God has created and arranged every organ in an order with a purpose . The unique relationship of the food tube and the heart which run silently , posterior to the heart has evoked much interest for the cardiologists.
Whenever LA is enlarged it pushes the Esophagus back .We also know the vintage clinical entities of cardiac dysphagia that occurred with rheumatic mitral stenosis.
Since the lower end of esophagus just hugs the left atrium , this anatomical concept was successfully exploited for imaging heart in TEE.Now cardiac anesthetists routinely use the esophagus as an imaging port during complex mitral valve surgeries.
How esophagus can be utilized to resuscitate the heart at times of emergency ?
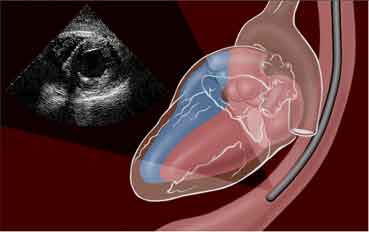
Note , the esophagus does a friendly hug as it crosses the heart posteriorly .It is a perfect anatomical sense , to Image and pace the heart from within the esophagus !
In a cardiac arrest situation , when we need to rapidly access to heart , we have multiple options .Each has some advantage and few draw backs.
- Trans-venous pacing is the standard method, but even for experts it needs few minutes to reach the heart for pacing
- Trans cutaneous pacing (Zoll) is a viable option , but not widely popular for some unknown reason (Patient discomfort ? High threshold ?)
- Emergency trans-thoracic needle pacing option is a primitive method still can save a life or two on it’s day !
It was in 1980 , a dramatic concept was conceived . Why not use the esophagus as an access for pacing the heart
after all , it reaches as close as possible to the heart !
How to convert a Ryles tube into a a trans – esophageal pacing lead ?
There was a certain article on this topic , which I read , when I was cardiology resident. It answers the following. Distance form mouth , Discomfort of the lead , Pacing threshold , Esophageal burns .
I am unable locate that article. Will post it once I get it.
Limitations of trans-esophageal pacing*
- The most important limitation is it can pace only the atria with high degree of success.
- Ventricular pacing is not that successful for the simple reason esophagus is anatomically insulated by the atrial chambers.
- Tran gastric positioning may reach the basal aspects of Left ventricle , but the threshold needed is too high that will invariably cause discomfort.This can be used in a dying patient when there is no other option .
* Primarily useful in acute SA nodal defects, sinus arrest or any other atrial electrical failure. Infra- nodal complete heart block trans esophageal pacing may not be effective .
Other potential uses of trans-esophageal leads
Over drive pacing
Overdrive entrainment of tachycardias , including resistant ventricular tachycardia is possible.
Trans esophageal ECG recording .
This can magnify p waves during supra ventricular tachycardias and aid in decoding narrow qrs tachycardias
Safety Issues and Caution
Good earthing is necessary .Burns can occur.
Final message
Every cardiac physician is expected to possess the expertise to rapidly pace a heart by trans jugular /subclavian access at times of emergency .
Further , any modern CCU will have a defibrillator equipped with trans-cutaneous pacer as well. (The disposable pads are too costly and is a deterrent in many hospitals !).
This article explores other possible way to pace the heart in dire emergency situations.
It has one more purpose ! It rekindles the acumen , motivation and hard work of our cardiac ancestors (Which many of us are pathetically lacking !)
http://circ.ahajournals.org/cgi/reprint/65/2/336
Role of trans-esophageal lead during EP study atrial fibrillation
http://cardiovascres.oxfordjournals.org/content/38/1/69.full
Read Full Post »




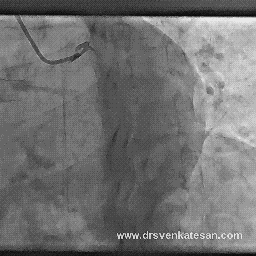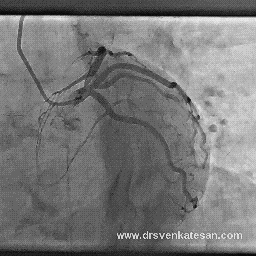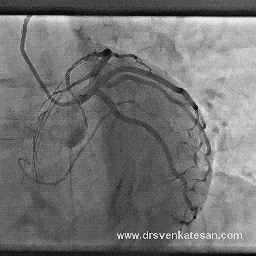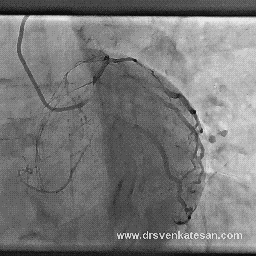








TRANSFER-AMI study : Transfer with caution . . . bumpy roads ahead !
Posted in Cardiology -Interventional -PCI, cardiology -Therapeutics, Cardiology -unresolved questions, cardiology journal club, cardiology journals, Uncategorized, tagged comments about transfer ami, facilitated pci, FAILED THROMOLYSIS, journal watch transer ami, letters to the editor transfer ami, nejm transfer ami, REACT STUDY, rescue pci, routine early pci, stemi, tenecteplase failure, time window for pulmoanry thromolysis, TRANSFER -AMI STUDY on January 14, 2011| Leave a Comment »
Preamble
The much published TRANSFER -AMI study has few important queries to ponder about.It was supposed to test the role of routine PCI following thrombolysis. In other words it compared rescue only strategy with routine strategy.The caveat is , even among failed thrombolysis, the rescue strategy has not convincingly proven superior to medical management (if the time is lapsed ) as much of the damage is done .
Will the investigators share their experience ?
Finally
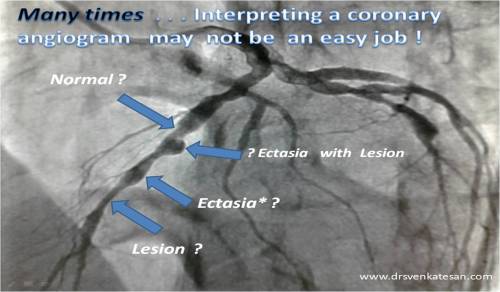
Why the title of the paper says it is about “Routine angioplasty” and the conclusion emphasizes it is indeed “high risk subsets ofangioplasty” (While the study itself involves a 92 % least risk Killip class 1 ) . Why this double dose of confusion ? (Is it deliberate ! Which i think is unlikely )
NEJM please take note of this . . .
All that glitters are not natural glitter . . .some are made to glitter !
Rate this:
Read Full Post »