Atrial fibrillation is one of the common tachycardias encountered in cardiology practice.In this condition even though atria fibrillates up to 600 times a minute, only a fraction of that reach the ventricles. Thanks to the AV node.It acts like an electrical sink . Hence in most episodes of AF , the ventricular rate will be manageable and hovers between 150-220 .We also know , in the presence of accessory AV nodal pathway there is a risk of 1:1 conduction and result in ventricular fibrillation and risk of sudden death. (Sudden death in WPW syndrome)
A case scenerio
The other day my resident called me to inform about a patient with atrial fibrillation and hypotension .
I told him , to control the heart rate with Amiodarone and I shall come in shortly ,
He replied , the rhythm looked to him like a bradycardia ! I asked him to wait , when I went there , it turned out to be an interesting ECG .
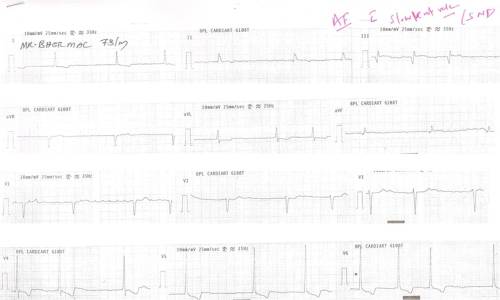
This was a 73 year old man in our ER with a syncope .

Magnified view of lead V 1 and V 2. Note the ventricular rate of 40 /mt even a the coarse f wave are recorded > 300 mt .He had a structurally normal heart .This patient has been adviced a VVI pacemaker .
While atrial fibrillation is primarily a tachycardia , occasionally like the above patient it may present as bradycardia !
How this happens ?
As mentioned before AV node acts like an electrical sink .
How AV node is able to filter out much of the incoming impulses is not clear. This property of AV node is actually the major physiological property of AV node .This is refered to as decremental conduction (The faster it is bombarded with electical stmuli the longer it will take rest !) When this filtering function of AV nodal tissue is too much we call it pathological AV nodal response.Some believe , it is an expression of associated pathological high-grade AV nodal block . Others belive it is simple vagotonia.
Another possibility is it is a sequale to complete AV block and what you witness is nothing but a junctional escape rhythm ( But here RR interval would be fairly regular )
Excessive AV nodal blockers (Digoxin/Verapamil ) can mimic the same picture .
What is the relationship between sinus node dysfunction(SND) and atrial fibrillation ?
AF with slow ventricular response is common in elderly population with sinus node dysfunction.
AF can be associated with SND in two ways
- Atrial disease and sinus node dysfunction is known to occur together . This is not surprising, considering the close proximity they live. SA node is surrounded by atrial tissue in its entire length and breadth .When degenerative and infiltrative disease of atria occur it may trigger a simultaneous SND , as well as atrial fibrillation .
- While another possibility is that AF is a default electrical response to SND . There is some evidence to suggest the atria may release a ectopic escape rhythm which may either degenerate into AF or mainfest a primary AF .
What is controlled ventricular rate and what is slow ventricular rate in AF ?
- This aspect is not well-defined in literature.
- Controlled response generally means HR 70- 90/mt
- Slow ventricular response would be <60 /mt
- Pathological bradycardia is diagnosed with HR < 50 or at any symptomatic slow rhythm .
- Holter or event monitors would help in these situations.
What is the incidence of AV nodal disease in SND ?
AV nodal disease is seen in significant population of SND.(Some series show up to 30 %) .Further , the incidence of new onset AV block increase with every year of follow up ) Reversible forms are commnly due to drugs and electrolyte disorders. The AV nodal disease has another importance as they determine the selction of pacemaker mode .SND with intact AV node function can be managed with atrial based pacemaker ,while ventricle must be paced in patients with AV block or in whom the risk of AV block is high.
Is there a clinical advantage of having some AV nodal disease in AF ?
It may seem so , as long as the AV nodal disease do not lead to severe symptomatic CHB.A slow ventricular rate is a desirable response in patients with angina and cardiomyopathy (especially tachycardic ). While we continue to debate for years about the superiority of rhythm control over rate control , if the AV node chooses to slow down by natural means , ventricles would welcome it with pleasure !
Final message
Atrial fibrillation is primarily a tachyarrhytmia , occasionally it may present as bradyarrhytmia .In this scenario one has to suspect hidden AV nodal as well as sinus nodal dysfunction. ( This entity was also refered to as Tachy brady syndrome ) It is important to recognise this entity because many times dangerous bradycardias have occurred with a single dose of Amiodarone bolus or DC shock . These episodes represent “unmasking effect” of occult AV nodal disease.