Ventricular tachycardia is considered as one of the most dangerous cardiac arrhythmia .Rather , it is the label VT that spreads more fear than the arrhythmia itself. It is a fact many patients with VT walk into hospital , still VT will always be a sinister arrhythmia as long as it carries a risk of degenerating into ventricular fibrillation.
What determines hemodynamic stability in VT ?
- Origin and location of VT
- The ventricular rate
- Presence or absence of AV dissociation
- Impact on mitral inflow pattern
- Associated left ventricular dysfunction or valvular heart disease.
- VT in the setting of acute coronary syndrome.(Ischemic VT)
- Inappropriate drug selection
Origin and location
VTs originating high up in the ventricle( High septal VT,Proximal VTs) have more organised ventricular contraction and they are more stable.Distal VT originating in the myocardium away from the conducting system has chaotic myocyte to myocyte conduction.These are very unstable.
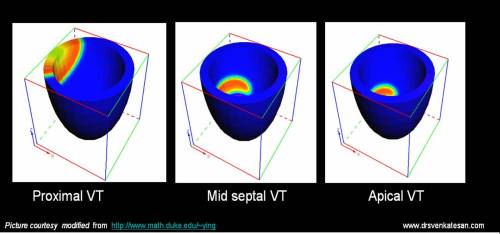
The term fascicular VT is nothing but VTs originating in the His bundle and it’s branches( Can also be termed Septal VT ).These VTs are also stable and some of them respond well to calcium blockers indicating that they are very close to the AV junction and carry the properties of junctional tachycardia. QRS width gives a rough estimate about the location of VT. Narrower the VT higher it’s origin.( But remember even in VT , qrs can further widen on it’s way downhill !)
LV dysfunction.
This is probably the most important determinant of the outcome in VT. Patients with severe LV dysfunction (EF <30%) fare badly .Hence the land mark concepts from MADIT 1& 2 demanded ICDs in these patients.The most common clinical setting is dilated cardiomyopathy.SomE of them have bundle branch re entry(BBR).This particular VT can be stable for many hours.
Ventricular rate.
Usually VT has a rate between 120-200.Higher the rate of VT more the chances of instability .This rule is also not always true as fascicular VT can be well tolerated at high rates.So location of VT focus and LV dysfunction usually over rides the impact of ventricular rate.
Mitral inflow pattern
Proper left ventricular filling is the key to hemodynamic stability in VT. In proximal, septal,fascicular, LVOT VTs doppler studies suggest (ACC /AHA Type C evidence : Personal observations in CCU during VT) near normal preservation of bi modal filling of mitral valve inflow.In ischemic myocardial VT the mitral inflow profile is critically affected . There is no distinctive forward filling was observed .In fact at rapid rates a short pulsatile MR jets are noted instead.
Associated valvular diseases
It is obvious, aortic and mitral valve disorders can aggravate the hemodyanmic instability.
Final message
The clinical behavior of ventricular tachycardia is widely variable and dependent on multiple factors.
Associated LV dysfunction and structural heart disease ultimately determine the outcome.
Read Full Post »


