This RIFLE shoots without bullets . Yes ! it helps the cardiologist to trouble shoot the kidneys which often suffer from cath lab cross fires .
As the cardiologists indulge in sophisticated cardiac procedures , in more and more sick and co- moribund patients , it is becoming increasingly important for them , to give due respects to other organs as well !
Renal function is an important determinant in the over all outcome in any cardiac patient.
- How to assess the baseline renal function ?
- How to measure the impact of the cardiac procedure ?
- How to follow up and monitor the progress of renal function in coronary care unit.
- How to reduce the enhanced renal risk ?
- When do you call for the Nephrology consult ?
Every step becomes vital . Do not ever think , a cardiologist’s job is over once few stents are deployed . Wheeling out a sick and fragile diabetic with borderline creatinine out of the cath lab may be considered as a procedural success , but the real success happens only after every organ of the your patient comes out unscathed after the procedure . In this context , we should first aim to become a nephron savvy and a nephron friendly cardiologist .
I have witnessed cardiologists spend hours together in cath lab with liberal injections of contrasts even in elderly who have delicate kidneys .Cardiologist should realise kidneys are soft and gentle organs which unlike the heart , do not know how to cry (Angina) at times of stress as they lack well developed pain fibers (unmedulated type c fibers to be precise!) .Only thing they know is ( like touch me not plant !) they strike work the next next morning (What we refer to technically as Acute renal shut down !)
Now , we see little interaction occurring between a cardiologist and nephrologist prior to PCI , even though those two organs ( The respective experts behold ) are constantly in touch with each other , every minute , by neural and hormonal mechanisms. The new generation organ specialists has to learn a lot from these sincere , interactive , democratic human biological system.
Coronary arteries can gulp any amount of dye but not the renal arteries .The future looks still more frightening , as we have a variety of devices lined up to invade human vascular tree (TAVI, Renal ablation, per cutaneous aortic pumps etc)
So what should we do ?
- Patients prone for CIN should be promptly recognized .
- Ask repeatedly the question . Am I sure ? . . .does this patient require this procedure at all ? If so , have I taken all the precautions ?
- Use the nephrologist’s services more liberally
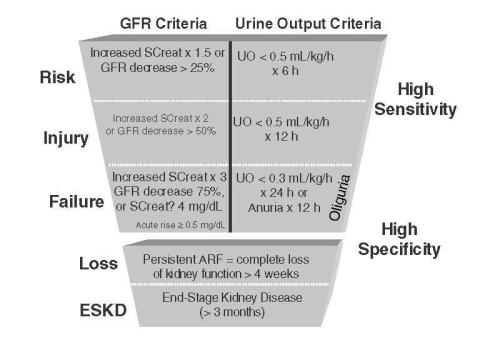
Finally , read the basics of nephrology lessons once again . The international consensus group has classified the Acute kidney injury (AKI) with a simple and lovely criteria for risk triaging . It is a five faceted , inverted (Tip less ) triangular cartoon called RIFLE .
The beauty of RIFLE lies in its simplicity . All it requires is serum creatinine (eGFR) levels and urine output. Let every cardiologist master this scheme of AKI . It will immensely help our patients and make us a complete physician instead of being labelled as a “master of an organ” or ” An accessory sub physician”
The CIN prevention recipe.
References
For review about Contrast nephropathy (CIN) there are lots of excellent articles.
One company is trying to find a new solution for this complication . Let us welcome it ! The device is called rena guard .