On this special day , wishing all the readers and followers of this blog an energetic, creative , insightful and of-course a happy new year 2016 !
Just wanted to share the 2015 annual report of this site with the readers.
On this special day , wishing all the readers and followers of this blog an energetic, creative , insightful and of-course a happy new year 2016 !
Just wanted to share the 2015 annual report of this site with the readers.
Posted in Uncategorized | Tagged 2015 annual report dr s venkatesan | 1 Comment »
Metformin is one of most commonly used oral hypoglycemic drug listed by WHO as an essential anti diabetic drug. .It is a biguanide which blocks the hepatic gluoneogenesis . Since lactate is the major substrate for the process of gluco-neogenesis , excess of which spills into blood .Lactate is swiftly cleared by the normally functioning kidneys .Metformin is completely excreted by the kidney. Hence in patients with compromised renal function (or when contrast agents compete with Metformin in renal excretion ) high levels would not only cause lactic acidosis (> 5meq), it can also aggravate contrast induced renal injury resulting in a downward hepato -reno-metabolic spiral.
Though the incidence of Metformin induced Lactic acidoss is low , the outcome can be bad , hence the concern. The European society of urogenital radiology has provided clear cut guidelines regarding Metformin usage when contrast agents are being used.
What can be done in emergency situations
Reference
2. http://ccforum.com/content/pdf/cc12886.pdf
A good article from drug review Contrast induced nephropathy and metformin
Posted in contrast induced nephropathy | Tagged contrast induced nephropathy and metformin usage, eusr guidleines for contrast and metformin, metformin and coronary angiogram, should we stop metformin in all ? | Leave a Comment »
Wall motion defect , in patients after CABG is fairly common.These defects are difficult to interpret as the mechanisms can be multiple.Though the commonest wall motion defect appears to involve the interventricular septum. it can occur anywhere in antero-lateral zone.
The mechanism attributed is the effect of pericardiotomy , which surgeons as we understand leave it open after grafting .This can cause lack of localised ventricular interdependence and results in a a brisk septal movement (bounce )It is an indirect effect .
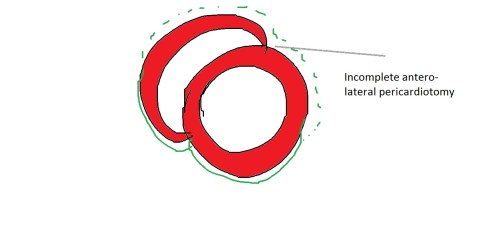
Note the, wall motion defects are confined to the exposed areas of the heart during cardiac surgery .In short axis echocardiography it correlates anywhere between 9 to 3 O clock position. Though interventricular septum is not covered by pericardium in the true sense , there is a indirect bounce effect over IVS due to interference with anterior ventricular interdependence .
More commonly a direct wall motion defect in the 12 to 3 O clock position in short axis is seen .This can closely mimic true wall motion defect as pericardial adhesions can tether these segments. Careful observation is warranted.Myocardial thickening is the key differentiating feature.
What is the physiological impact of these wall motion defects ?
It is generally considered benign (It is !) .Though in echo it looks awkward and suggest desynchrony. The real issue is , it can mislead the echocardiographer to errors in calculation of that universally sacred parameter called EF %
Importance of knowing pre existing wall motion defect.
This has to be reviewed with old reports as it can wrongly create a new wall motion defect de-crediting the surgeons.
New pathological wall motion defect.
Of course it can happen due to peri-operative ischemic insult or infarct . However , It need to emphasised transient wall motion defects are common post CABG due to apparent hypoxia.This seems to be more pronounced with on pump surgeries than off pump .(Expected though) In my opinion, 2-4 weeks cooling off period is required before a meaningful assessment of wall motion post CABG.
Late pericardial reactions and localised constrictive features has been reported.
Disappearance of wall motion defect : How common ?
Any disappearance of WMA is welcome . It happens rarely though . Some of the post ACS population (Both STEMI and UA/NSTEMI) can experience this , as they could harbor zones of myocardial segments afflicted by ischemic stunning rather than true necrosis , that might disappear.
Posted in CABG, Cardiology -unresolved questions, Echocardiography - LV dysfunction | Tagged echocardiography following cabg, paradoxical wall motion defect in ivs septum cabg, post cabg wall motion defect | Leave a Comment »
Inferior STEMI is as common as Anterior STEMI .Unlike the anterior STMI which auto localises to LAD , inferior STEMI has to be fixed either RCA or LCX.
Following ECG features help localize Inferior STEMI .
Finally , and most importantly RV infarction as documented by ST elevation in V4R almost always localises the lesion in proximal RCA.
Role of Echo
If ECG features are not clear , a rapid bed side echo has a very good localizing value. To fix RCA look specifically for wall motion defect between “6 to 8” O-clock position .It corresponds to infero basal septum that is invariably supplied by RCA. For LCX involvement concentrate on “3 to 6” o clock position.
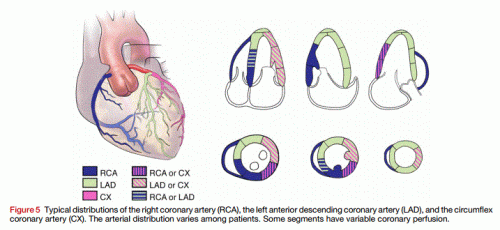
Image source and courtesy http://www.aseuniversity.org
Which has better outcome RCA or LCX STEMI ?
Interventions in RCA is fairly straightforward ,while acute LCX PCI has some issues . Apart from technicalities of intubating the posteriorly curving LCX ,realistically it involves fishing in troubled waters , as we need to cross the left main , likely physical contacts with LAD ostium , which is the sole supply chain for the injured and ischemic LV myocardium . Meanwhile , If RCA is the culprit , its a well cordoned crime scene where one can spend time liberally and fix the lesion.
Final message
It is easier to localisethe culprit artery in inferior STEMI ,but its a tricky to predict outcome .Both can be troublesome .It depends on dominance of the RCA/LCX ,proximal nature of lesion, the number and caliber of OMs, and PLVs and RV branch .However, it remains a fact LCX STEMI has a overall turbulent course.
Posted in echocardiography, Infrequently asked questions in cardiology (iFAQs) | Tagged echocardiographic segments in lcx vs rca, localising inferior stemi rca vs lcx | Leave a Comment »
Co-dominant coronary circulation is defined as , when posterior crux of the heart receives twigs from both right and left system making this water shed area with advantage of twin innervation.They essentially supply inferior and posterior aspect of both left and right ventricle including the posterior aspect of interventricular septum.

Image courtesy modified from :http://www.meddean.luc.edu/lumen/meded/mech/cases/case1/image4.JPG
Traditionally inferior and basal aspects of heart are perceived (wrong tough !) as less important than anterior surface of heart.Infero posterior MI can be extensive and cause significant LV dysfunction and poor outcome. Longitudinal function (AV grooval velocity) and Mitral valve function is critically dependent on posterior circulation.
Is there an advantage for co-dominant circulation with reference to ischemic mitral regurgitation ?
Obviously ,one would expect there is some advantage in co-dominant circulation when ACS occurs either LCX or RCA.It could theoretically protect against development of MR as posterior papillary muscles could receive supportive twigs from its companion.
However , there is a caveat .The antero-lateral papillary muscle normally has twin blood supply from LAD(Diagonal ) and LCX (OM) . But in co-dominant circulation this pap muscle is at risk of becoming single blood supply as the dominant RCA has a trade off with OM with its large PLV branch. It is likely in co-dominant circulations if LAD is the culprit outcomes are likely to be worse.
Final message
A rare study involving more than 200,000 patients which specifically addressed this issue of dominance and outcome , threw some surprising findings. In concluded PCI outcomes with left or co-dominance has a worse outcome than Right dominant system.
Reference
2.Papillary Muscle Perfusion Pattern A Hypothesis for Ischemic Papillary Muscle DysfunctioPaolo Voci, Federico Bilotta, Quintilio Caretta,Circulation. 1995; 91: 1714-1718
Posted in Uncategorized | Leave a Comment »
Verdict ?
Only complicated or high risk STEMI, would require immediate anatomy based management. Please note, this population at worst is never beyond 20 % of all STEMI. Hence more than majority of patients can be managed effectively without CAG.
My reasoning tells me,though knowing the coronary anatomy appear vital , it is rather the physiological impact of those anatomical lesions that will determine the outcome. So,post STEMI, if at all , we need to investigate, it should be about the adequacy of the over all blood supply to left ventricle.This is done by a pre or post discharge sub maximal stress /nuclear test .If it’s negative with a good exercise tolerance CAG will never be required as any critical flow limiting lesion ( that would require intervention )is excluded with near 100% surety.
Postamble :Try asking any neurologist , how often they demand to know cerebral arterial anatomy for managing stroke ? You will get a real surprise answer !
Posted in Uncategorized | Tagged fibrinolysis vs priamry pci, indications for coronary angiogram following stemi, priamry pci vs thrombolysis, revascularisation for cad, stemi guidelines, stemi management controversy, timing of coroanry angiogram in stemi, when to do coronary angiogram stemi ? | 2 Comments »
Holter monitoring is the Initial test for all those with documented syncope (or Pre syncope ) with suspected cardiac arrhythmia .It is a 24 hour ambulatory ECG monitoring , expected to pick up any electrical abnormality and its correlation with the resultant symptom if any. Though the test looks attractive , the diagnostic yield is far less. (About 10%) .The reason being the episodes can be rare to be missed by 24hr sample time. We have extended Holter (48hr) , Event monitors , Loop recorders and implantable devices that can record ECG for extended periods.(18 Months ,Reveal Plus Medtronic) that improve the yield up to 45%.
One common issue that often confuse us while reporting Holter is, the pauses that occur during day / night .
What is the significance of these pauses * ? Nocturnal vs Daytime
Pauses are obviously significant when the patient is awake . It is generally accepted pauses more than 3 seconds during day time (ie Heart rate of < 20/mt ) is significant . This is logical , as pauses more than that, is expected to cause syncope ( or atleast pre-syncope ).The problem comes when you document pauses more than 3 seconds without any symptoms . Then this difficult question comes up ,At what degree of pause syncope occurs ? How is that some persons mange even prolonged pauses with just giddiness.(Good overall vascular integrity and tone ! )
We know such pauses are especially common during sleep. How does the brain react when pauses occur during sleep ? as there is no question of fall as such and loss of muscle tone is non existing.
*Please note ,when we say pause we mean only Sinus pause , Pauses due to AV blocks are very significant
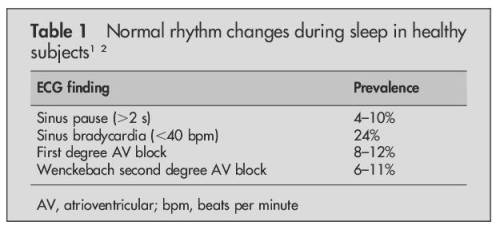
Source : Brodsky M, Wu D, Denes P,et al.Am J Cardiol 1977; .
Dramatic pauses during sleep do occur
There has been prolonged pauses reported during sleep without fatality . A 35 second nocturnal pause resulting in seizures has been documented by implantable recorders.(Mairesse 2003)
Causes for prolonged pauses
Final message
Most bradycardic episodes during sleep are benign.This is due to depressed autonomic control during sleep. Holter interpretation is primarily done with awake rhythm data in most individuals .So, empirically shall we fix a 5 second pause as significant during sleep ? We don’t know.While this may seem applicable even with structural heart disease , one may be vigilant while interpreting the nocturnal pauses in this population .
Caution
** Please note, all these rhythm monitoring extravaganza is meant for people with equivocal symptoms .Patients with well documented syncope with ECG features suggestive of cardiac rhythm disorders would never require these tests and go for pacemaker straightaway.
Reference
Posted in Uncategorized | Leave a Comment »
What are the determinants of dissecting path in Aortic dissection ?
Aortic dissection is taught to us as a dramatic cardiac emergency where the blood enters one of the planes of aortic wall and travels in a random way . The wrong way blood instead of flowing within the lumen invades the vessel wall .(Vascular Tsunami ?) It may (or may not) leave the aorta at a distance resulting in various combinations of true and false lumen. Much like a tsumani its also triggered by an energy releasing blood pressure spikes hitting on the weakened aortic wall rupturing the Intima. While acute dissection are often dramatic chronic dissection can be more subtle clinically.
Apart from the site of entry , blood pressure , condition of aortic vessel wall , there seems to be an invisible force that direct the dissecting tract.How it spares or compromises the arch vessels in selected few , as it travels down remain a mystery . If we can predict and track the plane of dissection by any means with computational hemodynamic models , that will help us plan strategies. Beta blockers are used to reduce the shearing pressure , and emergency surgery is required in many type A dissections.
Do we see a “mini” Interventional opportunity here ? To arrest or direct the dissecting tracts into less benign zone. Shall we deploy an emergency metal ring barrier just proximal to aortic arch in Type A or just above renal arteries in type B to prevent vital organ compromise ? This procedure can be done fast , instead planning a elaborate endovascular intervention which is logistically difficult in arch vessel dissection .This could also act as a bridge to definitive surgery. (Can we compare this with bush fire fighting which are tamed by c0ntroled artificial fire lines and thus avoiding spread to residential areas ! )
Posted in Cardiology -unresolved questions | Tagged aortic dissection, plane of aortic dissection, tracking arch dissection | Leave a Comment »
Preamble * This article is meant specifically for cardiac professionals only .There has been so many queries to me about this device Megavac from patients and public. It is just another tool for assisting angioplasty in very special situations . Successful angioplasty can be performed without the need for such devices 9 out of 10 times. I request the non medical readers to skip this article and follow your cardiologist’s advice and don’t get unduly anxious.
Dr Venkatesan .Chennai.India
If thrombus is the chief culprit in any vascular emergency there can be no second thoughts as it needs immediate arrest without warrant! (STEMI,Acute pulmonary embolism , DVT, Acute limb ischemia etc) Since pharmacological lysis of thrombus is easy and be done immediately it will continue to play a major role still , in many clinical situations that critically compromise organ function .
However , large thrombus burden (or in which medical therapy fails to do a good job ) we must intervene mechanically to change the course of event.Though vascular surgery is a definitive option its always better we try out catheter based thrombectomy.
Many hardwares are being developed in the recent times. Aspiration catheters, baskets etc * .This one from vascular capture (Minnesota USA) appear promising as its a universal capture device that can be used anywhere coronary , pulmonary or even in deep veins .
Clinical case examples using megavac : Video
*Few examples of Thrombectomy devices.
1.They can be mechanical rotational devices like Amplatz Thrombectomy Device (ATD) Microvena, Straub Rotarex (Straub Medical, Wangs, Switzerland) and the Tretorotola Device ( Arrow International, USA) employ a high-velocity rotating helix or nitinol cage that macerates the thrombus.Disadvantage is endothelial contact with moving mechanical parts.
2.The Angiojet device (Angiojet; Possis, Minneapolis, USA) uses a rheolytic mechanism with possible less endothelial injury as there is no true contact with endothelium.
3.Ultrasound mediated lyis ( EKOS Endowave (EKOS Corporation, USA) and Omniwave (Omnisonics Medical Technologies, USA) fragment with high frequency ultrasonic waves.
Posted in Hadwares in cardiology, Hardware techniques tips, Newer hardwares in cardiology, Technology Emerging | Tagged coronary hardware, distal protection device, Thrombus capture megavac, thrombus suction in pulmonary embolism | Leave a Comment »
Effect of PCI on Long-Term Survival in Patients with Stable Ischemic Heart Disease are just out in NEJM.
The results are as expected !
“Let us get more Courage , to say no when we want to say no !”
Reference
http://www.nejm.org/doi/full/10.1056/NEJMoa1505532?query=TOC
Posted in Uncategorized | Leave a Comment »