It is tempting to fix the “Force of cardiac contractility” , to be the prime determinant of systolic blood pressure* . Rather , it is influenzed heavily by multitude of anatomical and physiological factors.
” In most life instances the primary determinant blood pressure is not the state of cardiac contractility “
For many , this would appear as shocker of a statement !
Fellows should not be confused with above inference . What it means is , the heart initiates the blood pressure by a brief period of systole .The pulse wave attains a peak during ejection phase . This is the peak systolic blood pressure . There is nothing called sustained systolic blood pressure . The quantum and duration of peak systolic pressure contributed by the LV contraction is far less than we imagine .
If blood pressure is to be controlled primarily by cardiac contractility , how is that , a blood pressure of about 80mmhg is maintained throughout diastole when the heart is taking rest and the aortic valves are closed ?

Image courtesy http://www.mayoclinicproceedings.com/content/85/5/460
The major elastic blood vessels aorta and the major branches use the potential energy gained during systole (Like a rubber band ) into kinetic energy as vessels recoil during diastole . This recoil imparts an important component to the diastolic blood pressure augmentation and maintenance.
It is prudent to note since diastole is much longer than systole , integrity of the vascular tree become much more important to maintain the blood pressure till the next systole arrives.
Note
*The cardiac contractility , might still be important in determining systolic BP in patients with severely compromised LV function** For example , in dilated cardiomyopathy with LV failure , systolic blood pressure will be directly related to LV function. When LV function is critically low , the elastic blood vessels fail to amplify the blood pressure beyond a limit.
**Still it is not uncommon to find high systolic blood pressure recorded in the back ground of with severe LV dysfunction especially hypertensive individuals.
What happens during aging ?
The aorta and it’s major branches gets thickened , the vascular collagen goes cracking with wear and tear of life. In effect , these vessels become less compliant . So , when blood is rapidly ejected from the left ventricle into aorta and their branches it’s distensibility is reduced .This fails to dampen the pressure wave and hence systolic pressure spiking occurs. This we refer to systolic hypertension of elderly.
It is important to emphasise major elastic arteries has a big say in fixing the systolic pressure. For the same cardiac output systolic pressure can surge in elderly this is why we have kept the normal in adults as 16o mmhg.
Another key point to be understood is , Aortic compliance has an impact on diastole blood pressure too ! . The stiff vessels during diastole bring less diastolic recoil. Diastolic recoil of large elastic arteries determines the diastolic pressure . Hence there could be a mild fall in diastolic pressure with physiological aging when recoil is attenuated . Since the reduced diastolic recoil ensures diastolic pressure from being elevated the entity is aptly named as isolated systolic hypertension.(ISH)
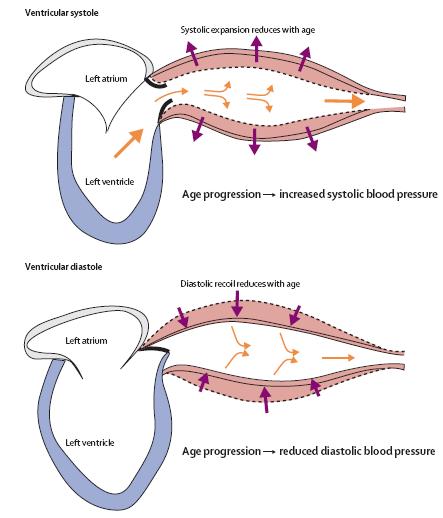
Image courtesey :Norman M Kaplan, Lionel H Opie Lancet 2006; 367: 168–76
Final message
While the traditional teaching ramains as systolic blood pressure would be determined by cardiac contractility / cardiac out put , while the diastolic pressure is determined by peripheral vascular resistance .This is not an absolute reality , rather it is too simplistic way of teaching circulatory physiology !
The peak systolic blood pressure is more often determined by the integrity of Aortic and major arteries rather than cardiac contractility and stroke volume. Similarly , aortic properties do have a say in the diastolic pressure as well !
Further reading and debate
The net effect of aging on blood pressure : Is it physiological or pathological ?
Should we treat this raised pressure due to aging related systolic hypertension ?
There is a huge controversy going around , regarding the need of treating this mild elevation of systolic blood pressure due to arterial stiffening .This will be addressed separately in this forum .
Reference
http://www.mayoclinicproceedings.com/content/85/5/460.full.pdf+html