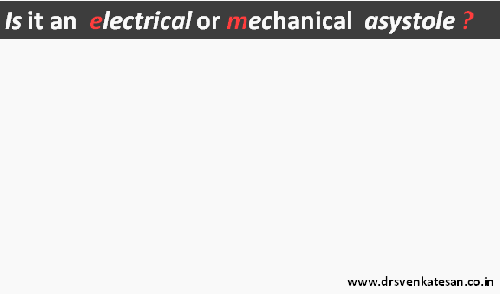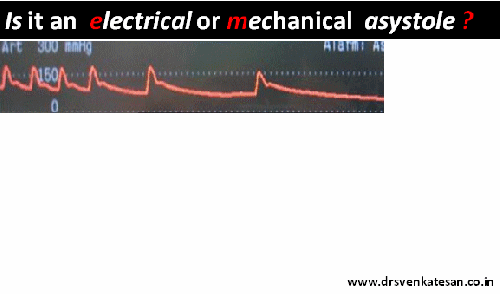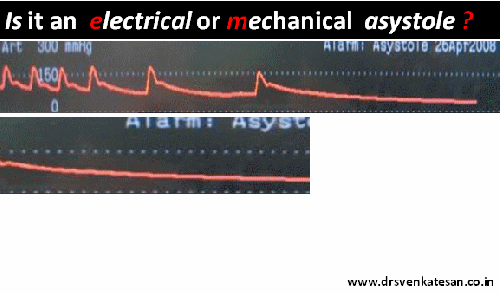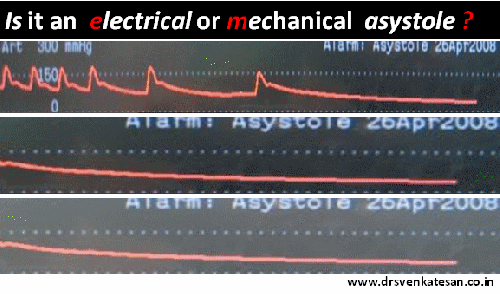
When a life leaves the body silently in CCU , an undulating flat line in the monitor has a hidden scientific tale to tell !
A 56 year old obese women died a instant death immediately after engaging the Left main ostium after first injection of 5cc dye. The monitor showed only a short pause, few sinus beats , a long pause , asystole and death . In the last 2 minutes of survival she threw a random wave forms of suggesting EMD . At any point of time she never showed any evidence for ventricular fibrillation . 1o minutes of intense resuscitation failed that included temporary pacing , repeated shocks and ventilation.(ECMO /LV assist excluded)

What is the mechanism of death ?
- Is it electrical or mechanical ?
- Acute mechanical stunning / the stone heart ?
- Is it a primary electrical asystole ? (Acute sinus arrest or AV block )
Post hoc analysis of CAG did not show any significant clues except a tight distal left main.Apparently the catheter has triggered the event .( Or is it the dye ? as some body suggested it as anaphylaxis ?)
Even though we conveyed the message to the relatives, it’s was an unexpected massive heart attack , obviously we were not convinced with our uttering ! Mind you , she had normal LV function but had recurrent angina prior.
We know if cardiac arrest is due to VF, it tends to give us at-least some time and sense. Further,the VF protocols are more clear and success rate is more .
There is always an issue of fine VF vs asystole.If the flat line is indeed VF , there is more chance of revival as we try to pump adrenaline to make the fine VF into coarse one and shock again .The sequence can continue few times.
It is well known asystole has a dismal outcome .Even among the asystole there is some hope* if asystole is purely electrical . (Like Stokes Adams in CHB or electrolytic asystole like hyperkalemia etc ) .But if asystole is due mechanical cause , death ensues in spite of prompt temporary pacing .
* Important note : We have this common form of treatable mechanical asystole .It is called cardiac tamponade .It always present with extreme bardycardia and asystole. It is extremely rare to see a tamponade to present with VF. A prompt needle tap will do the job .It is vital to recognise this in cath lab as our efforts are rewarding .
I would recommend a hand held echo machine , to hang like a catheter in every cath lab , ready to screen unexplained cardiac arrests with zero delay !
Why some hearts respond with VF , while others go for asystole with acute coronary insult ?
- A million Rupee question ! We are yet to find a legible answer .What is probable is the the heart doesn’t even have energy to fibrillate !
- The underlying disease need to be so intense .In this case it was left main stenosis supplying a truncated LAD and LCX. We could also see it supplying twigs to RCA suggesting it to be a total occlusion .
- So ,when a “physiologically single” coronary artery that precariously supply the entire heart is suddenly insulted the heart behaves violently with runs of VT/VF. Our ignorance is complete when we realise the heart can do the opposite as well .It does not react at all , goes for a deep slumber and result in electro-mechanical sudden death.
- It is expected , in acute mechanical deaths one may encounter flash pulmonary edema if the LV alone gets stunned. However , if both right and Left ventricle come to standstill in a synchronised sudden fashion , lungs will be as silent as deep sea . We believe this is what happened in our patient and it can be logically correlated as the critically narrowed left main was supporting the RCA as well.
Final message
Sudden cardiac deaths 9 out of 10 times is electrical . Majority of them is due to fibrillation. Next comes the electrical asystole ,Rarely (is that really rare ?) an ultra fast sudden death due to mechanical asystole (Non -Tamponade ) is possible , as experienced in our patient .
These mechanical asystole are yet to be decoded.Whether it is a form of Acute stunning , electro -mechanical uncoupling or mechano electrical standstill is not clear.
Read Full Post »