Preamble
The resting coronary blood flow (CBF) is about 5 % of cardiac output. It amounts to 250 ml /min (0.8 ml /mt/gram of myocardium ) It is estimated, blood flow across LAD is 50% . LCX and RCA share 25% each, depending upon the dominance. No need to say , the net return to coronary sinus should match the CBF at rest or exertion.(Minus a small fraction contributed by thebesain and vene cardia minimi flow, into the right heart chambers)
Great cardiac vein (GCV) is the venous cousin of LAD. It must receive and empty 125ml of deoxygenated blood every minute into the coronary sinus, if LAD flow is normal. When LAD microcirculation is obstructed as in severe obstruction , GCV will fill and empty sluggishly.
Let us move on from physiology to bedside.
Primary PCI & No -reflow in LAD
We have painfully realized, no-reflow is almost a hemodynamic death sentence to the concerned coronary artery during primary PCI. For practical purposes, no-reflow is common in left coronary circulation, that too in LAD. Decades of research and experience haven’t really helped us to either overcome or treat this complication effectively.
So, it’s worth considering experimental mechanical options.
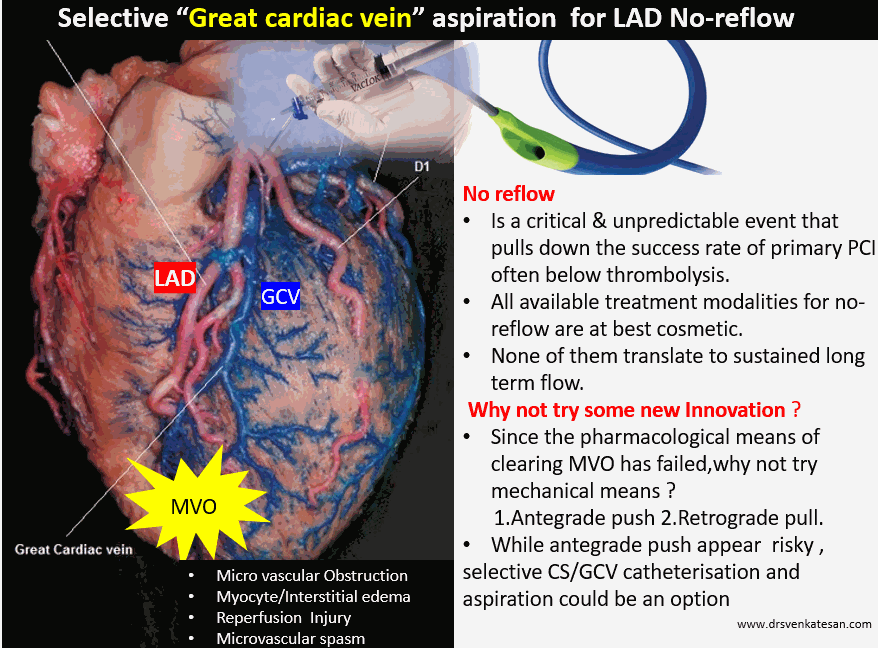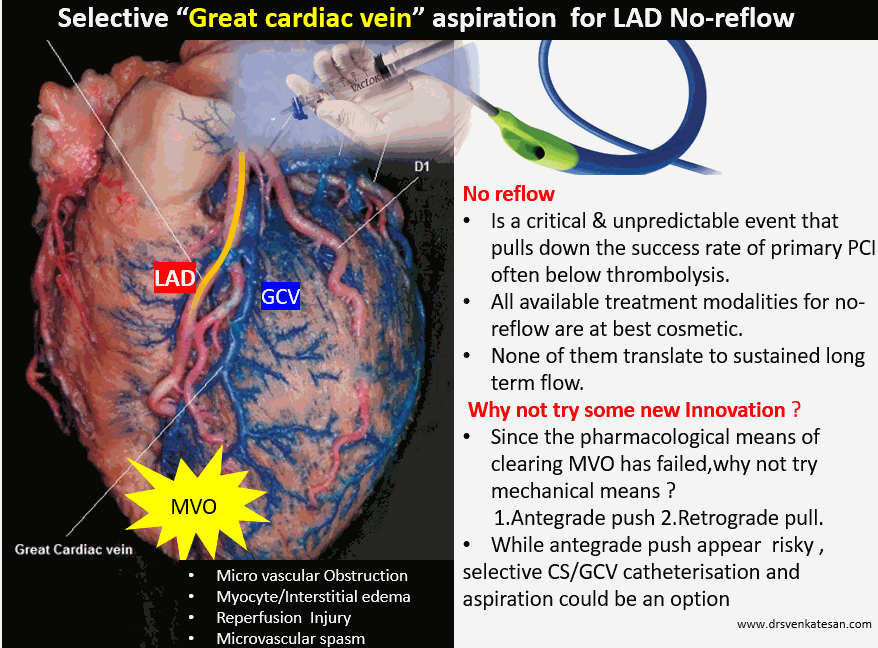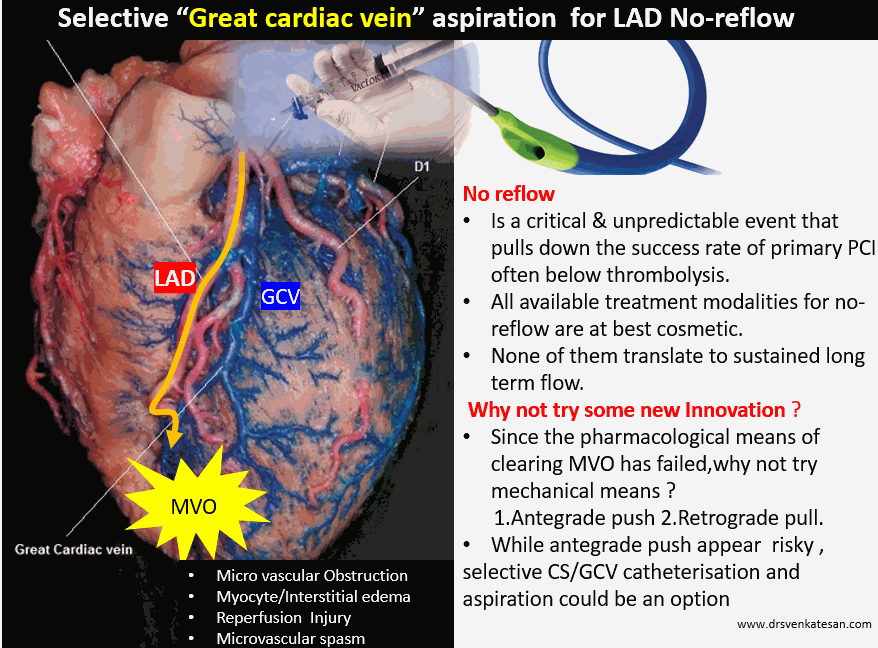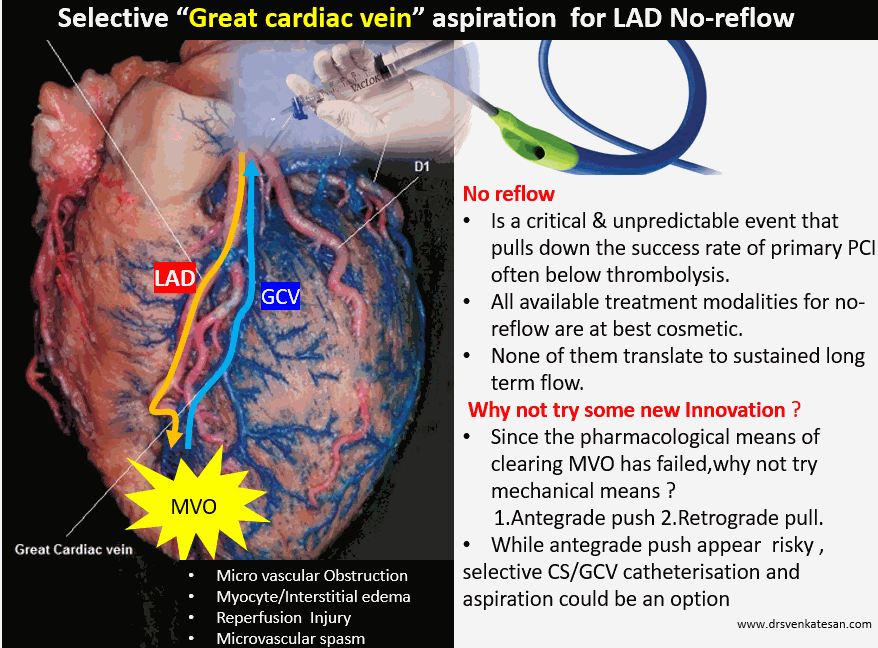
- The first option is, to forcibly open the closed microvasculature by pushing the debris across arterioles, venous capillaries and subsequently to the coronary sinus. This appears tricky as the high-pressure injection can be hazardous. This can be done either hand or even controlled pressure Injection. (It is believed few centers do this unofficially and found some success. I am not sure)
- The second option is again mechanical but uses negative pressure to suck from the far end of microcirculation. We can pull the debris into the coronary venous circuit by using vacuum suction deep inside the main stem of the coronary sinus or even the great cardiac vein, the venous counterpart of LAD. This appears to be more comforting to the coronaries at least theoretically. (Never under-estimate the power of vacuum as a biological Intervention.I recall tender newborns pulled out with massive vacuum pressure without any issues during my O&G days)
We have proposed this idea to scientific committee. It was rejected promptly as expected even prior to applying for ethical clearance. In fact, we were eager to try our hands on this, as a life saving modality in desperate situations. Now, It is an appeal to all those scientificaly liberal centers to try this concept that can be made legal as a part of an official trial.
Antegrade vs retrograde aspiration
It is wiser to introspect, why most antegrade thrombus aspiration strategies in epicardial coronaries failed in STEMI .Still, what is the possiblity it might work retrogradely? Let us hope this concept becomes a success and doesn’t add on to the long list of failed attempts to this ubiquitous hemodynamic entity.
Potential risk
Since the mechanism of MVO and no=reflo is multifactorial, mechanical suction might help only in the clearance of thrombotic debris. Further risk of microvascular endothelial injury is real.
Final message
Many fellows write to me, asking for some research ideas. Please acknowledge if anyone proceeds with this one (If you really believe no one has thought about this Intervention before)
Reference for Interventions within Coronary sinus
- EP guys do it , in a regular fashion with CRT.They also specifically enter the Anterior cardiac and great vein during ablation in VTs originating from LV summit .
- Coronary sinus aspiration done for contrast removal after angiogram to prevent AKI in renal compromised patients.(Ref Osama Ali Diab Circulation: Cardiovascular Interventions. 2017)
- Stem cell delivery has been done through coronary sinus (Wouter A. Gathier J Cardiovasc Transl Res. 2018)
- Coronary sinus retrograde perfusion has been tried for refractory angina (David P. Faxon Circ Cardiovasc Interv. 2015)