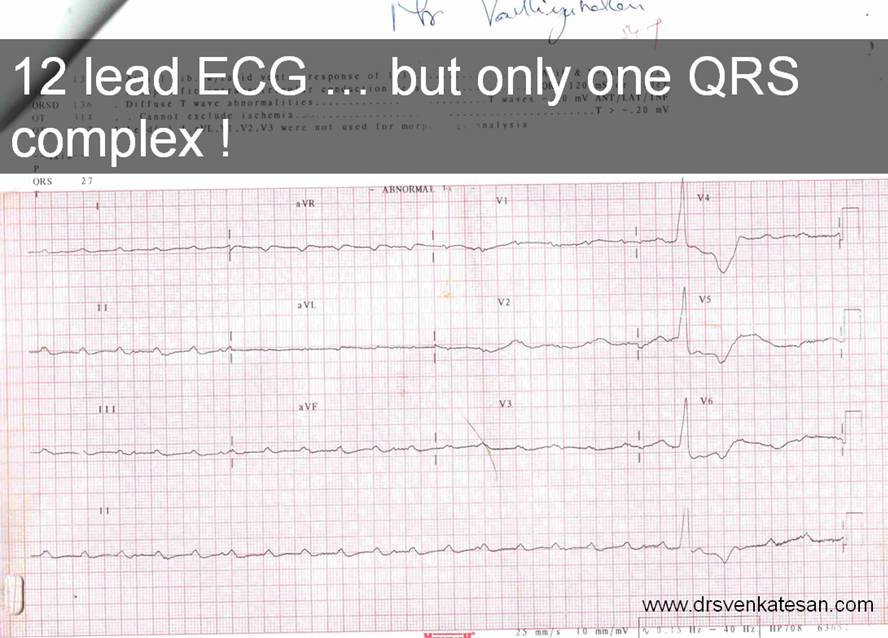
This ECG can help you find an answer .HR is 50/mt. Find the PR interval .It is also printed right there.
What happens to PR Interval in sinus Bradycardia ?
A. Remains normal
B. Prolonged but within normal
C. Prolonged beyond normal
D. Depends on the cause of Sinus bradycardia
Answer
When cardiac cycle slows down, every interval must get prolonged. PR interval is no exception. If you apply that rule the answer would be simple (Its B ).But this question has much more issues hidden into it. In this ECG it touches on the doors of first degree AV blcok. Normally PR doesn,t stretch that far in isolated benign sinus bradycardia.
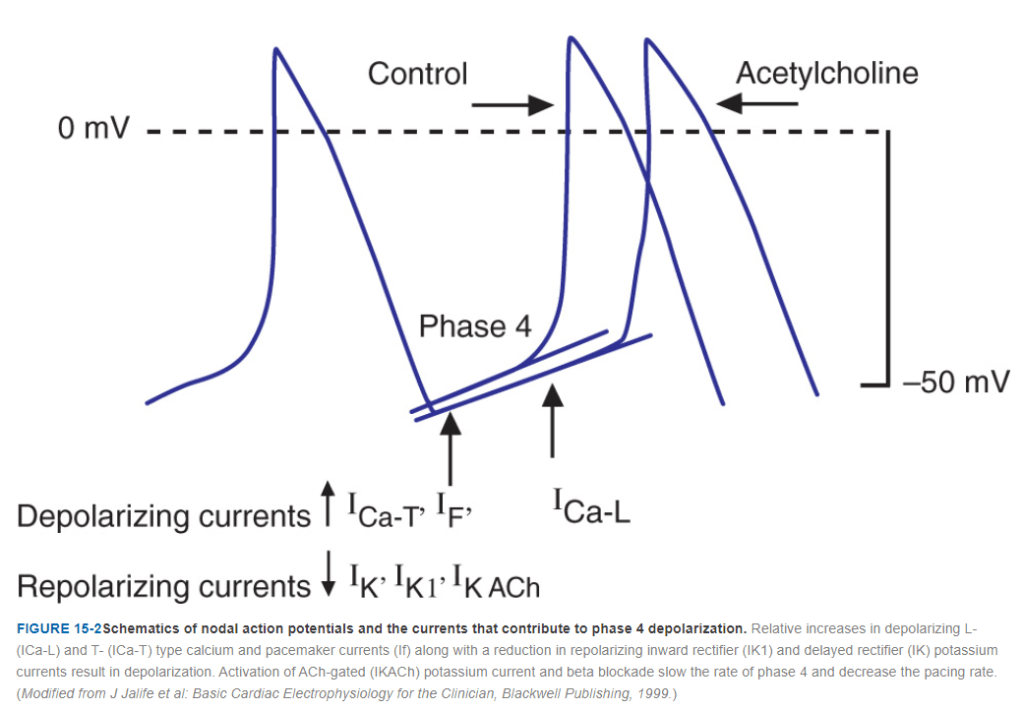
Sinus rate is determined by SA nodal, funny pacemaker current(if) .The rate of which is determined by the delicate balance between sympathetic and para-sympathetic signal flux. The dynamicity of the slope of phase 4 , ie spontaneous resting membrane is another key determinant apart from sift in the density of mean P cell firing focus .(see below)
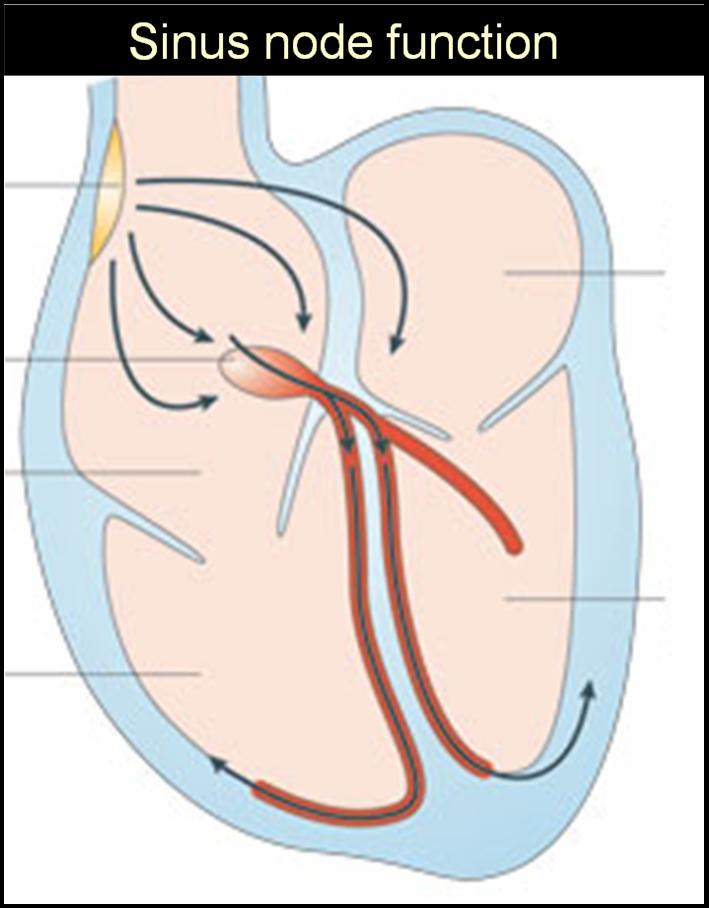
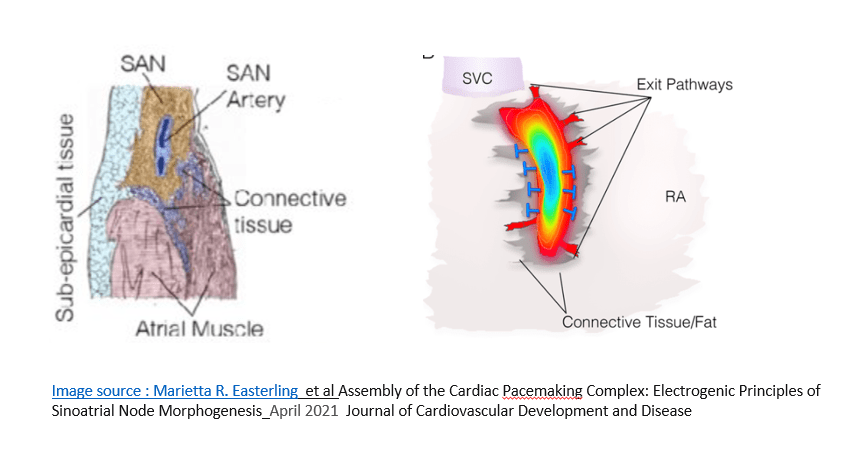
The sinus rate depends upon the cranio- caudal shift that occur within specialized tissue .(10-15mm slender the basmati rice shaped SA node)
When do PR interval prolong in sinus bradycardia ?
The commonest cause of sinus bradycardia is due to increased vagal tone . It is no secret , vagal tone do Influence AV node as much as it does the SA node . So, what can we expect ? Logically .the AV node must also slow down . But does it happen really ?
No, most of the time the AV nodal delay doesn’t not occur in sinus bradycardia . Does that mean the vagal spill over do not reach the AV node ? It does, but the fact is, the reduced heart rate attenuates the normally prevalent decremental conduction property of AV node. So we do not expect a prolonged PR in sinus bradycardia.
However, if PR interval is prolonged in sinus bradycardia , we can except silent pathological states like , sinus node dysfunction where AV node can also be affected. Also, prolongation of PR is very common in ACS situations in Infero- posterior (RCA/LCX) territory where both SA and AV nodes are simultaneously targeted.
Prolonged PR in bradycardia some times is a hemodynamic necessity as ventricular filling time is prolonged.
Clinical Implication
It is a good habit to have rapid glance at PR interval in every patient with sinus bradycardia. This will ensure a rare miss of AV nodal dysfunction .
Final message
PR interval is normal or show little prolongation in most of sinus bradycardia. If it is prolonged, without any circumstantial evidence for enhanced vagotonia , then, it could indicate some thing wrong in the conduction system. Atropine test might help us out in differentiating true vagotonia from intrinsic delay.