- Hypertension is major determinant of cardiovascular health of our global population
- Millions suffer, hundreds of societies , and as many guidelines , and drugs are still struggling to control the menace.
- An important sub group of HT , (ie IDH ) population has been neglected and never received the scientific interest , which it deserves !
- In our study it occured in 7.2% of all HT patients.
- JNC, the world authority on HT never considered IDH as a separate entity, and as of now there is no specific guidelines.
- And the irony is complete . There is not a major study available to analyse the differential effects of anti hypertensive drugs on systolic and diastolic blood pressure.
If a patient with the BP of 120/96 asks you , “Doctor , will the drug, you have prescribed , selectively lower my diastolic blood pressure ” what will be your answer ?
A clear , I don”t know !
The following paper was presented in the World congress of cardiology Sydney 2002
Isolated Diastolic Hypertension
S.Venkatesan,S.D.Jayaraj.Gnanavelu, Madras Medical College. Madras, India.
Abstract : Systemic hypertension continues to be a major determinant of cardiovascular morbidity. While isolated systolic hypertension(ISH) has been identified as a specific clinical entity, isolated diastolic hypertension(IDH) has not been reported as a separate group. When we analysed our data from our hypertension clinic we found a distinct subgroup of patients who had elevated diastolic blood pressure with normal systolic pressure. We report the clinical profile of these patients. 440 newly registered hypertensive patients between the year 1998-99 formed the study population. All patients with secondary hypertension were excluded.. IDH was defined as diastolic BP more than 90mmhg and systolic BP less than 140mmhg.
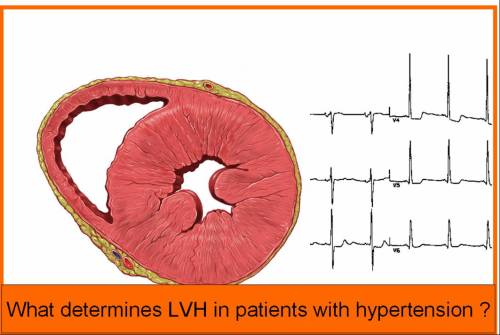
IDH was present in 32(7.2%) patients. The male female ratio was 3:1, mean age was 42(Range32-56) The mean diastolic pressure was 96 mm (Range 90-110).The mean systolic pressure was 136mm(Range 128-140). LVH was observed in 4 patients(12.5%). Diastolic dysfunction was detected by echocardiography in 20patients.(62%)
We conclude that isolated diastolic hypertension constitute a significant subset among hypertensive patients and they need further study regarding the pathogenesis, clinical presentation and therapeutic implication.
Link to PPT will be available soon .

 A normally functioning circulatory system is vital for our survival . We have about 6000 ml of blood, circulating all over the body in an approximate time of 15-20 seconds.The pressure at which this blood moves across the body is called the blood pressure . Hypertension or simply , high blood pressure is an undesirable hemodynamic disturbance in human circulatory system.Systemic hypertension is the most common type of hypertension. The blood pressure is primarily dependent on the status of the blood vessel(vascular resistance) and cardiac contractility. This regulation is under many neural and hormonal factors.Further the blood pressure varies depending upon the blood vessel calibre, and the local milieu.There is a progressive drop in blood pressure from major arteries to the small arteries .The pressure drop is maximum across the arterioles to reach the venules .The venous circulation has the lowest pressure, it ends up at right atrium with a mean pressure of 0- 5mmhg.
A normally functioning circulatory system is vital for our survival . We have about 6000 ml of blood, circulating all over the body in an approximate time of 15-20 seconds.The pressure at which this blood moves across the body is called the blood pressure . Hypertension or simply , high blood pressure is an undesirable hemodynamic disturbance in human circulatory system.Systemic hypertension is the most common type of hypertension. The blood pressure is primarily dependent on the status of the blood vessel(vascular resistance) and cardiac contractility. This regulation is under many neural and hormonal factors.Further the blood pressure varies depending upon the blood vessel calibre, and the local milieu.There is a progressive drop in blood pressure from major arteries to the small arteries .The pressure drop is maximum across the arterioles to reach the venules .The venous circulation has the lowest pressure, it ends up at right atrium with a mean pressure of 0- 5mmhg.
