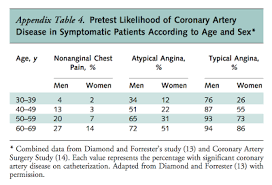
If anyone asks to shortlist the best papers that were, ever published in clinical cardiology, I am sure, this one will reach the top ten. It was 1979, the field of cardiology is just waiting to explode. CAD was managed primarily with drugs and occasional CABGs. Coronary angiograms were an academic luxury. Both thrombolysis and PCI were unknown. Fortunately, Clinical cardiology was still alive and kicking. Dr. George Diamond and Dr. James Forrester from Cedars Sinai, New York worked together to bring this masterpiece. How and when to suspect CAD in the general population? For the first time probability was applied as a diagnostic tool.
The paper begins by analysing basic clinical symptoms, risk factors, then gradually dwell deep into the population-based likelihood ratio, of CAD with the help of stress ECG, Thallium, and fluoroscopic coronary calcium. It finally ends up with a magical fusion of the Bayesian theorem into clinical medicine. It essentially taught us how to accrue scattered knowledge, clinical judgment, and diagnostic acumen among physicians in a community and aggregate them to a powerful statistical evidence base.
It’s more than four decades since this paper was published. There have been some concerns about DF classification in the current era. It was compared with the new Duke risk and found to be less valuable in the low-risk CAD population.(Wasfy MM, et all AJC 2011) The concept of pre-test probability deciding the diagnostic value of screening tests is very much valid. We need to recalibrate the DF scale for the current population and new generation screening methods like MDCT etc..(Gibbons et al Jamanetwork 2021 )
Forget the pros and cons, DF study told us the importance of clinical judgment in the decision making process. Now, we are living in a glamorous new world of cardiology. Cath labs have become our 24/7 office suits, always in hot pursuit for instant fix solutions. Still, we often find ourselves desperately blinking at the doors of EBM, for the elusive answers to some critical queries. Why the same intervention seems to work in one large study and totally go wanting in another? (MITRA-FR vs COAPT)
Where are we erring?
The problem is the way evidence is created. It is often made up of data collected from poorly framed questions and methods, which are incompletely collected or wrongly interpreted. I wish, Bayesian theorem derivatives also address the probability of how pure is the pre-test (research) evidence base available in a scientific community. The core of truth in statistical science lies in, how we understand and define the number needed to treat, (NNT) and the number needed to harm (NNH) with any treatment or diagnostic modality.
Final message
Artificial intelligence and machine learning are projected to be the next big thing in medical science However, the probability of machines prevailing over, human clinical acumen, backed by a sound knowledge base and observation skills appears very minimal. Let us see. Meanwhile, I wish every young cardiologist to go through this paper by D&F to get enlightened.
Reference
Further reading