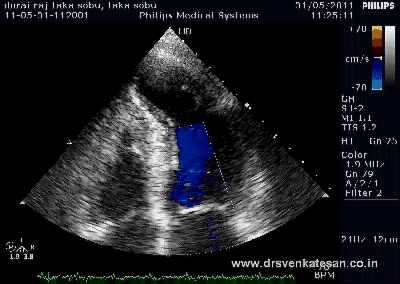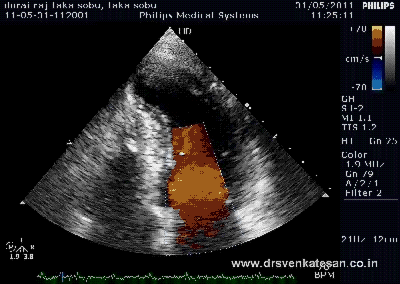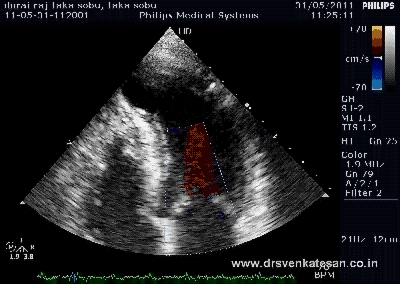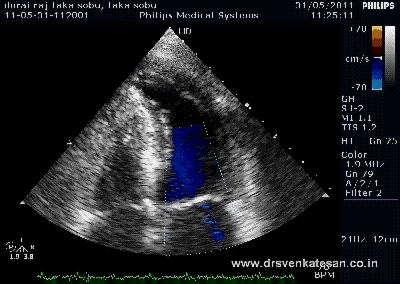
Brugada syndrome continues to fascinate us for two reasons.
One , it deals with mysterious sudden deaths of young men and women
Two , it is one of the fine examples of how advances in molecular biology , links physical defects in ionic channels to sudden electrical death (Most of them are due to inherited defects sodium channels of myocyte cell membrane )
While high risk subsets of Brugada are easily managed , it is the asymptomatic ones that bother us.
The following are some of the difficult questions , a cardiologist faces when dealing with patients , who exhibit only Brugada pattern in ECG .
- Should I go for an EP study Doctor ?
- Will I require an ICD Doc ?
- Do I carry a significant risk of dying suddenly ?
- Do I need a genetic test for sodium channel mutation ?
Fortunately, we can answer all these questions with much courage than before.
(Thanks to the European Finger registry published in 2010 !)
“No” is the clear answer for all of them !
Summary from the FINGER registry.
(France , Italy, Netherlands, GERmany)
The registry included 1029 consecutive individuals
(1) Aborted SCD (6%);
(2) Syncope otherwise unexplained (30%);
(3) Asymptomatic patients (64%).
In the follow-up of 31.9 (14 to 54.4) months . A total of 7 death occurred .
The cardiac event rates per year was
-
7.7% in patients with Aborted SCD,
-
1.9% in patients with syncope
-
0.5% in Asymptomatic patients.
Predictors of cardiac event
- Previous syncope
- Spontaneous type 1 ECG
Non predictors ( Surprisingly there were more non predictors ! )
- Gender has no predictive role
- Familial history of SCD,
- Inducibility of ventricular tachy-arrhythmias during EP study,
- Presence of an SCN5A mutation
Follow up
PRELUDE study almost reaffirms Finger data
(PRogrammed ELectrical stimUlation preDictive valuE)
Just publicized in JACC 2012 from the pioneer of Brugada Silvia Priori of university of Pavia Italy
Reference
http://circ.ahajournals.org/content/121/5/635.full.pdf+html