Let me see how many find sense in this Nonsense !
Archive for the ‘Uncategorized’ Category
Evidence less cardiology : Is “No-flow” better than “No-reflow” in STEMI ?
Posted in Uncategorized on January 26, 2019|
Cath labs are probably the best place to practice preventive cardiology . . .
Practice of medicine is primarily guided by Infinite Information , plenty of Intuition, little bit of Intelligence and unquantifiable amount of Ignorance.The science of coronary reperfusion is standing example for variable mix of the above.The term no reflow is a jargan used liberally in cath labs right from first year fellow to super consultant without knowing what exactly they mean by it.
What really is No-reflow then ?
The academic definition :According to Kloner no-reflow is defined as suboptimal myocardial reperfusion through a part of coronary circulation without angiographic evidence of mechanical vessel obstruction.( Kloner RA, Ganote CE, Jennings RB. “The “no-reflow” phenomenon after temporary coronary occlusion in the dog.” Journal of Clinical Investigation, 1974; 54: 1496–1508.)
With due credits to his seminal paper, I always wonder what exactly Dr Kloner meant when he labelled it as No-reflow!
No is ok , Flow is ok , What does the adjective “re” mean to you ?
Re stands for repeat ? recurrent ? Yes , it may mean any one of it. It may mean nothing in many patients as their post PCI flow is same or found to be no better than pre PCI flow with no significant forward flow at all ! In this situation No-reflow is same as No-flow (Never flown ) in physiological terms irrespective of epicardial patency.
Literally, the term no re-flow tell us, there has been a dramatic procedure related*( or preexisting ) destabilization in distal blood flow. It can be any downgrading of basal TIMI flow. ( Example : TIMI 3 becoming Zero , or TIMI 1 becoming 3 then back to 1 or Zero.) The terms slow flow, low flow, stuttering or trickle of flow all fall under the common category No reflow. In a crude manner one may conclude no reflow to be masquereding term for failed PCI.
*Mind you , No reflow can also occur with pharmacological lysis as well.(Less common)But personal experincee suggest it has a less benign course.
Mechanism of No- reflow
Many mechanisms has been proposed and disposed by experts. However , all suggested mechanisms end up in the final common theme ie micro vascular obstruction.
Can no-reflow precipitate a fresh ACS ?
Could be yes . How ? The distal thrombus migration clogs the active collateral channels at its entry point.This is probably the most unrecognised concept which is difficult to prove though.The problem is , we may not realise this as it could be silent or may just present as LV dysfunction , Infarct extension, or Ischemic cardiac failure.
Why is treatment of no reflow is so dismal ?
I think, by now you can guess the answer and get it right too !
Is no flow better than No-reflow?
It may seem a foolish question one could come across in coronary hemodynamics. The prevailing coronary doctrine, as we understand is , all ATOs need to be opened in STEMI in an emergent fashion. (Other wise patients or their myocardium can’t be salvaged )But, we also realise ATO do get converted to CTOs in a safe manner following a STEMI in a significant number. It’s the ultimate myocardial mystery when we realise even the ATO fails to damage the myocardium significantly in some patients.
Presence of acute collateralisation to IRA from non IRA is observed instantaneously and spreads rapidly towards myocardium in distress.It is observed in atleast 40% of all patients.(Ref 2,3).
The anatomical and physiological codecs of acute collaterals in ACS is secretly located close in the God’s domain.But, Interfering with it, is definitely in human domain.
Should we need to worry about the impact of PCI on these acute collaterals ?
It is estimated up to 5 grams of thrombus could spilled over to the distal coronary bed. Mind you thrombus formation is not a one time process.Can you guess where these thrombus lodge in ? We don’t know what is thrombus clearing capacity of LAD/LCX/RCA vascular bed. But. we have observed naturally formed thrombus is less likely to disseminate and migrate than the catheter and wire induced.My presumption is , coronaries show their dissent and disapproval in the only way they know, ie non stop generation of thrombus (Not withstanding our DAPT/2b 3a /Bivaluridins etc)
Acute collateral shutdown : A new concept

We are not sure if there is a collision between two streams of reperfusion that happens after a STEMI. One spontaneous from the collateral and other from antegrade(Either spontaneous or man made)
Is it benefitial, detrimental or neutral ? We don’t know the answer for sure. My understanding is some of subset of critical STEMI are heavily dependent on this life line however miniscule it may be.
It doesn’t require a double blinded study to prove what would happen when a hurried cardiologist attempt hurried PCI who often has to a change his target to thrombus instead of myocardium .
When aggression is shown on the thrombus, it’s more likely you end up in no reflow . One possible new mechanism(Proposed by the author) of No reflow is distal dissemination of thrombus debri that plugs the lateral entry points of collaterals.
This is the time , no reflow shows its violent face. Invariably hemodynamic deteriation occurs and the entire reperfusion team would seem to count their luck than expertise.
Can we perceive, predict and prevent this ?
We should , we need to , but how ? Since we know the true success rate of no reflow is miniscule, serious introspection to be done. Funnily (but realistically) one can take a famous cue from the most underrated medical specialty Social and preventive medicine .
Yes it’s “Prevention is better than cure” and mind you, if there is no cure, how important prevention becomes.Strangley , preventive cardiology is meant for lesser professionals , who and talk about diet, excercise and lifestyle.
No , it’s not . Preventive medicine needs a new defintion , rather new understanding .Its’ all about preventing an expected or unexpected adverse event anywhere.
How many of us really believe there is no effective cure for No-reflow and it is directly related to aggressive thrombus clearance strategies .
Should we argue new age Interventionists to practice preventive cardiology right inside the cath lab and do away with non-academic temptations.(Surprise , this is exactly mega trials on thrombus aspiration told us (Class 3 Indication for routine thrombus meddling)
Final message
Stable and comfortable, late ATOs need not be opened like defusing a time bomb. We will never know which side of the bomb the cardiologist is sitting.
The incidence of new onset No-reflow can be higher than what we presume.Further it can trigger a fresh ACS by whipping up the injured and resting myocardium.(Mostly attributed to late reperfusion Injury and the acute collateral shutdown.)
Postample and Counterpoint
As an interventional cardiologist, No-reflow is one among the expected complications , which are part of the profession.Never bother about these unscientific utterrings . That’s the job of critics. You go ahead and fight with the coronary artety in every case of ACS. Only weak minded unprofessionals would love to sit on a case of ACS and play a waiting game in CCU. True professionals shall look for multiple criminal targets beyond thrombus, myocardium, IRA , non IRA, doesn’t matter . Do it with confidence.Hope for the best, don’t bother too much about the endpoint.
Mind you, that’s what , we are trained and paid for and possibly respected too in this most glamorous subspecialty of Medicine.
Coming next
*Is Catheter, Guidewire Induced thrombus radically different from natural denovo thrombus ?
*How common is angiographically blind No reflow.(TIMI 3 with good and bad blush included)
*What are the residual defects and long term myocardial sequale ? (Inspite of successful tackling of No reflow )
Reference
1.Claire Bouleti et all The no-reflow phenomenon: State of the art Le no-reflow : état de l’artArchives of Cardiovascular Disease (2015) 108, 661—674
2.L YJ,Masuyama T,Mishima M, et al Effect of pre-reperfusion residual flow on recovery from myocardial stunning: a myocardial contrast echocardiography study. J Am Soc Echocardiogr 2000;13:18–25. doi:10.1016/S0894-7317(00)90038-5
Impact of coronary collaterals on in-hospital and 5-year mortality after ST-elevation myocardial infarction in the contemporary percutaneous coronary intervention era: a prospective observational study
The crazy science of coronary reperfusion : When TIMI 1 & 2 beats “TIMI 3” in the myocardial salvage race . . . cardiologists get confused !
Posted in Uncategorized on December 8, 2018|
The prime job of cardiologists is to restore coronary blood flow in an emergency fashion. While we do this with reasonable success ,there is still a missing link between our Initial aim and achieved goal.
It’s all too common situation in any busy cath lab , to see two similar STEMI patients with identical time window & proximal LAD as IRA , in totally different scenarios. In the first patient we find a trickle of flow in LAD , who is relatively comfortable with normal LV function (In whom , emergency primary PCI might appear redundant.) While the other patient , even after rapidly established TIMI 3 flow , LV wouldn’t look good at all . All our efforts to reperfuse is found wanting. Ultimately LV goes in a downward spiral , ends up in irreversible cardiogenic shock or fatality inspite of Impellas, ECMOs and other LV assist exotica !

I can promise , you can never guess from the angiogram whether this ACS patient was very much comfortable or he is in cardiogenic shock on ventilator unless I reveal the history. Am I right ? That is the mystery of coronary circulation and hence its so critical to serve the myocardium what it wants ? Never treat a coronary artery in isolation !
What is the possible explanation ?
The first trickle (Say TIMI 1 which is usually spontaneous or lytic related ) is the one that’s going keep the muscle viable and possibly prolong the time window for the subsequent reperfusion strategies .Hence it is the timely TIMI 1 or 2 is much more critical than delayed TIMI 3 (Still rapid).
Time window woos :
Who fixed the reperfusion time window as 6 to 12 hours ? Do you know on what basis the acceptable delay of 30 to 60 mts related to primary PCI ? was made acceptable by cardiology community ? If you analyse the published data both are highly contentious and empirical. ( Suggest you scrutiny the data from DANAM2 , PRAGUE and AIR PAMI and come to your own conclusion) (*These are the 3 sacred studies done with few thousand patients that redefined our approach to STEMI and gave the licence to waste the golden hour ! )
I remember reading the Robins pathology book (Bible of pathology William Boyd as well ) in early days of medical school myocardium may die even within 1 hour with wavy necrosis, contraction bands etc. Looking back some times I wonder how the clinicians have conveniently prolonged time window with whims and fancies of science Intact.
Concurring with the pathologists , we have learnt some harsh lessons inside the cath labs. One of them is that even ultra fast pPCI can fail to salvage myocardium, meaning that time is not the ultimate thing in our race. (There should be other important determinants )
A brief journey back into our pathology classes : Have a look at this table
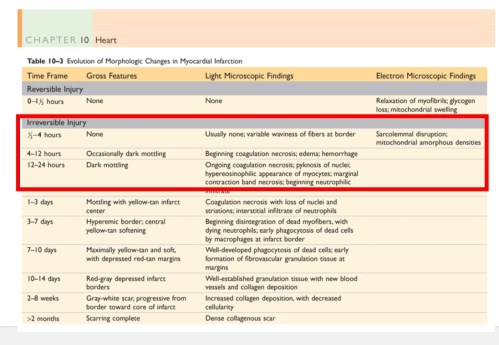
Please note, Irreversible Injury might happen any time after 30 minutes .Of course it can vary . But, the question is how are you going to identify these patients with ultra short time windows? source : Robbins Basic Pathology 9th Edition.Elsevier
Other factors that influence myocardial cell survival
- Tendency of myocardium becoming electrically unstable
- Criticality of non IRA lesions
- Ischemic preconditioning
- Gender dependent reperfusion times
- Efficiency of collateral circulation
- Reperfusion Injury (R.A. Kloner, Ultrastructural evidence of microvascular damage and myocardial cell injury after coronary artery occlusion: which comes first?)
- Co-morbid conditions
Re-perfusion is not a single edged sword
We may wish the concept of re-perfusion Injury is a myth : Unfortunately it is not ! Myocardium doesn’t relish (not always) the return of circulation in full dose. (May be it’s laying and taking the much needed rest with the initial Injury!)
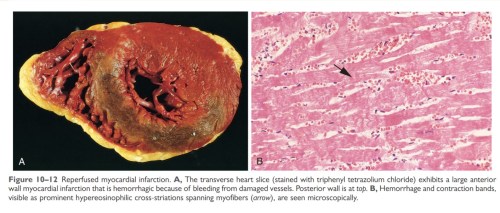
Sudden gushes of blood leads to extravasation into the interstitium (due to damaged capillaries) increases the Intra myocardial resistance and obstructs the microvascular flow. We have witnessed more than a handful of patients going for cardiac arrest once IRA is opened (of course, we might be able to resuscitate many of them )
Myocardial hypoxia resistance time
Please realise ,true STEMI clock starts not with onset of symptoms but with time of total occlusion.There is more than subtle difference between the two. Onset of total occlusion to symptom time is not a well explored or understood Interval. We take it for granted that the onset of symptoms coincides with total occlusion.
But in multi vessel CAD, even a CTO can cause a STEMI through loss of distal collaterals. Further ,the presence and absence of pre-infarction angina (PIA*) , ischemic pre-conditioning (IPC*) sensitizing effect of remote CAD , manifest vs recruitable collaterals all these make the fixed time windows with which we did our land mark studies of PCI / lysis academically questionable.
* Both PIA IPC are master confounders in the true time window calculations .We don’t know whether its due to ischemia tolerating myocytes or pain tolerating nerve fibres responsible for this varying presentations.But the mystery is certain , when we realise the angiographic spectrum of ACS can range from silent ATOs to painful CTOs
Final message
Is timely reperfusion (and its favorable effect ) lies in God’s domain ? If you we believe myocardial susceptibility , arrhymogenicity and recovery to hypoxia is genetically determined ,then the difference between fate and science Is much narrower than we think .Its appears we can change the former with the later with both positive and negative outcomes. So ,the “f” word may not be a forbidden at-least in the STEMI management. It resides not only within the human genomic codecs written with double-helical nucleic acid fonts . . . but also in the nimble and restless hands of both novice and experienced interventionists !
A study proposal
Let me make a hypothetical statement .A significant subset of patients with STEMI have ultra short myocardial survival and we are unable to identify these hypoxia challenged hearts where primary PCI related delay could be a myocardial sin. Any one willing to prove or disprove this hypothesis ? If some body take this quixotically important study in STEMI management please give me some credit as a contributor !
What is the blood supply for the coronary artery ?
Posted in Uncategorized on July 10, 2018|
One may recall some stunningly simple facts from our high school biology classes that every living cell needs energy on a moment to moment basis.
Blood vessels which take care of the vital organ’s energy supply also need the same blood (Nutrients /Oxygen) for its own survival.
Coronary arteries carry about 250 ml of blood every minute , 24/7 supplying ATP enriched fuel to the heart.
Who is feeding these delicate vessels which carry on this life-sustaining work ?
It is easier to assume the three layers of the blood vessels which are bathed with blood would never suffer from Ischemia. Reality is different .Blood vessels do suffer from Ischemia.We do have evidence medial necrosis, plaque instablity , fibrous cap disruptions may be due to a vascular insult or vessel wall energy deficit.
The much debated entities like endothelial erosion and dysfunction are often atributed to mechanical stress , sympathetic spike , or smoke . This may be a virtual guess as no one knows what causes these. It could well be a patchy Ischemia due to endothelial perfusion defect from within or a vasavasoral dysfunction from outside. Coronary ulcers some times mimic gastric ones and guess the cause ! yes it is mucosal ischemia !) *Ischemic ulcers in GI tracts can be common (Schweiz Rundsch Med Prax. 1993 Jun 15;82(24):709-13)

Image source http://www.wikidoc.com
How does coronary artery gets it blood supply ?
Busy cardiologists have no time to worry about nourishment of the coronary arteries . . . even as they play inside with unlimited arms and ammunition.We leave it to our basic scientists.
So , how does coronary artery gets its blood supply ?
The easiest answer is, blood supply to coronary artery is taken care by a vast network of micro vessels called vasa vasorum(VV) . Of course, the inner layers of Intima and media do get some nourishment by the flowing blood as mentioned earlier.No one really knows the quantum of blood flow that perfuse within the planes of coronary artery.
*By the way , does the vasa -vasorum comes from extra-coronary source or from the same parent vessel ? (I think the answer is both ! will try to find out!)
It should be noted Vasa vasorum is well developed only in large arteries. VV has one more important function ie to drain the metabolic excreta from the walls of blood vessels. This function could never be taken lightly as failure to do so will result in vascular wall edema in acute setting or thickening In chronic setting.
Does coronary arterial tree goes for necrosis in STEMI ?
There is some evidence , when acute total occlusion happens in an epicardial vessel , not only the myocardium is ischemic , the entire distal coronary vascular tree becomes vulnerable. The ischemic time and resistance of coronary macro vs micro vasculature is currently not known. It is expected to show significant variation . We know ,one of the important mechanism of no re-flow following PCI is due to microvascular damage(Non thrombotic)
Many times we fail to realise myocardial viablity and micro-vasculature integirty are two different things. ! This questions the concept of reperfusion based on the status of viable myocardium alone.This we have experienced in many patients as myocardial viability doesn’t guarantee you full recovery from LV dysfunction as microvasculature may recovery may lag behind or never restored (Permanent vasa-vasoral damage ?)
What is our knowledge base about exclusive pathology of coronary vasa vasorum ?
Do you know, ectasia, arteritis, aneurysms and external band like compression of coronary artery all are related to some sort of vasa vasoral dysfunction ? We are not yet clear whether atherosclerosis really involves the vasa vasorum.(Takayasu does it for sure ! )
What is the relationship between vasa vasorum and coronary collaterals ?
It seems to me , many of bridging collaterals are nothing but extension of vasa vasorum and ultimately arise from epicardial coronary collaterals. (Some youngster’s take up this topics for research)
Why is high pressure post dilatation a double-edged sword ?
It’s often thought , larger the lumen its better. Need not be. These are all some questions which we don’t have an answer.
What is the radial pressure exerted by coronary stents on coronary trans -arterial perfusion ?
Does coronary artery go for Ischemic necrosis with high pressure Inflations ? As such there is no published evidence . By the time we wait for published evidence enough number of coronary arteries might get damaged. So try to use common sense .
Relationship between delayed Mal-apposition & vasa vasoral damage
It is very likely ,the so-called endo-leak which is quiet prevalent in aortic interventions is could be seen in coronary arteries. We are not recognising it. It could be same as Intramural hematoma in certain subsets.
Meanwhile, self expanding stents with good radial strength has made a come back .While it may prevent a mal-apposition ,has a potential to stress the vessel wall (Radially) and in the process interfering with perfusion.
Does Vasa vasorum promotes Atherosclerosis or negates it ?

hehttps://www.hindawi.com/journals/bmri/2014/701571
The irony is, while de-novo vasa vasorum is the life line for coronary arterial nutrition, neo-vascularisation is problematic .Then how to selectively promote good vasa vasoral growth and avoid the pathological network that promotes adventitial nodular degeneration ? This is were the curious basic scientists and casual cath lab guys need to interact.What is positive remodelling ? (Often referred to the famous concept of Glagov ) How can we promote it to maintain good luminal diameter inspite of large burden of atherosclerosis by manipulating the vasavasorum.
Final message
Cardiologists are ahead of others in many cutting edge technology. There is no two opinions about it. Who can repair a live beating heart without stoping it for a moment ? Still, there is a whole lot of coronary Ignorance waiting to be explored. Blood supply to coronary artery is one such area to be decoded.This will have larger implications as Vascular healing , plaque survival and growth depends upon vasa vasoral integrity as well as neo vascularisation.
While , metallic management of CAD seems to be the order of the day as it tends to give an instant fix .My guess would be medical sense would ultimately prevail one day with controlled vascular aging and natural ,pharmacological ,biological repair of cells will prevail over temporary patch work in cath labs.
Reference
What is the role of newer Imaging and OCT in visualising Vasa vasorum ?
It is going to open up new avenues in our coronary vision.
(Kensuke Nishimiya European Cardiology Review 2017;12(2):121–3)
As CABANA waves a final good bye to catheters in AF . . . let the pulmonary veins rejoice !
Posted in Uncategorized, tagged ACC AHA ESC guidelines for AF, affirm race cabana, amiodarone for atrial fibrillation, atrial fibrillation, CABANA trial, carto pulmonary vein ablations, cryo balloon for af ablation, heart rhythm society atrial fibrillation guidelines, pulmonary vein ablation, rate vs rhythm control on May 31, 2018|
There is a tough ongoing rivalry between drugs and catheters to conquer the commonest electrical chaos in human heart, namely Atrial fibrillation (AF). Mind you,the confusion about the importance of this arrhythmia is huge and real.Bulk of these episodes are transient , paroxysmal and do not require rigorous management.While stroke prevention seems to be the major aim and target , the real world scenario seems to tell a different story.
The nomenclature conundrum
AF may be classified as many ways a learned cardiologists can think . Often it’s done with reference to etiology, duration , rate, neural (sympathetic or parasympathetic) humoral , cardiac or non cardiac , reversible or irreversible ( Endocrine, Electrolytic, hypoxia etc).
Unlike VT , bifurcating AF with reference to the presence or absence of structural heart disease is rarely meaningful.Subclinical atrial interstitial fibrosis in elderly is so common especially so in hypertensive individuals making all lone atrial fibrillation as true structural disease.
Classifying AF with reference to atrial enlargement again is problematic as any sustained AF can dilate these thin atrial chambers in few weeks time making it a sequel to AF rather than a cause to it.
Adding further fuel to the confusion is the recent man-made (read cardiac scientists!) problem .Linking the etiology of AF with the presence or absence of valves pathology is definitely not helping us. In the process , we forget a casual fact that valvular AF needs aggressive valvular Intervention and not arrhythmia Intervention !*A patient with dilated cardiomyopathy with mitral regurgitation and LA enlargement with AF is considered non valvular AF in spite of clear pathology in mitral valve apparatus.(Is there myocardial AF by the way ?)
What is the current role for catheter ablation in AF ?
The question of advanced catheter based management boils down to a minority of refractory, fast , troublesome AF which has failed by most available drugs. More Importantly the long-term success of ablation is lowly 20% ( PV reconnection, geographical miss, atrial focus etc) and follow-up medication is absolute must even after successful ablation. Its well-known , severe the underlying heart disease more likely is the recurrence .Ironically these are same ones that attract the catheters.
The previous debate of rate control vs rhythm control gave sufficient lessons that complex modalities to restore sinus rhythm is unwarranted . As scientific cardiologists we continue to be adamant and don’t learn from our mistakes and blindly adore and adopt technological excessess.
Now, thanks to CABANA* the ablation for AF has proven to be a fruitless process considering the time ,effort and potential (& real )complications.
*The Catheter Ablation Versus Anti-arrhythmic Drug Therapy for Atrial Fibrillation . Just presented in HRS annual meet at Boston MAy 2018.

Image source : http://www.auntminnie.com
The bright spot is even in these commercial medical world the study like CABANA is a silver lining. Mind you it’s partly sponsored by Industry , still went against them. Three cheers to the genuine medical research team of CABANA for bringing out a truth. Now, I am optimistic more such trials in cardiology will be proposed
A companion to CABANA from UK
A 2018 landmark paper from published in BMJ reveals a dramatic truth that the risk of stroke continues to persist even after resolved Atrial fibrillation, largely concurring with CABANA.(Nicola J Adderley, Risk of stroke and transient ischaemic attack in patients with a diagnosis of resolved atrial fibrillation: retrospective cohort studies BMJ 2018;361:k1717)
So, how to get out of these AF conundrum ?
Practically , an extreme simplification of AF classification is warranted . It should answer these couple of questions !
1. Will the AF in a given patient require long-term oral anticoagulants or not ? (or ok with antiplatelet drug !)
2. Should I make any meaningful attempt to convert the AF to sinus rhythm at all* ?
* You can also redefine the second question , does this AF deserve a EP consult or not ?
Final message
AF is largely a benign arrhythmia in global perspective . However, In those patients were its troublesome , safe and effective drugs are available to tackle it.We shouldn’t Insist to make it complicated.
Meanwhile . . .the anxious pulmonary veins seems to enjoy the moment as they escape from the fire .No wonder they will thank and celebrate the CABANA.
Reference
http://www.acc.org/latest-in-cardiology/clinical-trials/2018/05/10/15/57/cabana
Post-amble and counter point
The RF ablation is a high risk procedure , as we develop less injurious cryo balloons the results of Invasive ablation procedures may score over drugs.Let us wait and don’t prematurely ditch the catheters.
When are you not available doctor ? . . . Please confirm , I am reaching the hospital shortly.
Posted in Uncategorized, tagged ethics in medicine on March 12, 2018| 2 Comments »
Yes, Medicine is a funny science ( some don’t agree , Isn’t Art ?) Many of the noble professionals are silently pursuing their job of saving lives and removing human suffering .Meanwhile, people like this author are needlessly bothered about some Imaginary Issues and write stuff like this one , . . that you are reading now !
Yes, there is an invisible tectonic shift taking place in the name of science.The way we practice medicine currently, it fits in with any of the following descriptions . Divine, Godly,dramatic,miraculous , comical ,cruel or even outright brutal ! (I dare not quantify the weightage of each adjectives used above !)
The field of cardiology as I know personally for the past three decades is challenged by uncontrolled growth (How about proposing 1000 dollar PCSK blocker Evolocumab for a meaningless reduction of few mg of LDL over and above Statin ) Further,the technology goes on to Implode at every corners of wall street ,(Mitra clip for mild MR of DCM ! TAVR for aged Aortic valve ) hijacking commonsense and cost (where is the effectiveness ?) of every stake holder .
In the process ,the critical healing power that resides within every biological system is ignored and ridiculed upon .(You become a fool if you say endothelial tissue plasminogen activator and lytic system will take care of a bulk of the intravascular vascular thrombus if we wait, and we shall permanently defer an Intervention! Current space aged physicians want to invade every existing (or non existing ) problem with multi pronged military strategy and guess what will happen to the humble body which becomes the battle ground.
Coming to the content proper
Sometimes I feel God throws some random truths at an unexpected time through some extraordinary men ! Here is a most unusual study of its kind from the Sanctum sanctorum of Medical science , namely Harvard medical school and Massachusetts General hospital .I think it was presented in ACC Scientific sessions 2018 , Orlando and published in Journal of American heart Association.
Cheers and congratulations to the lead author Dr.Anupam B Jena* , Physician and professor , Department of health care policy , and Health economist
* A video profile of author is in the reference
There is no surprise a paper with such a title had a huge media backlash. USA today reacts . . .
My observations and final message
The paper from MGH, Boston dwells a sensitive area ,of course it has come with a gross conclusion (However, I feel it has hit the bull’s eye.) Still, for the critics, I want to tell one thing , who can deny the fact ? the massive evidence base with 100s and thousands of research papers created by cardiology scientific Industry over the decades is largely a damn squib.
(The problem with acquiring this sort of ready to synthesise knowledge stuff is, It sits right inside our brain and bonds irreversibly , refuse to leave even if these dubious practices are proven dangerous ultimately !)
It might appear , the only option to tackle fake science would be through some dramatic ,less than ideal or mediocre research papers (Or even another fake!) As long as final outcome is good for the public don’t bother about methodology of such studies.(Does it sound in any way I am a supporter of Donald Trump ,! No I am not !)
Reference
Now have a look at this (a long post ) which I wrote some time back. Find out whether these scribblings of mine seem to have grown some scientific backing now .
A brief Info about the author of this unusual paper that has put the field of Interventional cardiology into tail spin and fluttering in cross winds !
How to read medical journals ? Please ensure . . . your knowledge has a short expiry date !
Posted in Uncategorized, tagged venkat quotes on February 25, 2018| Leave a Comment »
One car company recalls 100s of thousands of cars for faulty equipment issues in recent years . It goes on to add , beware , it’s potentially dangerous . . . please fix it and bring your car at the earliest !
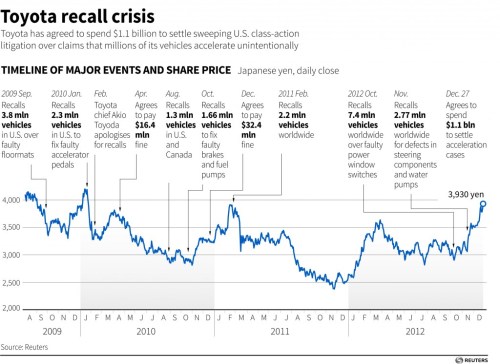
Mean while , scientific medical literature is flooded with dangerous articles, papers and guidelines . . . and pose serious threat to your patients !
Please search for the junk knowledge and then go on to expose, erase and , . . . and throw it to dustbin ! After all , research is searching for truth , again and again !
Let us welcome a new era , where we shall get alerts about wrong knowledge withdrawals and reversal ! Let it challenge the self proclaimed sancto-scientific medical world and a new medical literature cleansing movement (MLCM) begin in every sub specialty.
One such paper from Yale is linked below .
Finally . . . the forbidden message !

How to manage a patient with LA clot and Mitral stenosis ?
Posted in Uncategorized on February 3, 2018| Leave a Comment »
Answer
Though PTMC in the presence of LA clot is an option in low risk clots , my strategy would be the last one ,whenever feasible. Intensive, monitored Heparin /Oral anticoagulants ( Heparin 5000 units tds or qid or Low molecular weight heparin Enoxaparin 40-60mg twice a day , Tablet Warfarin /Acitrom with an INR of 3 ) will dissolve LA clot in 30-50% of times.(Our experience).
The percutaneous clot retrieval system is not available as on 2018.Aortic filters are FDA approved during TAVR. (Why not use the same in PTMC ?) LA Catheter based regional lysis through PFO is can be an option if patient agrees to the risk.
How long to wait for clot dissolution with Heparin /OAC?
Most small clots or intermediate sized clots ((Up to 2 CM ?) have been dissolved by 3 months. Even large clots gets dissolved at least in few Instances.Please note, this strategy is applicable only with valves that is fit for PTMC. All others are referred for surgery.
How does heparin lyse a clot ?
Its a miracle to see it happen, though heparin / OAC are never considered as thrombolytic agents .It happens because both heparin and OAC tilts the local endogenous fibrinolytic forces and thrombus melts , dissolves or disappear altogether. (I am waiting for the day , the scientific community to re-label heparin as a thrombolytic agent, Indirectly though !)
Is there a risk of dislodgement of LA clot during heparin /OAC therapy ?
This question shall be addressed to God ! It all happens if bad luck strikes you and your patient.
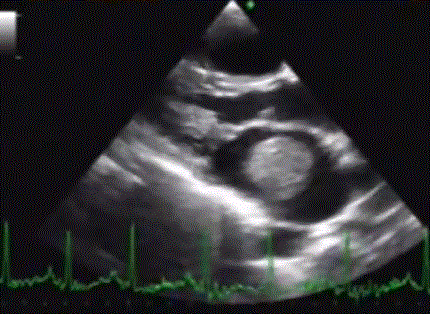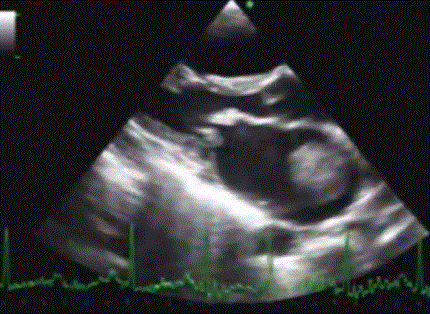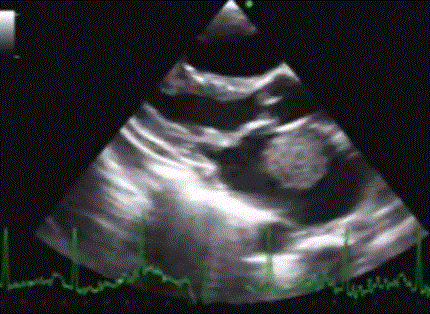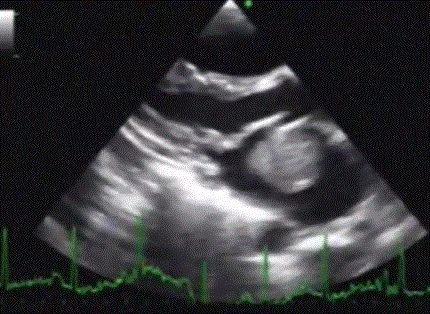
Be wise . . . and call your surgeon Immediately when you encounter something like this !
Even if the valve is perfectly eligible for PTMC , high risk mobile clots, history of embolic episodes , probing and hyper-googling patients , its better to refer for surgery Immediately. Wait and watch game has a definite risk of stroke and it is especially bound to happen if your patient or their family is anxious !
Reference
Cath lab tips : Post dilatation is an unique “Art” . . . can’t learn it from textbooks or workshops !
Posted in Uncategorized, tagged post dilatation, pre vs postdilatation, ptca post dilatation on December 24, 2017| 1 Comment »
In the modern era of cardiology, PCI has become the single therapeutic modality that determines the survival of both cardiologists and possibly their patients! The procedure is all about launching a metal coil inside the coronary artery of a live beating heart.

Millions of diseased and (not much) diseased coronary arteries are serviced (either re/deconstructed ) world-wide on a day-to-day basis.The benefits of the modality is directly related to the wisdom of treating cardiologist and patient’s luck than the original severity of the disease. However, with greatly improved coronary metallurgy , well assisted by drug coating technology and antiplatelet Industry , cardiac physicians believe they have reached the zenith of this procedure.
But the truth is , PCI still has many lingering issues regarding safety , efficacy and cost effectiveness.Early hazard in the form of acute stent thrombosis and sudden death is a reality. Blaming it on patients and their lesions ( condition of blood , gene included) , metal behavior is easy , but, wrong selection (Ignoring the option of CABG) and technical inadequacy of the procedure in the setting of complex vessel wall disease (Hard calcium , deep tunnels , fissures , dead spaces ) is a major cause for concern.
Some personal thoughts about Post dilatation
Lesion preparation , pre/per-dilatation /POTS , etc by itself a big topic (which is not discussed here) Post dilatation after direct stenting is much more vital concept that determines not only the immediate but also the , Intermediate and long-term outcome.
Is routine post dilatation harmful ? or beneficial ?
This is the most tough question to answer . The answer is both Yes and No ! While it was thought useful and mandatory by some , the oppositeis also being adviced few (CCL 2003 POSTIT trial)
What balloon pressure one should post dilate ? At what compliance ? What is the Inflation time ?
It’s akin to asking a musician how to play a piano with fingers or guitar with various strings !
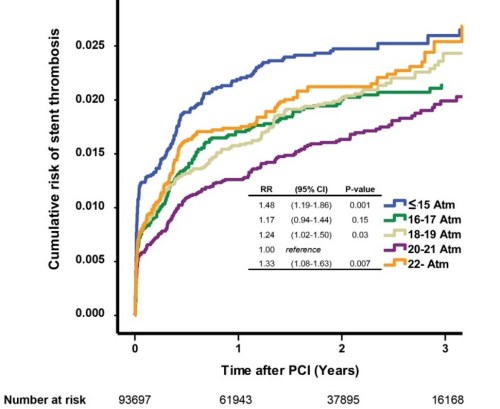
The effect of balloon pressures in the long term outcome. note both low and high pressure dilatation ( blue and orange worms ) hike the risk of restenosis. Too gentle is as dangerous as too harsh making post dilatation a secret and unique art.
Physics of post-dilatation . . . again more questions !
- Is there a role for compliant balloons ?
- Does the compliance of balloon gets altered with hard lesions?
- Is regional compliance matters ?
- Can balloon exert same radial pressure all 360 degrees ?
It’s very likely, the moment balloon encounters an area of resistance it tends to avoid that area and would love to drag on to the area of least resistance and this is often diagonally opposite zone of hard lesions ( if that segment is free from hardness).Then , it will face more stress and likely to bear the brunt of the force risking endothelial disruption . In other words , concentric hard lesions are more amenable for dilatation than patchy hard segments. While the physical forces vary in a stented vs non stented segment , the principle of dynamic forces on static tissue masses with Intervening metal is too complex. (Mind you , we are not discussing entirely different issue , ie thrombus laded ACS lesion , where displacement and pinching of of inter-strut thrombus into distal circualtion would cause no reflow!)
Impact of newer hardware
*Ablation catheters either rotational or Orbital can help , but must be done prior to stenting .Unfortunately , the hardness of a lesion is often realised only after stenting
Is selective high pressure inflations over a particular struts possible ?
As of now , it would be challenging ,( if not outright impossible) .
Let us realise with all our intellect, complex PCI as a whole is taking an uncalculated risk and leave the rest to GOD and DAPT !
Reference article
In an elegant study of more than 90000 PCIs from Sweden and Holland (Ref : Fröbert O, PLoS ONE. 2013 ) found routine post-dilatation pushes the harm curve little more than benefit. The was more with both low and very high pressures .
The outcome of post-dilatation in 900,00 PCIs
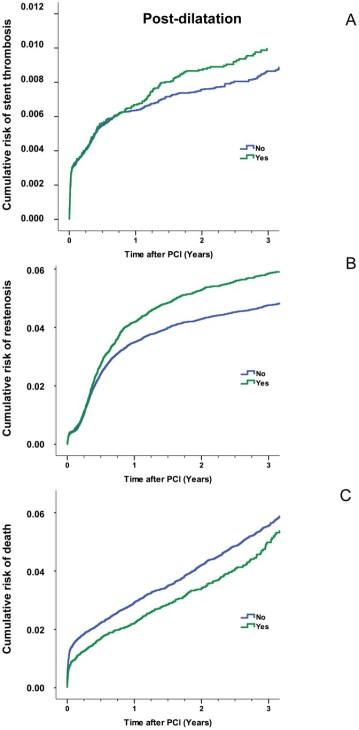
Estimated cumulative event rates of stent thrombosis (Panel A) Restenosis (Panel B ) Cumulative death (Panel C) in relation to post-dilatation .Note the height of coronary Irony, Post dilatation Increase stent thrombosis and restenosis but saves life too !
The stunning truth revealed in this study was , early deaths were more common if post dilatation was not done ! (Panel C in above figure)
Role of Imaging in the decision-making prior to Post dilatation
IVUS, OCT has been extensively used in recent times to diagnose suboptimal deployment and to asses lesion morphology.Though they are expected to improve the quality of angioplasty and hence the outcome , the real world scenario is not really confirming our expectations.
This is because , eagle-eyed HD imaging throws more questions than answers in many and it converts coronary artery into a confused Pandora’s box . In fact these Imaging modalities has created fresh confusions , definitions and guidelines for malapposition under and over expansion , strut fracture, plaque prolapse, internal elastic laminar stress.( Still , I am not able eo understand whats malapposition vs under deployed stent from a practical , pateint point of view !)
Is the Self expanding stent is the answer ?
The conundrum of post dilatation might be cracked if the built-in radial force of self expanding stents is optimally utilised .This could be useful in some tricky lesions when the vessel goes for progressive Glagovian remodeling post PCI. The self expanding stent because of the stored potential energy keep hugging the vessel wall as it expands centrifugally.
Final Message
Post dilatation is neither a mandatory nor a sacred protocol in cath lab. However , it would seem bulk of PCI’s still will require it . Its done judiciously with reference to clinical setting, (ACS vs CCS) , type and location of lesion , stent characteristics etc .Most Importantly , the experience of the cardiologists counts ,and he or she will decide when, where, how much of post dilatation is required (or not required) .
Please remember , PCI as a whole (more so the Pre/ Post dilatation !) is an art by itself. It’s never learnt in text books or even watching live work shops. Every young Cardiologists are enouraged to master the art of PCI , with a huge caveat . Always ensure patient’s Interest are placed first in every step forward. If you are not clear in comphrehending “What is meant by true patient’s Interest ? never Indulge in the procedure or call your mentor , if you have one !
Reference
1.Brodie BR1, Cooper C, Jones MCatheter Cardiovasc Interv. 2003 Jun;59(2):184-92. Is adjunctive balloon postdilatation necessary after coronary stent deployment? Final results from the POSTIT trial. Postdilatation Clinical Compartative Study (POSTIT) Investigators.
















ORBITA trial : First let us do some harm . . . second , we shall . . !?
Posted in Cardiology -Interventional -PCI, Cardiology -Technology, Cardiology -Therapeutic dilemma, cardiology -Therapeutics, Cardiology -unresolved questions, cardiology journal club, cardiology wisdom, Medical education, Medical ethics, Uncategorized, tagged ABUSE OF STENTS, ACC AHA ESC ORBITA GUIDELIES, CHRONIC STABLE ANGINA GUIDELINES, drsvenkatesan, HOW ORBITA TRIAL WILL CHANGE MY PRACTICE, INAPPROPRIATE USE CRITERIA AUC STENTS, LANCET ORBITA STUDY, ORBITA COURAGE BARI2D FAME 2, ORBITA IMPERIAL COLLEGE, ORBITA study, ORBITA TRIAL LANCET, ORBITA trial review and comments, ORBITA VS COURAGE, reviewing ORBITA trial study critically, TCTMD 2017 ORBITA, WAHT WE LEARN FROM ORBITA STUDY on November 6, 2017| 2 Comments »
Cardiologists at confused cross roads !
Perils of limited Intellect & Infinite greed
When not so appropriately trained cardiologists do Inappropriate things “use becomes misuse” . . . then, it won’t take much time for science to become total abuse. That’s what happened with the murky world of coronary stents .No surprise, it’s time to firefight the healers instead of the disease !
Now ,Comes the ORBITA study . Yes , it looks like a God sent path breaking trial that spits some harsh truths not only in cardiology, but also in behavioral ethics .Let us not work over time and hunt for any non-existing loop holes in ORBITA. Even if it has few, it can be condoned for sure as we have essentially lived out of flawed science for too long Injuring many Innocent hearts !
Yes , its enforced premature funeral times for a wonderful technology !
GIF Image courtesy http://www.tenor.com
Meanwhile, let us pray for a selective resurrection of stenting in chronic coronary syndromes and stop behaving like lesser professionals !
Postamble
Extremely sorry . . . to all those discerning academic folks , who are looking for a true scientific review of ORBITA , please look elsewhere !
Rate this:
Read Full Post »