A simplified animation strictly meant for understanding the concept
Archive for the ‘Cardiology – Clinical’ Category
Anticoagulation protocol in pregnancy with prosthetic valve
Posted in cardiac drugs, Cardiology - Clinical, Uncategorized, tagged anticoagulation in pregnancy, low molecular wieght heaprin in pregnancy, switching to heparin, warfarin vs heaprin on November 16, 2010| Leave a Comment »
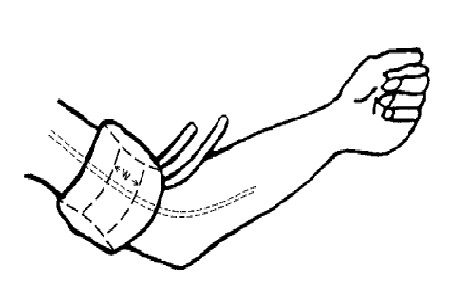
The most important article on hypertension ever to be published :Loose cuff hypertension !
Posted in Cardiology - Clinical, Cardiology hypertension, Uncategorized, tagged cuff length, cuff width, fallacies of blood pressure measurement, how to measure blood pressure, korotkoff sounds, loose cuff hypertension, phase 4 vs 5, riva rocci, sphygomanometer, systemic hypertension on November 13, 2010| Leave a Comment »
Blood pressure measurement , probably is the commonest investigation done in our patients in the entire field of medicine . It is such a common thing , both physicians and patients fail to perceive it as an investigation . (It indeed is !)
Even though BP is considered as a clinical sign , measuring it requires a device called sphygmomanometer . The BP apparatus has to be properly calibrated with the mercury , the tubing, the bladder , inflation balloon etc need to be perfect.
The following fallacies are noted in the measurement of blood pressure . Some of them are rampant* !
Patient
- Posture of recording
- Anxiety -White coat /Gender
Device
- Cuff width/Length
- Arm circumference
Ocular errors
It is surprising , such an important tool has a scale of 2mm markings which is prone for parallax errors of light with mercury column undulating .
Physician factors*
- Hasty cuff syndrome , Rapid deflation .
- Absent minded recording – Failure to note phase 4 to phase 5 due to inattention
- Failure to hear phase 4 muffling (Aging medico -Auditory insufficiency !)
It is not at all surprising to note, two BP readings rarely match , even if it is recorded by the same person with same machine at the same time !
There are many articles that describe in detail , how to record blood pressure properly. But this article from a relatively unknown journal from Purdue university , tells us most scientifically , what has been taken for granted by the medical community for so long .
Loose cuff hypertension (Link to the journal of Cardiovascular engineering )
How much stiffness is to be applied in the arm for optimal pressure recording ?
What is the incidence of hypertension due to loose cuff ?
Final message
The BP apparatus , though appears as an innocuous machine , the readings that emerge from it determines , how millions of our fellow human beings are going to be labeled ! ( High pressured humans , slaves to anti hypertensive drug marketeers for rest of their life ) .
So , realise how important it is , to measure the blood pressure properly ! Never be casual . . . with this machine .
Experience has taught us , while it is very easy to name an individual wrongly as hypertensive , it often needs Herculean efforts to remove this medical tag from their neck . The reasonings are many .( Academic , non academic and patient factors included )
Finally , in this funny planet it is a personal observation ( Or is it an imagination ?) some men and women tend to enjoy , being referred to as high pressured ! Loose cuff or tight cuff , it simply do not bother them !
Clinical implications of Inter atrial septal aneurysm
Posted in Cardiology - Clinical, cardiology congenital heart disese, tagged ias aneurysm, ias aneurysm and focal atrial tachycardia, inter atrial septal bulge, inter atrial septum, ostium secundum asd on October 25, 2010| 1 Comment »
This is a relatively common abnormality of IAS. It is often observed as IAS bulging into left or right atrium in routine echocardiogram.If this happens without atrial hypertension it is termed as IAS aneurysm .
This is due to valve of foramen ovale bending into the RA/LA* cavity for various distance. By definition , the radius of curvature of the bulge should be more than 10 mm to label it as IAS aneurysm.
*Bulging into RA more common
Click on the Image to see the animation
General features
- Mostly a benign entity.
- More often observed in association with PFOs or ostium secundum ASD.
- When occurs in isolation does not result in any shunting across it
- The septal bulge can be static or dynamic . It could swing into LA, RA, and back to LA or vice versa.
- Anatomically 5 types are proposed.
- Multiple fenestration in the aneurysms have been noted.
- Aneurysm formation may aid in spontaneous closure of ASD.
Clinical implications
- IAS aneurysm tend to aggravate stasis of LA blood flow and predispose to minute LA clots and systemic thrombo embolism .
- IAS aneurysm can act as an arrhythmic focus , generating focal atrial tachycardias.
- A non ejection click may be occasionally heard as the IAS aneurysm bulges and tenses within LA/RA cavity .
Reference
1 . Olivares -Reyes A, et al. Atrial Septal Aneurysm: A new classification in 205 adults. J Am Soc Echocardiogr
1997;10:644-56.
2. Longhini C, et al. Atrial septal aneurysm: echocardiographic study. Am J Cardiol 1985;56:653-67.
3. Gondi B, Nanda NC. Two-dimensional echocardiographic features of atrial septal aneurysm. Circulation 1981;63:452-57
4. http://www.fac.org.ar/revista/00v29n4/congreso/premio3.PDF
Why there is wide and fixed split of S2 in ASD ?
Posted in Cardiology - Clinical, Uncategorized, tagged asd, ATRIAL SEPTAL DEFECT, fixed split of asd, hang out interval, hangout interval, impedence of pulmonary circulation, puklmonary vascualr resistance, shaver hangout interval, ssytemic vascular ressitance on October 13, 2010| 3 Comments »
- Second heart sound is widely split because the pulmonary hangout interval* is wideFixed because , the RV stroke volume does not show the normal respiratory changes.This is due to dynamic phasic shunting across the IAS ( For example : During inspiration , if RA,RV volume gets augmented by 50ml from IVC inflow , in expiration this IVC augumentation is removed but a 50 ml augmentation from left atrium takes place , this keeps the RV diastolic , as well as systolic volume relatively constant.) This makes the 2nd heart sound fixed .
* Hangout interval is the gap ( in time ) between the arterial pressure curve and the respective pumping chamber pressure curve (RV, LV) at the level of incisura.
Incisura is the notch on the descending limb of arterial pressure curve , when the pulmonary or aortic valve closure occurs . When we analyse the simultaneous pressure recordings of RV ,LV/Pulmonary artery/Aorta , the arterial pressure curves faithfully accompanies the chamber pressure curve along the dome of the chamber pressure curve till it descends , where it dissociates , from the chamber pressure curve and hangs out for a certain milliseconds. This time interval is called as hang out interval (Named by Shaver et all )
What is the normal pulmonary hangout interval and systemic hangout interval /
Pulmonary hangout interval is 60-80ms
Aortic hang out interval is 20 ms
Why does it happen ? What does it signify
It happens because , even as the chamber pressure falls below the arterial pressure ( Note: Semi lunar valves close at this cross over point ) blood continues to rush forward , with momentum in to the pulmonary and systemic circulation, in spite of the pressure cross over has happened, the semilunar valve doesn’t get closed exactly at the cross over point .It gets closed little later than true cross over point.This gap in time is the hangout interval. This Interval keeps the arterial pressure not only to be sustained little longer but also slightly higher .
This interval is an indirect( inverse) marker for vascular impedance of the distal draining circulation .The impedance is same as vascular resistance for all practical purposes.Since pulmonary circulation is a low impedance circulation , it has a wide hangout interval and the systemic circulation vice versa.
How much of S2 widening is contributed by RBBB in ASD ?
This is not known .But it has a minor role in prolonging S2 split. This is because , the RBBB in ASD is most often incomplete and peripheral one .( Pesudo RBBB due to RVOT dilatation )
What happens to S2 when pulmonary arterial hypertension develops in ASD ?
It is often narrow and fixed . Pulmonary arterial hypertension makes the pulmonary circulation to behave like systemic , hence the impedance becomes high and the hang out interval is significantly lost and second sound is narrowly split. (But fixity may be maintained.)It also depend upon the RV function and associated RBBB. RV dysfunction and RBBB both tend to widen the split.*Mild PAH usually does not alter the S 2 splittingIs there any other cause for wide and fixed splitting of second heart sound ?
Having known the reasons for widening and fixity it is easy to understand , a patient with right heart failure and RBBB can have a wide and fixed split .
Widening is due to RBBB (Delayed activation of RV ) . Fixity is due to severe right heart failure makes the RV out put relatively constant .(As RV inotropism is not good enough to handle the inspiratory augmentation of RV end diastolic volume.)
Why in VSD the second heart sound is not wide and fixed split even though hemo- dynamically it fulfills the same hemodynamic scenario ?
* Hangout interval is the gap ( in time ) between the arterial pressure curve and the respective pumping chamber pressure curve (RV, LV) at the level of incisura.
Incisura is the notch on the descending limb of arterial pressure curve , when the pulmonary or aortic valve closure occurs . When we analyse the simultaneous pressure recordings of RV ,LV/Pulmonary artery/Aorta , the arterial pressure curves faithfully accompanies the chamber pressure curve along the dome of the chamber pressure curve till it descends , where it dissociates , from the chamber pressure curve and hangs out for a certain milliseconds. This time interval is called as hang out interval (Named by Shaver et all )
What is the normal pulmonary hangout interval and systemic hangout interval /
Pulmonary hangout interval is 60-80ms
Aortic hang out interval is 20 ms
Why does it happen ? What does it signify
It happens because , even as the chamber pressure falls below the arterial pressure ( Note: Semi lunar valves close at this cross over point ) blood continues to rush forward , with momentum in to the pulmonary and systemic circulation, in spite of the pressure cross over has happened, the semilunar valve doesn’t get closed exactly at the cross over point .It gets closed little later than true cross over point.This gap in time is the hangout interval. This Interval keeps the arterial pressure not only to be sustained little longer but also slightly higher .
This interval is an indirect( inverse) marker for vascular impedance of the distal draining circulation .The impedance is same as vascular resistance for all practical purposes.Since pulmonary circulation is a low impedance circulation , it has a wide hangout interval and the systemic circulation vice versa.
How much of S2 widening is contributed by RBBB in ASD ?
This is not known .But it has a minor role in prolonging S2 split. This is because , the RBBB in ASD is most often incomplete and peripheral one .( Pesudo RBBB due to RVOT dilatation )
What happens to S2 when pulmonary arterial hypertension develops in ASD ?
It is often narrow and fixed . Pulmonary arterial hypertension makes the pulmonary circulation to behave like systemic , hence the impedance becomes high and the hang out interval is significantly lost and second sound is narrowly split. (But fixity may be maintained.)It also depend upon the RV function and associated RBBB. RV dysfunction and RBBB both tend to widen the split.*Mild PAH usually does not alter the S 2 splitting
Is there any other cause for wide and fixed splitting of second heart sound ?
Having known the reasons for widening and fixity it is easy to understand , a patient with right heart failure and RBBB can have a wide and fixed split .
Widening is due to RBBB (Delayed activation of RV ) . Fixity is due to severe right heart failure makes the RV out put relatively constant .(As RV inotropism is not good enough to handle the inspiratory augmentation of RV end diastolic volume.)
Why in VSD the second heart sound is not wide and fixed split even though hemo- dynamically it fulfills the same hemodynamic scenario ?
Guess the answer .It will be posted soon.
How will you manage failed pulmonary thrombolysis in acute pulmonary embolism ?
Posted in Cardiology - Clinical, cardiology -Therapeutics, tagged acute pulmonary embolism, failed pulmonary thrombolysis, pulmonary embolectomy for acute pulmoanry embolism, rescue pulmonary thrombolysis, thrombolysis for pulmoanry embolism, time window for pulmoanry thromolysis, what is failed thrombolysis on October 10, 2010| Leave a Comment »
Acute massive pulmonary embolism is a dreaded medical emergency . In the past, surgical embolectomy was the main option . Now , we have thrombolysis as a viable option.But , it does not work in all cases.* (90% success ?). It is critical to evaluate the success of thrombolyis , before embarking upon rescue embolectomy.
As it is often in critical care medicine , this decision making is not easy .
The key question is how long , we shall wait before labeling thrombolysis a failure !
In-fact , premature assessment is the commonest cause for failed thrombolysis. True failure is different from deemed to be a failure . This is often related to , lack of patience among the members of treating team . Unlike acute MI ,there is not a strict time window to follow .The issue hear is , not lung salvage but restoring VP/VQ and dead space ventilation . The assessment is made , by clinical , MDCT ,Echo parameters.
When there is difficulty in judging success , clinical parameters will prevail over medical images !
Key clinical parameters for monitoring
- Heart rate
- Saturation
- Blood pressure
There are four options available to manage in failed pulmonary thrombolysis.
1.Emergency embolectomy in an unstable patient *
2.Elective , planned embolectomy in a sable patient **
3.Repeat thrombolysis ***
4.Continue Intensive heparin regimen for up to a minimum of 72hours and up to a week .
* Dismal outcome .
** Best option (Ironically, these are the patients , who improve with medical management , as well !)
***This is especially useful when partial success is noted in a stable patient . ( For rescue thrombolysis it is logical tom use TPA if SK was used initially and vice versa.) The logic here is the initial dose was either insufficient or ineffective to lyse the thrombus completely. If TPA is not available /or not affordable, repeat SK can still be considered .It can be safely administered within the 5 days of initial dose.
**** Least popular and considered inferior but has worked wonders in many .
How to manage a relatively stable patient with a large thrombus load in his pulmonary artery ?
Option number 3 could be tried. Prolonged monitored heparin
What are the surgeons concern about management in failed pulmonary thromolysis ?
Every surgeon( Especially the cardiac surgeons) loves to operate in a stable patient . If you hand over a case for pulmonary embolectomy , with sinking O2 saturation and falling blood pressure ,the outcome can be easily predicted !
Further, RV dysfunction is notoriously known for pump dependency . CT surgeons are vastly experienced in the intra operative tips and tricks of managing LV dysfunction (They may not be in so in RV dysfunction !)
Bleeding risk is also high especially in the milieu of intensive anticoagualtion and thrombolysis .
The mortality could be as high as 30 % in many centers.
Final message
- The incidence of failed pulmonary thrombolysis is often subjected to the whims and fancies of treating physician and the imaging modalities used.
- Timing of assessment is critical .One need to give a long rope for medical management , in spite of the urge , to do something more. .
- Clinical improvement should be the main guiding force.
- Normalisation of tachycardia , improving trend of o2 saturation( >90-95%) , regressing RV size are useful parameters.
- Thrombus load detected by a repeat CT scan , need not be the sole guiding parameter.In -fact , mobilising these patients for CT scan by itself is fraught with a risk of worsening the hypoxia.
- The issue of tackling the source of thrombus should be addressed separately .Luckily, the same anticoagulant protocol takes care of this issue also. It is rarely a emergent issue.
- Deploying an IVC filter as an emergency procedure is a bigger controversy .At best , it is useful in few high risk individuals with high risk mobile ileo-femoral clots .
- Finally, not every one can handle this situation .Ideally such patients should be to be shifted to a well established cardiac surgical set up .
From Chest journal
http://chestjournal.chestpubs.org/content/129/4/1043.full.pdf+html
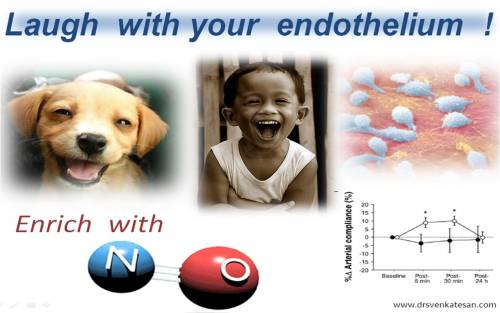
Laughter and enothelial function
Posted in Cardiology - Clinical, tagged beneficial effects of laughing, cardio vascualr effects of laughing, endothelial function, laughter and medicine, nitric oxide, positive emotions and heart on September 24, 2010| 1 Comment »
- Endothelium is the largest vascular organ in the body .
- It is constantly being serviced by both the circulating blood from the luminal side as well as from the abluminal plane.
- The discovery of nitric oxide and endothelin was a breakthrough .
- They are under neural, mechanical and endocrine control .
- Negative emotions like anger and depression has a high correlation with hypertension and cardiac event
- Positive emotions like laughter and happiness is expected to have good vascular tone
This fascinating study from Japan and USA (Texas) published in American journal of cardiology , discusses how a comedy movie possibly releases nitric oxide profusely from our endothelium
Link placed with the courtesy of AJC
http://www.ajconline.org/article/S0002-9149(10)01050-7/abstract
50th anniversary of cardiac resucitation had just gone by . . . silently !
Posted in Cardiology - Clinical, Cardiology-Land mark studies, tagged cpr, jhon hopkins, Kouwenhoven on September 23, 2010| Leave a Comment »
In 1960 , exactly 50 years ago , a group of doctors from Jhon Hopkins published their observation in 20 cases. It went on to become , one of the most remarkable discovery in the history of cardiology .
They taught us how to use a pair of hand , as an artificial heart and save lives
They are . . .
- Dr Kouwenhoven*
- Dr James R. Jude, and
- Dr G. Guy Knickerbocker .
* He was not a medical doctor but an electrical engineer at Hopkins but he worked in the medical school as well .
They meticulously documented , each patient’s case history , whom they were able to successfully revive , (It was in the same period , the AC/DC shock was also invented in the Hopkins ) .One of the highlights of their paper was , with each chest compression they were able to elevate the carotid pressure up to 90mmhg and was recorded in a pressure tracing .
We have to thank the JAMA (Journal of American medial association ) for making this original article available free in their website .
Must read for every cardiologist
http://jama.ama-assn.org/cgi/reprint/173/10/1064?ijkey=33bb40fe3062331bae50e10c8a04263f3e26b317
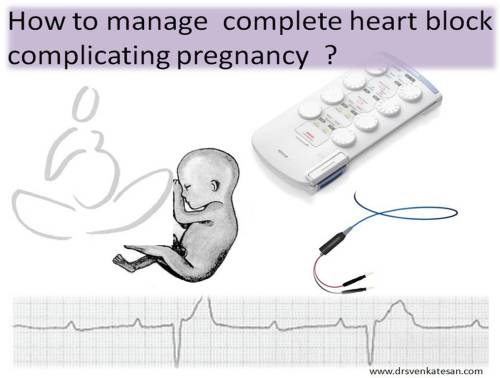
How to manage complete heart block during pregnancy ?
Posted in Cardiology - Clinical, cardiology -Therapeutics, Uncategorized, tagged chb, complete heart block in pregnancy, congenital complete heart block in pregnancy, how to manage complete heart block in pregnancy, management of chb in pregnancy, pacemaker in pregnancy, temporary pacing in pregnancy on September 19, 2010| 1 Comment »
For the lay public the term complete heart block (CHB) often convey a sinister message . When encountered in pregnancy, it is frightening for the physicians as well . One need not say . . .the anxiety to the Obstetrician !
Congenital complete heart block is the usual etiology. Though there are other important causes of CHB in general population , it is very rare to get an ischemic or degenerative heart blocks in the reproductive age group.
There are many ways it can present .
How does it present ?
- Symptomatic CHB detected first time during ante natal screening
- Asymptomatic CHB detected incidentally during ante natal screen
- CHB first time recognised during active labor. Either symptomatic /Asymptomatic
- A more familiar situation is CHB diagnosed in child hood . Women in question can undergo an elective marriage and a managed pregnancy.
* The success of modern medicine lies in the mantra of “early diagnosis ” .Ironically , early detection of CHB in pregnancy adds considerable anxiety to mother , family and the treating physician . So ignorance can be a bliss here , as 99/100 with CHB would not require any intervention during pregnancy .But , in this hyped up scientific world one needs lot of courage to simply watch a pregnant mother with a heart rate of 45 ! .You are tempted to do something . We have seen CHB presenting in labor room as emergency and delivering successfully by vaginalis .
Where is the pathology in congenital complete heart block ?
It is usually due to anatomical discontinuity between AV node and the bundle of his. The most fortunate thing here is , these patients develop a junctional escape rhythm at around 40-45/mt .This is enough for most basal activities. Further this junctional rhythm can increase up to 100 in many, or even up to 120 at times of stress.(Accelerated junctional rhythm )* .An ECG which shows a narrow qrs complex is nearly 100 % specific for a stable junctional escape rhythm.
What is the hemodynamic stress of pregnancy ? Will a heart rate of 50 /mt enough , to support the labor or cesarean section ?
Nature is a wonderful equalizer. What the pregnant mother requires is a good cardiac output to nourish the baby as well as herself. A heart rate of 50 is often able to sustain and support the entire pregnancy with ease.
How it is done ? . . . is it not simply amazing ?
In pregnancy there is less of systemic vascular resistance due to various reasons (Low impedance placental circulation, reduced sensitivity to Angiotensin 2 ) . The heart can always increase it’s out put by increasing the heart rate or stroke volume. In patients with CHB , as the rate can not be increased much , the heart accepts the alternate option quite easily without any protest . The low SVR also facilitates increase in stroke volume. This is the reason pregnancy is often well tolerted even with the heart rate < 50 /mt.
But , at the time of delivery increase in heart rate may be important in some.We do not know , who will require this HR support .This makes it mandatory to have a temporary pacer standby.
What are the ominous signs and symptoms of CHB in pregnancy ?
Having discussed a lot about the benign nature of congenital CHB , one need to realise it is also a potentially dangerous heart rhythm . Syncope, symptomatic hypotension (BP<90) and some times signs of PIH , all possibly indicate a pacemaker support .
Can we do an exercise test to assess the chronotropic competence in pregnancy ?
Tread mill test is generally not done in pregnancy. It is a good option , to test the adequacy of heart rate increase during activity . If the heart rate increases up to 100 -120 it is a good response .
What about holter ?
A less predictive , but more acceptable investigation is the 24 hour holter monitoring that gives a rough idea about lowest and highest heart rate. If there is a long pause > 5 sec , she will be a technical candidate for permanent pacing ! once you have documented this , we will be sued if not paced however asymptomatic the patient is ! So beware of this investigation !
Atropine stress test ?
This again is a simple test , that will measure the chronotropic reserve. A concern for fetal tachycardia is genuine !
Pre-conceptional counseling
A patient with congenital complete heart block should never be adviced against pregnancy.
“Pace and become pregnant ” strategy is also not warranted.This is based more on the perceived scientific approach the and litigation fear than reality !
Only issue is we have to make sure , the women in question has adequate hemodynamic reserve. This can be easily accomplished by asking some basic questions about exercise capacity .Or , she can be put on a tread mill (or atropine stress test). If the heart rate increases up to 100/mt there is absolutely , no need to put permanent pacemaker.
Peculiar issues in pregnant women with permanent pacemaker
The paradox of modern medicine felt at it’s best here !
We think , we are implanting a pacemaker in CHB of to provide good hemodynamic support during the stress of labor. But a fixed rate VVI pacemaker will not do this job . The real reason to put a pacemaker is to avoid a dangerous bradycardia during the labor .
Hence , patients with CHB carry equal concern (if not more !) during labor as the pacemaker fires at a fixed rate of 70/mt and the native rhythm is often suppressed due to long-term pacing . Hence their heart rate often fail to increase beyond the pacemaker rate of 70 . Paradoxically , patients with untreated CHB (with their native rate ) , can increase their heart rate often up to 100-120 at times of stress .This is possible because their AV node is still under the control of autonomic system , while artificial pacemakers* are not !
*Some of the current pacemakers have overcome this problem with rate adaptive pacing .
Mode of delivery ?
- Natural , expected
- Induction of labor
- Elective cesarean
- Emergency Cesarean
Can complete heart block per se , become an indication for cesarean section ?
No. It is always an obstetrical indication .It is better to avoid GA / Regional anesthesia in cardiac disease. The stress of second stage of labor is always less than that of surgery provided it is not unduly prolonged .
Assisted /accelerated vaginal delivery is the best option .However , one should be ready for any intervention. Some obstetricians feel that, elective cesarean section could be less stressful than labor( which could be prolonged for some unpredictable reasons ) while a , Cesarean section can not be a prolonged one !
Cardiologist’s role in the labor room
The role of cardiologist is to provide support to the obstetrical and anesthetic team prevent extreme bradycardia. Inserting a temporary pacemaker with back up pacing of 50/mt is preferred.Trans-jugular approach is ideal .In difficult cases fluroscopy guided temporary pacing in cath lab is advised.
Role of temporary trans cutaneous pacing as stand by ?
This method of pacing with two sticky electrodes in the chest wall with external pacing .It is proven , efficient useful modality of pacing in coronary care units .However this can be a substitute for only few hours of support . May have patient discomfort .In places from expertise for temporary pacing is not immediately available this can be used .However presence of such a machine increase the comfort level of physicians.
Is there a rate adaptive temporary pacing available ?
Currently available temporary pacemakers are not rate adaptive , and hence we have to pace roughly at about 90 or 100 give allowance for labor related demand (We would not know, how much the mother is compensating with increasing with stroke volume ) in this case pacing rapidly may reduce the net cardiac output as the mother’s heart is used to operate at different point in the frank staling curve right through the 10 months
Anesthetic issues in complete heart block during cesarean section
Anesthetists have a concern here.(Genuine one of course) A cardiologist with a standby temporary pacemaker is to be arranged. Cardiologist will decide whether to have sheath or sheath plus lead in standby mode .
Many anesthetic drugs have an adverse effect on heart rate. Drugs to be avoided are Fentanyl ,suxamethonium, neostigmine Induction with propofol has risk of worsening bradycardia . Controlled epidural anesthesia is preferred .This ensures slow onset anesthesia and limits hemodynamic instability.Bupivacaine is known to cause depression of heart rate .(Even with epidural route )
Miscellaneous questions
A often debated query among obstetricians : Should I refer a CHB patient to a cardiologist or electro-physiologist ?
There is no academic answer to this question.Logic demands conservative (without compromising patient/baby safety ) management .Electrophysiologists are rarely conservative
Radiologically how safe it is ( for the fetus ) to undergo permanent pacemaker implantation ?
For implanting a permanent pacemaker, about 15 minutes of fluro time is required which could be significant .So it should be used in exceptional situations only.
What is the effect of maternal complete heart block on the fetal hemodynamics?
Nil or almost nil (Surprise ! surprise)
Issues during weaning of pacing in postpartum
Post partum period can be troublesome in few as fresh blood volume injected from contracting uterus.If temporary pacing has been done , it is usually possible to wean by 48 hours. Permanent pacing is rarely required
Final message
- Congenital complete heart block* during pregnancy is a well tolerated rhythm.
- The panic this entity creates is largely unwarranted. This conclusion is derived from decades of observation by eminent clinical cardiologists.
- The heart rate reserve can be estimated by a minimal exercise test .(Atropine test with caution )
- Insertion of either permanent pacemaker is not necessary* in most .
- If there is symptomatic hypotension /syncope during any time during pregnancy pacemaker becomes mandatory .
- During labor /or cesarean section insertion of temporary pacemaker “may be” needed. Hence a cardiologist stand by with a temporary pacemaker is advised to tackle any emergency(Which is anyway highly unlikely !)
.
* This rule is applicable only in isolated congenital CHB. Ischemic CHB or CHB with associated LTGV,AV canal defects etc need special attention.
References
Books
Journal articles
The famous paper which first described safe outcome four patients with CHB in preganancy without pacemaker
http://medind.nic.in/iad/t06/i1/iadt06i1p43.pdf
http://www.joacp.org/index.php?option=com_journal&task=check_subscription&id=1077
anesthetic issues in pregnancy and CHB
A new coronary risk factor : Community smoking
Posted in Cardiology - Clinical, Cardiology -unresolved questions, tagged air pollution and cad, community smoking, new cad risk factor, passsive smoking, smoking and cad on September 10, 2010| 1 Comment »
Coronary artery disease can be termed as “New age plague” afflicting the mankind ! It probably has killed ( or Killing ) as many lives as most other diseases put together. Why only a section of our population is vulnerable is not fully understood .
We are familiar with coronary risk factors for too long . . . still . . .
We do not understand why 50% CAD occur in people who have no known coronary risk factor !
There has been propositions and dispositions of various risk factors . The latest one is the Air pollution. This is quiet interesting, as air is the staple food of human survival . We eat , drink , (Rather inhale ) about 500 ml /of air every 3 to 4 seconds for 24 hours a day for 365 days , for our life time !
Does the air we breath reach the largest cardiovascular organ namely the vascular endothelium ?
Yes definitely , not only it reaches the endothelium but also injures it (When it contains gases other than oxygen ) .While tobacco is a well established endothelium destroyer , it is no surprise community smoking ( Air pollution !) will do the same job with perfection .
What are the proposed toxins in the air pollution that harm the endothelium ?
It is a mixed masala gas out there over our polluted cities ! .(Atmosphere, Industrial, Automative ,Domestic, Human , and other invisible sources ) We need to analyse further to answer this question authentically .
Though , common sense is enough to establish the link between air pollution and CAD. We have lots of evidence coming up . . .
Reference
Further research
We will be shortly reporting our experience with endothelial function assessment in traffic police population of our city Chennai ,India .
The “must read” books on Intra-operative transesophageal echo and mitral valve repair !
Posted in cardiac surgery, Cardiology - Clinical, echocardiography, tagged echocardiogram, mitral, mitral valv e, mitral valve repair, tee, transesophageal echo on September 7, 2010| Leave a Comment »
Mitral valve can be termed as the most important valve of heart . The reason for this : It is the only valve that is dependent on the Left ventricular function (The parameter which determines the ultimate outcome in any form CAD ! )
So , indirectly mitral valve function will invariably be affected by some degree at least in most patients with LV dysfunction. (After all LV free wall , is a component of mitral valve apparatus.)
While , we have numerous modalities to assess mitral valve function , the one that has fascinated the surgeons during mitral valve surgery is the intra operative TEE.
Many believe TEE provides live images of mitral valve which are not possible even under direct vision ! The eye of the TEE sees the mitral valve from a posterior location , (of -course It can see at any angle !) while surgeon can see in one angle . The types of repair , the adequacy of repair, the annulus status, even a trial mitral run , can be done with the help of TEE.
The TEE probe silently does this job sitting inside the esophagus , without obstructing the surgeon’s operative field .
The success of TEE as an investigative tool did not come easy.Decades of observation , innovation and learning( Especially from department of cardiac science Mayo clinic USA , where they standardized the views. ) are involved .
Now we have omni plane, real time 3D TEE probes .
The books which are considered the best for TEE aspects of mitral valve and it’s repair are